Unexpected Complications Of Severe Eczema
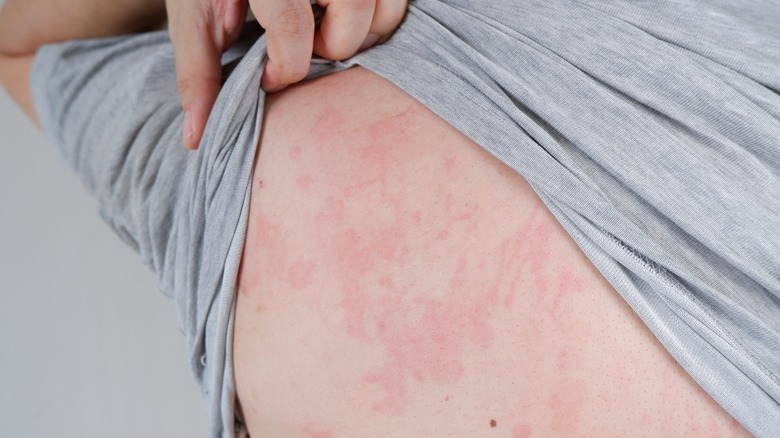
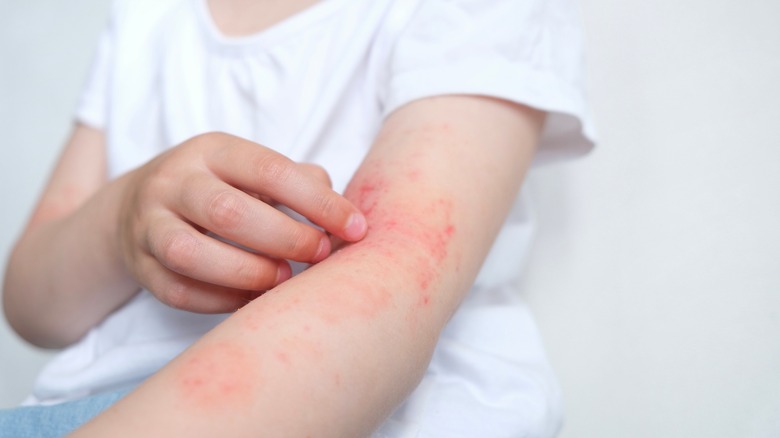
Eczema is one of the most common skin conditions out there, and for people living with it, it can present some challenges. Around a tenth of all people in the United States live with eczema, with children being particularly susceptible to developing it, as the National Eczema Association discusses. Also known as atopic dermatitis, eczema occurs due to an inflammation of the skin, and people who have it can expect to deal with changes to their skin, including persistent itchiness and dryness, notes the American Academy of Dermatology Association (AAD). But for some people, it doesn't end there: Eczema can present in increasingly severe forms, and create skin symptoms and rashes that start to inhibit their day-to-day lives.
And unfortunately, with this condition can come a host of other medical considerations. While the symptoms of eczema itself are skin-based, it can prompt some knock-on effects and medical issues that can not only be surprising, but pretty serious. As such, it's vital to remain informed about how eczema might affect you beyond your expected symptoms, and how to spot the signs of other complications. And we've got some of them right here.
Severe eczema can increase the risk of heart disease
While eczema is a skin condition, it can affect other parts of your body that you might not expect. And one of these parts could be your heart. As research published in the BMJ discusses, people who have severe eczema appear to be more likely to develop cardiovascular disease and experience complications as a result. The London School of Hygiene & Tropical Medicine's Anna Ascott, who worked on the research, points toward inflammation being potentially behind this: As she told the National Eczema Association, when individuals have severe eczema, they have more inflammation across the board in their systems, and this inflammation can then impact the cardiovascular system, leading to more risk of disease.
Myocardial infarction, angina, and heart failure risk are all perceived to be more likely for folks who have more severe forms of eczema. While this may understandably be concerning for some, Ascott does state that "although people with moderate and severe atopic eczema are at higher risk of heart disease, the overall risk is low." Regardless, it's always a good idea to discuss your heart health with your doctor regularly, especially if you experience severe eczema, to ensure you can stay on top of it.
