Chlamydia Explained: Causes, Symptoms, And Treatments
Chlamydia is a bacterial infection caused by Chlamydia trachomatis. It is one of the most common sexually transmitted diseases (STD), with 1,579,885 cases reported in 2020, per the Centers for Disease Control and Prevention (CDC).
Chlamydia is spread through unprotected sexual contact with an infected person. The fact that many people do not show symptoms, either immediately or at all, contributes to the prevalence of this STD. Even if you are asymptomatic, you can still spread the disease (via WebMD).
If you are sexually active and practice safe sex, OB Gyn Care recommends that you be tested at least once a year. Testing every three months is recommended if you have multiple partners or your partner has sex with others. Although talking about STDs can be awkward, protecting yourself and your partners is necessary. Chlamydia and other STDs can have severe consequences if left untreated. Finally, it is essential to understand the possible symptoms, how chlamydia can be contracted, and how the disease should be treated.
Chlamydia symptoms in men
According to Healthline, men may or may not exhibit symptoms if infected with chlamydia. However, most symptoms will develop within a few weeks after exposure. If you are sexually active, you must test regularly. Males can contract chlamydial urethritis, which can manifest itself without symptoms at first.
Urethritis is the inflammation of the urethra, the tube that transports urine from your bladder to your penis. When you have urethritis, this structure becomes swollen and irritated, which can cause burning and pain when you urinate. It can also cause swelling of the tip of the penis, redness, and itching. Furthermore, a yellow or light brown discharge from the penis may be present. Healthline also mentions that testing for chlamydia in men can be uncomfortable, because most healthcare providers will insert an oversized sterile Q-tip into the tip of the penis to aid in diagnosis. Blood work may also be done.
According to the CDC, using condoms consistently and appropriately can provide the best protection against STDs, including chlamydia.
Chlamydia symptoms in women
Women, like men, may or may not initially exhibit symptoms of chlamydia, making it known as the "silent infection" (via Healthline). If symptoms appear in women, they typically begin several weeks after exposure to the bacterium. A woman's first sign of symptoms may be abnormal yellow vaginal discharge with a foul odor. Females may also experience abnormal bleeding between periods, which they may dismiss because of numerous causes other than chlamydia (via WebMD).
Pain in the lower back or abdomen is also common, in addition to pain during sexual intercourse. Women may also experience burning pain and frequency while urinating, which may be misinterpreted as a urinary tract infection. Other symptoms may include itching and burning around the vagina.
It is critical to note that if you have abdominal pain and a fever, you should consult your doctor to ensure you are not developing a severe complication (via STDWatch).
How common is chlamydia?
In the United States, chlamydia is the most common sexually transmitted disease; however, it is also easily treated with antibiotics, according to the American Sexual Health Association (ASHA).
In 2019, the CDC recorded nearly two million cases of chlamydia, though it is important to note that this figure only includes reported cases. Many instances of chlamydia go undiagnosed due to unreported cases or patients who are asymptomatic and are unaware they have chlamydia. The Cleveland Clinic estimates that the figure is much higher, particularly among those aged 15 to 24. This age group accounts for more than half of all reported chlamydia cases in the United States.
You might also be surprised to learn which states have the highest and lowest chlamydia rates. According to World Population Review, Alaska ranks first, with Louisiana and Mississippi close behind for the highest chlamydia rates. Unlike the top three states, Vermont has the lowest chlamydia infection rates in the country, with West Virginia and Maine also ranking low.
Chlamydia is transferred from person to person in the following ways
Chlamydia is spread from person to person via unprotected sexual contact with an infected individual (via ASHA). Healthline says using a condom is the best way to protect yourself and your partner if you are not in a mutually monogamous relationship. However, it is also essential to understand that chlamydia can be spread through genital skin-to-skin contact without actual penetration. This is because the bacteria that cause chlamydia can live on your genital mucous membranes. For this reason, it is critical to exercise caution when engaging in oral sex as well.
Furthermore, Pregnancy Birth and Baby recommends that women under 30 be tested for chlamydia if they are pregnant or plan to become pregnant to prevent complications with the pregnancy or the transfer of the infection to their baby during birth.
Lastly, you can spread the bacteria to your eyes, causing conjunctivitis or redness and eye infections (per Tufts Medical Center). Chlamydia in the eye happens when you touch or rub your eyes with contaminated hands or share washcloths with an infected partner. In this case, hand washing is essential to protecting against infection.
Oral sex and chlamydia
ASHA defines oral sex as any time someone places their mouth or tongue on a male or female's genital area or anus. Oral sex can be just as dangerous as sexual intercourse when it comes to transmitting chlamydia from an infected partner to a non-infected partner.
