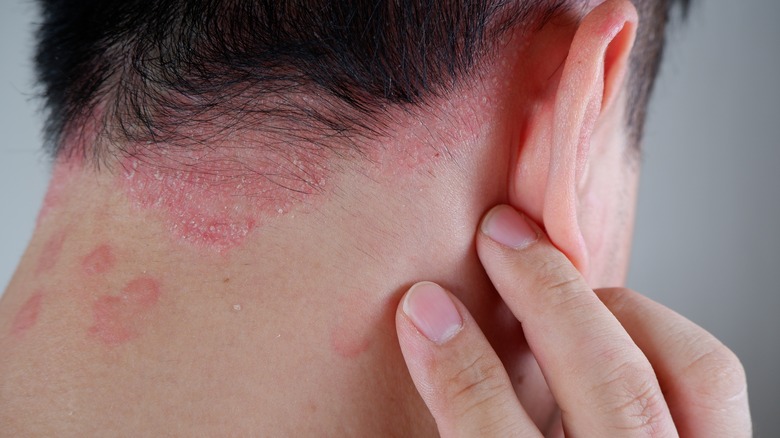
Psoriasis Explained: Causes, Symptoms, And Treatments
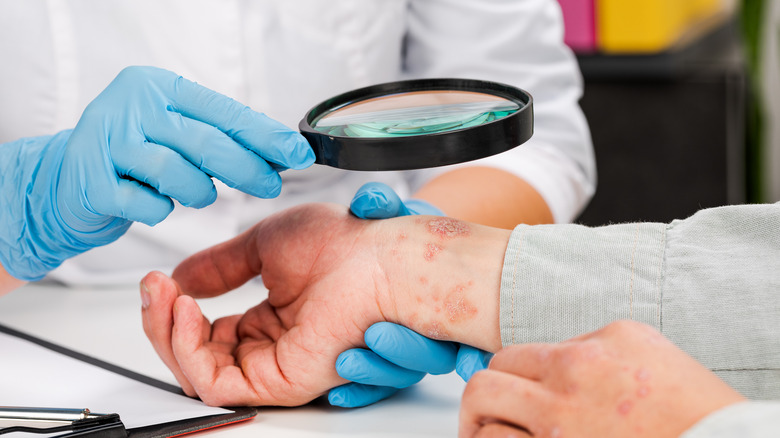
One of the most commonly presented skin disorders, psoriasis is an autoimmune condition that causes inflammation in the body. It shows up in the form of red, itchy, scaly patches that can form pretty much everywhere. According to the National Psoriasis Foundation, it affects more than 7.5 million U.S. adults, with differences in intensity and severity of symptoms.
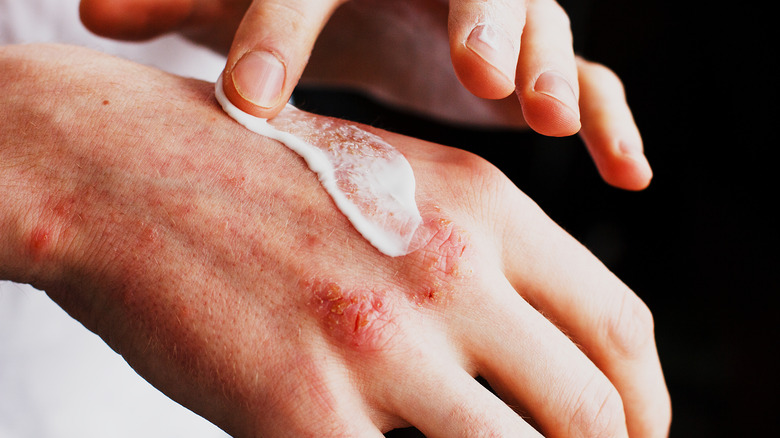
The skin usually sheds on a monthly basis, but psoriasis speeds up this process. What would typically take a month occurs in just three to four days — and instead of falling off, the dead skin cells pile up on top of the skin, creating plaques which then get easily inflamed. These plaques can appear practically anywhere on the body, but they usually show up on the knees, elbows, trunk, and scalp.
Unfortunately, autoimmune diseases are chronic diseases with no actual cure, but that doesn't mean they can't be managed and controlled. The plaques themselves aren't as dangerous, but if left untreated, the inflammation caused by psoriasis can affect organs and other tissue, potentially spreading inflammation all over the body and causing more severe health complications (via Mayo Clinic).
