Myths About Birth Control You Can Stop Believing
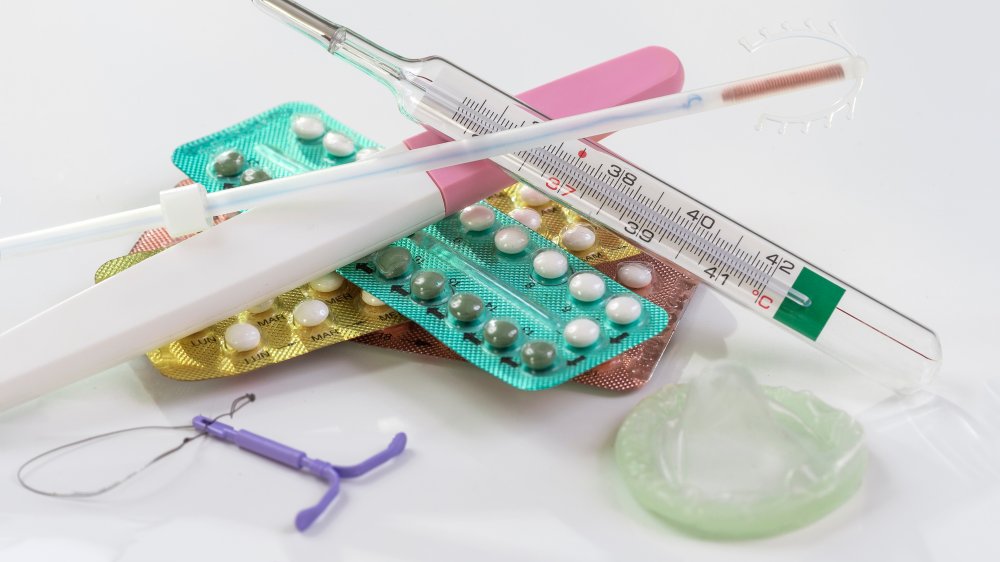
Birth control may have been a taboo subject not too long ago, but these days it's absolutely commonplace. According to statistics from the Centers for Disease Control and Prevention (CDC), 99 percent of women age 15-49 who have ever had sexual intercourse have used some form of birth control from 2015 to 2017. No surprise, 94 percent have used male condoms, the most easily accessible form of birth control. A whopping 81 percent of those women have been on the pill at one time or another, while 24 percent have used three-month injectable contraception (Depo-Provera), 24 percent have had an intrauterine device (IUD) or another contraceptive implant (usually inserted in the upper arm), and 22 percent have used emergency contraception like Plan B.
But despite the fact that the majority of women have used birth control at some point, there are so many myths floating around about how various forms of birth control work and what they do to your body. Before you decide that you're for or against hormonal birth control — the pill, the hormonal IUD, Depo-Provera, or the NuvaRing — or a non-hormonal form of long-term birth control like a copper IUD, read up on the current evidence and what experts have to say.
Hormonal birth control causes weight gain
Maybe you had a friend in high school who told you that her older sister gained some weight after starting the pill in college. Maybe you know some vague information about how hormones affect your weight and immediately jumped to the conclusion that the hormones in the pill will cause weight gain.
In general, that isn't true. Most women will not gain weight because of the pill, Dr. Andrea S. Fernandez, an OB-GYN at Wake Forest University School of Medicine, told Everyday Health. While every woman responds differently to birth control, there's no evidence that the pill or other forms of hormonal birth control cause significant weight gain. One 2006 review of the literature looked at 44 existing studies and found no significant effect of birth control on weight.
If you're worried about gaining weight when you start the pill, the best thing to do is keep up with your healthy habits. Eating a balanced diet and exercising regularly is the best way to maintain a healthy weight (via Everyday Health).
You should take a break from hormonal birth control every once in a while
Have you ever wondered if "giving your body a break" from your birth control and the hormones it comes with is a good idea? If you have, you're not alone. "There's this thought that it's good to give your body a break from the medication, so some people will just stop it," Jennifer Kickham, an OB-GYN at the Massachusetts General Hospital, told Self.
But that's just not the case. "I usually don't recommend [taking a break from the pill] if people are sexually active, because that's how unintended pregnancies happen," Kickham said.
If you're noticing bad side effects after going on the pill — headaches or lack of sex drive, for example — talk to your OB-GYN about other birth control options. But don't take a break from the pill just because. Your hormone levels will go back to what they were before you started taking the pill, which for many people means heavier periods and more painful cramps. And again, it'll leave you unprotected against pregnancy, which isn't a good idea unless you're actively trying to get pregnant.
A hormonal IUD will stop your period
No one's denying that periods can be inconvenient and sometimes painful, so it's natural that you'd cling to the message that a hormonal IUD can end your menstrual woes by totally stopping period. Plus, how great would it be to not have to shell out cash for tampons every month?
