Mono Explained: Causes, Symptoms, And Treatments
As described by the Cleveland Clinic, mononucleosis, also called mono or "the kissing disease," is a contagious illness caused by the Epstein-Barr virus (EBV), a type of herpes virus. The infection occurs most often in teenagers and young adults, and is characterized by extreme fatigue, fever, and body aches. Children may be infected with mono as well, but they typically do not have symptoms.
While mono may persist for several weeks, it is not a serious illness for most people. Treatment is centered on symptom relief while the illness runs its course. EBV is most often spread via bodily fluids, particularly saliva. Thus, reports the NIH, the virus is typically introduced into the body through the throat and then spreads throughout the lymphatic system, where it preferentially targets immune cells called B-lymphocytes. In response to the infection, the body produces antibodies against the virus.
The term 'mono' is derived from the abnormally high numbers of mononuclear cells — a category of white blood cells (e.g., B-lymphocytes) with a single, round nucleus — found in the circulation of infected individuals, reports the Merck Manual. Once infected with EBV, an individual becomes a lifelong carrier of the virus, but in a dormant (inactive) form. Over time, EBV undergoes periodic shedding of viral particles in the saliva without causing symptoms, though potentially infecting others.
Prevalence of mono
According to the professional edition of the Merck Manual, infection with EBV that causes mono is highly prevalent. EBV infects half of all children under 5 years of age, while more than 90% of adults have serum antibodies for EBV, indicating past infection. The highest occurrence rate of EBV infection occurs between the ages of 15 and 24 (via the NIH). Due to previous exposure, clinical illness from mononucleosis is rare among adults. The rate of symptomatic infection in the United States is 30 times greater among white people compared to Black people. Since EBV does not usually cause noticeable symptoms when contracted in childhood, it's likely that Black people had earlier EBV exposure along with asymptomatic infection, thus accounting for the huge gap in infection rates.
A 2020 review of studies published in the Journal of Global Health noted that higher serum levels of EBV antibodies positively correlated with increasing distance from the equator. While this finding suggests that vitamin D may play a role in EBV infection, the researchers noted an absence of studies directly investigating a link between vitamin D and EBV antibodies.
Symptoms of mono
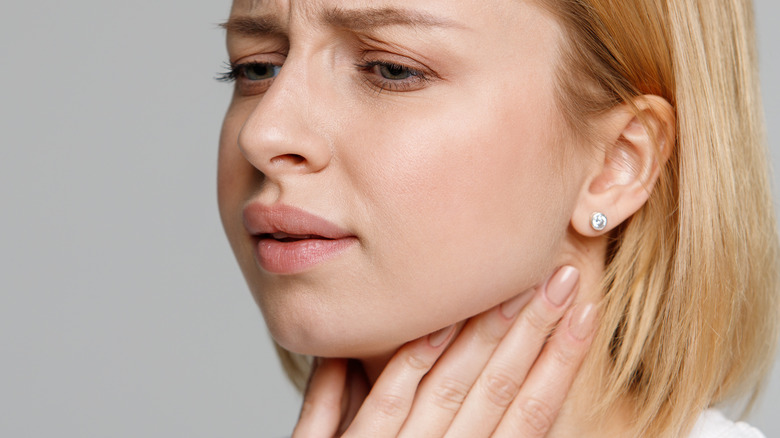
Symptoms of mono usually appear four to six weeks after infection with EBV occurs, reports the Mayo Clinic. They include fatigue, sore throat, fever, swollen lymph nodes in the neck and armpits, swollen tonsils, headache, skin rash, and a soft, swollen spleen. Per Medical News Today, the more common symptoms (e.g., fever, sore throat) usually improve after several days, but fatigue may persist for weeks or months.
Symptoms are more severe in teens and young adults, while young children are often asymptomatic or may experience mild symptoms that can be mistaken for a cold or flu. One possible explanation, suggested in a 2015 study in the journal Clinical & Translational Immunology, is that the immune system may not be primed by early childhood exposure to EBV, as is common in developed countries. Thus, teens and young adults may have less resistance against EBV infection. Findings from another study in a 2006 edition of the journal Age and Ageing confirm that adults over the age of 40 rarely acquire EBV. If they do get infected, older adults generally do not experience the typical triad of sore throat, swollen lymph nodes, and fever.
According to the Merck Manual, approximately half of people who get mono develop an enlarged spleen, though this causes few or no symptoms. Slight liver enlargement and swelling around the eyes may also occur. A rash is more commonly observed in people with mono who take penicillin derivatives such as ampicillin (per Clinical & Translational Immunology).
What are the causes and risk factors of mono?
As reported in Medical News Today, the vast majority of mono cases are caused by EBV. The virus is most commonly spread through saliva, though EBV may also be transmitted via breast milk, blood, or semen. An individual may contract mono from someone who is asymptomatic. In addition to EBV, other viruses and infections may trigger mono as well. These include cytomegalovirus (CMV), toxoplasmosis, HIV, rubella (German measles), adenovirus, and hepatitis A, B, or C.
