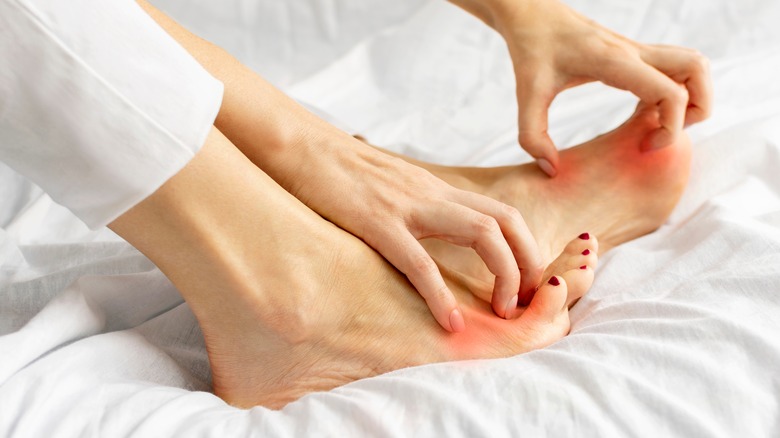
What It Really Means If You Have Itchy Feet At Night
While itchy feet can be annoying, it's usually nothing to be alarmed about, per Healthline. Often, feet can become itchy from exposure to moisture (e.g., sweat), dry conditions, or irritants from walking barefoot. However, itchy feet may also be a sign of something more pressing, such as an underlying systemic disease or skin disorder. Peripheral neuropathy, cancer, liver disease, kidney disease, and thyroid disorders are a few of the conditions that may cause feet to itch. Skin disorders that may be associated with itchy feet include dry skin, psoriasis, eczema, scabies, athlete's foot, and allergic contact dermatitis.
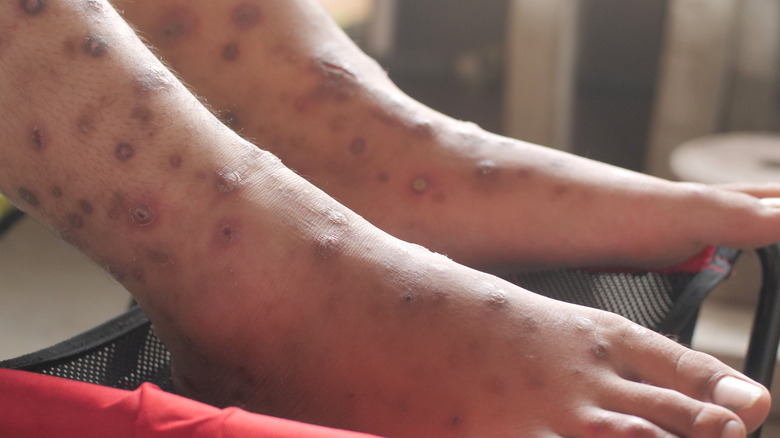
In some people, feet can become itchy without any visible skin changes. Others may experience redness, swelling or blisters on their itchy feet. The skin on your feet may also be cracked or appear dry and scaly. Treatment of itchy feet primarily involves topical or oral medications that relieve the itch. Emollients (like petrolatum) and steroid creams can suppress itching on the skin surface, while antihistamine pills work systemically. Anti-fungal sprays and creams, as well as prescription medications, can be used to treat fungal infections such as athlete's foot. If you're curious about the possible reasons why you experience itchy feet at night, keep reading.
Types and causes of itchy skin
Itching in general can be categorized according to the cause (via Medical News Today). While cutaneous itching (e.g., allergic reactions, scabies) is related to a condition in or on the skin, systemic itching emanates from a disorder that affects the entire body (like diabetes or liver disease). Neuropathic (e.g., peripheral neuropathy) and psychogenic itchiness are associated with the nervous system and psychological issues, respectively. Most cases of itching, however, involve a combination of these factors.
