Everything You Need To Know Before Starting IVF
In vitro fertilization, often called IVF, is a series of procedures that helps people who have difficulties getting pregnant, according to MedlinePlus. It falls under a group of procedures called assisted reproductive technology. During IVF, eggs are taken from one person and sperm is taken from another. The eggs and sperm are then combined in a laboratory to produce an embryo. That embryo is matured until it is stable enough to be transferred into a uterus so it can develop into a fetus.
Fertilization and embryo creation usually occurs within the body of a person with female reproductive organs. Eggs are released during ovulation, and when they encounter sperm — usually introduced into the body through sexual intercourse, but sometimes introduced via medical procedure — the egg becomes fertilized. It travels to the uterus and implants in the uterine lining to grow.
However, this process doesn't always go smoothly. For some couples, medical problems interfere with the fertilization process. IVF offers another way for these couples to get pregnant by recreating the fertilization and embryo maturation process in a lab setting. It also offers couples who both have female reproductive organs, people without partners, and people using a surrogate a way to have a biological child. According to the Mayo Clinic, IVF is "the most effective form of assisted reproductive technology."
IUI is different from IVF
Intrauterine insemination, often called IUI, is another type of assisted reproductive technology (per Northwestern Medicine). Like IVF, IUI assists the fertilization process that results in conception. However, IUI achieves this by assisting fertilization within the body of a person with female reproductive organs.
During IUI, sperm from a parent or donor is inserted directly into the uterus while eggs are being released during ovulation. This increases the likelihood that a sperm and egg will meet and complete fertilization. Before the sperm is inserted into the uterus, fertility specialists examine the sample and identify the most motile sperm, the ones that are the "strongest swimmers." Only these sperm are inserted into the uterus, increasing the chances that they will find an egg to fertilize.
Some people prefer intrauterine insemination over in vitro fertilization because it's more in line with how the body normally gets pregnant. It's also less invasive than IVF because eggs don't have to be harvested to achieve fertilization outside the body. Many people who have trouble getting pregnant or can't get pregnant on their own start with IUI and if unsuccessful, they move on to IVF.
Who gets IVF?
People try in vitro fertilization for a lot of different reasons, but the overarching reason is that they can't get pregnant on their own. According to the American Pregnancy Association, common medical issues that lead people to IVF include blocked or damaged fallopian tubes, ovarian failure, ovulation disorders, low sperm count, decreased sperm motility, uterine fibroids, previous fallopian tube removal, and genetic diseases.
Additionally, lesbian, gay, bisexual, and trans couples may use in vitro fertilization to conceive, per Verywell Family. One or both of the intended parents will donate reproductive material — either sperm or eggs — and the other reproductive material needed to complete the process is provided by a donor. Sometimes that donor is someone the intended parents know and sometimes it's an anonymous person. The genetic materials are mixed and matured in a lab and then transferred either to a gestational carrier, someone who is carrying the baby for the couple, or one of the intended parents.
When each of the intended parents has a uterus, they may opt to go through a process called reciprocal IVF (Verywell Family). One parent donates their eggs to be fertilized and the other parent has the embryos implanted into their uterus. This way the child is biologically related to one parent while the other parent gets to give birth.
Preparation
In vitro fertilization is a complex process that involves several phases, according to the Mayo Clinic. It starts with the preparation phase. The Colorado Center for Reproductive Medicine (CCRM) suggests that focusing on healthy habits is the very first step in IVF. They recommend that you eat a variety of nutritionally dense foods and start taking a prenatal vitamin. They also suggest you stop drinking alcohol, smoking, taking recreational drugs, and reducing your caffeine intake. If you can, you might even want to kick the caffeine habit entirely as you prepare for IVF.
CCRM states that taking care of yourself emotionally is an important part of the preparation phase as well. IVF can be incredibly stressful and, unfortunately, high stress levels can make the procedures less effective. Caring for yourself emotionally, perhaps by going to support groups or yoga classes, will help prepare your body and mind for IVF.