According to the CDC, if you have poor oral hygiene (such as gum disease or tooth decay), you are more likely to contract chlamydia or any STD during oral sex. In addition, a break in the mucus membranes, such as a sore in the mouth, can also put you at risk because the mucus membrane is a protective layer that helps keep bacteria out of the body. The CDC also recommends ways to protect yourself during oral sex by using a non-lubricated condom for oral sex with a penis or a dental dam to protect your mouth during vaginal or anal oral sex.
Furthermore, Healthline reports that even though it is uncommon, performing oral sex on your partner can result in chlamydia in the throat. If you are not in a mutually monogamous relationship, protection is essential.
Anal sex and chlamydia
If you have unprotected anal sex with an infected partner, you may contract chlamydia in your rectum or anus. During anal intercourse, the virus can infect the anus or rectum or spread from vaginal or penile secretions to this area. Rectal and anal symptoms can occur in men and women (via Health). If you have anal chlamydia, you may experience rectal pain or bloody discharge from your butt. Most people, however, do not develop symptoms or may misinterpret symptoms for other conditions, per Medical News Today.
Dr. Peter Leone tells Women's Health that you can get anal chlamydia not only through anal intercourse, but also through a rectally inserted sex toy containing infected secretions or even a finger containing the bacterial secretions.
Protection is essential for avoiding anal chlamydia. A common misconception is that precaution is unnecessary because you cannot become pregnant through anal sex. Condoms, on the other hand, are just as important for anal sex protection, because the rectal area does not produce natural lubrication and can thus tear fairly easily with penetration. Any sexual contact should be cautiously approached, especially if you have multiple partners.
How is chlamydia diagnosed?
Diagnosis and screening for chlamydia are simple procedures. There are several ways for your healthcare provider to test for bacteria. The Cleveland Clinic states that Nucleic Acid Amplification Tests (NAAT) is the gold standard for detecting chlamydia bacteria. A urine sample can be used to perform the test. You will be given a sterile cup and asked to provide the first part of your pee to ensure the highest concentration of bacteria is present for accurate results. Furthermore, the sample should be taken at least a few hours after you last urinated to ensure it is concentrated. This may sound strange if you've ever had to provide a urine sample for another reason. With that said, it is nonetheless critical to follow the instructions given by your provider when obtaining this sample (via MedlinePlus).
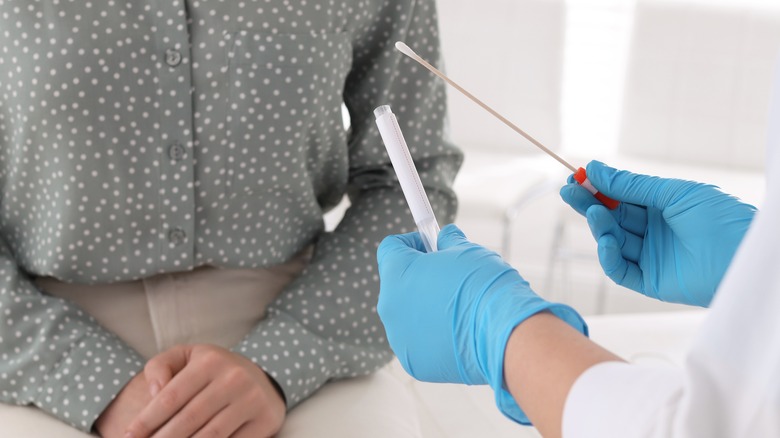
Alternatively, the Mayo Clinic reports that if you are a female, your healthcare provider may prefer to take a sample of your cervix discharge with a cotton tip swab to ensure accuracy, depending on your symptoms. This swab may produce immediate results or be sent to culture for analysis. Similarly, if you are a man, your doctor may want to take a sample of urethral secretions with a thin cotton swab inserted into the penis. Although this may be unpleasant, it may result in more accurate results. A swab may also be inserted into the rectum for testing if you have symptoms or concerns about anal chlamydia.
Ways to reduce your risk of contracting chlamydia
Abstinence is the only sure way to eliminate your risk of contracting chlamydia. However, for many people, this is not the most practical solution (via ASHA).
The CDC recommends mutual monogamous relationships as an excellent way to avoid contracting chlamydia or any other STD. However, communication and honesty are essential in this situation, because both parties must agree to be monogamous and be free of infection at the start of the relationship.
According to Be In The Know, using external male condoms every time you have vaginal, anal, or oral sex is the most effective way of protecting yourself if you have sex with multiple partners. You can also use an internal female condom or a dental dam to protect yourself during oral sex. It is also important to note that covering sex toys with condoms and washing them with soap and water is critical for protection against chlamydia and other STDs.