Types of psoriasis
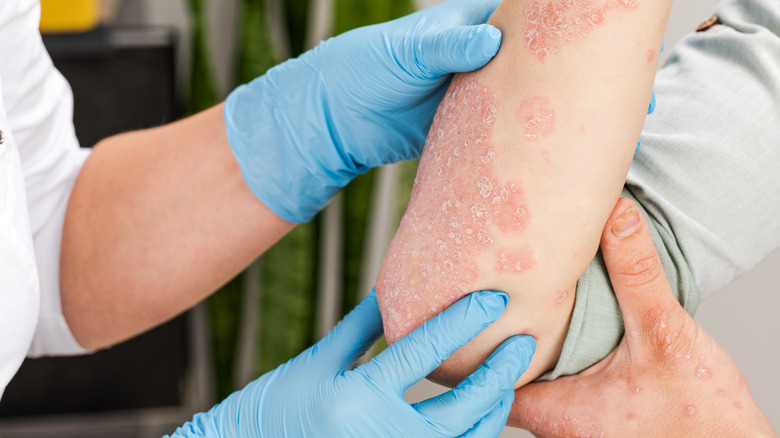
According to WebMD, there are many different types of psoriasis. Depending on which one you're dealing with, you'll probably experience different symptoms, as well as be presented with different treatment options. Plaque psoriasis is the most common kind, and it's characterized by red, itchy plaques all over the skin that might burn and cause skin breakage. It's the type of psoriasis with the most number of treatment options. It's also been said that eight out of ten people with psoriasis suffer from this particular kind.
Guttate psoriasis is quite uncommon, causes small, pink-red spots on the skin, and usually develops in young children. Inverse psoriasis shows up in skin areas that are moist, like armpits and where your skin folds. It's characterized by bright red patches of skin without scales. Pustular psoriasis is also rare and causes pus-filled bumps or pustules surrounded by red skin. Erythrodermic psoriasis is extremely rare, but also very serious. Manifesting in most areas of the body, it tends to resemble patches of red, burning skin.
As the name implies, nail psoriasis alters the appearance of a person's nails. Lastly, psoriatic arthritis is a condition where the inflammation has spread to the joints and caused arthritis. Incidentally, many people who suffer from psoriatic arthritis have nail psoriasis as well.
Signs and symptoms
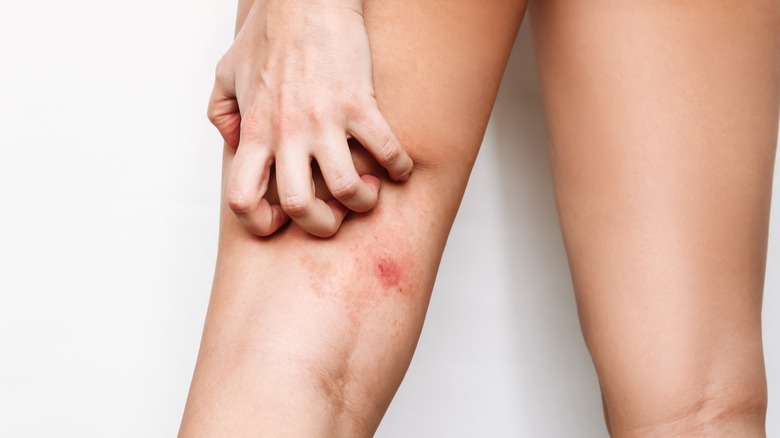
The American Academy of Dermatology (AAD) states that the most common symptoms and signs of psoriasis are red, itchy, dry, raised patches on the skin that are usually covered with white scales. Their size, shape, and spread depend on a myriad of factors, from the type of psoriasis you're dealing with and the level of inflammation to the locations where they present on your body.
Most of these patches are itchy, burning, and in some cases really painful. In the case of pustular psoriasis, if it affects your hands and feet, the pain makes it almost unbearable to walk. In erythrodermic psoriasis, you might experience muscle weakness and a rapid pulse that can be life-threatening.
Since psoriasis can present itself in a variety of different ways, it's important to find ways to manage your symptoms as soon as possible, so that they don't lead to life-threatening complications.
Causes of psoriasis
Experts and medical professionals still cannot find the real cause of psoriasis, even though it's thought to be caused by a disorder in skin cell growth and shedding (via Johns Hopkins Medicine). Something triggers the skin cells to start multiplying at a much quicker rate than normal, making them pile up on top of one another and causing inflammation in the process. Psoriasis is not contagious, but it can be genetically transmitted. It can sometimes go into remission, but certain triggers (like stress, injury, or infection) can make it come back, often with even stronger intensity.