Unfortunately, most women who get hormonal IUDs placed don't actually lose their periods altogether. In a 2016 study of 1,802 women published in the journal Contraception, the authors found that only 4.9 percent of women reported amenorrhea — that is, the absence of a period — within three months of getting a hormonal IUD, and only 15.4 percent reported amenorrhea within 12 months of getting a hormonal IUD. The authors also found that women who had lighter and/or shorter periods before starting any kind of birth control were more likely to report amenorrhea as a side effect of the hormonal IUD than women who typically had heavier, longer periods.
But it's not all bad news. According to the Mayo Clinic, a hormonal IUD can make your periods lighter and can eliminate menstrual cramps or make them less severe.
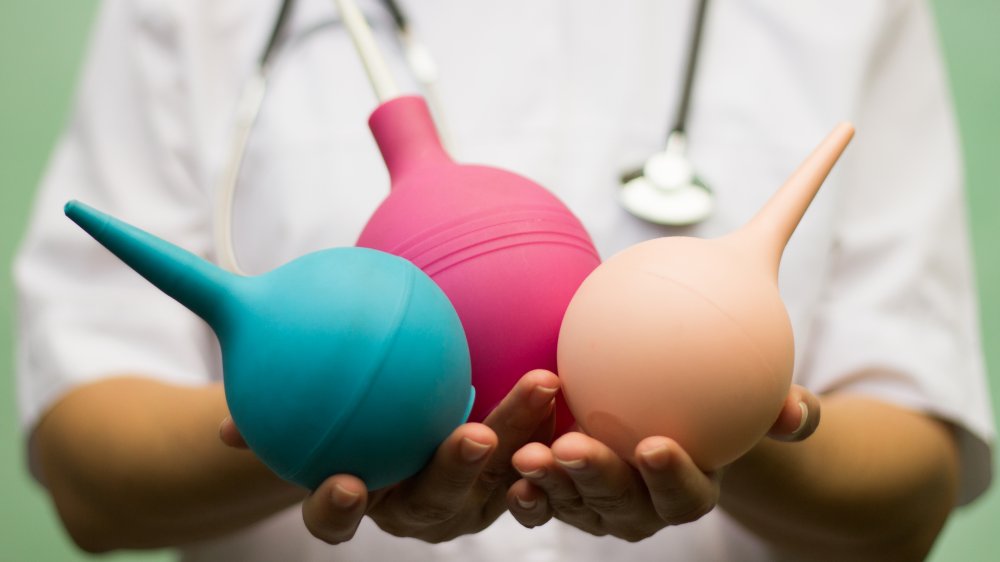
Douching is an effective form of birth control
Let's cut straight to the chase here: Douching is a bad idea all around. For anyone who doesn't know, douching refers to the process of shooting liquid into your vagina using a tool called a douche. The idea is to "cleanse" the inside of your vagina, although that isn't really what happens. According to Johns Hopkins Medicine, "The vagina has its own natural cleaning system that flushes out bacteria. The chemicals and perfumes in douches or feminine sprays don't help and can actually cause problems like allergic reactions, irritation, or infections."
Douching doesn't work as a form of birth control. In fact, according to Johns Hopkins Medicine, sperm swim very quickly, and when a man ejaculates inside a woman's vagina, thousands of sperm could reach the uterus before the woman even has a chance to douche. What's more, the pressure of the douching liquid squirting into a woman's vagina can actually push the sperm along, helping them reach the uterus even faster. Hopefully, all of this is enough to convince you to throw away your douche if you have one, or to never buy one if you don't.
You don't need to use condoms during your period
The myth that you can't get pregnant while you're on your period isn't totally out of nowhere, but it's not completely true either. According to WebMD, the odds of getting pregnant are lower on your period, although conception isn't impossible.
Here's how your menstrual cycle works, according to the Office on Women's Health. Starting on Day 1 of the cycle, you menstruate (AKA, you get your period) for four to eight days. Around Day 11, your estrogen levels peak. On Day 14, you ovulate, meaning your ovaries release an egg. This is when your egg is ready to be fertilized by sperm. An egg will travel down to the uterus in Days 15 through 24; if it has been fertilized by sperm, it will attach to the lining of the uterus, and pregnancy will begin.
What does that have to do with anything? Well, that schedule isn't exact, and sperm can live in the reproductive system for three to five days. So if you're having unprotected sex at the end of your period, there's a chance that the ejaculated sperm will still be alive when you start to ovulate.
Hormonal birth control affects future fertility
It's not crazy to worry that intentionally using birth control to make yourself temporarily infertile might affect your fertility even after you've gone off the birth control. Luckily, it doesn't actually work that way. While it might take a few months after stopping birth control for you start ovulating again, there's no significant risk of infertility, according to Everyday Health.
