Brittle Diabetes Explained: Causes, Symptoms, And Treatments
While most people have heard of type 1 and type 2 diabetes, not everyone has heard of brittle diabetes. That's because brittle diabetes is a rare disease. People with brittle diabetes experience extreme swings in their blood sugar levels (per Medical News Today). These rapid changes from high to low blood sugar and back again negatively affect the lives of brittle diabetes patients, disrupting their daily lives, making it hard to manage their symptoms, and causing long-term health consequences.
Brittle diabetes is not just a rare diagnosis; it is also a controversial one. The American Diabetes Association does not recognize it as a unique form of diabetes, and not all doctors agree that brittle diabetes is a real condition. This lack of recognition can be frustrating to people with brittle diabetes, who struggle to manage unpredictable changes in their blood sugar levels and experience the very real negative health effects it causes.
The definition of brittle diabetes
Brittle diabetes, also known as labile diabetes or unstable diabetes, is a rare condition that affects just three out of 1,000 people with insulin-dependent diabetes (per the Cleveland Clinic). According to a 2021 study published in the Journal of Diabetes and Its Complications, brittle diabetes is a form of diabetes found most often in patients with type 1 diabetes, but is sometimes seen in patients with "severely insulin deficient" type 2 diabetes.
People with brittle diabetes have extremely poor glycemic control that leads to rapid changes in blood sugar levels. According to the Juvenile Diabetes Research Foundation, patients with brittle diabetes experience blood sugar drops that lead to dangerously low levels or spikes that can lead to ketoacidosis (DKA), no matter how carefully they monitor and manage their diabetes.
The Journal of Diabetes and Its Complications describes the serious health effects of brittle diabetes. As a result of these unpredictable changes in blood sugar levels, these patients experience greater diabetes distress and more diabetes-related complications when compared to other people with diabetes. They make more visits to the emergency room, are admitted more frequently to the hospital, and utilize more healthcare services overall. They also experience greater relationship strains because of their health condition.
Brittle diabetes is a controversial diagnosis
Not everyone agrees that brittle diabetes is an actual condition. Per Healthline, the term "brittle diabetes" was coined before glucometers were in use and was originally used to describe patients who experienced severe hypoglycemia and DKA regularly. After the advent of glucometers, brittle diabetes became a catch-all term for any case of diabetes that was difficult to control because of inexplicable changes in blood sugar levels. Because it lacks a precise definition, there is some debate about whether it is a specific condition or simply a term used when doctors don't know why their patient struggles to manage their diabetes.
One argument against brittle diabetes as a stand-alone diagnosis is that for some patients, their symptoms of brittle diabetes go away when they receive treatment for one or more underlying conditions. While these patients still have diabetes, it becomes manageable, and they no longer experience severe fluctuations in blood sugar. This relief implies that brittle diabetes is just a subset of diabetes. However, the National Institutes of Health now recognizes it as a rare disease, giving credibility to those who argue that it is a separate condition, not a subset of diabetes.
Those at risk for developing brittle diabetes
According to a 1985 article in the British Medical Journal, overweight adolescent females with insulin dependent diabetes as well as emotional disturbances were the first group of patients diagnosed with brittle diabetes. This observation suggests that age and gender put people with insulin dependent diabetes at risk of developing brittle diabetes.
However, a 2021 study from the Journal of Diabetes and Its Complications shows that young women with diabetes are not the only group at risk of developing this condition. Four distinct groups of people who already have diabetes are at risk of developing brittle diabetes: patients with psychiatric diseases, patients with underlying conditions that cause a disruption in insulin sensitivity or glucose utilization, geriatric patients with type 1 diabetes combined with other diseases of aging, and patients with type 1 diabetes who also experience food insecurity and a lack of access to insulin.
Based on this information, people who have type 1 diabetes or severely insulin deficient type 2 diabetes as well as one other risk factor are at greatest risk of developing brittle diabetes.
Psychological causes of brittle diabetes
Several studies have demonstrated the relationship between mental health and brittle diabetes. A 2017 study in the Journal Nutrients found that eating disorders such as anorexia nervosa, bulimia, binge eating disorder, rumination, and pica can complicate the clinical course of type 1 diabetes. Patients with type 1 diabetes and a diagnosis of an eating disorder are more likely to have episodes of DKA and hypoglycemia, the hallmarks of brittle diabetes. They are more likely to be hospitalized and when they are, their hospital stays are longer than the stays of other patients. Overall, patients with type 1 diabetes and an eating disorder are at higher risk of premature mortality.
