Baby Acne Explained: Causes, Symptoms, And Treatments
Babies are delicate beings that require our undivided love, attention, and care. They rely on us for safety and stability. As their caretakers, it can be difficult to know what it is they need, especially during the first few months when they are still unable to fully express themselves. A lot of things can happen during the newborn period, and it can be scary for any parent when something unusual happens with their baby.
According to a 2017 article (via StatPearls), compared to adult skin, the skin of newborns is "thinner, less hairy, and has less sweat and sebaceous gland secretions." It is no surprise then, that some of the most common conditions that can be seen in newborns are those that involve the skin. They are the most easily recognizable ones as well. Many types of skin lesions can be seen in babies, such as peeling, discoloration, bumps, bruising, bald spots, skin tags, and moles (per Stanford Medicine). Most of these are benign, but others may be a sign of something more serious.
Acne is a skin condition that is common in teenagers and adults. Surprisingly, babies can develop acne as well. If your baby was born with acne, or they got it within weeks after they were born, don't worry — they may have a relatively common condition called baby acne (which is not to be confused with "bacne", a term used to describe acne on the back).
What is baby acne?
Baby acne has many alternate medical names, including neonatal acne and neonatal cephalic pustulosis (via UtahDERM). It is a common type of skin condition that often appears around 2 weeks old, but it can also be seen in babies at birth, or until 6 weeks of age (via Enfamil). It is a short-term condition that can affect up to 20% of healthy babies in the United States.
The exact cause of baby acne is still unclear, but there are a couple of theories. According to Cleveland Clinic, baby acne may be due to changes in your baby's hormones caused by the placenta. The placenta may increase the production of sebum, which may clog skin pores and cause acne if produced in excess. Hormones present in breast milk may also affect your baby's skin, but this should not in any way stop you from breastfeeding them. In addition, contrary to what some people may believe, kissing your baby on the cheeks will not cause them to develop acne.
With that said, the Department of Dermatology in the University of Utah School of Medicine disagrees that baby acne is caused by excess sebum (per UtahDERM). There is evidence that baby acne may be an inflammatory reaction to the yeast Malassezia, although this requires more research. Regardless of how it develops, baby acne should not be a cause for concern. It is a benign, harmless condition that typically goes away on its own.
Signs and symptoms of baby acne
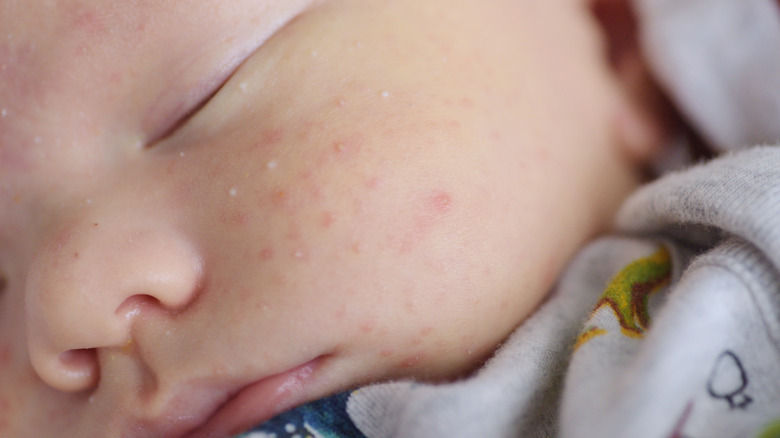
It may be difficult to distinguish baby acne from other skin conditions that can develop in newborns. In general, baby acne appears as small, red or white bumps on the face (per Healthline). It is often seen on the cheeks, and can sometimes develop on the upper back and neck as well. You may see white pustules or whiteheads, and the surrounding skin may be red. The lesions may last for days, weeks, or sometimes even months.
Cleveland Clinic adds that aside from the face, neck, and upper back, baby acne can also develop on the scalp. The lesions seen in baby acne can suddenly or slowly appear, and begin as dots that may progress to pimples. As time passes, the redness will slowly go away and the lesions will start to shrink. Unlike adult or adolescent acne and other skin conditions, baby acne completely clears, and does not lead to permanent scarring on your baby's skin. It also is not known to increase your baby's risk of developing acne when they start undergoing puberty (via What to Expect).
