Inflammation Explained: Causes, Symptoms, And Treatments
There are many things that happen in your body in response to an injury or illness that you likely never knew occurred. Inflammation is sometimes one of those processes. For example, if you get a cut on your finger, it might be so small that it doesn't hurt. However, inside your body, inflammation is causing your white blood cells to ramp up production and prevent bacteria from getting into the cut. However, inflammation can also be incredibly painful, like in people living with autoimmune disorders where the immune system flares up when it doesn't need to (via WebMD).
In most cases, inflammation is a helpful process that lets us know something is wrong. But chronic inflammation can do significant damage to the body. According to a paper published in Nature Medicine, chronic inflammation leads to several other conditions, like cancer, diabetes, and chronic kidney disease. If you consider the mortality rates of inflammation-related conditions, they make up about half of all deaths.
Understanding why inflammation happens and how to control it can help those prone to inflammation feel relief and avoid further damage. Let's take a look at important things to know about inflammation and its role in your body.
Chronic versus acute inflammation
The two primary types of inflammation are acute and chronic. Acute inflammation is short term, so it might only cause pain for a day, week, or month. In other words, you don't live with acute inflammation every day. Instead, it happens when you have an injury or an illness that causes your immune system to react to fight off bacteria. You'll typically notice pain, redness, and swelling if you have acute inflammation, while hotness and loss of movement or function can also occur in some cases (per Medical News Today).
In contrast, people with chronic inflammation live with the condition long term. This type can last weeks, months, years, or a lifetime. Healthline states that other conditions and irritants, like chemical exposure, chronic stress, and autoimmune disorders, can cause chronic inflammation. If acute inflammation goes untreated, it may also lead to chronic inflammation.
While chronic inflammation can be very problematic, acute inflammation is often helpful. In an interview with Harvard Health Publishing, associate professor of medicine at Harvard Medical School Robert H. Shmerling said, "Acute inflammation is how your body fights infections and helps speed up the healing process. In this way, inflammation is good because it protects the body." But chronic inflammation doesn't have the same rapport. According to Shmerling, those with chronic inflammation have heightened immune systems that always believe they're being threatened, which can take a toll on the body.
Inflammation can harm your digestive system
We often think of inflammation as the process that swells knees after a fall or causes joint pain from arthritis. But your digestive system can also meet inflammation in the form of inflammatory bowel disease (IBD).
According to Cleveland Clinic, this common condition affects as many as 3 million Americans. Although genetics and environmental influences can trigger IBD in some people, the immune system often plays a role. When food enters the body, the immune system could think it's something harmful, provoking inflammation as a way to protect the body.
IBD usually takes on one of two forms: Chron's disease and ulcerative colitis. Both conditions happen when chronic inflammation persists in the digestive tract. People with these conditions end up with symptoms like diarrhea, weight loss, bloody stools, and abdominal pain. Typically, doctors use a combination of diagnostic imaging and a colonoscopy or endoscopy in addition to a patient's record of symptoms to diagnose these inflammatory conditions (via Centers for Disease Control and Prevention).
Common and uncommon symptoms
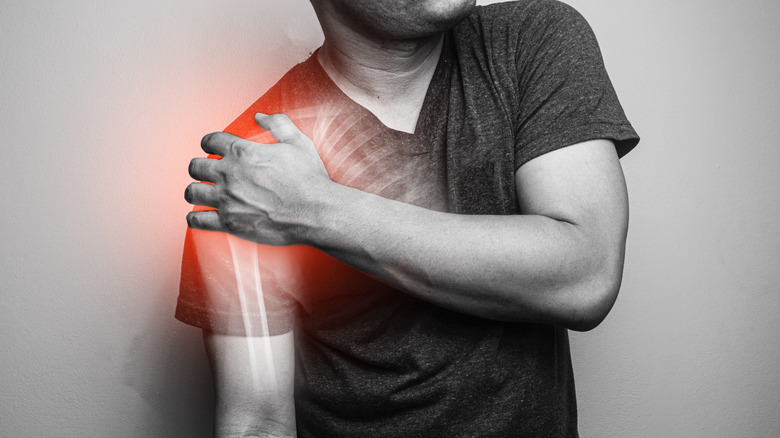
When inflammation happens, you can sometimes see it. Common visible symptoms of inflammation are redness and swelling. You might see these happen after a toddler learning to walk falls and bumps their head. Swelling and redness can develop quickly after a blow. Soon after an injury, pain usually occurs. And, joint pain might lead to joint stiffness as a result of inflammation (via WebMD).