Like psoriasis, many other autoimmune conditions have still-unknown causes (via MedlinePlus). In such cases, the immune system tends to malfunction and mistake the body's healthy cells for harmful pathogens. We do know, however, that certain microorganisms, toxins, stress, and inflammatory agents can play a role in the development of autoimmune conditions.
Psoriasis triggers
Even though the exact causes of psoriasis are still unknown, experts agree on a number of triggers that can exacerbate the symptoms and bring the flare-ups back even after a case of remission. According to the results of a national survey published in Dermatology and Therapy, among these triggers are specific foods such as gluten, dairy, shellfish, nightshade plants like tomatoes and eggplants, red meat, and sugar. The findings indicated that people who eliminated these foods from their diet saw incredible improvement in their symptoms.
Other identified psoriasis triggers include cigarette smoking, cold and dry climate, stress, certain medications, different kinds of infections such as strep throat, insect bites, and skin injuries, according to the Mayo Clinic. The condition may also be triggered by low estrogen levels in women (per the International Journal of Women's Dermatology), excessive alcohol intake (per a 2010 study), and certain compounds such as taurine and choline (via Psoriasis: Targets and Therapy).
It's important to note that most of these triggers can be monitored, controlled, and even eliminated, even without excessive and intense treatment or medication.
How to diagnose psoriasis
The best way to treat your psoriasis is to know exactly what type and intensity you're dealing with, so that the approach you take toward treating it is as effective and efficient as possible, preventing any complications down the line.
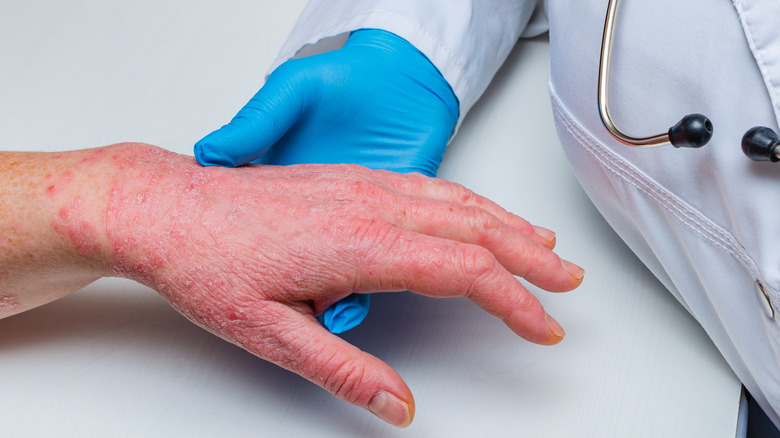
Typically, a dermatologist can diagnose psoriasis with ease via a skin examination. As the AAD explains, an expert in skin health and skin conditions will take a thorough look at your skin and symptoms. They'll also ask you about what you're experiencing (itchiness, burning sensations, pain). Depending on the appearance of your skin and your answers, they will be able to conclude what type and intensity you're dealing with, as well as recommend the right treatment and/or medications.
Sometimes, the doctor will be able to tell you everything just by the look and feel of your skin. In certain cases, however, they might need to take a small piece of your skin and check under the microscope to confirm their thoughts.
Psoriasis treatment
As is the case for autoimmune conditions in general, finding the right psoriasis treatment for you might be challenging and complicated. It may also be completely different from someone else's; what may work for you and the type of psoriasis you have may not work for other patients, and vice versa.
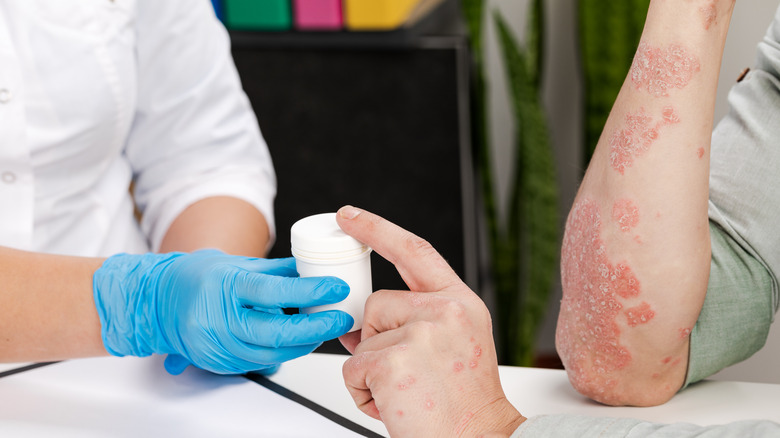
According to the National Psoriasis Foundation, the usual treatment options include topicals (either prescribed or over-the-counter), phototherapy or light therapy (which involves medically supervised ultraviolet light exposure), prescription drugs (usually for more serious psoriasis cases), and complementary and integrative medicine (a blanket term for alternative treatments).
