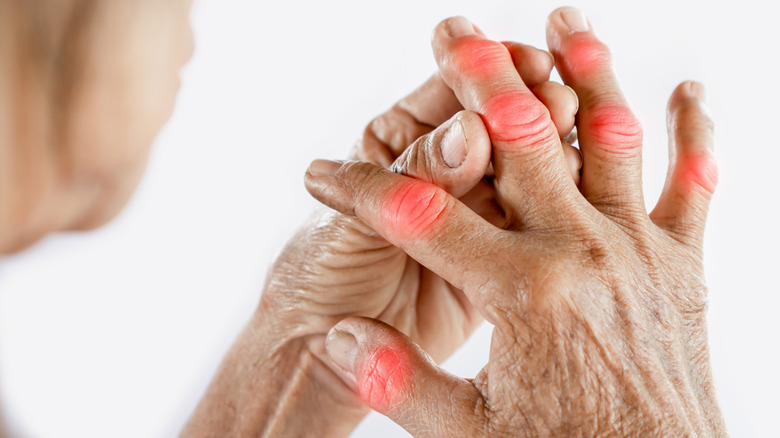
The Real Difference Between Psoriatic Arthritis And Rheumatoid Arthritis
People often attribute their creaky and achy joints to "arthritis," but arthritis is not a simple, one-size-fits-all condition. According to the Centers for Disease Control and Prevention (CDC), there are well over 100 different forms of arthritis affecting the joints and connective tissues. Common forms include osteoarthritis, rheumatoid arthritis (RA), and psoriatic arthritis (PsA), to name just a few. While PsA and RA are both inflammatory forms of the disease and share several similarities, their differences are important and can dictate severity of disease along with proper diagnosis and management (via VeryWell Health).
The majority of people with RA are diagnosed between 30 and 50 years of age, and women account for approximately 75% of cases according to the American College of Rheumatology (ACR). While PsA also tends to be initially diagnosed within the same age range as RA, it is noted that men and woman tend to be more equally at risk for its development (via ACR).
Perhaps one of the most striking differences between the two forms of arthritis is how the diseases impact the skin. People with rheumatoid arthritis do not commonly have associated skin rashes or lesions. In contrast, 15 to 20% of people with psoriasis go on to develop psoriatic arthritis. Of note, approximately 85% of people with psoriatic arthritis will be affected by psoriatic lesions of the scalp, skin, and/or nails at some point in their disease. There are also some other key differences.
Additional notable differences between psoriatic and rheumatoid arthritis
In psoriatic arthritis, the affected joints usually present in an asymmetric pattern, whereas with RA the pattern is typically symmetrical (via Rheumatic and Musculoskeletal Diseases). RA tends to affect the knuckles and wrist, while PsA tends to affect the small joints of the hands, along with the spine. The swelling seen in PsA is also very different than that of RA. In PsA, often times an entire finger will be swollen, a symptom commonly referred to as dactylitis or "sausage digit" for, well, the finger's sausage-like appearance (via ACR). In RA, usually only the affected joint itself is swollen, sparing other parts of the digit.
The two diseases also differ on a genetic level as well. There is no specific blood test for PsA in particular, however the presence of a HLA-B27 genetic marker is seen in people with spondyloarthropathies, of which PsA is one (via Rheumatic and Musculoskeletal Diseases). This genetic marker is not present in people with RA, who instead tend to have detectable levels of the autoantibodies known as rheumatoid factor (RF) and anti-cyclic citrullinated peptide (CCP) (via VeryWell Health).
Diagnosis of both diseases can be made by a rheumatologist through a thorough history and physical exam, X-ray imaging, and pertinent laboratory testing. While initial treatments for both typically involve corticosteroids, long-term therapies need to be tailored to the individual's disease severity and prognosis.