Diagnosis of baby acne
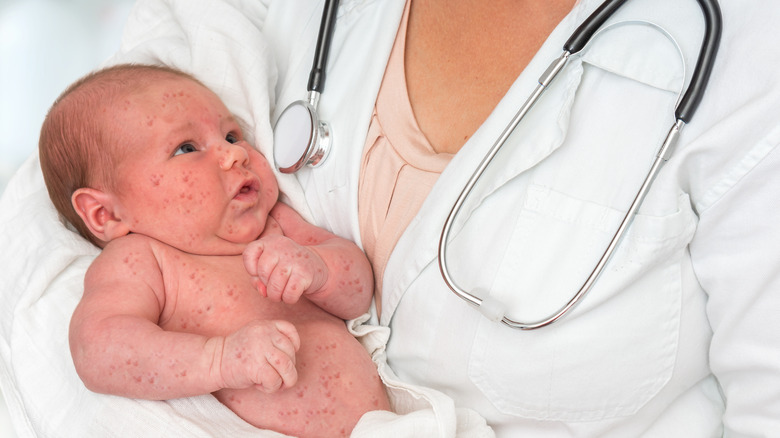
A doctor will typically be able to diagnose baby acne by closely examining your baby's lesions and asking you about certain things such as when it first appeared, how it initially looked, how it has progressed since, and what, if anything, has worsened or improved the lesions. This will help your baby's doctor rule out other possible causes for your baby's skin lesions. According to Mayo Clinic, diagnostic tests are not usually needed, unless your doctor is suspecting the lesions may be caused by something else.
It is important to remember that your baby's doctor is not only there to examine and treat your baby, but also to answer any questions or address any concerns you may have as a parent and caretaker. Cleveland Clinic suggests that you ask your baby's doctor certain questions during your appointment. These include asking them how you can help get rid of your baby's acne, what kind of skincare products you should and shouldn't use on your baby, how often you should apply medicine on your baby's skin (if any), and if there are any side effects to any of the medications they prescribe for your baby.
Medical and at-home treatments for baby acne
Treating baby acne is usually not necessary, since the lesions typically go away on their own. However, if your baby's lesions are persistent, a doctor may prescribe a medicated cream or ointment for you to put on your baby's skin. You should never use over-the-counter medicated products, as well as any facial washes or moisturizers, without consulting your baby's doctor first (via Healthline). A baby's skin is not built to tolerate products for older children or adults, and using these products may lead to more harm.
You can ask your baby's doctor for advice on what you can do at home to help with your baby's acne. According to Mayo Clinic, some of the things you may do include making sure that your baby's face is always clean; drying your baby's face gently by patting it dry; and avoiding manipulating (e.g., pinching, scrubbing, picking) your baby's lesions, as this can lead to further irritation and may even cause an infection. Wash your baby's face daily with warm water. You can use plain water one day then water with a mild, moisturizing soap the following day.
Per Pampers, you should avoid letting your baby's skin come into contact with sheets, blankets, or clothing that may have harsh laundry detergent residue, as this can irritate your baby's delicate skin. You can follow this by using laundry detergent that is specifically used for babies, or by placing a properly washed blanket under your baby's head.
When to seek professional help for baby acne
Baby acne usually clears on its own, but if your baby has persistent lesions (ie, has not gone away after several months), or if they develop acne past 6 weeks old, it may be a good idea to have it checked by a pediatrician or dermatologist (per Babycenter). Your baby's doctor will also most likely notice these lesions during your child's well-baby visit, but you should still bring it to their attention in case they miss it.
While waiting for baby acne to clear up, observe your baby for any signs of inflammation, presence of blackheads, or development of pus-filled lesions. These may be indicative of an infection. It is also important to speak with your baby's doctor if your baby develops acne shortly after getting sick or taking medication. The underlying cause is unlikely to be baby acne, but may be something more serious (e.g., drug allergy, childhood exanthems).
According to WebMD, when you seek help for your baby's skin lesions, you will most likely be asked by your baby's doctor about any family history of acne, as well as what products and medications you have used on your baby's skin. To help ensure that your doctor has all the information they need, be sure to take note of any products you have used beforehand. As a general rule, however, you want to avoid applying anything to your baby's skin without consulting with your baby's doctor first, as not all products are safe for use in newborns and infants.
Difference between baby acne and infantile acne
According to the American Academy of Dermatology (AAD) Association, infantile acne develops in babies past the age of 6 weeks, typically appearing between their 3rd and 6th month of life. While infantile acne can clear on its own, it can leave permanent scars on your baby's skin, and may persist until adolescence. This is why unlike baby acne, infantile acne may be a cause for concern, and should be examined by a specialist (ie, board-certified dermatologist or pediatric dermatologist).
