HPV Explained: Causes, Symptoms, And Treatments
Sexual intercourse (a.k.a. coitus, copulation, making love, or quite simply, sex) is defined by the Merriam-Webster Dictionary as the act of penetration of a female's vagina by a male's penis. Biologically speaking, the anatomy of humans are designed this way for the purpose of reproduction, i.e., the creation of offspring that ensures continuity of life. Today, Flo Health explains that the meaning of sex has evolved into something different, and it is highly dependent on a person's sexual orientation and own opinions.
Aside from its traditional definition, the word "sex" is also used to describe other forms of sexual activities. For example, anal sex is the penetration of a man or woman's anus by a male's penis, and oral sex is the act of stimulating the genitals using a person's mouth. But no matter the definition, sex (and all other sexual acts related to it) should always be performed safely among consenting and willing participants to avoid consequences like unwanted pregnancies and sexually transmitted infections (STIs).
According to the U.S. Department of Health and Human Services, there are over 20 million new cases of STIs reported in the U.S. every year, and this number is continuously rising. In the world, more than a million people get infected with an STI every single day. Based on data from the World Health Organization (WHO), majority of STI cases are caused by eight pathogens, which are syphilis, gonorrhea, chlamydia, trichomoniasis, hepatitis B, herpes simplex virus (HSV), human immunodeficiency virus (HIV), and human papillomavirus (HPV).
The human papillomavirus
The National Center for Biotechnology Information (NCBI) explains that papillomaviruses are a group of small viruses that colonize the skin and mucous membranes of humans and other animals such as birds, dogs, and monkeys. Infection from human papillomavirus is most commonly acquired via direct skin-to-skin contact (horizontal transmission), and rarely can be passed on by a pregnant mother to their unborn child (vertical transmission).
Horizontal transmission of HPV occurs during sexual contact (i.e., vaginal sex, anal sex, oral sex, close skin touching during sex) with an infected person. According to the Centers for Disease Control and Prevention (CDC), it can be difficult to trace exactly when a person acquires the infection because some don't have any signs or symptoms, and an infection can happen even if you only have had one sexual partner. It is also possible for you to experience no symptoms immediately after exposure, but then develop them years later.
HPV is the most prevalent STI, and has the highest incidence among all STIs in the United States. In 2018, there were approximately 42.5 million existing cases of HPV, and an estimated 13 million new cases (via the CDC). To put things in perspective, there were a total of 68 million existing cases of STIs overall (1 in 5 people), which means that HPV made up as much as 62.5% of all STI cases. Aside from its disease burden, HPV also exerts a tremendous economic burden of around 755 million dollars in direct medical costs.
Are all types of human papillomaviruses infectious?
More than 100 different types of human papillomaviruses have been discovered (per the NCBI). Around half of them are known to infect the genital tract (e.g., vulva, vagina, cervix, penis), and many are associated with certain cancers. They are often categorized as low- or high-risk, depending on their ability to cause cancer.
As explained by NYU Langone Health, low-risk HPV infections usually don't cause symptoms, are not associated with cancer, and may resolve on their own even without treatment. However, they can cause genital warts, which are fleshy outgrowths that can grow on a woman's vulva, cervix, or vagina, or on a man's penis or scrotum. They can also grow in and around the anus of both men and women (i.e., anal warts), in the mouth or throat (i.e., respiratory papillomatosis), and on the skin. Although low-risk HPV can cause some cellular changes in the cervix of females, these changes are mild, and are not considered a precursor to cancer. The most common low-risk strains are HPV 6 and 11, which collectively are responsible for 90 percent of HPV warts.
In contrast, high-risk HPV strains are appropriately called high-risk due to their propensity to develop into cancer. The most common types are HPV 16 and 18. Similar to low-risk HPV, infections from high-risk HPV strains can clear on their own within a couple of years. It's also important to know that while high-risk HPV can cause cancer, it doesn't mean they always will.
Who is at risk of getting HPV?