Furthermore, a number of risk factors increase the odds of getting mono (via WebMD). For example, the virus can spread through any contact with the mouth and saliva such as kissing and sharing food, drinks, or eating utensils. If silverware is still moist, the virus is likely still contagious. Transmission of EBV may also occur via blood transfusions, organ transplants, and sexual contact. Per Medical News Today, an individual with a weakened immune system has a greater likelihood of developing symptoms upon first exposure to the virus. Immunocompromised people are also more susceptible to a second bout of mono caused by reactivation of EBV.
Complications of mono
Though rare, some complications of mono can be quite serious and even life-threatening, reports Medical News Today. For instance, an enlarged spleen may rupture from a jolt to the abdomen (e.g., in sports) causing sharp, sudden pain in the upper left abdomen, left shoulder, and left chest area. In addition, a ruptured spleen may cause low blood pressure and consequent confusion, dizziness, paleness, or loss of consciousness. As noted in a 2012 study in the International Journal of Surgery Case Reports, a ruptured spleen, whether spontaneous or trauma induced, is the most common cause of death in infectious mononucleosis.
According to the Merck Manual, mono may also cause rare neurologic complications such as encephalitis (brain inflammation), seizures, viral meningitis, and peripheral neuropathy. Blood-related complications (e.g., anemia and low platelet counts) and respiratory problems such as upper airway obstruction from swollen lymph nodes may occur as well. Liver problems include elevated levels of the liver enzyme ALT (observed in ~95% of mono patients), jaundice (yellowing of the skin and the whites of the eyes), and hepatitis. Other potential complications of mono, per Johns Hopkins Medicine, include kidney inflammation and inflammation of the heart muscle (myocarditis).
How is mono diagnosed?
To diagnose mono, a healthcare provider will initially assess signs and symptoms and perform a physical exam (via the Mayo Clinic). Signs of mono include swelling of the lymph nodes, tonsils, spleen, or liver. Blood tests may be performed to confirm or support a diagnosis. More white blood cells (lymphocytes) than normal, or unusual-looking lymphocytes, may support the diagnosis.
Per the Merck Manual, a monospot blood test that measures antibodies to EBV is used to diagnose mono. However, this test may not detect infection early in the illness, and thus may produce a negative result. The test can be repeated a week later when levels of heterophile antibodies rise; otherwise, a more highly sensitive EBV antibody test may be utilized as an alternative. These antibodies are specific for EBV and include IgM and IgG antibodies. IgM antibodies signify a recent primary EBV infection, and are no longer detectable after three months. In contrast, IgG antibodies indicate a past infection and do not disappear; they are detectable throughout a person's life.
Since some symptoms of mono resemble those of other viral and bacterial infections, a differential diagnosis may be performed to rule out other possible causes of the illness, per the NIH. These other infectious conditions include cytomegalovirus (CMV), human immunodeficiency virus (HIV), human herpesvirus type 6, hepatitis B, and Lyme disease. If a person with mono tests positive for IgG antibodies and negative for IgM, a different diagnosis may be considered (via the Merck Manual).
Medical treatment of mono
According to the Mayo Clinic, there are no available medications, including antiviral drugs, to treat mono per se. Antibiotics work against bacterial infections and are not indicated for viral infections. However, medications may be useful if an infected individual develops complications such as secondary infections. Antibiotics may be prescribed for some people with mono who develop bacterial infections such as strep throat, sinus infections, or tonsillitis. Antibiotic treatment has also been successfully used in a mono patient who was co-infected with a tick-borne illness, as documented in a 2021 study in the journal BMC Infectious Diseases. When antibiotics are indicated for people with mono, drugs in the penicillin family (e.g., amoxicillin) are not recommended, because may cause a rash in some individuals (via the Mayo Clinic).
An antiviral medication effectively treated two cases of acute hepatitis (liver inflammation) secondary to mono, per a study published in a 2009 edition of the Korean Journal of Internal Medicine. Corticosteroids may be prescribed to treat other complications such as blockage of the airways, anemia, and low platelet count (via the Merck Manual).
Lifestyle and home remedies for mono
Symptoms of mono can be managed with self-care and at-home remedies, reports Healthline. To avoid dehydration, people with mono should drink plenty of fluids such as water, herbal teas, soups, and broths. Liquids may help alleviate a sore throat or fever as well. A fever can also be treated with a wet towel compress, a cool bath, or cold food (e.g., ice cream). A sore throat can be further eased with salt water (or apple cider vinegar plus water) gargles.
Getting lots of rest is very important for a speedy recovery. Staying home also minimizes the spread of infection. Eating healthy foods and avoiding sugary, processed foods may also contribute to a faster recovery by boosting immune defenses against EBV. Foods rich in antioxidant and anti-inflammatory compounds are preferred. These include, in particular, salmon, olive oil, green tea, and green, leafy vegetables. Supplements such as omega-3 fatty acids and probiotics can help suppress inflammation and improve gut health, respectively.
