11 Possible Warning Signs That Mean A Person Is Nearing Death
In the delicate and often emotional journey of caring for a dying loved one, your role as a caregiver is crucial. Recognizing signs that indicate the final stages of life can be essential. According to a study published in the American Journal of Hospice & Palliative Medicine, these signs not only help you prepare for what lies ahead and educate loved ones on what to expect to reduce anxiety levels but also allow you to provide the best possible support, ensuring the comfort and dignity of the person nearing the end of their life. While it's essential to understand that every individual's experience with dying is unique, there are common indicators that may suggest someone is approaching the end of life.
Common signs that a person is nearing the end of life include a decline in energy levels, appetite loss, increased pain or discomfort, and changes in breathing patterns, toilet habits, skin color, and temperature. Emotionally, a person nearing death may become more withdrawn or less responsive. However, it's crucial to note that these signs can manifest differently depending on various factors, such as the specific illness they're fighting, the medications they might be taking, and their overall health condition. Understanding these warning signs can ultimately empower you to create a peaceful and comfortable environment for your loved one's final days. Keep reading to learn what to expect when a person is nearing death.
Irregular breathing pattern
Changes in breathing patterns can suggest the body is gradually shutting down. These changes can vary from subtle to more pronounced and may include several distinct patterns. Cheyne-Stokes breathing is one common pattern seen in the final stages of life that's believed to be a result of heart failure. Per the National Library of Medicine (NLM), it involves a cycle of gradually increasing and decreasing breathing (aka hyperventilation and apnea, respectively). Respiration with mandibular movement (RMM) is another highly specific change in breathing pattern indicating the end of life. According to a review published in Gerontology and Geriatric Medicine, RMM involves periods of shallow breathing where the person appears to grasp for air by opening their mouth or through a visible movement of the jaw or neck muscles as they attempt to take in more oxygen.
Dyspnea, also known as difficulty breathing or shortness of breath, is another common sign. In fact, per a review of 2,416 patients published in the American Journal of Hospice & Palliative Medicine, up to 57% of people showed dyspnea in the last 2 weeks of life. In this case, the person may appear to struggle to breathe, gasping for air in an effort to get air into the lungs (via the Cleveland Clinic). Lastly, death rattle is a distinctive end-of-life breath change that creates a sound caused by fluid accumulation in the throat as the person's muscles relax. Fortunately, it is generally not uncomfortable for the person experiencing it. Yet, it may suggest that the person has little over a day of life (via Medical News Today).
Changes in vital signs
According to a review published in Gerontology and Geriatric Medicine, one of the most notable changes as a person approaches the end of life is a drop in vital signs, namely blood pressure and oxygen levels. Per the review, research even indicates that these changes may occur in the last 48 hours of life. For example, a study of terminally ill cancer patients published in The Journal of Pain and Symptom Management found a small but significant decrease in these vital signs in the last two weeks of life, with a sharp drop in the final three days. According to the study, these changes often signal cardiovascular and/or respiratory instability.
A drop in blood pressure (hypotension) can lead to feelings of dizziness or lightheadedness, and the person's extremities may feel cooler to the touch (via the Mayo Clinic). In contrast, a drop in oxygen levels (a condition known as hypoxia) happens when insufficient oxygen reaches the body's tissues, leading to symptoms like confusion, dyspnea, and bluish discoloration of the lips and extremities (per the Cleveland Clinic). While the study warns that it is difficult to distinguish whether these vital sign changes are a part of the natural process of dying or whether they are related to major complications from a pre-existing condition, monitoring them can still offer valuable insights and help you as a caregiver anticipate the person's needs.
Loss of appetite and thirst
In the final days of life, it's common for the desire to eat and drink to gradually decline, with the person refusing meals or only taking small amounts. Per a review published in Gerontology and Geriatric Medicine, this decline in appetite and thirst is a natural part of the body's transition towards the end of life as the body's systems begin to shut down, explaining that it doesn't mean your loved ones are starving themselves. Instead, it's a sign that their body is going through the process of actively dying.
One of the reasons behind this loss of appetite is that, during this last stage of life, the body doesn't have a need or use for nutrients. Similarly, loss of thirst often helps patients deal with coughing, congestion, and other complications linked with excess fluids (via VNS Health). It's important to understand that this decline in appetite is normal and does not necessarily mean the person is suffering. In fact, according to a study published in Current Opinion in Supportive and Palliative Care, attempting to force the person to eat or drink against their will or providing artificial nutrition and hydration can be more harmful than helpful and may lead to increased discomfort. Instead, you can focus on providing comfort measures and alternative ways to ensure the person remains hydrated and comfortable, such as offering small sips of their favorite drinks, soft foods like purée, soups, gelatin, or ice cream, and moistening the person's mouth with a damp cloth, ice chips, or lip balms (via VNS Health).
Increased pain
While some people may pass peacefully and painlessly, increased pain is a common symptom that a person is nearing death. What's more, according to a review published in the Annual Review of Sociology, over half of older patients experience some level of pain during their last month of life. This pain can be caused by a variety of factors, often related to the person's illnesses. For instance, the review states that pre-existing diseases such as arthritis, musculoskeletal conditions, depression, and cancer tend to lead to considerably higher pain rates.
Addressing pain management becomes one of the most important goals when providing care to someone nearing the end of their life. Per the NLM, pharmacological pain relief measures may include medications such as opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), or acetaminophen. However, it warns that they should be assessed individually according to the person's needs due to potential adverse side effects, including gastrointestinal issues. Additionally, non-pharmacological interventions like adjusting the positioning of the body, oral and skin care, and alternative medicinal therapies like acupuncture and Reiki can also provide relief and improve the person's comfort, not only improving their quality of life but also allowing them to spend their final days with dignity and as little discomfort as possible.
