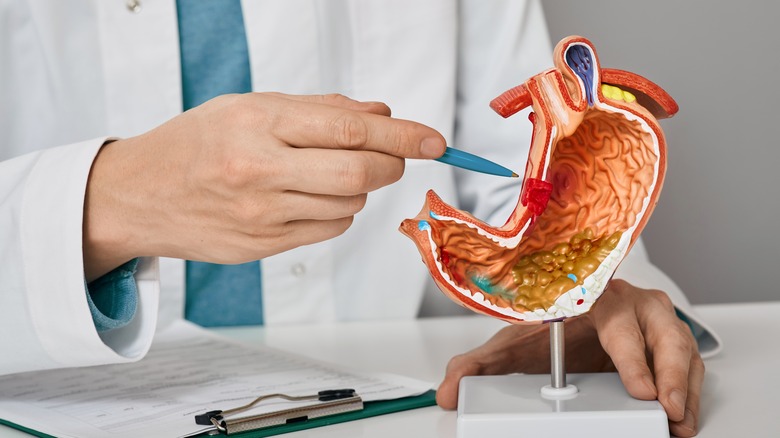
Mesenteric Venous Thrombosis Explained
If you have mesenteric venous thrombosis, it means you have a blood clot blocking a major vein (such as the superior mesenteric vein) that drains blood from your intestines, per Medline Plus. Blood clots are a natural process. They form when you get a cut, stopping the bleeding and facilitating the wound's healing (via American Academy of Family Physicians). According to the North American Thrombosis Forum, these clots should break down after the wound heals; however, some clots fail to dissolve after an injury, while others emerge even if you don't have an injury. This condition is known as thrombosis — the blocking of blood vessels by inappropriately formed blood clots.
Vascular Medicine: A Companion to Braunwald's Heart Disease (Second Edition) reviewed numerous studies of mesenteric venous thrombosis. According to the book's authors, the condition is rare; however, it can be linked to many life-threatening complications. One of the studies reviewed pegged the condition's mortality rate at 34%, which is higher than the World Health Organization's mortality rate for cancer.
Causes of mesenteric venous thrombosis
According to Healthline, there appears to be a significant relationship between mesenteric venous thrombosis and various digestive diseases that inflames the tissues around the intestines. These conditions include abdominal injuries and infections like appendicitis or inflammatory bowel diseases like diverticulitis, ulcerative colitis, and Crohn's disease, per Healthline. The source adds that inflammation of the pancreas or scarring of the liver can make a person more susceptible to mesenteric venous thrombosis. For this reason, smoking, which destroys organs, can increase your susceptibility to the condition.
There seems to be growing evidence supporting the claim that mesenteric venous thrombosis can be linked to hormonal drugs and birth control pills. A 2017 study published in the Open Access Journal of Contraception describes mesenteric venous thrombosis as associated with the use of oral contraceptives. However, the study confirms the condition is still rare in women who take oral contraceptives. In fact, the condition is more common in men than in women, according to Medline Plus.
While the risk of mesenteric venous thrombosis stems from various medical conditions, some people may get the disease through genetic factors. Vascular Medicine: A Companion to Braunwald's Heart Disease (Second Edition) links the condition to hereditary or acquired hypercoagulation disorders, including factor V Leiden, protein C, protein S, and antithrombin III deficiencies.
Symptoms of mesenteric venous thrombosis
According to a 2022 study published in the journal StatPearls, mesenteric venous thrombosis is described as idiopathic and spontaneous, meaning that it's hard to tell its causes or symptoms. As a general guide, the symptoms can include fever, constipation, septic shock, lower gastrointestinal bleeding, and nausea (via Medline Plus). Such symptoms usually require urgent medical care. Besides these vague symptoms, you might also have unexplained abdominal pain linked with a feeling of tenderness in the abdomen, per the study by StatPearls. The pain can be sudden or develop slowly, spanning weeks (via WebMD). Unlike other pain-manifesting problems in the stomach, pain caused by mesenteric venous thrombosis might not worsen with external physical pressure. If your doctor pushes the affected area, you might not feel any significant pain, per WebMD.