Per the Cleveland Clinic, over-the-counter pain relievers can be used for fever, headaches, inflammation, and muscle aches. These medications include acetaminophen (e.g., Tylenol) and NSAIDs (nonsteroidal anti-inflammatory drugs) such as ibuprofen (like Advil) and naproxen (like Aleve). The Clinic also recommends avoiding intense exercise and contact sports for about one month, in order to prevent rupturing of the spleen.
Recurrence of mono
For the vast majority of people, mono usually occurs only once (per Medical News Today). EBV remains in the body forever, but in an inactive form. Anyone who gets infected with the virus develops antibodies to EBV, which confer lifelong immunity against recurrence. If the virus is reactivated, symptoms do not usually develop. Among those who do develop mono symptoms a second time, it may actually be due to the initial symptoms not being completely resolved, or a different condition exhibiting similar symptoms (like influenza).
Nevertheless, though uncommon, mono can still recur in some people. Reactivation of EBV (along with relapse of mono symptoms) occurs predominantly in individuals with an impaired immune system. In some cases, a person's immune cells may be battle-weary from dealing with other conditions (like cancer) and thus become overwhelmed. However, even people with a fully functional immune system can have a recurrence of mono, as reported in a case study in the World Journal of Clinical Cases.
According to a 2017 study in Frontiers in Immunology, in rare cases, individuals can contract chronic active EBV (CAEBV) disease, a dangerous form of mono that never resolves. Since CAEBV infection cannot be controlled, it can be fatal unless a blood stem cell transplantation — the only curative treatment — is performed. While the cause of CAEBV is unknown, genetics may have a role, since it occurs more frequently in Asia and South and Central America (and there is some evidence of an immune defect).
Associated conditions linked to EBV
The cause of mono, EBV, may increase the risk of developing some cancers, autoimmune disorders, schizophrenia, long Covid, and other health conditions (via Healthline). The American Cancer Society reports that people infected with EBV have a greater chance of developing stomach cancer, nasopharyngeal cancer (affecting the back of the nose), and some lymphomas such as Burkitt lymphoma and Hodgkin lymphoma. Africa and parts of Southeast Asia have a higher prevalence of cancers related to EBV. According to a 2011 study published in the Science Translational Medicine, approximately 200,000 new cases of cancer linked to EBV occur yearly around the world.
As reported in a 2018 study published in the journal Nature Genetics, children infected with EBV have a 50-fold greater risk of developing systemic lupus erythematosus (SLE), the most common form of the autoimmune disease lupus. The researchers describe a gene-environment interaction whereby EBV significantly alters the expression of genes associated with lupus, increasing disease risk. A similar gene-EBV interaction is implicated in other autoimmune disorders such as multiple sclerosis (MS), rheumatoid arthritis, inflammatory bowel disease, type 1 diabetes, juvenile idiopathic arthritis, and celiac disease.
Prognosis of mono and return-to-play
Mono typically goes away on its own without any repercussions, reports the Merck Manual. The more intense phase of mono clears up by two weeks, with half of infected people returning to work or school. Others recover faster, with 20% resuming normal activities. However, up to 10% of patients may continue to experience fatigue for weeks or even months.
For young athletes with mono, the decision regarding the right time to return to play is more complex due to their higher incidence of injury and consequent increased risk of complications, as discussed in a 2014 study in the journal Sports Health. For example, athletes have a greater risk of rupture of the spleen, particularly those engaged in contact sports or any activity that causes increased pressure within the abdomen. Also, high-intensity exercise may have a negative effect on immune function. Nevertheless, while athletes may need 2 to 3 months to fully bounce back from mono, they can return to play long before, provided they are well hydrated, free from fever, and fully recovered from fatigue. Ultimately, an athlete's decision to resume participation in sports after having infectious mono should be individualized.
Is there a vaccine to prevent mono?
Currently, there are no authorized vaccines to prevent infection with EBV.
A 2022 mouse study published in Science Translational Medicine, as well as other animal studies, demonstrated that an experimental EBV vaccine can trigger an effective immune response against EBV infection. Specifically, the EBV vaccine induced neutralizing antibodies in mice that blocked entry of the virus into immune cells, thus protecting against EBV infection. It is noteworthy that the mice used in this study were 'humanized' mice. Humanized mice are genetically engineered to contain human immune system components (via a 2013 study in the journal Pathogens). These mutated mice are readily infected with EBV and exhibit many features of human EBV infection. As noted by the 2022 study authors, an effective vaccine could prevent infectious mononucleosis and other diseases linked to EBV, including a variety of cancers.
Based on the above study and other animal studies, a clinical trial was launched on March 29, 2022 by the National Institute of Allergy and Infectious Diseases (NIAID) to evaluate an investigational vaccine for EBV (via ClinicalTrials.gov). This is a phase 1 study to be conducted at the NIH Clinical Center in Bethesda, Maryland. It is designed to test the safety and immunogenicity (ability to induce an immune response) of a 3-dose EBV vaccine. The estimated enrollment is 500 participants, and the estimated completion date is July 1, 2025.