According to the Mayo Clinic, testing is a major part of the preparation phase as well. People whose eggs will be harvested undergo testing to determine the amount and quality of the available eggs. The person who intends to carry the baby will have a uterine examination performed to check the quality of the uterine lining. The person donating the sperm will provide a sperm sample for testing. Additionally, both partners will be tested for infectious diseases like HIV. If everything is satisfactory, they'll move on to the next phase.
Ovulation
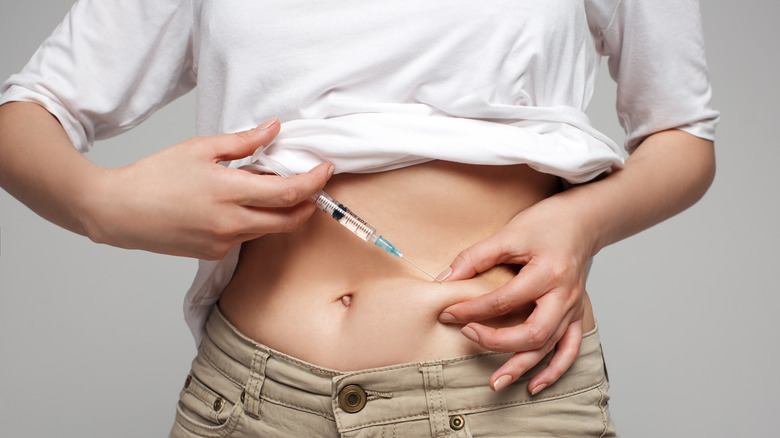
The point of the ovulation phase is to get the egg donor's ovaries to produce as many eggs as possible during a single ovulation cycle. According to the University of Iowa Hospital and Clinics, this is achieved by giving the egg donor regular doses of synthetic hormones. These hormones are administered via daily shots, which can be done at home either by the egg donor or a partner.
Egg donors may be advised to take oral contraceptives (birth control pills) prior to beginning hormone injections for IVF. "Taking birth control pills before an ovarian stimulation cycle may help the ovaries respond better to the stimulation medications," according to Fertility Specialists of Texas. It also makes the ovulation window easier to predict.
Before the egg donor starts taking synthetic hormones, they'll also need a transvaginal ultrasound to confirm that the ovaries are healthy. Once the egg donor starts taking the hormone shots daily, the ovulation process will be carefully monitored by their doctor. Regular blood tests will be done to check estrogen levels and transvaginal ultrasounds will be performed to see how the eggs are developing in the ovaries. If things aren't progressing as expected, the doctor may change the combination of the hormones being administered. Once two or more eggs develop and reach the right size, the donor will be ready for the egg retrieval phase.
Egg retrieval
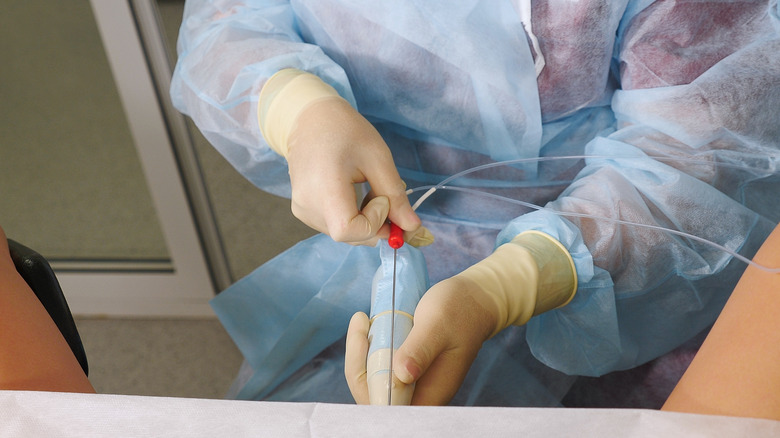
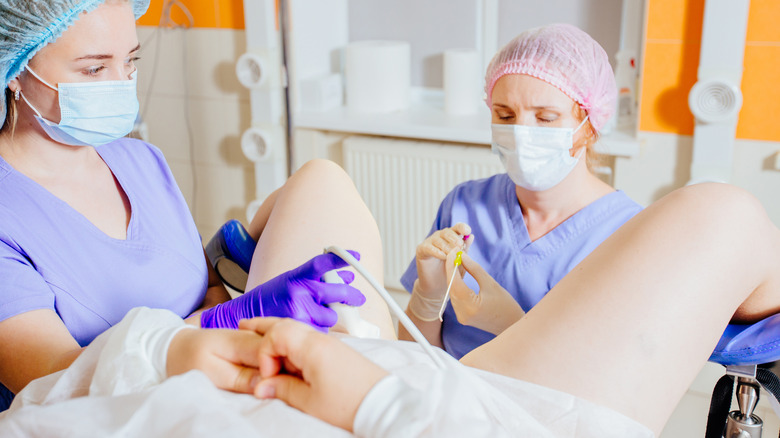
Now that the eggs are ready, it's time to get them out of the ovaries so they can be fertilized in the lab. Dr. Lauren Roth, a board-certified OB-GYN and reproductive endocrinology and infertility specialist, detailed the process for Parents magazine. The expert explained that the egg donor is given a mild sedative via IV before the procedure starts. Once the egg donor is asleep, they'll be positioned on the exam table and their legs will be placed in the stirrups, similar to a regular pelvic exam. A vaginal ultrasound is performed to visualize the ovaries and the eggs that will be retrieved.