Any person who is sexually active or has had genital contact with another person can get infected with HPV. Men and women are equally at risk, but there are certain people who will be more prone to acquiring it compared to others. A person's risk of getting HPV also depends on their current health status, as well as lifestyle practices.
According to HPV Hub, one of the main risk factors for HPV is a person's age. The highest infection rate of HPV is seen among young adults in their 20s, and it is so widespread in this age group that screening women during this time in their lives is deemed to be unhelpful. In addition, sexually active people who have weak immune systems from another medical cause are also more likely to get HPV and consequently, they may not be able to clear the infection as effectively as a healthy person can. The same principle applies to those who did not get, or have not gotten, the HPV vaccine.
The U.S. Food & Drug Administration (FDA) adds that having sex at an early age, having many sexual partners, or having a sex partner who has (or had) many partners also increases your chances of getting exposed to, and subsequently infected with, HPV.
Based on the latest data provided by the CDC in 2017, the prevalences of oral HPV and genital HPV were lowest among non-Hispanic Asian adults and highest among non-Hispanic Black adults.
Signs and symptoms of HPV
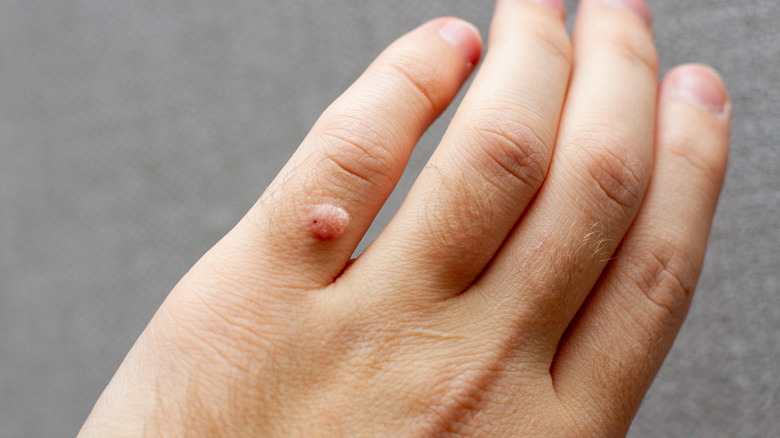
An HPV infection can go unnoticed in most people, especially if their bodies are able to get rid of the infection before it can cause any problems. If symptoms do exist, they are usually variable and depend on what the infecting HPV strain is. Low-risk HPV strains can cause warts, contagious growths on the skin that can be painful, itchy, or generally uncomfortable (via Healthline). On the other hand, high-risk HPV strains can cause many types of cancers, which unfortunately don't present with any symptoms until later on in the disease (per Planned Parenthood).
Medical News Today states that warts are classified according to their location and appearance. For example, common warts are rough and round, and sometimes have tiny black dots. They usually develop in areas with broken skin, and can be found on the fingers, nails, toes, and back of the hand. Warts that grow underneath or around the nails are called periungual warts. They are often painful, affect nail growth, and are difficult to treat. Plantar warts are similar to common warts, but are found on the feet or ankles. When they develop on the sole of the foot, walking may feel like stepping on a pebble inside a shoe. Flat warts are smooth, slightly raised, and mostly develop on the face. Meanwhile, genital warts can appear anywhere along the genital tract, and the same strains that cause them can also cause warts on the lips, mouth or throat (i.e., mucosal warts).
How is an HPV infection diagnosed?
If you have an HPV infection that is causing skin or mucosal warts, a doctor can typically make a diagnosis just by examining them. According to the American Academy of Dermatology Association (AAD), very rarely, a doctor may take a sample of your wart and send it to the lab (i.e., skin biopsy) to confirm the diagnosis. Women with genital warts and women who are being screened for HPV may be further assessed by a doctor using the visual inspection with acetic acid (VIA) test, a Pap smear, or a DNA test. The VIA test is done by applying vinegar to genital areas with suspected HPV. Areas that turn white are considered positive and will need further testing. A Pap smear is done by swabbing the cervix and vagina and sending the sample to the lab. The sample is examined for the presence of abnormal cells that may lead to cancer. A DNA test can detect high-risk strains of HPV in the cells of the cervix, and is recommended only for women 30 years and older, in combination with the Pap test (via the Mayo Clinic). Men with genital warts don't usually undergo any testing, although for high-risk individuals, a doctor may decide to swab the anal region to check for HPV (per Medical News Today).