According to a 2019 review of studies published in the Journal of Allergy and Clinical Immunology, roughly 15% of the general population suffers from chronic pruritis — the medical term for itching. Itching mediated by histamine is well-established. Histamine is released from immune cells called mast cells when they are activated by (such as allergic reactions). Histamine subsequently binds to its receptors (docking stations) on nerve cells in the skin to cause the itching sensation.
Many itching disorders do not respond well to antihistamines, suggesting that factors other than histamine play a role in the mechanism underlying itching. Several mediators of itching have been identified, including the neurotransmitter serotonin and various molecules involved in the inflammatory response, like prostaglandins and leukotrienes.
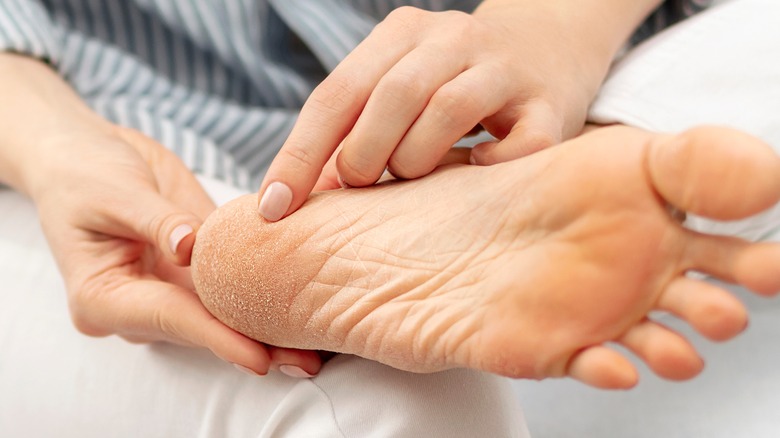
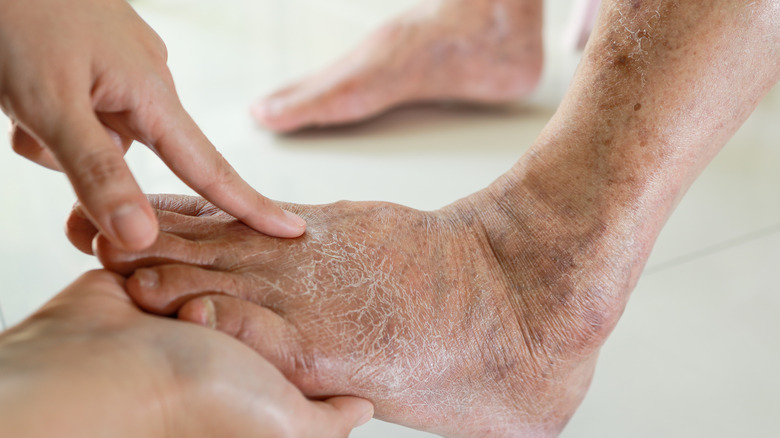
Dry skin on the feet
Your skin contains sebaceous glands (oil glands) that secrete sebum to help retain moisture and prevent dryness, reports the Cleveland Clinic. Since, for the most part, sebaceous glands are hitched to your hair follicles, they are absent from the hairless soles of your feet. Thus, the bottoms of your feet are devoid of the protective effect of sebum which, along with daily wear and tear, can lead to dry, cracked, and flaky skin (via Medical News Today). Though usually harmless, dry skin on the heel and sole, as well as on the sides of your feet and between the toes, can become itchy.
Dry and calloused skin on the feet can also result from wearing poorly fitting shoes that cause skin irritation, or from wearing closed shoes that generate heat and humidity. Harsh chemical in some soaps and body washes as well as certain medications (e.g., diuretics) can also dry out the skin on the feet. Unfortunately, aging takes its toll on your feet as well. Older people are more prone to dry skin as natural hydration of the skin diminishes with age.
People with athlete's foot often have dry, scaly skin between the toes. Other skin conditions such as psoriasis and eczema are commonly associated with dry skin anywhere on the body, including the feet. Some people with diseases such as diabetes and hypothyroidism can also experience dry or cracked skin on the feet.