Topicals are usually the first treatment option presented to someone newly diagnosed with psoriasis. However, in situations where the type of psoriasis is more severe, medications and phototherapy may also be recommended. Additionally, it's important to find the right care team for your psoriasis, as the process of treating this condition will most likely be a lifelong one.
Psoriasis medication
When it comes to psoriasis medication, it's usually presented if other treatment options don't yield a positive result. WebMD lists 11 biologic medications that are most commonly used in psoriasis treatment. These include Abatacept (Orencia), Adalimumab (Humira), Brodalumab (Siliq), Certolizumab pegol (Cimzia), Etanercept (Enbrel), Golimumab (Simponi), Guselkumab (Tremfya), Infliximab (Remicade), Ixekizumab (Taltz), Risankizumab-rzaa (SKYRIZI), Secukinumab (Cosentyx), and Ustekinumab (Stelara).
Whether or not your doctor will recommend a biologic medication depends on how much of your skin is affected by psoriasis, how it affects your life, your health history, insurance coverage, and your own preferences. Clinical trials show that certain biologics are really effective in helping treat psoriasis symptoms, lowering their activity by at least 75% in many people (via a 2021 article in Biologics: Targets and Therapy). Unfortunately, they are still very expensive, so if you don't have a good insurance plan, there's a good chance you will still be paying plenty out of pocket.
Alternative psoriasis treatment
While Western medicine has proven to be quite effective in remedying a vast assortment of health conditions, it still has its limitations, particularly with regard to autoimmune diseases. Unsurprisingly, many people turn to alternative treatments and procedures, with the expectation that such methods would help them more than traditional medication or procedures could.
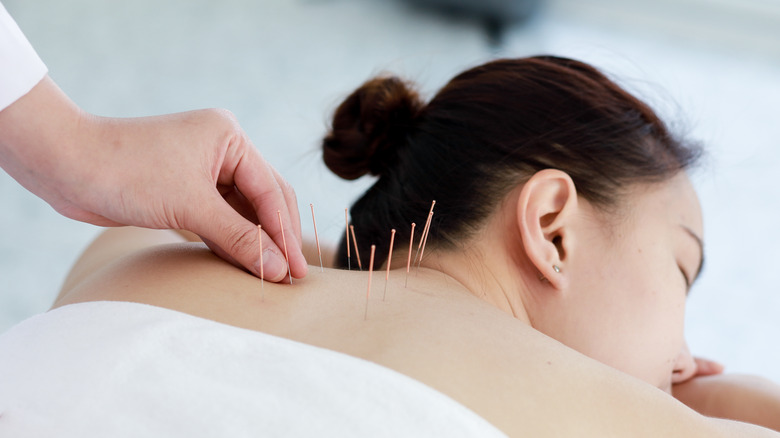
The National Psoriasis Foundation lists a variety of integrative approaches to care which might or might not work (although plenty of people will probably tell you that they're worth trying out). These include rehabilitation, massage, acupuncture, aloe vera, apple cider vinegar, capsaicin, dead sea salts, oat extracts, tea tree oil, turmeric, and mahonia aquifolium. These treatments are based on homeopathy, traditional Chinese medicine, naturopathy, and Ayurvedic medicine.
In addition to these alternative treatments, there are also some lifestyle changes that can have a positive effect on your psoriasis symptoms. These include diet changes, increasing exercise levels, implementing stress-releasing techniques, improving sleep patterns, and abstaining from alcohol and cigarettes.
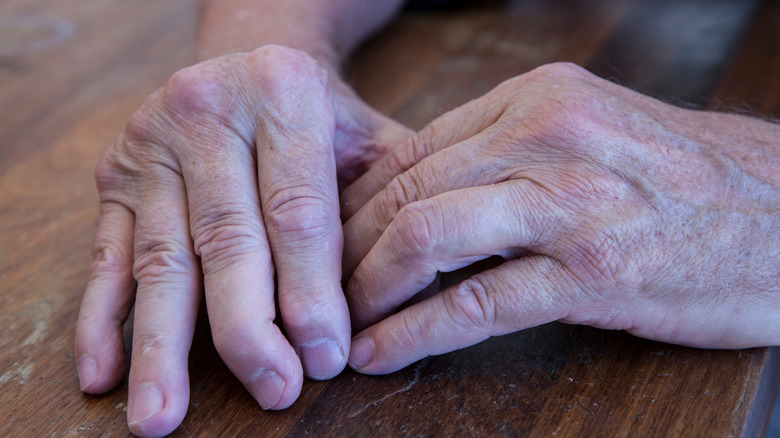
Psoriatic arthritis
A special type of psoriasis is psoriatic arthritis. It's a combination of psoriasis and arthritis that occurs when the inflammation spreads to the joints, causing pain, swelling, and restricted movement (via the National Psoriasis Foundation). It usually appears 10 years after the development of psoriasis, but sometimes it appears a lot sooner. In addition to a good dermatologist, it is extremely important to work with a rheumatologist who can develop the right kind of treatment plan to help prevent the disease from progressing, alleviate pain, protect your joints, and preserve their range of motion.