Pregnancy and chlamydia
It is critical to be tested for chlamydia and other STDs before conception or as soon as you suspect a pregnancy. According to BabyCenter, some women may not have symptoms. If the pregnant woman had untreated chlamydia before becoming pregnant, she could pass it on to the baby and potentially cause harm to the unborn child or herself. As a result of the STD, chlamydia can cause amniotic fluid infections, which could lead to preterm birth and premature rupture of membranes.
The Office on Women's Health states that if a baby is born prematurely due to chlamydia, it can lead to long-term health and developmental issues. Furthermore, if the mother is infected at the time of delivery, babies can contract chlamydia in their eyes or lungs. Signs of infection may be delayed, and may not present themselves until weeks or even months after delivery. Therefore, it is essential to consult with your doctor about testing and prevention while pregnant.
Treatment for chlamydia
The best case scenario is to avoid chlamydia through safe sex. However, if you contract chlamydia, don't worry — it's treatable with antibiotics.
According to the CDC, if you receive a single dose of antibiotic, you should avoid all sexual contact for at least seven days. Furthermore, if you are prescribed antibiotics for several days, you should refrain from sexual activity until the entire course of treatment is completed and your symptoms have subsided. Additionally, if you are being treated for chlamydia, you must notify your recent sexual partners and anyone with whom you may have had intimate contact other than intercourse. The CDC also states that repeat infections are expected due to sex partners who do not receive treatment. The more infections you get, the more likely you are to develop complications, including reproductive issues.
Finally, If you need chlamydia treatment, your doctor will recommend the best antibiotic for treatment. It would be best if you got retested three months after your antibiotics. This will ensure that the antibiotics are effective (via Mount Sinai).
Could you be at risk for developing pelvic inflammatory disease?
Pelvic inflammatory disease (PID) results from untreated sexually transmitted diseases such as chlamydia. It is a female reproductive system infection that has the potential to impact the ovaries, fallopian tubes, uterus, and cervix (via WebMD). PID may not result in any symptoms developing. Even if this is the case, the infection can still cause severe damage to the reproductive system, leading to infertility if not treated, per the American Academy of Pediatrics.
According to the Mayo Clinic, if you do develop symptoms, they can range from mild to severe. Lower abdominal or pelvic pain, odorous vaginal discharge, and abnormal vaginal bleeding are the most common symptoms, which can occur at any time or be noticed after sexual intercourse. You may also experience burning upon urination, and fever is possible.
WebMD also suggests if any of these symptoms are present, it is critical to contact your healthcare provider because PID can make it difficult for women of childbearing age to become pregnant.
Can natural remedies cure chlamydia?
Natural remedies for STDs, including chlamydia, have been used for centuries, according to Health Site. Because of its antibacterial effects, garlic is a natural remedy with numerous benefits. It is known to boost the immune system, and works well in aiding the body's defense against bacteria and viruses. According to Stanford Medicine, garlic supplements are available in capsules, extract forms, and other varieties. Of course, there is natural garlic that can be consumed as well. However, It is important to note that the ability to fight bacteria or cure infections such as chlamydia is not supported by evidence. As a result, it is still recommended that you consult with your healthcare provider.
Health Site also mentions goldenseal as a plant used to treat chlamydia. Goldenseal is also available in capsule and topical forms. With this alternative treatment, you should consult a doctor about dosing and the effects of other medications.
Despite claims that alternative natural remedies can help with chlamydia or other STDs, Healthline says that while they can relieve symptoms, they cannot cure the disease. Therefore, contacting your healthcare provider is the best way to ensure the infection is completely eradicated.
What can happen if you do not treat chlamydia?
If you have chlamydia and do not get treated, it can have severe consequences for you and any partners with whom you may have unprotected sex. According to Teen Source, men can develop testicular pain, swelling, and possible infertility. However, infertility is rare in men. Untreated chlamydia can also result in an increased risk of acquiring HIV, as the protective lining of the vagina, penis, anus, and mouth become compromised with chlamydia and other STDs (via the New York State Department of Health).
Females with untreated chlamydia have more complications than males. PID, as well as scar formation in the fallopian tubes, can result in infertility, according to the CDC. Furthermore, scar tissue can result in ectopic pregnancies.
Finally, the National Health Service warns that untreated chlamydia can lead to sexually acquired reactive arthritis (SARA). This is more common in men, and occurs when the joints become inflamed. SARA also affects the eyes and urethra (the tube through which you pee). While symptoms of SARA usually go away on their own, there is no cure for the condition. Ibuprofen and other anti-inflammatory medications may help relieve symptoms.