If you have severe eczema, you may be more at risk of food allergies
People with eczema likely have enough to handle while managing their condition, but unfortunately, some folks may have a little more on their plate to deal with. Or, they may have to think about what's not on their plate. As research published in Food Allergy: Molecular Basis and Clinical Practice discusses, food allergies are fairly common in kids who have severe eczema, with roughly 33% of all children having both conditions. These allergies are generally prompted by dairy products like cow's milk, or eggs, as Medical News Today states. According to research published in Current Opinion in Allergy and Clinical Immunology, allergies are more likely to develop in kids with eczema because their skin can be less protective and prone to having more bacteria on it, which heightens the likelihood of allergies developing.
In adults, the good news is that if you have severe eczema, your likelihood of having a food allergy is far lower, due to allergies frequently being outgrown as people move into adulthood (per Anaphylaxis UK) — and if you do still have a food allergy, you'll probably already know about it. In children, though, it could be the case that introducing them to potentially triggering foods at a young age could help them keep allergies at bay. It's vital, however, to always look out for the symptoms of an allergic response, which can include vomiting, changes in skin appearance, and difficulty breathing.
Having eczema increases your risk of staph infections
Having eczema may affect your skin health in other areas, and one of these could be an increased likelihood of other skin infections. Staph infections, which often cause lumpy, swollen, or crusty skin, according to the National Health Service, can be more likely if you have severe eczema. This is because when you have eczema, the bacteria that can prompt staph infections are more likely to be able to thrive on your skin, and therefore prompt an infection (per Health Central). In fact, if you have eczema, the chance of having staph bacteria on your skin is pretty high — it's found on as many as 90% of people with severe atopic dermatitis.
It's worth remembering, too, that these infections are far from harmless, and can have some serious health effects — not only on your quality of life, but potentially on your longevity itself, says WebMD. If you suspect you've developed a staph infection as a result of your eczema, or you notice any changes in your skin, you must seek treatment immediately. Your healthcare provider may have to prescribe medicine in addition to your standard eczema medication to deal with the infection.
Your flu shot might be less effective
A flu shot is an essential part of many people's yearly routine, and for good reason: Getting a flu vaccination can lower the risk of becoming sick with the flu when it's circulating the most by up to 60%, as the Centers for Disease Control and Prevention (CDC) discusses. But individuals who have severe eczema may have more trouble with their flu shot working in the first place, as research published in the Journal of Allergy and Clinical Immunology shows. The researchers found that when people had atopic dermatitis that was accompanied by staph bacteria residing on the skin — a common feature for people with eczema — flu vaccines injected into the skin tended to be less effective, and did a worse job at stimulating an immune response.
It's not all bad news, though: The research also demonstrated that when individuals were injected with a vaccine directly into their muscles, there was no difference in efficacy. If there's any doubt when going to get your flu shot, make sure that you let the person administering it knows that you have eczema, as this could inform how they deliver the vaccine. Remember, too, to check whether a flu shot will interact with any medicine you take for your eczema, as Healthline advises.
Severe eczema might make the smallpox vaccine riskier
The smallpox vaccine is one of modern medicine's biggest success stories, with the vaccine having wiped out the disease in naturally-occurring settings, as the CDC states. There are, however, certain instances in which people might still need the smallpox vaccine. For instance, people who work in laboratory settings that might contain the virus are still at risk (per the CDC).
For those folks, having eczema might create difficulties. Receiving the vaccine when you have eczema, or even coming into physical contact with a person who's had a smallpox vaccine in the last month, can result in eczema vaccinatum, a dangerous infection that can cause a high fever and medical complications, states the AAD. Even if you haven't had an eczema flare-up in years, or your symptoms have seemingly disappeared, you can still be susceptible to contracting the infection. As such, it's vitally important to withhold any contact with people who have had the vaccine until their wound site has fully healed and they don't have a scab anymore. If you think you are at risk of smallpox and you do have eczema, speak to your doctor about your options.
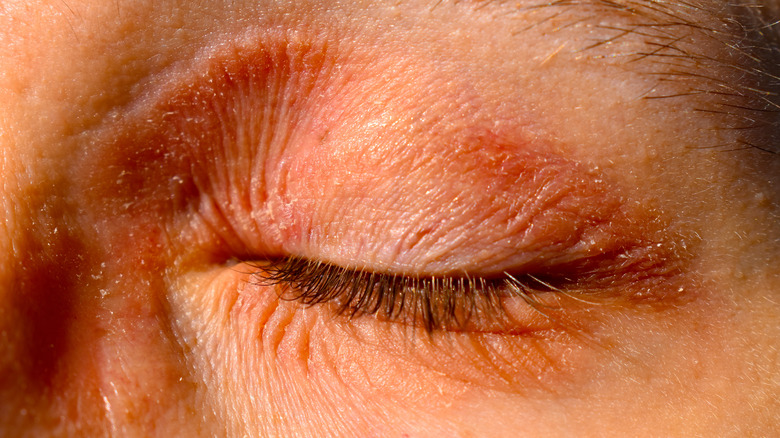
Your eczema may prompt eye problems
Eczema can affect pretty much any area of skin around your body, and that includes the skin around your eyes. And unfortunately, this can lead to some issues for your eyes themselves, as the AAD explains People with severe eczema can be particularly vulnerable to eye conditions like conjunctivitis, also known as pink eye (for the color that it causes your eye to turn). Conjunctivitis can also cause your eyes to become crusty or itchy, and may make dealing with bright environments more difficult.