These common symptoms aren't usually causes for concern unless they're causing you severe pain. But other uncommon symptoms of inflammation might warrant a trip to the doctor. According to WebMD, inflammation can also cause insulin resistance leading to high blood sugar levels, lower back pain, and diarrhea. Chronic inflammation may also leave you feeling fatigued, make your eyes feel dry, and cause muscle aches. Some people experience trouble balancing when inflammation revs up because the process can attack the body's nerve coatings and make it challenging for signals to move through the nervous system.
Inflammation can influence other conditions
Inflammation is often a helpful process that perks up the immune system to get it to do what it needs to do. But when inflammation is happening consistently, as is the case with chronic inflammation, people can develop conditions that can be harmful to the body.
One potential problem? Heart attacks. According to NPR, a person with high levels of low-density lipoprotein (LDL), or bad, cholesterol may experience chronic inflammatory responses to the cholesterol. This response can form blood clots that often lead to heart attacks. Other conditions influenced by inflammation include type 2 diabetes, depression, and Alzheimer's disease.
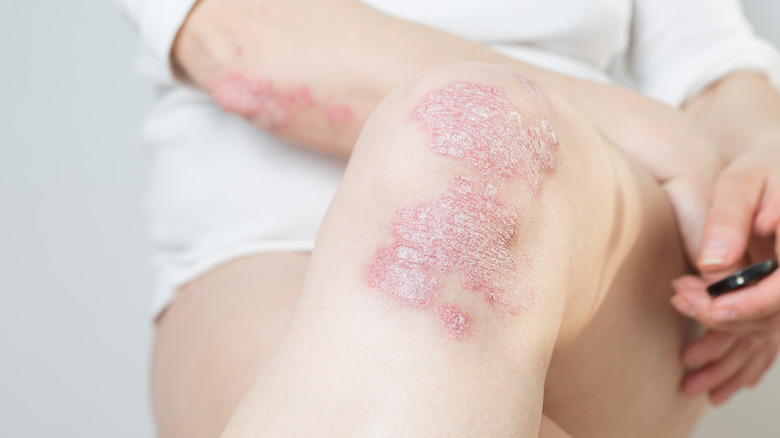
Arthritis can also be caused by inflammation. Inflammatory arthritis occurs with overactive immune systems that trigger chronic inflammation. Rheumatoid arthritis and psoriatic arthritis are two types influenced by inflammation that can severely impact a person's daily life. Doctors typically treat the symptoms and pain associated with these conditions with non-steroidal anti-inflammatory drugs (NSAIDs) and corticosteroids, but there are currently no cures (per Hospital for Special Surgery).
Smoking and drinking can cause inflammation
If you smoke or drink and experience some symptoms of inflammation, there's a chance that your habits could be contributing to your immune system's response. A 2016 study in the Journal of Leukocyte Biology explored the effects of nicotine consumption on the body, particularly how it causes inflammation by sparking neutrophil extracellular traps (NETs) to get to work. NETs are an important part of the immune system that develop protection against infection. Results show that nicotine induces NET formation and "this process in turn could contribute to smoking-related diseases by chronic inflammation," noted the study authors.
The significance of the impact of drinking alcohol on inflammation has some mixed results, but there does seem to be a relationship between the two. Rheumatologist Karen Costenbader told the Arthritis Foundation, "Moderate alcohol consumption reduces biomarkers of inflammation, including c-reactive protein (CRP), interleukin-6, and TNF-alpha receptor 2," meaning that occasional drinks could actually prevent inflammation. However, people who already experience inflammation could find that their symptoms worsen when drinking, and heavy drinking could trigger inflammatory responses, according to Ria Health.
Your diet can boost inflammatory responses
Do you notice a change in how you feel after eating certain foods? Some people experience problems like feeling fatigued, bloated, or even nauseous after eating processed or sugary foods. Some foods can cause inflammation, and when you eat them consistently enough, you could find yourself experiencing chronic inflammation.