Next, the doctor inserts a thin, hollow needle through the vaginal wall and into the ovary. "The needles go into each ovarian follicle and use gentle suction to pull out the fluid and the egg that comes with it. Doctors give this fluid to the embryologist, who can immediately tell how many eggs they're getting," Roth revealed.
The egg donor is then transferred to a recovery room. When they wake up, they'll spend an hour or two in the recovery room and then head home to rest. They'll need someone to drive them home since the effects of the sedative may take a while to wear off. After the procedure, some people experience pain, bloating, spotting, and/or constipation. At-home remedies should be sufficient to relieve these symptoms.
Sperm retrieval
Once the eggs have been retrieved, the other half of the genetic material needs to be procured. According to the Society for Assisted Reproductive Technology, the most common way that sperm is retrieved for IVF is through masturbation. If one of the intended parents has male reproductive organs, they can provide a sample the same day as the egg retrieval is performed, or they can provide a sample in advance and have it frozen. If neither partner has male reproductive organs, then the sperm sample will need to be procured by a donor.
However, if the person providing the sperm has a medical issue that makes it difficult to provide a sperm sample via masturbation, other methods will have to be employed. According to Johns Hopkins, several methods can be used including testicular sperm aspiration (TESA), percutaneous Epididymal Sperm Aspiration (PESA), testicular sperm extraction (TESE), Microepididymal Sperm Aspiration (MESA), and Microdissection TESE (microTESE).
Both TESA and PESA are performed under local anesthesia at a doctor's office. A small, hollow needle is inserted into the testicles and sperm are pulled into the needle. TESE, MESA, and microTESE are more invasive procedures, as they all involve retrieving sperm through small incisions made on the testicles.
Fertilization and embryo maturation
Once the eggs and the sperm have been retrieved, the medical team has everything they need to make an embryo. However, they're not ready to create that embryo just yet.
According to Boston IVF, the first step in the fertilization and embryo maturation phase is determining which eggs to use for the fertilization process. Experts examine all the eggs retrieved and determine which ones are of the highest quality. Higher-quality eggs are more likely to produce a healthy embryo when fertilized, so only the best eggs are chosen for the fertilization process.