Depression and other mental health conditions can also contribute to brittle diabetes. Depression can increase hyperglycemia (per a 2016 study from the Journal of Medicine and Life), which is concerning because depression is roughly three times more prevalent in patients with Type 1 diabetes than in their healthy peers. In addition, a 2002 study from the Journal of Psychosomatic Research shows that, "Children with diabetes have a two-fold greater prevalence of depression, and adolescents up to three-fold greater, than youth without diabetes."
Other mental health conditions linked to brittle diabetes include borderline, histrionic, and narcissistic personality disorders (per a 2016 study from the Journal of Diabetes and Its Complications). Because of the relationship between mental health and brittle diabetes, doctors should conduct mental health screenings for patients with uncontrolled diabetes.
Underlying conditions can cause brittle diabetes
In some cases, an underlying physical condition can cause brittle diabetes. A 2021 case study from the Journal of the ASEAN Federation of Endocrine Societies reports that a 29-year-old man suffered from brittle diabetes caused by his undiagnosed celiac disease. Celiac disease can cause malabsorption, which may lead to unexplained hyper- and hypoglycemia.
Diabetic gastroparesis is another underlying condition that can cause brittle diabetes. A 2017 study from the Journal of Diabetes and Its Complications found that roughly 5% of patients with type 1 diabetes have diabetic gastroparesis, or delayed gastric emptying, which results in food and liquids remaining in the stomach for long periods. Gastroparesis puts patients with type 1 diabetes at greater risk of severe hypoglycemia.
Another condition that can cause brittle diabetes is lipohypertrophy, which is a complication of type 1 diabetes (per Healthline). Lipohypertrophy is a lump of fat under the skin caused by repeated insulin injections. It can blunt insulin action and absorption, leading to deteriorating glucose control (per a 2016 study in the journal Diabetes Care). Simply moving the injection site can resolve the symptoms of brittle diabetes.
These are just a few examples of underlying conditions that can lead to brittle diabetes. They stress the importance of looking for undiagnosed underlying conditions when dealing with patients who have brittle diabetes.
Geriatric conditions can cause brittle diabetes
While type 1 diabetes was once strongly associated with premature mortality, life expectancy for people with this condition has increased in recent years, according to a 2012 study from the journal Diabetes. In addition, people can develop type 1 diabetes late in life (per a 1984 study in the journal Diabetes Medicine). As type 1 diabetics reach old age, they may be at greater risk of developing brittle diabetes. A 2001 study in the Journal of the Royal Society of Medicine identified 55 patients with brittle diabetes between the ages of 60 and 79. Of these patients, 29% experienced recurrent DKA, 27% experienced recurrent hypoglycemia, and 44% experienced mixed brittleness.
One reason that elderly type 1 diabetes patients may be at risk of brittle diabetes is that diabetes self-management can be challenging for people experiencing cognitive decline and other comorbidities associated with aging. According to a 2021 study in the Journal of Diabetes and Its Complications, elderly patients may have a hard time remembering to administer insulin or may rely on family members who are unfamiliar with diabetes management to administer it for them. They may also experience problems with hearing and vision loss, challenges with dexterity, depression, and other health problems that result in symptoms of brittle diabetes.
Food insecurity and lack of insulin access can lead to brittle diabetes
While the original definition of brittle diabetes implied a biological basis for this condition, a newer definition includes uncontrolled blood sugar swings caused by a lack of insulin access and food insecurity, according to a 2021 study in the Journal of Diabetes and Its Complications. People who lack access to insulin may ration their insulin supply, which can lead to DKA, blindness, heart disease, and disability, according to a 2019 article in the American Journal of Managed Care.
The World Health Organization (WHO) only considers medication affordable if a 30-day supply costs one day's wages or less based on the wages of the lowest-paid unskilled government worker. A 2017 study published in the journal PLOS One found that in low-income and lower-middle income countries, the median cost of a 30-day supply of diabetes medication was more than one day's wages. In other words, "Paying more than one days' wages was considered unaffordable" (via PLOS One). These findings highlight the difficulty of obtaining insulin because of financial stress in many parts of the world.