The most common symptoms include pain and swelling over tendons and joints, swollen digits, a limited range of motion, fatigue, altered nails, and eye inflammation (uveitis). Treatment options usually range from oral medications and injections to biologic therapies. Depending on the severity of the inflammation and progression of the disease, a medical professional will be able to design the right treatment plan for you.
Psoriasis complications
If left untreated, this autoimmune disease can cause a plethora of complications. The abovementioned psoriatic arthritis is just one of the possible psoriasis progressions, and it may be the easiest to treat and handle.
According to Medscape, more serious complications can increase one's risk of developing secondary infections and inflammatory states, lymphoma, different types of heart diseases, mitral valve prolapse, and even inflammatory bowel disease (IBD). All of these complications can cause irreversible damage to your joints, tissue, and skin cells, increasing your risk for developing a variety of different conditions in the future.
Recent studies even link psoriasis to certain cancers (via AJMC Center for Biosimilars), which just shows why this disease shouldn't be ignored or underestimated. The sooner you get an accurate diagnosis and start a treatment plan that's right for your symptoms, the better your chances are of reducing the inflammation and protecting your overall health and longevity.
Psoriasis and nutrition
Diet plays a huge role in the development, maintenance, and treatment of many diseases, psoriasis included (via MDedge Dermatology).
Since inflammation is one of the most significant factors in psoriasis development and intensity, fine-tuning your nutrition in a way that addresses inflammation will undoubtedly be of great help in alleviating any symptoms. Eliminating foods that contribute to inflammation (such as processed foods, sugars, hydrogenated oils, and most allergens) will be crucial in your fight against psoriasis.
In turn, adding more whole foods and colorful fruit and vegetables, as well as beans, legumes, nuts, seeds, and omega-3 rich fish into your diet will help replenish your body with fiber, vitamins, minerals, and an abundance of antioxidants that lower inflammation and fight harmful free radicals, preventing oxidative damage and supporting your immune system (via the National Psoriasis Foundation). If you're having an issue with managing your food intake, try keeping a diary and noting which foods help (and which make your symptoms worsen after ingesting them).
Psoriasis and stress
One of the most common triggers of psoriasis is stress, and according to Everyday Health, stress management should be part of any treatment plan. Even though the exact causes of psoriasis are still unknown, stress is called a silent killer for a reason. It can exacerbate symptoms of many diseases, cause inflammation and flare-ups to worsen, and potentially even prevent treatments from being effective.
Learning how to cope with stress is crucial in your fight against any disease and its symptoms. How you manage your stress levels will depend on you and your lifestyle routine, so it's important to find a way that works for you. What works for someone else might not help you out, so work with your doctor in identifying what you can incorporate into your daily routine. Many people find meditation and other self-care practices helpful in allowing them to relax, unwind, and bring their bodies and mind into balance.
Psoriasis and exercise
Engaging in consistent moderate exercise is one of the best ways to take care of your health, no matter what kind of issue you're dealing with. A sedentary lifestyle can worsen inflammation, and can therefore make your psoriasis flare up even more. Exercising helps you maintain a healthy weight, improves circulation, promotes the release of toxins through your lymphatic system, and stimulates the release of endorphins that can reduce your stress levels (via MedlinePlus). It also helps you improve your mental health by elevating your mood and self-esteem.
It's important to keep some things in mind when working out with psoriasis. Wear clothes that are comfortable, not too tight, and not made out of moisture-wicking fabric. Otherwise, your skin may get irritated, worsening your condition. If you're going to work out at the gym, always use your own towel. Additionally, wipe any surfaces you are about to use, to help you prevent any potential infections. Lastly, make sure to stretch pre- and post-workout, particularly if you're dealing with psoriatic arthritis, to prevent mobility issues and reduce your pain (via psoriasisSPEAKS).