Psoriasis
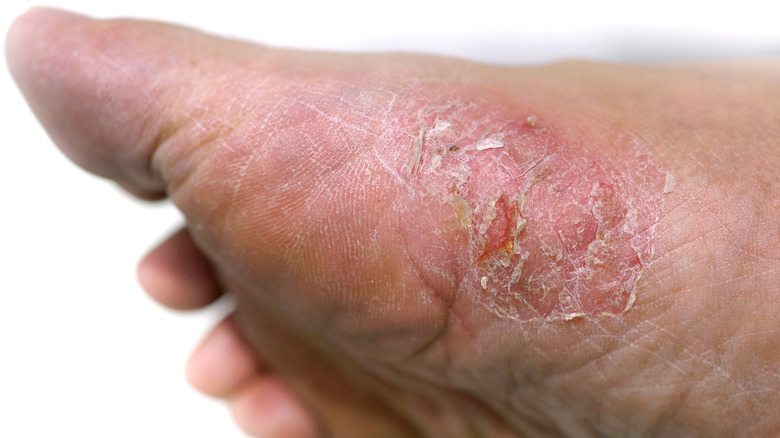
Psoriasis is a skin condition characterized by thick patches of red, scaly, discolored skin that are itchy and uncomfortable (via the Cleveland Clinic). Psoriasis is an autoimmune condition whereby the immune system overreacts and mistakenly attacks skin cells, causing them to become swollen and inflamed. They appear on the skin surface as scaly, flaky plaques that shed easily. While psoriasis often occurs on the elbows, knees, and scalp, it is also common on the feet.
According to the National Psoriasis Foundation, the symptoms of chronic foot psoriasis can be particularly intense and distressing, even life-altering. The discomfort associated with foot psoriasis can be likened to having a hangnail or a blister on a foot. People with a specific form of psoriasis (palmoplantar) on the soles of the feet often have difficulty with mobility and performing daily activities (via a 2018 article published in the Journal of the Dermatology Nurses' Association). This can lead to a diminished quality of life.
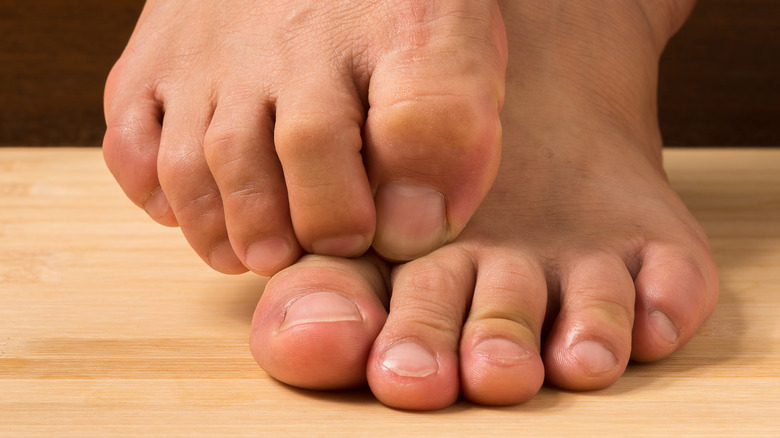
Athlete's foot
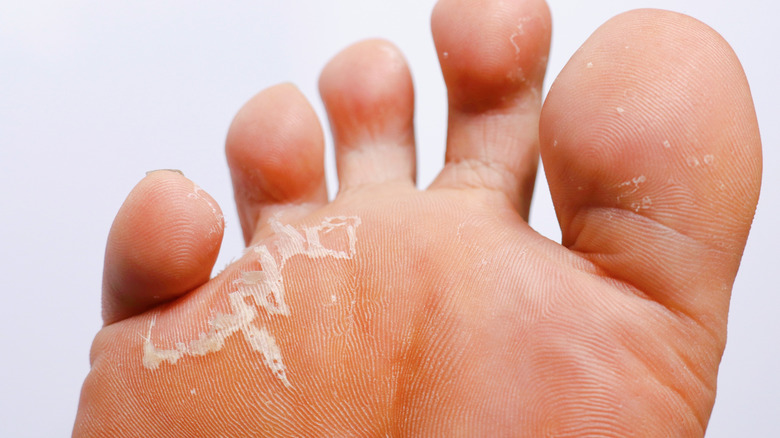
Athlete's foot (medically known as tinea pedis) is a fungal infection of the skin on the feet, occurring typically between the toes (via the CDC). It can be spread via direct contact with the infected person or exposure to the fungus in damp environments where it thrives (such as showers, locker rooms, and swimming pools). Athlete's foot often comes and goes and is treated with anti-fungal medication, either topical or oral.