Affording enough and good quality food is another challenge worldwide. Food insecurity — which is uncertain or limited access to safe or adequate food — also contributes to brittle diabetes. Children in food insecure families are more likely to have high HbA1c levels and to be hospitalized, notes a study in The Journal of Pediatrics. Though it is a sensitive topic, clinicians should screen patients with brittle diabetes for food and insulin insecurity when trying to identify the cause of their condition.
A doctor can diagnose brittle diabetes
If you currently experience inexplicable or uncontrolled symptoms of diabetes, you should seek medical attention. A doctor can thoroughly evaluate your symptoms and determine whether you have brittle diabetes. ClinicalTrials.gov describes a trial involving type 1 diabetes patients with brittle diabetes running through 2023, and it provides guidelines for a brittle diabetes diagnosis.
According to the study criteria, patients with brittle diabetes have two or more of these symptoms: persistence of severe hypoglycemia, occurrence of DKA events without obvious cause, diagnosis of unaware hypoglycemic episodes of less than 3 millimoles per liter based on continuous glucose monitoring (CGM) or "self-monitoring blood glucose data," a mean blood glucose standard deviation of greater than 50%, a mean amplitude of glucose excursions (MAGE) index of greater than 60 milligrams per deciliter, a low blood sugar glucose index of greater than 5, a Clarke score of greater than 4 (which suggests impaired awareness of hypoglycemia), or a HYPOSCORE (which quantifies hypoglycemia) of greater than 800.
Symptoms of brittle diabetes
The symptoms of brittle diabetes vary widely. Because people with brittle diabetes experience extremely high and low blood sugar levels, they may experience symptoms of each depending on their current blood sugar level (per Medical News Today).
When their blood sugar levels are low, patients may experience symptoms of hypoglycemia, which can include feeling tired, hungry, dizzy, or weak. Patients may also sweat, shake, have a rapid or irregular heartrate, feel confused, have a seizure, or faint. They may also end up in a coma.
At the other extreme, when their blood sugar levels are high, patients may experience symptoms of hyperglycemia, which can include excessive thirst, intense or unusual hunger, frequent urge to urinate, headaches, blurry vision, unexplained weight loss, irritability, and fatigue.
Severe hyperglycemia can lead to DKA, a potentially life-threatening condition (per the Centers for Disease Control and Prevention). When the body does not have enough insulin to allow sugar into cells, it starts to break down fat for fuel instead. Breaking down fat produces ketones, a type of acid that can quickly build up to dangerous levels in the blood. Patients should seek emergency medical attention if they have DKA symptoms such as blood sugar at 300 milligrams per deciliter or higher, fruity-smelling breath, difficulty breathing, or vomiting.
Technology can help you manage brittle diabetes
Brittle diabetes, by definition, is difficult to control. Because brittle diabetes causes erratic, unpredictable changes in blood sugar levels, patients struggle to manage their blood sugar and avoid complications. Despite these challenges, people with brittle diabetes can take steps to manage their condition.
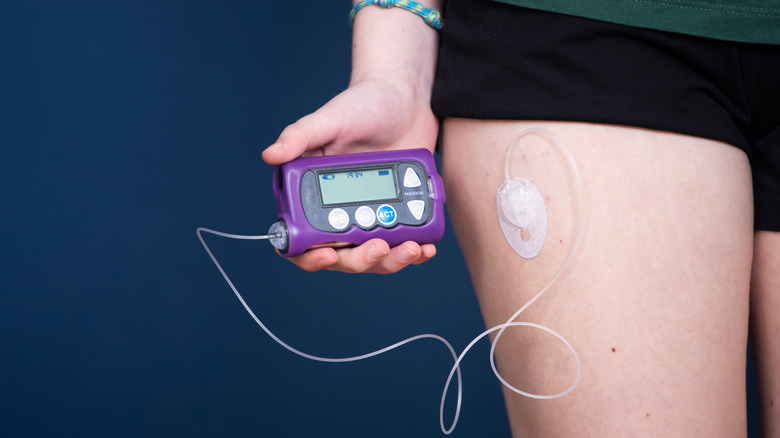
Your doctor may recommend a continuous glucose monitor (CGM) to help you track your blood sugar levels at all times. According to the National Institute of Diabetes and Digestive and Kidney Diseases, a CGM uses a tiny sensor placed under the skin of your arm or belly to monitor your blood sugar levels every few minutes. You can track the results on your computer, tablet, or smartphone. Some models come with an alarm that will sound if your blood sugar gets too high or too low. You can use this technology to alter your food intake, medicine use, and activity to prevent extreme highs and lows.