Sugary foods are a leading culprit, especially if they have added sugars. Sugar gives you excess fructose, which is linked to fatty liver disease, obesity, and diabetes. High amounts of fructose in the body increase inflammation. Other inflammatory foods include refined carbohydrates, which have little fiber and nutritional value, and processed meats (via Healthline).
Registered dietitian Erin Coates tells Cleveland Clinic that trans fats can also be harmful. "Trans fats raise your bad cholesterol (LDL) levels and lower good cholesterol (HDL) levels. Both actions can increase your risk for developing heart disease, stroke and type 2 diabetes," Coats explained. According to Coates, reading nutrition labels is key to avoiding trans fats. Look for hydrogenated or partially hydrogenated oils in the ingredients label to know whether foods include trans fats.
Several foods can fight inflammation
We know that some foods can contribute to inflammation in the body, which means it's best to limit them or avoid them altogether. Dr. Frank Hu, professor of nutrition and epidemiology at the Harvard School of Public Health, told Harvard Health Publishing, "Inflammation is an important underlying mechanism for the development of [chronic] diseases." Additionally, Hu told the publication, "A healthy diet is beneficial not only for reducing the risk of chronic diseases, but also for improving mood and overall quality of life." Fortunately, several foods have anti-inflammatory effects, too, according to Hu. Fatty fish and leafy greens are among the best inflammation fighters.
Berries, like blackberries and blueberries, can also reduce or prevent inflammation. The small superfoods contain antioxidants that prevent the inflammation notorious for causing chronic diseases. Other foods to consider adding to your diet include avocados, tomatoes, and mushrooms. And, if you use oils to cook with, consider swapping to extra virgin olive oil. It's an excellent source of monounsaturated fats — a good kind of fat — and has links to reducing the risk of developing conditions like cancer and heart disease (via Healthline).
Exercise decreases inflammation
Exercise is a healthy habit that can lead to decreased inflammation. According to Medical News Today, a substance called TNF, or tumor necrosis factor, contributes to the changing and killing of cells. To do this, TNF increases inflammation in the body, so higher levels of TNF are associated with more inflammation. Research suggests that exercising can effectively decrease TNF and, therefore, inflammation.
A 2017 study published in Brain, Behavior, and Immunity looked at the effects that just 20 minutes of moderate exercise had on TNF levels. Researchers found that TNF "was suppressed by exercise with moderate to large effects." How? It boils down to how exercise boosts the immune system, in turn decreasing inflammatory responses.
Senior author of the study Suzi Hong explained to UC San Diego Health that exercise is not just for physical fitness but also for immunity. "Our study found one session of about 20 minutes of moderate treadmill exercise resulted in a five percent decrease in the number of stimulated immune cells producing TNF," said Hong. Hong also noted that workouts don't need to be intense to do the trick. A brisk walk can have great benefits.
Stress can be a factor
Are you feeling stressed? Your stress could be the cause of your inflammation. Although medical experts haven't yet found the exact reason why a relationship between stress and inflammation exists, it's clear that it's there. Chronic stress can especially wreak havoc on your overall health and immunity, according to Dr. Alka Gupta, an integrative health expert. Gupta told Everyday Health that participating in stress-reducing techniques, like deep breathing, lowers inflammation. Unfortunately, when stress is consistent, the pro-inflammatory response that's meant to help your immunity temporarily can linger, leading to chronic inflammation that damages the body.
A 2017 article in Frontiers in Immunity covers this issue in depth. The authors pointed out that several studies that found that chronic stress in early life and adulthood has ties to an increased risk of coronary heart disease. Stress also contributes significantly to insulin resistance, which is associated with diabetes, metabolic syndrome, and other inflammation-related conditions. Further evidence shows that stress induces or worsens cancer, depression, and other conditions through its inflammatory effects.
Yoga may combat inflammation
Constant stress can take a toll on your body when it leads to inflammation. Therefore, dealing with stress head-on is one of the best things you can do to prevent negative inflammatory responses that can cause other health problems. According to Harvard Health Publishing, yoga, well-known as a stress-relieving exercise, can reduce chronic, low-grade inflammation. Specifically, research has pointed to yoga reducing inflammation when practiced regularly as part of a healthy lifestyle.