Itchy skin is a common symptom of athlete's foot. The itching is more intense immediately after removing shoes and socks. Other common signs and symptoms of athlete's foot include skin that is dry, inflamed, discolored (reddish, purplish, or grayish), peeling, burning, or stinging. The skin between the toes or on the bottom of the foot may have scales, fissures, or blisters. Sweaty feet enclosed in tight-fitting shoes creates an ideal moist environment for the infection and spread of athlete's foot.
Eczema
Itchy feet can also be caused by eczema (via MedlinePlus). Like athlete's foot, eczema is marked by dry, itchy skin, though it is not contagious. Scratching the skin can aggravate the condition and cause the itching to intensify. The cause of eczema is undetermined, though genetic and environmental factors likely play a role. It is often associated with a history of hay fever (pollen allergies) and asthma.
Apart from the feet, eczema can also occur on the face, hands, inside the elbows, and behind the knees. Atopic dermatitis is the most common type of eczema, and is predominantly seen in infants and children. Eczema can be treated with oral drugs, topical creams, light therapy, avoidance of skin irritants and allergens (e.g., foods, pollen, animals), and stress management.
In addition to being dry and itchy, the skin of people with eczema can be flaky, scaly, or crusty. It can also appear as thick and leathery patches, bumps, or swelling. Depending on skin tone, eczema can cause skin discoloration, making it appear pink, red, purple, brown, or even gray.
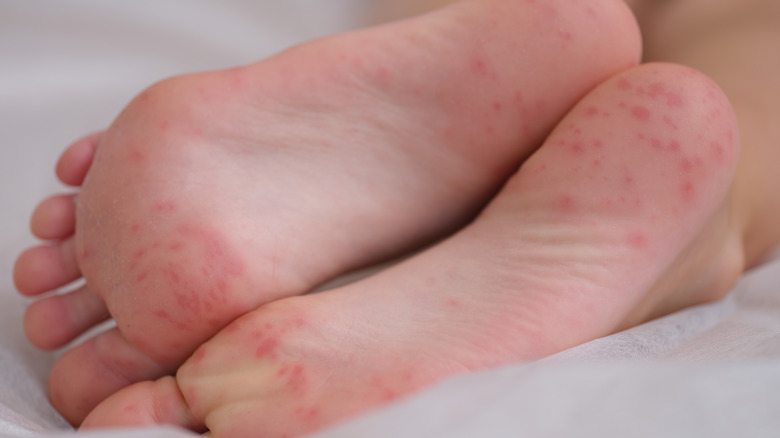
Allergic contact dermatitis
Allergic contact dermatitis occurs when a substance contacting the skin triggers an exaggerated response by the immune system that results in skin inflammation and intense itching (per the Merck Manual). The skin (including the skin on the feet) of an allergic person must first become sensitized to the offending substance through one or more contact exposures. Upon subsequent exposures to the substance, itching and other symptoms become noticeable within 4 to 24 hours, or they may be delayed for up to 3 to 4 days.
Included among the most common substances that cause allergic contact dermatitis are latex rubber and metals, particularly nickel, which is found in most jewelry. Preservatives, fragrances, and plants (e.g., poison ivy) can also be allergenic in some people. Sometimes, even the topical medicines used to treat dermatitis can provoke a reaction on the skin. Substances that are tolerated well for years can suddenly become reactive. Photoallergic reactions can also occur whereby exposure to both a particular substance and sunlight causes dermatitis. This type of sun-induced skin reaction is often associated with fragrances (e.g., musk, sandalwood), antiseptics, NSAIDs, and sunscreens.