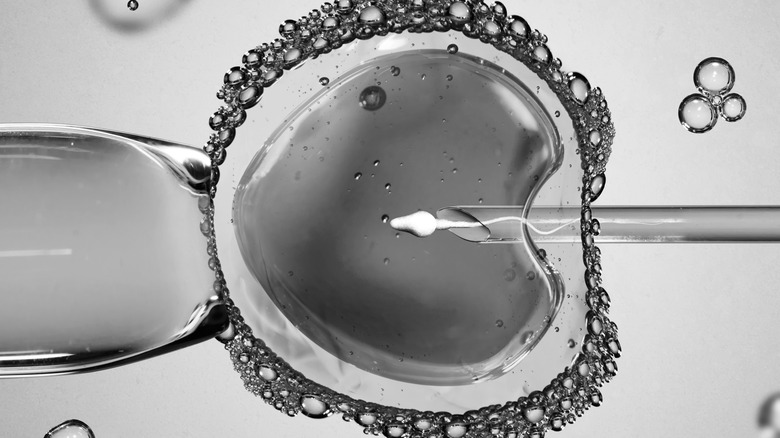
Those eggs are mixed with the sperm. Usually, the sperm will enter the egg to fertilize it on its own, per Stanford Children's Hospital. However, if there are issues with this process, the doctors can use a method called intracytoplasmatic sperm injection (ICSI) to insert the sperm directly into the eggs.
Once the eggs are successfully fertilized, they will begin to develop into embryos. The embryos are placed in incubators and monitored by the medical team as they develop. Three days after fertilization, the medical team has a good idea of which embryos have developed enough and will be strong enough to be transferred into the uterus. Once those embryos are identified, they are incubated for two to three more days to mature before being transferred.
Embryo transfer
It's time to transfer the embryos into the uterus, where they'll hopefully implant in the uterine lining. According to Medical News Today, the embryo transfer is actually a fairly simple procedure that's comparable to getting a Pap smear.
The parent that will be carrying the baby gets on the exam table and puts their feet in the stirrups, as they would for a vaginal exam. The doctor inserts a speculum into the vagina to give a clear view of the cervix. The doctor will then use an ultrasound wand on the person's lower abdomen so they can visualize the uterus. Once the doctor has a clear picture, they'll guide a small tube into the vagina, through the cervix and into the uterus. According to the Mayo Clinic, the embryos and a small amount of fluid will be placed into a syringe. That syringe is then inserted into the tube. When the plunger is pressed, the embryos and the fluid move through the tube into the uterus.
For most people, the embryo transfer procedure is not painful. The procedure may be performed with or without a mild sedative. Some people experience abdominal cramping, similar to period cramps, during the procedure.
After the embryo transfer, the intended birthing parent should head home to get some rest. Normal side effects are similar to those that some experience after egg retrieval — some mild spotting or vaginal bleeding, bloating, cramps, and constipation. Some people also experience breast tenderness because of high estrogen levels (via Mayo Clinic).
Waiting for the results
After the embryo transfer, there's nothing to do but wait to see if one or more of the embryos implants in the uterus. According to New York University Lagone Health, the embryo or embryos won't completely implant until about five days after the embryo transfer. Then it will take an additional four to five days for levels of human chorionic gonadotropin (hCG), the hormone that signals pregnancy, are high enough to be detected by a blood test.
According to Healthline, self-care is incredibly important during this time. The wait to find out if you're pregnant can bring up a lot of feelings, so it's important to be gentle with yourself during this time. It's also important to be vigilant about taking your medications. Continue to take a folic acid supplement every day, as it is crucial for the developing embryo. Some people will also need to continue to take synthetic hormones after the embryo transfer to help the process along.
You should also take it easy in the bedroom while you wait for the results of your embryo transfer. Research suggests that the uterine contractions that sometimes happen as a result of sex may make it harder for the embryo to implant in the uterine lining (via Healthline). So, keep the bedroom PG for at least a couple of weeks, or until you have the results of your pregnancy test.
Success rates
Though in vitro fertilization is the most effective form of assisted reproductive technology, the likelihood of having a baby from IVF depends on several factors. According to statistics from the Society for Assisted Reproductive Technology (SART), age is the most significant factor in whether or not IVF will result in a live birth. The success rates are much higher for people under 35 and drop dramatically after age 40. People over 40 have a better chance of success if they use donor eggs instead of their own eggs.