"Once ovulation resumes, you can become pregnant," Dr. Andrea S. Fernandez, an OB-GYN at Wake Forest University School of Medicine, told Everyday Health. "About 50 percent of women will ovulate in their first month after stopping birth control pills. Most women will begin to ovulate in the first three to six months after stopping the Pill." So, there's no need to worry that taking birth control now will negatively impact your ability to conceive later. You should just expect to wait a few months after stopping birth control to return to your regular menstrual and ovulation cycle.
Pulling out is just as effective as using a condom
Most of a man's sperm is released when he ejaculates upon having an orgasm, but some sperm can get released before a man (or the woman he is having sex with) realizes it's happening. The "pulling out" method — when a man literally pulls his penis out of a woman's vagina just before ejaculating — is only about 75 percent effective, according to Everyday Health.
Put another way, one in four women who use "pulling out" as their only form of birth control will get pregnant. Those aren't good odds at all! Instead of relying on this method that's very prone to user error, opt for a more effective form of birth control. If you're open to hormonal birth control, talk to your OB-GYN about starting the pill, the NuvaRing, the Depo-Provera shot, or getting a hormonal IUD placed. If you'd rather opt for a non-hormonal, over-the-counter form of birth control, male condoms are an accessible option that are effective in preventing pregnancy 98 percent of the time, according to Planned Parenthood.
All forms of birth control protect against STDs
Wouldn't it be great if a pill, a shot, or an IUD could prevent against sexually transmitted diseases (STDs) and sexually transmitted infections (STIs), as well as protecting against pregnancy? Unfortunately, no form of hormonal birth control has the power to do that.
In fact, only male condoms made of latex have been proven to reduce the spread of STDs and STIs. According to the National Institute of Child Health and Human Development, female condoms made of latex likely also reduce the spread of STDs and STIs, although their effectiveness has not yet been studied because they're relatively new. Natural or lambskin condoms are not an effective way to reduce the spread of STDs and STIs, however, since there are tiny pores in these materials that can allow viruses to spread.
Of course, hormonal birth control doesn't slow the spread of STDs and STIs, either, because partners still exchange fluids, which is what can lead to the spread of infection. If you have multiple partners, it's always a good idea to use condoms to lower your chances of contracting an STD or STI, even if you're on another form of hormonal birth control.
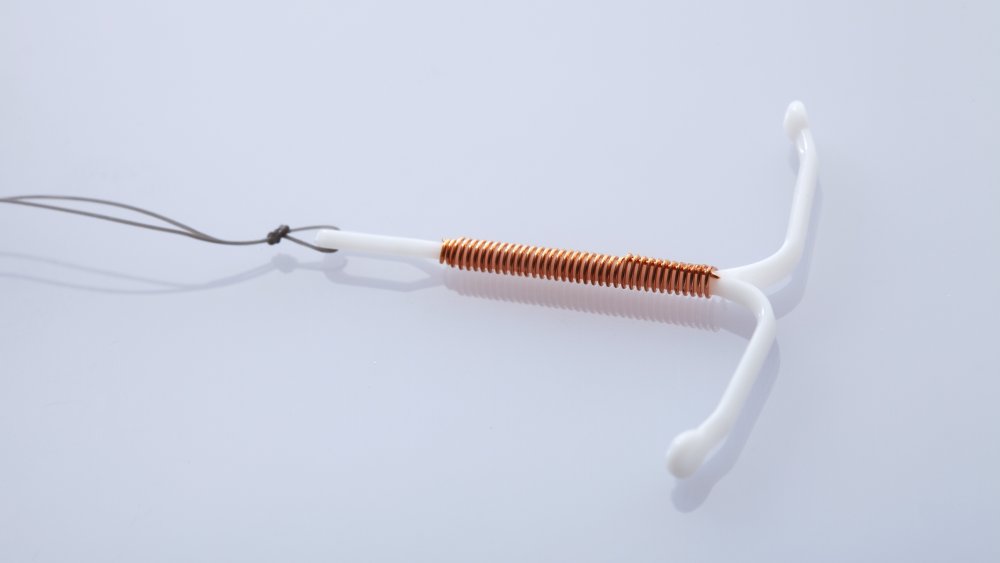
Copper IUDs are a dangerous form of birth control
Copper IUDs are an extremely effective non-hormonal form of birth control. Instead of releasing hormones into your body to prevent ovulation, the copper from the IUD transforms your uterus into a hostile environment for sperm and prevents egg fertilization (via Cleveland Clinic). Like the hormonal IUD, the copper IUD is over 99 percent effective in preventing pregnancy. The copper IUD is great for someone who doesn't want to alter their natural hormone levels. Another benefit is that while a hormonal IUD needs to be replaced at least every three to seven years, depending on the specific IUD, a copper IUD will last for 10 years.