Symptoms of allergic contact dermatitis include a red rash, itching, and dry skin. In some cases, more severe symptoms such as pain, swelling, and blisters on the skin may occur. An itchy rash can also appear in areas of the body (including the feet) that were not in contact with the offending substance.
Neuropathic itch
According to a 2018 review of studies published in Seminars in Cutaneous Medicine and Surgery, neuropathic itch is a type of chronic itch that results from a malfunction of itch-sensing nerve cells. Nerve damage in either the peripheral nervous system (PNS) or central nervous system (CNS) can lead to neuropathic itch. Nerve disorders that are associated with pain (e.g., shingles) can cause itching in lieu of pain, or in addition to pain. In particular, a type of peripheral neuropathy known as small-fiber polyneuropathy (SFPN) begins in both feet. Damage to small nerve fibers in the skin is most often caused by diabetes and prediabetes, as well as impaired glucose tolerance (elevated blood glucose following meals).
Apart from itching that can be severe, neuropathic itch can cause a sensation of "pins and needles." Other manifestations of neuropathic include numbness, burning, wetness, and electric shocks. Some people with the condition may experience sensations of crawling, prickling, or chilling of the skin. In others, the skin may become either more sensitive or less sensitive. Constant and vigorous scratching may not alleviate the itch; rather, it may cause worsening of the itch and unintentional self-injury.
Diabetes
Itching is a common symptom among people with diabetes, primarily affecting the lower extremities including the feet (via a 2021 study in Biology). Based on current evidence, poor diabetes control leads to dry skin and diabetic neuropathy (nerve damage) which, in turn, trigger itching of the skin. In participants with diabetes, fasting blood glucose levels were shown to be significantly higher in those who were itchy compared with those who did not itch. Fasting blood glucose as well as hemoglobin A1c (average blood glucose) levels correlated with neuropathy, which was more prevalent among participants who were itchy.
One explanation for the dry skin seen in people with diabetes is the formation of advanced glycosylation products in the collagen of the skin. Also known as advanced glycation endproducts (or AGEs), these compounds, formed as a result of the bonding together of glucose and proteins in the body, decrease the production in the skin of hyaluronic acid, a skin moisturizer (via a 2022 review article published in Frontiers in Medicine).
Dry, itchy skin on your feet or other body parts can be an early sign of elevated blood glucose, and possibly undiagnosed diabetes or prediabetes. It can also be an indicator of poor blood glucose management in a person with diabetes.
Liver disease
Itchy feet at night may be a sign of certain types of liver disease, notes a 2015 review published in Clinical Medicine (Lond). Itchiness is frequently associated with cholestatic liver diseases such as primary biliary cirrhosis, primary sclerosing cholangitis, and intrahepatic cholestasis of pregnancy. In these conditions, the flow of bile from the liver is blocked or slowed, resulting in buildup of bile acids in the bloodstream and various tissues. Bile acids and/or their metabolites then stimulate itch-sensing nerve fibers in the skin, which signal the brain and spinal cord.
This type of itch caused by the accumulation of bile acids is known as cholestatic pruritis, and most often affects the soles of the feet (and palms). It is most intense in the late evening and early nighttime. While scratching provides minimal itch relief, vigorous scratching can worsen the condition and cause major damage to the skin. In most cases, the itch is mild and bearable. However, some experience a very harsh and incontrollable itch that affects their quality of life. They may suffer from insomnia, cognitive problems, mood changes, anxiety, and depression.
Cholestyramine is the first-line treatment for itching related to the buildup of bile. This medication binds with bile acids to prevent their reabsorption and promote their excretion via the feces. Although cholestyramine significantly reduces itching, its use is limited by its nasty taste and potential side effects (like diarrhea or constipation). Overall, treatment with multiple drugs is often necessary in current therapies for cholestatic pruritis.
Scabies
Scabies is a itchy, skin condition that develops when a mite burrows into the skin where it lives and lays its eggs, reports Medical News Today. Any part of the body, including the feet, can be affected by scabies. The scabies mite is spread by skin-to-skin contact with a person who has scabies. Treatment with topical prescription medicines usually leads to resolution of scabies.