If you don't have any signs, symptoms, or risk factors, there is usually no reason for a doctor to test you for HPV unless you are undergoing routine screening.
What is the treatment for HPV?
There is no treatment that can remove HPV from the body, but there are several ways a doctor can treat warts and abnormal cells in the cervix, if there are any.
According to the Cleveland Clinic, cryosurgery (freezing lesions using liquid nitrogen), loop electrosurgical excision procedure (using an electrically charged wire loop to get rid of lesions), and laser therapy (utilizing intense light to destroy lesions) can be used to remove warts or any abnormal cells. Other methods include electrocautery (burning warts using electricity converted to heat), application of trichloroacetic acid (a chemical that can burn warts), and using prescription creams like imiquimod and podofilox on warts to get rid of them.
If a doctor finds abnormal cells in a woman's cervix, they may perform a cold knife cone biopsy (a.k.a. cervical conization). A cone-shaped sample is taken from the cervix, which is then sent to the lab and checked for abnormal cells. It is a potentially curative procedure, if all abnormal cells were confined to the sample that was removed (per Mount Sinai).
Several studies have also looked into natural remedies for HPV. According to Healthline, vitamin B9 (folate) and vitamin C (ascorbic acid) may help reduce the risk of developing cervical cancer, and there is an ongoing trial being done on whether or not shiitake mushroom extract can cure HPV. However, it is still too early to tell, as the outcome from previous stages of the study so far have shown mixed results.
Can men have HPV?
It is a common misconception that only women can be affected by HPV, perhaps due to its well-known risk of developing into cervical cancer. But the truth is, men are just as at risk as women are of developing warts and cancers related to HPV. While tests are available to routinely screen women for HPV and cervical cancer, unfortunately, no such test exists for men.
WebMD states that more than half of sexually active men in the U.S. will acquire HPV at some point in their life, and around 1% will have genital warts at any given time. In addition, gay and bisexual men (i.e., men who have sex with men) are 17 times more likely to develop anal cancer compared to men who have sex exclusively with women. Because of this, some doctors perform anal Pap tests to check for the presence of high-risk HPV strains. Like women, infection with high-risk HPV strains usually don't cause any symptoms, and low-risk HPV strains can cause warts, which can typically be diagnosed by a doctor through close inspection. The VIA test can sometimes be used in men, but this test is prone to false positives, since normal skin can sometimes turn white as well.
An interesting thing to note is that, although opinions regarding circumcision are still somewhat divided, a 2016 study published in the European Society of Clinical Microbiology and Infectious Diseases (ESCMID) found that circumcision lowers the risk of acquiring several infections such as HPV.
HPV and cervical cancer
Cervical cancer occurs due to abnormal growth of cells in the cervix. According to the American Cancer Society, there are three types of cervical cancers: squamous cell carcinoma, adenocarcinoma, and mixed carcinoma. Nine out of ten cervical cancers are squamous cell carcinomas, and HPV is responsible for 99.7% of cases. Although cervical cancer is most often linked to high-risk strains of HPV, low-risk strains have been found in some cases as well.
Common symptoms of cervical cancer include abnormal bleeding from the vagina (e.g., bleeding after sex, bleeding outside of regular menstrual periods, longer or heavier menstrual bleeding), pelvic pain, pain during sex, and unusual vaginal discharge. These symptoms can be seen in other medical conditions as well, so it's important to speak with a doctor if you are experiencing any of them.