A 2022 article published via StatPearls explains that infantile acne may be related to a person's genetics, and may also be caused by increased sebum production as a response to circulating androgens in the body. Because of greater androgen production, male infants are more likely to develop infantile acne compared to female infants. Unlike baby acne, infantile acne is not that common, and affects less than 2% of children in the United States. However, it usually develops quickly, presents more severely, and may be accompanied by other symptoms (e.g., abnormal and excessive body hair, enlarged testicles in males, enlarged clitoris in females). These symptoms are rare but may be caused by a tumor in the adrenal gland, which is another reason why further evaluation is usually necessary with infantile acne. Although there is currently no approved treatment, infantile acne is often managed similarly to acne vulgaris if the lesions do not resolve on their own within six months to a year.
Baby acne versus milia
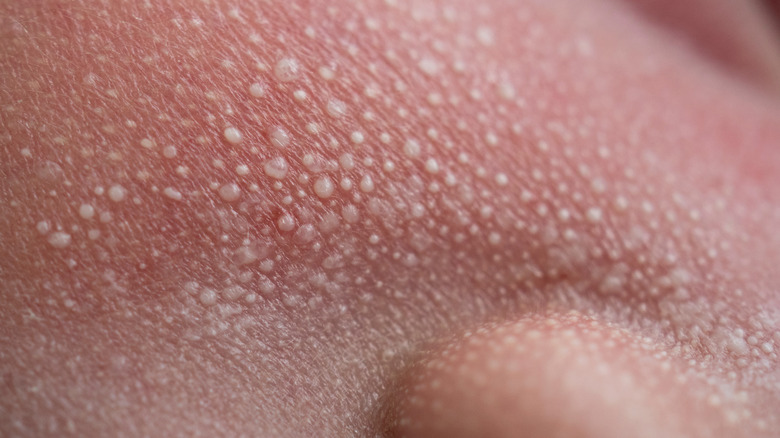
Milia or milk spots look similar to baby acne, and are not at all related to breastfeeding or formula-feeding (via Flo Health). They are small, pinpoint white or yellow bumps that develop on the face; most notably on the nose, chin, cheeks, or eyelids. They may also appear on the chest, arms, legs, and genital area.
While not contagious, anyone at any age can develop milia, especially newborns. Milia that form during childhood or adulthood develop on skin that has been damaged (e.g., acne, burns, rashes, drug reaction), but milia in newborns appear on healthy skin. Unlike baby acne which may be caused by excess sebum or infection from Malassezia, milia result from an accumulation of keratin debris (per Entirely Kids Pediatrics). They become trapped and form clusters, which are the tiny bumps that you see under the skin.
According to Stanford Medicine, milia can be seen in up to 4 out of 10 newborn babies. They are usually evident as soon as a baby is born, and although it is possible for baby acne to also be present at birth, baby acne more often develops in newborns after 2 weeks old. It is also less likely for milia to show signs of inflammation (e.g., redness) compared to baby acne. However, similar to baby acne, milia should not be manipulated in any way, as this can prevent its resolution and may lead to infection. Treatment is also unnecessary, because the lesions typically go away on their own.
Baby acne versus miliaria
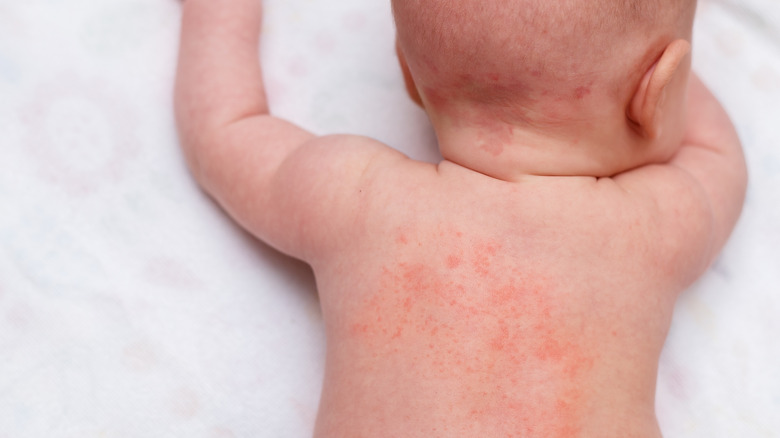
Miliaria sounds very similar to milia, but they should not be confused with one another. The former is also called heat rash or prickly heat because it occurs when sweat becomes trapped under the skin, causing irritation that leads to itchy, prickly skin (via Medical News Today). Similar to milia, anyone can experience miliaria, but babies are particularly prone to this due to their underdeveloped sweat ducts.