Having eczema may also affect your cornea. Your cornea is at increased risk of becoming inflamed, a condition known as keratitis. The cornea can even start to change shape thanks to eczema increasing how often you rub your eyes, eventually having an impact on your eyesight. That's why, if you have atopic dermatitis, you should keep an eye on things (if you'll excuse the pun). Make sure that you're seeing an eye doctor and having an eye exam at frequent intervals, and alert your regular doctor at the first sign of something unusual. Early diagnosis can help to minimize the risk of long-term complications.
Weeping eczema is a complication to watch out for
People with severe eczema are wise to be on guard for when their condition worsens. And one particular warning sign to keep on the lookout for is the development of small, fluid-filled blisters or bumps, which can develop into weeping eczema (per the Cleveland Clinic). Weeping eczema, as you might expect, occurs when your eczema becomes particularly inflamed and develops to a point where it weeps light-colored or clear liquid, which then can scab over and create crusts on the skin. Generally, this will be accompanied by your other eczema symptoms getting more severe, with pain and redness also common.
Some individuals may experience particularly acute weeping, and this can lead to full-body symptoms like fatigue, aches and pains, or fever, as well as an increased likelihood of contracting other topical infections. If you notice that your eczema is weeping, it's wise to speak to your doctor. They may be able to prescribe additional treatments to manage symptoms, such as oral or topical steroids and immunosuppressants to bring down inflammation. It's also wise to practice a robust skincare treatment. Keep your skin well-moistened, and avoid particularly harsh skin or haircare products.
People with eczema may develop eczema herpeticum
While eczema isn't caused by a virus, it can make you more susceptible to viruses that cause skin issues. And one of these is herpes. Herpes can pass from person to person via sexual activity or more general skin-on-skin contact, and while it's usually not hugely problematic, if it passes to people with eczema, it can create a condition named eczema herpeticum (per Medical News Today).
Eczema herpeticum usually develops when a cold sore touches eczema-affected skin, and although it's pretty uncommon, it can also get serious quickly. The affected person may begin with a cold sore, but after that, they can develop painful, weeping rashes, and more general symptoms like a fever or tiredness. In its most serious form, eczema herpeticum can lead to vision loss, scars, and if the virus works its way to your internal organs, a loss of organ function and potential death. Individuals are at their most prone to contracting eczema herpeticum when their eczema is especially acute or if their skin has been damaged recently, and babies and younger kids are also more likely to develop it. Antiviral medication is one of the most established courses of treatment, and depending on how severe the condition is, you may have to spend some time in the hospital.
Severe eczema can seriously disrupt sleep
There are few things worse than having a bad night's sleep. But for folks who have particularly severe eczema, avoiding a bad night's sleep can be a little more complicated. Eczema and sleep have a complex relationship, and the skin itchiness that marks eczema can kick in when we wake up during the night — including during brief periods when we're not even conscious of being awake (per the National Eczema Association). As a result, we can then start scratching, which then increases the impulse to itch even more, which creates a vicious cycle — and all of this disrupts restful slumber.
Our changes in body temperature throughout the evening, and particularly before bedtime, can mean that we have an increased desire to itch before we go to sleep, and this can mean that getting off to sleep is harder in the first place, too. While this can all be hard to manage, it's worth following a few basic sleep hygiene principles to increase your chance of a good night's rest. Try to keep the time you go to bed and wake up regular, make your bedroom as inviting as possible and free of digital distractions, and try not to have that third coffee after lunch.
In some cases, kids with severe eczema have trouble growing
Having eczema as an adult can be difficult, but when your kids have it? That can be even more challenging. And when your child's eczema gets especially severe, it can have several cascading effects. One of these may be how much your kid grows, as research published in the Indian Journal of Dermatology discusses. The research found that when children have atopic dermatitis, they're more likely to experience trouble with achieving a regular height and weight for their age group, and this effect appears to be more likely the more severe their eczema is.