So, why are some people afraid of the copper IUD? There is a very, very small risk of an IUD moving through your uterine wall and into your abdominal area after insertion, but that only happens in 0.01 percent of cases (via Cleveland Clinic). It's also not recommended for women with extremely heavy periods, since it's possible that a copper IUD can increase bleeding and make cramping slightly more severe, according to the Mayo Clinic. However, these complications are not likely, and experts agree that the copper IUD is safe and effective for most women.
Your partner can feel your IUD during sex
Yes, the IUD is a physical device that gets inserted through your vagina, past your cervix, and into your uterus. No, a man's penis doesn't reach that far in.
However, it's not impossible that your partner might feel your IUD strings with his penis during sex. The strings hang down from the IUD and are about three to four centimeters long. In your body, they either soften, curl around your cervix, or are physically tucked behind your cervix, according to Cosmopolitan. "It's incredibly rare that your partner would ever feel the IUD strings," Dr. Rachna Vanjani, an OB-GYN in the San Francisco Bay Area, told the magazine. "I've been putting IUDs in for six years. I've put in hundreds of IUDs, maybe even thousands. Very rarely do I have complaints — maybe one to two patients in my career."
If your partner complains that he can feel your IUD strings with his penis, Vanjani said that this can happen if your IUD strings were cut too short to wrap around your cervix, and your OB-GYN can solve the problem in office by cutting the strings even shorter.
Hormonal birth control causes cancer
While there's some evidence supporting the myth that hormonal birth control might increase your cancer risk, the truth is complicated. According to Medical News Today, it's true that hormonal birth control may slightly elevate your risk of some cancers, specifically breast and cervical cancer.
However, most of this increased risk was found in women who used a triphasic pill, which is a type of oral birth control pill that delivers three different hormone doses throughout a woman's cycle. Asking your OB-GYN to prescribe a different type of pill — of which there are many — or instead opting for another form of hormonal birth control like an IUD might eliminate this risk (via Medical News Today).
There's also some good news here. Research shows that while hormonal birth control might slightly raise your risk of breast and cervical cancer, it also shows that hormonal birth control might slightly reduce your risk of endometrial cancer, ovarian cancer, and colorectal cancer. Like we said, it's complicated. If cancer risk is something you're really worried about, talk to your OB-GYN about the pros and cons of various forms of birth control.
You have to take Plan B within 24 hours
Plan B is a form of emergency contraception that temporarily stops the release of an egg from the ovary by introducing levonorgestrel, a synthetic form of the hormone progestin, into your body (via Plan B). It should never be used as regular birth control and should only be used after unprotected sex.
While some people think that Plan B must be taken within 24 hours of having unprotected sex, this isn't exactly true. If you take Plan B within 72 hours of unprotected sex, it is 87 percent effective in preventing pregnancy, according to Web MD.
However, Plan B is significantly more effective when taken within 24 hours of having unprotected sex, since it works by temporarily stopping the release of an egg from your ovaries in order to prevent fertilization and implantation on the uterine lining, AKA pregnancy. Why? Because it's possible that your ovaries will release an egg to be fertilized before you take Plan B. The longer you wait to take the Plan B pill, the more time your reproductive system has to release an egg to be fertilized by your partner's sperm.
Plan B is the same as having an abortion
Plan B, which used to be known as the morning-after pill, is a form of emergency contraception that can be used for up to 72 hours after unprotected sex, in order to prevent pregnancy. Essentially, Plan B contains levonorgestrel, a synthetic form of the hormone progestin. This temporarily stops the release of an egg from the ovary, in order to prevent that egg from being fertilized and attaching to your uterus (via Plan B).
This is not the same thing as having an abortion. While an abortion actively terminates an existing pregnancy (after an egg has been fertilized by sperm and attaches itself to the uterus), Plan B simply prevents a pregnancy from happening, which is why it's classified as a form of contraception (via Mayo Clinic). This is why it's important to take Plan B within the prescribed window of 72 hours after having unprotected sex, and why it's more effective the sooner you take it.
You have to take your birth control pill at exactly the same time every day
If you've ever been on a birth control pill or talked to your OB-GYN about starting one, you've probably been told that it's important to take your pill at the same time every day. That's good advice. Most forms of birth control pills work by releasing the hormones estrogen and progestin into your body, in order to prevent ovulation and thicken your cervical walls, essentially tricking your body into thinking it's already pregnant. So, what happens if you skip a day of birth control? Well, while you should take the Pill at exactly the same time every day, taking it within 24 hours of your previous pill will still be pretty effective, and you shouldn't sweat it if you miss your time window by a few minutes or an hour, according to Vice.
However, some (far less common) pills are what's known as a "mini pill" and only contain the hormone progestin. These don't always prevent ovulation, but do thicken your cervical mucus. However, there's only enough hormone in each pill to last for 24 hours, so it's actually important to stick to a strict schedule if you're on this type of pill (via Vice).