There are three different types of miliaria, categorized based on severity. According to a 2022 article published via StatPearls, miliaria crystallina develops on the superficial layer of the skin. They easily rupture, and look like water droplets without any signs of inflammation. They can be seen in babies usually less than 2 weeks old, and may appear on the upper trunk, head, and neck. They typically clear quickly, often within one day. On the other hand, miliaria rubra (the most common type) involves deeper skin layers and can show signs of inflammation. They are tiny, red bumps that can sometimes become infected and fill with pus (miliaria pustulosa). They are usually seen in babies between 1 to 3 weeks old, and may appear on the neck, armpits, and groin. Lastly, miliaria profunda involves even deeper layers of the skin and can be seen as skin-colored bumps. They are not typically seen in babies. Similar to baby acne and milia, miliaria usually clear spontaneously without any treatment.
Baby acne versus eczema
Eczema is a group of conditions that present with dry, itchy skin. Although it can be linked to autoimmune disease, eczema can present on its own and is not in itself an autoimmune condition (via Medical News Today).
According to Cleveland Clinic, around 15% to 20% of babies younger than 2 years old have eczema in the US. The location and appearance of the rash can differ depending on the type of eczema and a person's age, but in general, babies up to 6 months old have eczema on their cheeks or foreheads, manifesting on their knees, skin creases, or elbows as they age (per Healthline). It is still unclear how people develop eczema. Experts believe that it is an interplay between family history and the environment they are exposed to (via the National Eczema Association). Common triggers of eczema include dry air, allergens (e.g., pet dander, dust mites, detergents), and certain skincare products.
According to Mayo Clinic, babies with eczema should be bathed daily with a mild cleanser and warm water for less than 15 minutes. After gently drying, a fragrance-free moisturizer (e.g., petroleum jelly) should be applied. Moisturizing should be done at least twice a day. It is also important to identify and avoid irritants, and prevent your baby from scratching their skin by clipping their nails or using cotton mittens on their hands as they sleep. Although most children outgrow their eczema before the age of 6, it can still persist into adulthood.
Can skin infections cause baby acne?
Baby acne may possibly be linked to an infection with Malassezia, but other skin infections are not known to cause baby acne. Rather, the lesions seen in some skin infections may resemble and be confused with baby acne.
Hand, foot, and mouth disease (HFMD) presents with red blisters on the hand, foot, and mouth (per Healthline). It is commonly seen in children below age 5. Unlike baby acne, the lesions are often accompanied by other symptoms such as fever, drooling, irritability, decreased appetite, and headache. No treatment is necessary as the viral infection resolves within 7 to 10 days, but your baby's doctor may prescribe medicines that can help ease your child's symptoms.
Herpes, another viral infection, is rare in babies but can be very serious. Sometimes however, babies with neonatal herpes develop only cold sores around their mouth, which may be confused with acne (via Medical News Today). Similar to herpes in adults, it is a lifelong infection where lesions may come and go. Antiviral medications are used only to help treat cold sores, not to completely eradicate the infection.
Another skin infection that can resemble baby acne is scabies, caused by a mite that burrows into the skin. According to the Centers for Disease Control and Prevention (CDC), the itchy rash of scabies may resemble pimples and can develop on the face, neck, palms, and soles in infants. However, the rash is usually located elsewhere in adults and older children.
Differences between neonatal acne, erythema toxicum neonatorum, and transient neonatal pustular melanosis
Both neonatal (baby) acne and erythema toxicum neonatorum (ETN) are common, harmless skin conditions that can be seen in newborns. Authors from a 2022 paper (via StatPearls) describe ETN lesions as yellow-white bumps with a surrounding area of redness that may appear on the cheeks. These can quickly spread to the forehead, other parts of the face, chest, trunk, and limbs. It can be seen in up to 72% of full-term babies, and is more commonly observed in males than females. Although pus-filled bumps can form, no organisms are usually detected on culture and staining. It is still unclear how babies develop ETN, but it is believed to be a reaction of the baby's skin to meconium (baby's first stool). It may also be a result of an immune response to the mother's white blood cells or microorganisms on hair follicles.
On the other hand, transient neonatal pustular melanosis (TNPM) can also present at birth as pigmented bumps with or without pus, but is distinguished by the absence of surrounding areas of redness and its predilection to the palms and soles. According to the American Academy of Family Physicians (AAFP), it is less common compared to baby acne and ETN, and when a lesion ruptures, it leaves a circular rim of loose skin and a dark spot that clears over three to four weeks. Baby acne, ETN, and TNPM usually go away on their own without treatment.