Success rates are higher for people who undergo multiple cycles. SART's statistics indicate that many people need to go through multiple egg retrievals and embryo transfers before having a child. One study found that success rates remained in the 20 to 35% range for the first four cycles of IVF. Of the people who underwent six or more cycles, the success rate was over 65%. However, in vitro fertilization is expensive and can be very emotionally draining, per Verywell Health. Many people choose not to go through more than two or three cycles.
Other factors like weight, height, the number of times the person undergoing the procedure has been pregnant, the number of live births they've had in the past, and the reasons for their infertility can also impact the effectiveness of IVF (via Verywell Health). Because so many factors go into successful results, it's hard to predict whether IVF will work for you.
Risks
According to MedlinePlus, the biggest risks associated with IVF are emotional rather than physical. Since IVF involves a huge amount of time, emotional energy, and money, people or couples undergoing the treatments can suffer from depression and stress.
Each of the phases does come with some physical risks as well. During the ovulation stimulation phase, the egg donor or intended parent takes a lot of synthetic hormones. These can cause symptoms similar to menstrual symptoms, including abdominal pain, bloating, headaches, mood swings. Rarely, the hormones cause a condition called ovarian hyperstimulation syndrome (OHSS), which causes fluid to build up in the chest and the abdomen. Symptoms include nausea, vomiting, shortness of breath, abdominal pain, bloating, and rapid weight gain. Most cases are mild but some require hospitalization.
During the egg retrieval process, there's a small risk that the organs surrounding the ovaries could be damaged, according to the American Society for Reproductive Medicine. There's also a small chance of pelvic infection after the procedure. Rarely, these infections are severe enough to require hospitalization. Additionally, IVF increases the chance of a multiple pregnancy, which can cause pregnancy complications. IVF also carries a small risk for ectopic pregnancy, according to the Mayo Clinic.
Caring for you during IVF
Because in vitro fertilization is such a taxing process, it's crucial that everyone involved puts self-care first during the entirety of the process. The Colorado Center for Reproductive Medicine (CCRM) suggests surrounding yourself with a support network including a therapist and your closest people. Even if you want to be private about your IVF journey, it helps to talk to someone just to get your feelings out. CCRM also suggests journaling as an effective way to get your feelings out. Developing a regular meditation practice is a great way to manage the stress involved in IVF. Remember to eat well, move your body in ways that feel good, and do what you can to get a good night's sleep.
The Society for Assisted Reproductive Technology (SART) suggests that extensive planning before and during the IVF process may help some people manage the stress. Planning for each decision so they don't have to be made in the moment or when difficulty arises, focusing on what they can and can't control about the IVF process, and identifying coping mechanisms that work for you and your partner, if you have one, can help make the process easier. However, SART also encourages patients to set a limit on the amount of time they spend talking about IVF in one sitting. Making time for other discussions and activities is important.
What if IVF doesn't result in pregnancy?
When a cycle of in vitro fertilization doesn't result in a pregnancy, it can be heartbreaking. However, according to Verywell Health, it takes 2.7 cycles, on average, for a successful pregnancy.
Dr. Roohi Jeelani, a reproductive endocrinologist and infertility specialist, told Self that there are several common reasons why a cycle of IVF might be unsuccessful. Sometimes adjustments to the process like changing the hormones used in the ovulation stimulation phase or changing the fertilization process can result in a more successful cycle. You can also do further testing to find out what issues might be preventing success.
If cycles of IVF don't work when using the intended parents' eggs and sperm, then donation may increase the chances of success. When donors are used, one of the intended parents can still carry the child themselves. If IVF treatments are successful and the intended parent's uterus is identified as the cause, using a gestational carrier may increase the chances of success. When using a gestational carrier, also called a surrogate, the intended parents can donate their own eggs and sperm or use donated eggs and/or sperm.
If another cycle of IVF is not feasible for whatever reason, many people choose to alternate routes. "Deciding to move on from fertility treatment is not giving up," Verywell Health explained. "Choosing a childfree life or pursuing options like adoption may be alternatives to continuing with treatments."