This appears to be down to the amount of growth hormone that kids with eczema produce. In comparison to kids that don't have the skin condition, those with eczema have lower amounts of growth hormone, which in turn affects how they develop (per Ada West Dermatology). This could be because when children have eczema, they have more difficulty getting a good night's sleep, which disrupts their natural growth processes. Kids who have eczema may also experience further issues with bone and skeleton development, and a potentially higher risk of brittle bones, osteoporosis, and bone breaking.
Severe eczema can have an impact on your lifestyle
Some of the most unfortunate complications of eczema may not be purely medical, but could be related to the very way that you live your life. For a lot of people, eczema is a lifelong condition, and having it can mean you have to make some notable lifestyle adjustments, whether you want to or not. People with severe eczema might find that they have to apportion more of their income toward their healthcare, as having the condition can mean you spend more money on prescriptions, seeing your doctor, and covering any work days you have to miss, says WebMD. While frustrating, this can also be necessary to keep your eczema in check.
You may also have to adapt your day-to-day lifestyle to better manage your eczema. You'll likely be more triggered by certain substances, like fragrances or cigarette smoke, so try and minimize these in your home, states Boston-based dermatologist JiaDe Yu to Everyday Health. It can also be worth changing up your activities to reduce symptoms where you can. Some forms of regular exercise, for example, are excellent for eczema management. Swimming, says Yu, is "a great form of exercise that engages many muscle groups. The chlorinated water can be helpful in decreasing inflammation in the skin."
Eczema and asthma can come hand-in-hand
Unfortunately for those with eczema, incidences of eczema and asthma closely linked, as WebMD states. This is due to the inflammatory process that occurs with eczema — this inflammation is often prompted by an environmental allergen such as pollen, mold, dust mites, or dander from animals. The same is true of asthma (per Healthline). With both conditions, the body perceives the irritant as a harmful invader and provokes an intense response characterized by inflammation. It's for this reason that people with eczema may also be more likely to have hay fever or allergic rhinitis. As well as having itching on your skin, you may also experience itchiness in the nasal or mouth area when allergens prompt a reaction.
As WebMD notes, more than 50% of kids with eczema will also show signs of asthma, environmental allergies, and/or hay fever by the time they hit adolescence, and all of these conditions may potentially never be outgrown.
Severe eczema may increase your risk of mental health conditions
It can be easy to forget, but our mind is an intrinsic part of our body. And conditions that affect our body at large can also affect what's going on with our mental health. When it comes to eczema, the link between the condition and poor mental health is fairly complex. As eczema is an inflammatory condition, this can then affect our mind, as University of Wisconsin-Madison School of Medicine and Public Health's Department of Psychiatry professor Charles Raison discusses via the National Eczema Association. "We know that inflammation can talk to the brain, making us feel anxious, depressed, tired and foggy thinking," Raison states, and as such, the more inflammation you have, the more likely you are to potentially have mental health concerns.
However, there are other reasons why people with eczema may have mental health conditions. For instance, Raison discusses the fact that having severe eczema may result in feelings of shame or embarrassment, compounding what could already be a susceptibility to mental health problems. You must keep an eye out for any symptoms of depression or anxiety, which can include feeling low or sad persistently, finding it harder to focus, and a general loss of enthusiasm for activities you once enjoyed (per the National Eczema Association).
How can I treat my eczema?
Eczema can be managed in many ways, and it's really important to remember that what might work for someone else may not work for you, states WebMD. Your treatment plan should be decided with your doctor, who will be informed by how severe your condition is and any medical issues you've had in the past. Eczema can be treated with a combination of medications and ointments, with corticosteroid creams often used to bring down inflammation on the skin and provide relief from symptoms. Your doctor may also prescribe corticosteroid pills or certain moisturizers that can help to seal moisture into your skin and fight against dryness.
If your eczema leads to other conditions, your doctor may also prescribe you medication to deal with them, like antibiotics if your eczema leads to an associated skin infection. It's also worth remembering that how you manage your skin on a day-to-day basis can influence the effectiveness of treatment and your comfort levels. Make sure that you're not washing your body in water that's too hot, and limit the amount of time you spend in the shower or bath, or washing your hands. You may also want to avoid certain types of clothing, as wool or synthetics may irritate the skin, as may certain cleaning or cosmetic products.