Although mesenteric venous thrombosis is uncommon, some symptoms, like septic shock, can be life-threatening. This potentially fatal symptom has a hospital mortality rate of up to 50%, according to a 2021 study published in the journal Frontiers in Immunology.
Diagnosis of mesenteric venous thrombosis
Diagnosing mesenteric venous thrombosis isn't always simple. Your doctor might use various diagnostic measures to determine if you have the condition. Some are more invasive than others. Generally speaking, scanned images from your abdomen area can be obtained through various procedures, including X-rays, CT scans, computed tomography angiography (CTA), or magnetic resonance imaging (MRI) (via WebMD). Nuclear scintigraphy is another method, which is quite invasive. According to a 2014 study published in the Journal of Clinical and Experimental Hepatology, the procedure uses radioactive elements to diagnose diseases in delicate areas within bones and tissues.
Abdominal imaging is an effective non-invasive alternative. Mayo Clinic Proceedings explains this procedure can effectively present abdominal abnormalities in the veins in about 50% to 75% of cases. The procedure explores the presence of a thrombus within the vein using focal translucency images. After, it can measure the thickness of the bowel walls, ensuring the reading doesn't exceed 3 millimeters, per Mayo Clinic. Your doctor might detect signs of swelling in the intestines or blood vessel blockages around your intestines, helping to conclude whether you have mesenteric venous thrombosis.
Treatment of mesenteric venous thrombosis
Thrombosis is progressive, and the overarching treatment goal is to limit its extension and long-term prevention, per this 2020 study published in the Journal of Pancreatology. Another 2016 study published in the Journal of Vascular Surgery: Venous and Lymphatic Disorders reiterates the effectiveness of thrombosis treatments using anticoagulants, which treat about 68% of mesenteric venous thrombosis cases. Anticoagulants are a group of medications that can be administered orally, via injections, or intravenous routes to break down existing clots or prevent new clots from forming. (via Cleveland Clinic).
According to Medline Plus, in rare cases, some doctors also recommend surgical thrombectomy as a treatment for mesenteric venous thrombosis. During a thrombectomy, the surgeon makes an incision in blood vessels to remove blood clots and restore blood flow (via Johns Hopkins Medicine).
Other advanced treatment options for mesenteric venous thrombosis include fibrinolysis or bowel resection, which may work best for patients with hemodynamic instability or refractory symptoms, per a 2015 report in Circulation. According to the study, fibrinolysis performed using catheter tubes can be extremely dangerous and must only be performed if you have refractory symptoms that anticoagulants can't manage. People with highly sensitive mesenteric venous symptoms can also rely on surgical procedures like laparotomy. According to Medical News Today, this treatment option can help mesenteric venous symptoms like abdominal pain and peritonitis.
Complications of mesenteric venous thrombosis
Even though the benefits of taking anticoagulants outweigh their risks, the National Health Service warns of bleeding-related complications associated with anticoagulant medicines. This includes bleeding gums, prolonged nosebleeds, heavy periods in women, and blood in stools or urine. Other non-bleeding-related complications include dizziness, headaches, indigestion, or skin rashes. Regarding the side effects of thrombectomy, the surgery has been associated with bleeding disorders, multiple organ failures, and other life-threatening complications like sepsis, per this 2005 study published in the Journal of Vascular and Interventional Radiology.
Despite the various complications that may arise with treatment, a blood clot, in general, is a life-threatening condition, according to Cleveland Clinic. No matter how mild the symptoms of mesenteric venous thrombosis are, it's important to speak to your doctor early to ensure a proper diagnosis is made. This way, your doctor can determine which treatment option is best. Your doctor might also look into your medical history when prescribing treatment.