Based on a 2020 article published in the Journal of Obstetrics and Gynaecology, HPV infection often occurs at around 18 to 30 years old, while cervical cancer begins at around 35 years old. Because of this, vaccination is recommended at an early age, ideally before a person starts becoming sexually active. Additionally, screening for cervical cancer begins as early as 21 years old. Screening is done through a Pap test every three years for women 21 to 29 years old. For women 30 to 65 years old, a Pap test can be done every three years, an HPV test every five years, or a combined Pap test and HPV test every five years.
HPV and oropharyngeal cancer
According to the CDC, HPV can infect the mouth and throat (i.e., oral HPV), occurring most often through oral sex. Around 10% of men and 3.6% of women have oral HPV, and it is more commonly seen in older people. If a person's body is unable to clear oral HPV, it has the potential of causing cells in the back of the throat to grow uncontrollably and lead to oropharyngeal cancer. HPV infection is associated with 70% of all oropharyngeal cancer cases, while other risk factors include smoking, heavy alcohol use, history of other head and neck cancers, and chewing betel quid.
Possible signs and symptoms or oropharyngeal cancer include a neck lump, persistent sore throat, difficulty swallowing, problems with opening the mouth or moving the tongue, unintentional weight loss, ear pain, coughing up blood, and a white fuzzy patch on the tongue or insides of the mouth that cannot be scraped off (via the National Cancer Institute).
A 2022 article from the Nature Reviews Clinical Oncology journal states that in the U.S., HPV-related oropharyngeal cancer is more prevalent in Whites, as well as people belonging to a higher socioeconomic status. Nevertheless, because screening for oropharyngeal cancer is not available, prevention remains to be the best protection a person can have. The HPV vaccine works against strains that cause oropharyngeal cancer, and early studies show that those who are unvaccinated are at a significantly higher risk of developing the disease compared to those who are vaccinated.
HPV and anal cancer
HPV is associated with 90% of all anal cancers. Although rare, it is most often seen in people with weak immune systems (e.g., HIV, history of organ transplant, steroid use), women with cervical cancer, tobacco smokers, and men who have sex with men. Black men are particularly susceptible to anal cancer as well, possibly in connect to a higher incidence of HIV (per CureToday).
According to Johns Hopkins Medicine, anal cancer often presents with little to no symptoms. Pain, itching, bleeding, or a lump in the anus may occur, but these can be caused by other, more common health conditions as well. For high-risk individuals, a doctor may recommend screening for anal cancer, even if a person doesn't have any symptoms. Screening involves a Pap test similar to cervical screening, where the anus is swabbed and the sample is taken to a lab for further analysis. A digital rectal exam (DRE) may also be performed, where a doctor inserts a finger to check for any growths in the anus. If any abnormalities are seen, an anoscopy may be performed, which makes use of a scope to directly visualize the anus, typically followed by a tissue biopsy.
Medical News Today states that if cancer is found, a doctor may treat it using chemotherapy, radiation therapy, surgery, immunotherapy, or supportive care, depending on the severity and extent of the disease. Typically, survival rates are higher for localized disease (83.3%) and lower for cancer that has already spread (35.9%).
HPV and penile cancer
Penile cancer is rare in the general population. As explained by the Cleveland Clinic, it makes up less than 1% of cancers in males in the U.S., but more than 10% of cancers in males in Africa, Asia, and South America. HPV is seen in as much as 50% of cases of penile cancer, and other risk factors include phimosis (a condition where the foreskin of the penis is so tight that it prevents retraction), HIV, tobacco use (including smoking, chewing, and using snuff), radiation exposure, lichen sclerosus (a long-term inflammatory condition of the skin), and poor hygiene.
A 2017 article from the Translational Andrology and Urology journal reports that the incidence of penile cancer increases as a man gets older, and uncircumcised men have a higher prevalence. Signs and symptoms of penile cancer may include growths on the penis that may easily bleed, crust, or are bluish-brown in color; changes in the skin of the penis such as tightening or color shifts; foul-smelling fluid under the foreskin; swelling and irritation of the head of the penis; and a red, velvety rash. However, these symptoms can also be caused by infections or an allergic reaction. Therefore, it is important to see a doctor right away to have it checked, especially if the lesions are recurring or persistent (via the Urology Care Foundation). To maximally reduce your risk, consider getting circumcised if you haven't, get vaccinated against HPV, practice safe sex and good hygiene, and avoid smoking.