The most frequently occurring symptom of scabies is severe itching, mostly at night. In some instances, the itching is so fierce that sleep is disrupted. Many people with scabies develop a pimple-like rash on the skin; in others, scabies may take on the appearance of scaly, eczema-like patches. Crusted scabies (or Norwegian scabies) is a severe form of scabies marked by diffuse thick crusts on the skin that break up easily upon touching. It occurs in people who are immunocompromised (like the elderly) and involves hundreds to thousands of mites in the skin (a far cry from 15 to 20 mites associated with regular scabies). Some people with scabies scratch their skin incessantly. This non-stop scratching can cause an infection and even sepsis, a potentially fatal condition that occurs when the blood is poisoned by bacteria.
Thyroid problems
According to a 2015 review of studies published in The Scientific World Journal, both hyperthyroidism (overproduction of thyroid hormones) and hypothyroidism (underproduction of thyroid hormones) can cause itchy skin. In hyperthyroidism, it has been suggested that an excess of thyroid hormones increases blood flow and skin temperature as well as sensitivity to itchiness.
People with Graves' disease (an autoimmune form of hyperthyroidism) may develop a skin condition known as pretibial myxedema (via the Cleveland Clinic). Pretibial myxedema typically appears as itchy patches of thick, scaly plaques on the lower legs and feet. Edema (swelling) and nodules (firm lumps) beneath the skin are present as well. The skin looks shiny and waxy, and its color can change from yellow and orange to brown and red to purple.
Itchiness in people with hypothyroidism is likely related to dry skin, per Fox News. A slowed metabolism resulting from lower levels of thyroid hormones may reduce sweating. Less sweating means less skin hydration and dry skin.
Treatment of itchy feet
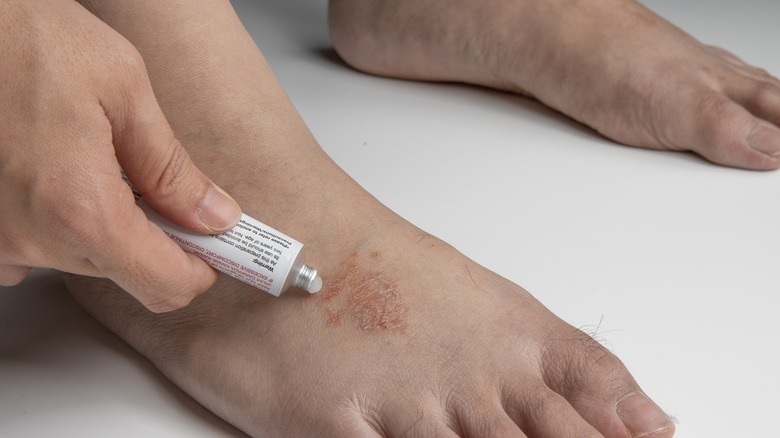
Treatment of itchy feet primarily depends on the specific cause (via Healthline). For example, itchy feet caused by an allergic reaction is resolved by staying away from the offending allergenic substance. Mild cases of itchy feet can be treated with topical antihistamines or steroid creams such as Benadryl. Oral antihistamines are also effective; however, they can come with adverse effects (like sedation) and may be too risky for the elderly.
While some people with athlete's foot may find relief from using antifungal sprays or creams, others may need prescription strength medications to get rid of the fungus. In mores severe cases of itchy feet, stronger medicines such as SSRIs (e.g., Paxil, Prozac), gabapentin (Neurontin), or tricyclic antidepressants (e.g., amitriptyline) may be warranted.
Apart from avoiding scratching, various home remedies may also be used to treat itchy feet, reports Medical News Today. Cooling the feet may help lessen the itch. This can be achieved by applying menthol, calamine, ice packs, or cold, wet cloths to the feet. Consistent use of moisturizers can prevent skin from drying out. Also, topical anesthetics containing pramoxine or an oatmeal bath (1 cup ground oatmeal in warm water) can be very soothing for the skin.