A 2015 study also looked at the effects of yoga on TNF, which sparks inflammation to strengthen the immune response. More than 200 people participated in the study, with 109 of them participating in yoga for one hour a day for five years. Blood tests that were taken before and after yoga consistently showed that TNF levels were lower in the yoga-performing group than those who didn't participate in yoga. Interestingly, strenuous exercise increased TNF levels in the body, indicating a heightened inflammatory response compared to the effects of yoga.
Weight gain could cause inflammation
Research has shown that when you gain weight, you may boost your body's inflammatory response. A study published in a 2019 issue of Metabolism Open looked at inflammation markers in more than 5,000 men and women. The researchers considered body mass index, waist circumference, and body fat percentage to gauge obesity over the seven-year study. At the end of the study period, these variables and inflammatory markers were reviewed again, and researchers found that inflammation decreased, on average, in those who lost weight.
According to EndocrineWeb, metabolic cells can cause chronic inflammation because obesity tricks them into thinking the immune system needs more power. Interestingly, inflammation may also affect how you lose weight. Systematic inflammation can increase insulin resistance, a common cause of type 2 diabetes and cardiovascular disease, increasing inflammation and harming metabolic processes. The result is a challenging cycle of weight gain causing inflammation and vice versa, which can be extremely difficult to break.
Testing for inflammation
If your doctor believes that inflammation is causing other symptoms or conditions, they may order one or more of the tests available to check for an inflammatory response. The most common test is the c-reactive protein (CRP) test. According to MedlinePlus, the liver makes c-reactive protein when inflammation exists in the body. Therefore, a simple blood test to check for this protein may indicate whether you have inflammation. Your doctor will typically use the result from the CRP test in addition to your symptoms and health history to decide if any further treatment is necessary.
In patients with an increased risk of heart disease, advanced inflammatory testing could be warranted. Quest Diagnostics explains that advanced inflammatory tests check for multiple inflammatory markers related to metabolic syndrome, diabetes, and other conditions that increase cardiovascular disease risk. Testing for fibrinogen and pro-inflammatory cytokines are other options for doctors to better understand how your immune system is handling inflammation (per StatPearls).
Treating with lifestyle changes
Many medical experts agree that making lifestyle changes can positively impact the immune system's response and potentially derail inflammation. According to Brigham and Women's Hospital, avoiding tobacco products, eating antioxidant-rich carbohydrates, and getting the right amount of sleep each night are helpful first steps. But the most important contributors to lowered inflammation are watching your intake of dietary fats, keeping your weight in check, and staying active.
Dr. Travis Stork, former ER physician and host of "The Doctors," spoke with Parade about chronic pain he lived with for years. Stork admitted that starting an anti-inflammatory diet has been one of the best things he's done to improve his condition. "I've always eaten for being lean but [an anti-inflammatory diet] really changed everything in terms of how I eat," said Stork. "Everything I eat now serves a purpose. And what I mean by that is the purpose is no longer, 'Hey, I want to maximize my lean muscle.' Really now it's all about maximizing my antioxidants." Stork said that he's done that by switching to mostly a plant-based diet.
Treatment with medications
If switching to a healthier diet and lifestyle and avoiding inflammatory foods don't do the trick, your doctor might suggest trying medications to curb inflammation. You might start with over-the-counter medications, which may help acute inflammation and mild cases of chronic inflammation. The most common drugs to use for inflammation are NSAIDs, like ibuprofen and naproxen. NSAIDs block prostaglandins, which make inflammation more painful by causing more sensitivity in your nerve endings (per Healthline).
For more severe cases of inflammation, a doctor might opt for prescription NSAIDs. These are the same drugs you'd find over the counter but with higher dosages that can inhibit pain more effectively. These are typically prescribed in cases of rheumatoid arthritis and osteoarthritis (via Cleveland Clinic). In severe cases, corticosteroids may also be prescribed. These drugs decrease the immune system response to, in turn, prevent inflammation. However, they also tend to have more side effects than NSAIDs, like weight gain, osteoporosis, and muscle weakness (per Cleveland Clinic).