HPV and vulvovaginal cancer
Anyone who has a vulva and vagina is at risk of developing vulvovaginal cancer, but it is very rare. The CDC reported that in 2019, 5,579 women were diagnosed with vulvar cancer and 1,368 women were diagnosed with vaginal cancer in the U.S. Compared to other races and ethnicities, White women had the highest rate of vulvar cancer, while Black women had the highest rate of vaginal cancer.
According to Calvert Health, women with vulvovaginal cancer may experience pain, itching, bleeding, spotting, abnormal discharge, swelling, or a lump on the vulva and/or in the vagina. Women are at an especially increased risk if they are older, have a history of smoking or are current smokers, are infected with certain strains of HPV (e.g., HPV 16 and 18), have a history of precancerous lesions in the vagina, have had a hysterectomy or cervical cancer, became sexually active at a very early age, or have had many sexual partners. Women who were exposed to diethylstilbestrol (DES) while they were still in their mother's womb are also more likely to develop vulvovaginal cancer, but this is rarely seen nowadays since DES is no longer being sold or used.
HPV is responsible for 70% of vulvovaginal cancer cases. Although screening is not routinely performed, any physical abnormalities may be noted during cervical cancer screening, and the risk of getting vulvovaginal cancer can be further minimized by getting the HPV vaccine, practicing safe sex, and avoiding smoking (per Moffitt Cancer Center).
Can HPV be prevented?
It can be difficult to prevent HPV, since most people don't experience any symptoms and may not even be aware that they have it. Like with other STIs, the best way to prevent an HPV infection is avoiding all forms of sexual contact (via Planned Parenthood). But of course, this is not always feasible, as many people eventually become sexually active. While condoms can help reduce the risk of HPV, it does not completely prevent it, since HPV is acquired through skin-to-skin contact and not through bodily fluids. Because of this, one of the best ways a person can protect themselves against HPV is through vaccination.
The HPV vaccine protects against infection from the most common strains that cause genital warts and cancer. The CDC recommends that children 11 to 12 years old should receive two doses of the HPV vaccine 6 to 12 months apart, but vaccination can begin as early as 9 years old. Teenagers and young adults between 15 and 26 years old who started their vaccination later, and people between 9 to 26 years old with weakened immune systems, need to receive a total of three doses. Unfortunately, adults over 26 years old who have never received the vaccine are less likely to benefit.
When it comes to warts, the Mayo Clinic suggests wearing shoes in public pools and locker rooms to avoid getting them on your feet, and refraining from picking at them or nail-biting to prevent the spread of existing warts.
Life with HPV
It can be daunting to hear "You have HPV" coming from a doctor, but it shouldn't be the case. While HPV increases a person's risk of developing warts and certain cancers, it is also a very common infection that nearly all sexually active males and females will acquire it at some point in their lives. The good news is, most healthy people will clear the infection within a couple of years. For others, however, the virus can stay in the body for a really long time.
If you have HPV, the most important thing to do is inform your sexual partner (or partners). HPV is a contagious infection, and while it can present as a mild, almost nonexistent disease in one person, it can still become deadly in another. It's also important to know that if you are in a monogamous relationship, a diagnosis of HPV doesn't necessarily mean that someone was unfaithful, as it can take up to many years after exposure before the virus can get detected or for symptoms to develop (per the National Cervical Cancer Coalition).
The next steps to take include educating yourself and looking after your health. A doctor will be able to answer any questions you or your partner may have about HPV, and there are also many credible resources online (via Healthline). To stay healthy, observe proper diet and nutrition, exercise regularly, avoid unhealthy habits such as smoking, and have a health checkup as often as needed.