Another option is an insulin pump, a wearable device (per Healthline) that administers insulin throughout the day via a cannula under your skin. Your doctor will determine the right rate for you, and you can also tell the pump to deliver a bolus (extra dose) of insulin as needed. Some pumps can work in conjunction with a CGM to adjust the rate of insulin based on your blood sugar readings. Insulin pumps require proper training to use effectively, so they are not always a good option for children.
A transplant can help with brittle diabetes
In addition to technological innovations such as CGM and insulin pumps, transplantation of a pancreas or islet cells may help with brittle diabetes. A healthy pancreas produces insulin to control blood sugar, and islet cells are a type of cell in the pancreas, according to Medical News Today.
A 2013 study in the journal Diabetes Care examined the outcome in brittle diabetes patients who received a pancreas transplant alone (as opposed to transplant of kidney and pancreas). These patients had recurrent hypoglycemic episodes or hypoglycemic unawareness and failed to improve with insulin therapy, including use of an insulin pump. The study found that the transplant helped patients achieve long-term normal blood sugar levels, avoid hypoglycemia, and avoid the development or progression of secondary diabetes complications.
An islet cell transplant is another treatment option for patients with brittle diabetes (per a 2019 review in Endocrine Reviews). Here, doctors transplant islet cells isolated from the pancreas of a deceased donor or islet cells isolated from the patient's own pancreas. In this procedure, the islet cells are infused into the patient's liver, where they can produce insulin.
Soon, patients may be able to utilize an artificial (bionic) pancreas (via the National Institutes of Health). The bionic pancreas trial was more effective at keeping blood sugar levels in a normal range than "standard-of-care management" in patients with type 1 diabetes. While it is not yet commercially available, it is a promising development.
Treatment for underlying psychological conditions can treat brittle diabetes
For people whose brittle diabetes is caused by underlying psychological issues, treating these issues may help manage their diabetes.
For example, a 1991 study in the Journal of the American Academy of Child and Adolescent Psychiatry compared two groups of children with diabetes. Both groups had grossly abnormal blood glucose profiles and required repeated admission to the hospital. A control group received inpatient medical intervention, while the experimental group received psychoanalytic therapy three to four times a week for an average of 15 weeks. The control group reverted to the prehospitalization level of metabolic control within three months, but the experimental group improved diabetic control and maintained these positive results at a one-year checkup.
A 2020 review published in Current Diabetes Reports discusses the importance of providing psychological interventions that have specific modifiable behavioral targets for people with diabetes (PWD). "Specific modifiable behavioral targets for behavioral health providers treating PWD include glycemic control, adherence, depression, motivational status, and lifestyle modifications. Psychological interventions can target these outcomes through a number of interventions, including behavioral management and reinforcement, guided problem-solving, supporting patients in setting realistic and attainable goals, and teaching relaxation strategies for managing diabetes-related stressors" (via Current Diabetes Reports).
Brittle diabetes can cause significant health problems
Uncontrolled brittle diabetes can lead to significant health problems. Many complications associated with brittle diabetes come from excess blood sugar. According to Johns Hopkins Medicine, glucose belongs in your cells, not in your blood. When sugar builds up in the bloodstream, it can damage blood vessels and nerves throughout the body. Over time, that damage can lead to problems with the eyes, kidneys, heart, and nerves (per the Cleveland Clinic).
A 2011 study published in QJM: Monthly Journal of the Association of Physicians followed a group of patients with brittle diabetes for 20 years. This study found that brittle diabetes was linked to premature death, as half of the traceable patients died, mostly because of diabetes-related complications, during the study. The patients who survived experienced a significant burden of complications such as nephropathy, which is the "deterioration of kidney function" (per Johns Hopkins Medicine) — and autonomic neuropathy which is "damage to the nerves that control automatic body functions. It can affect blood pressure, temperature control, digestion, bladder function and even sexual function" (per the Mayo Clinic).
According to the Cleveland Clinic, patients with brittle diabetes are hospitalized more frequently, have a lower quality of life, and have a shorter life expectancy. These negative outcomes stress the important of seeking proper treatment for brittle diabetes.