Cradle cap and red patches on your baby's face
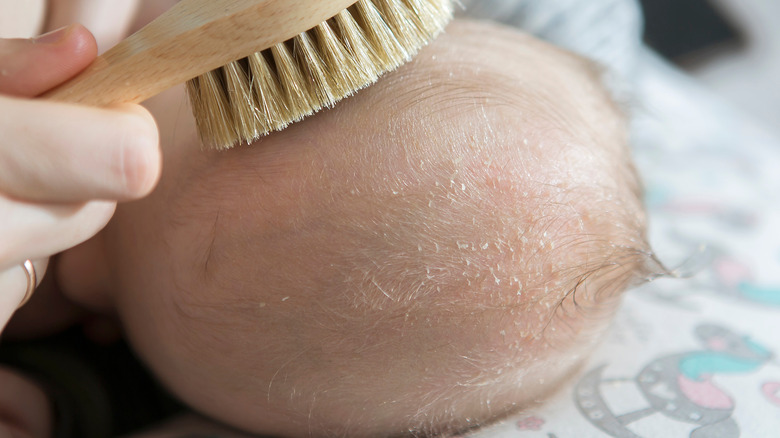
Cradle cap is the term used to refer to seborrheic dermatitis (dandruff) that forms on the scalp of babies (via Pampers). It causes flaky, greasy skin with yellowish crusting and an accompanying rash that may appear red, yellow, brown, purple, or gray. Cradle cap is not contagious and is usually not itchy nor painful. It typically resolves spontaneously within weeks or months, but in some cases, it may recur during puberty. This condition can be seen in babies between 2 weeks old to 12 months old. Aside from the scalp, it can also involve the face, back of the ears, neck, and armpits.
Treatment for cradle cap is not usually necessary, but if your baby has it, there are several things you can do at home to help. According to Healthline, you should use gentle shampoo when washing your baby's hair and scalp, but you should avoid washing them too often, as this can dry out their skin. You can use baby oil to soften the crust that forms on your baby's scalp and brush it out gently with a soft hairbrush. Mayo Clinic adds that if these don't help, consult with your baby's doctor and ask them what products you can use. They may prescribe a medicated shampoo or cream. It is important to remember that you should never use over-the-counter products that are not recommended by your baby's doctor, as not all of them can be used on your little one.
Other common rashes in newborns
According to Stanford Medicine, Mongolian spots are harmless, blue-gray lesions found most often on the lower back and buttocks of darker-skinned babies. They may resemble bruising (albeit not as colorful) and typically fade over time, but may not completely go away. Salmon patches or "angel kisses" are flat, pink lesions on the face, most commonly on the forehead. They are caused by abnormal capillaries, but also typically clear on their own.
On the other hand, port wine stains are purplish-red patches that are innately harmless but can signal the presence of a congenital or structural disorder (e.g., Sturge-Weber syndrome, spinal dysraphism). Therefore, unlike Mongolian spots of salmon patches, they require further evaluation. Sebaceous hyperplasia looks similar to milia, but the pinpoint bumps that develop are more yellow and are caused by exposure to maternal androgens in the womb. Similar to baby acne and milia, sebaceous hyperplasia is harmless and does not require any intervention.
Another harmless rash is teething rash or drool rash, which develops when the baby's skin reacts to drool (via Healthline). When babies start teething, they produce more drool, and when their skin is constantly exposed to saliva (as well as food remnants), it becomes irritated and develops a rash. It can also be worsened by friction from their clothing. You can prevent teething rash by making sure that your baby's skin stays clean and dry.
How to properly care for your baby's skin
Unlike children and adults, babies usually do not need to be bathed every day. Instead, two or three times a week should be more than enough. Of course, this does not include diaper changes and cleaning up after feeds, which should be done several times a day. According to the University of Rochester, you can give your baby a bath any time of the day. Initially, sponge baths are recommended, at least until your baby's umbilical stump has fallen off on its own. If you have a baby boy and had him circumcised, you should also wait until the wound has completely healed to prevent infection. After this, you can give your baby a tub bath.
During a sponge bath, make sure the room is warm without any wind drafts to avoid your baby getting cold. Use a clean, soft, moist washcloth and uncover your baby only one area at a time. You can use a small amount of baby soap for their body and wash their head last with shampoo. Once you are done, wrap your baby in a warm towel. The same principles apply when you give your baby a tub bath. Make sure to use warm water and never leave your baby alone. When it comes to skincare products, avoid heavily scented products, even if they are marketed for babies. When washing their clothes or bedding, only use baby laundry detergents that are free from fragrances and dyes (via WebMD).