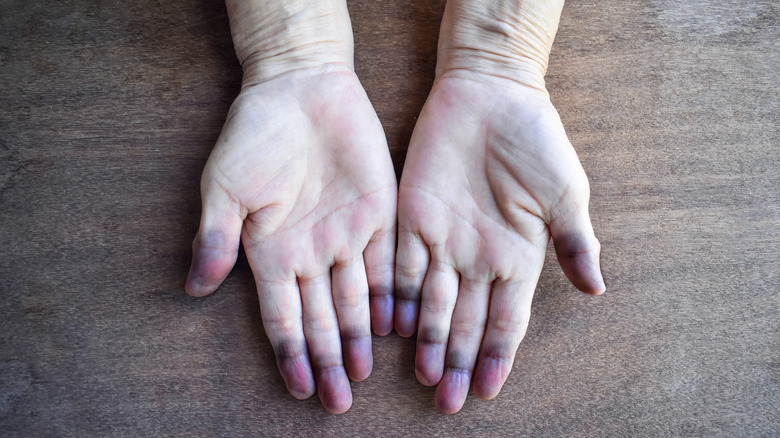
Abnormal bluish discoloration of the skin
An abnormal bluish discoloration of the skin, particularly in the hands and feet, is known as peripheral cyanosis, and it is a common end-of-life symptom caused by changes in the body's temperature and circulation. In fact, a study published in Cancer Research and Treatment found that 59% of advanced cancer patients showed peripheral cyanosis within the last 3 days of life. The NLM explains that when the heart is not pumping enough blood, either because of heart failure or shock or when the body temperature drops, causing blood vessels to constrict, the body is unable to deliver enough oxygen-rich blood to the peripheral tissues (aka your extremities), making the skin seem to have a blue hue, particularly in the fingers, toes, lips, and nose.
While cyanosis can be hard to witness, it's important to understand that it is a normal part of the dying process and does not typically cause discomfort to the person. Instead, it serves as a visual indicator of the body's declining function and a reminder that death might come in a matter of days (via Sunset Care). As a caregiver, you can help manage peripheral cyanosis by ensuring the person is kept warm and comfortable. Providing extra blankets or adjusting the room temperature can help regulate their body temperature. Yet, electric blankets or heating pads are not recommended (via the American Cancer Society).
Delirium
Evidence shows that delirium is a common occurrence in patients nearing the end of their life, with almost all patients experiencing it in the hours to days before passing. According to an article published in Age and Ageing, when patients are admitted to palliative care units or hospices, up to 40% already have delirium. Yet, after admission, this figure can range from 3 to 45%, and as death approaches, the prevalence increases significantly, affecting an astounding 75% of people. Per the article, delirium involves a disruption in attention, communication, and awareness, which, besides creating feelings of distress, can make the last moments more difficult for the person and their family, seeing that during this crucial period, being mentally present and engaging with loved ones is highly important.
According to a study published in Cancers, delirium can present in different ways: hypoactive (where the person is drowsy and less responsive), hyperactive (where they may be agitated or restless), or mixed (when it switches between the hypoactive and hyperactive subtypes). In addition, the signs or symptoms of delirium might come and go, which means there are times when the person seems clear-headed. This might lead to a missed diagnosis if it happens right when the doctor is giving an assessment. Per the study, delirium often predicts death within days to weeks, particularly in patients with advanced cancer. Thus, managing it focuses on comforting the patient. Achieving this requires a combination of medications, environmental adjustments, and supportive care to help the patient remain as comfortable and mentally aware as possible.
Increased sleep or fatigue
Fatigue is a prevalent symptom as a person nears the end of their life, particularly for those with terminal illnesses. According to a study published in UpToDate, it can affect up to 85% of people with severe and/or life-threatening diseases. This overwhelming sense of tiredness can affect both the body and the mind, making it challenging for the person to engage in daily activities (even the ones they enjoy). Additionally, they may need more frequent and longer periods of rest. Thus, fatigue can impact the person's quality of life and interactions with loved ones, as they may have less energy for socializing or engaging in conversations (via Marie Curie).
According to a report published in JAMA, causes of fatigue in the end-of-life context are multifaceted, making it challenging for caregivers to address it adequately. Physical factors such as trouble breathing, anemia, weight loss, and medication side effects can contribute to feelings of tiredness. Additionally, emotional and psychological factors such as isolation and depression can also exacerbate this symptom. Recognizing and addressing fatigue is essential for providing care to someone nearing death. This may involve providing medications to help with energy levels and appetite, ensuring proper nutrition and hydration, and organizing the day so they can do things when they feel most energetic. You might also assist by helping the person conserve energy, prioritizing rest, and assisting with activities of daily living as needed (via Marie Curie).
Detachment from surroundings
People near the end of life commonly withdraw from their surroundings. This withdrawal can manifest in various ways, such as becoming less responsive to stimuli or showing less interest in interacting with others, per the Hospice Foundation of America (HFA). While this detachment might be associated with the increased fatigue caused as the body's systems begin to shut down, the person may also start to emotionally withdraw themselves as they come to terms with the reality of their impending death. This can lead to a sense of introspection or reflection, causing them to retreat into their own thoughts and emotions (via MyHealth.Alberta.ca).
According to the HFA, while this withdrawal can be difficult for families and caregivers to witness, it's important to understand that it is part of the body's natural response to the dying process. Therefore, instead of trying to force the person to engage with their surroundings, you should focus on providing comfort and support in whatever form is most appropriate. This may involve offering gentle reassurance, creating a peaceful and supportive environment, or being present and available if the person wishes to talk or spend time together. This allows the person to pass away with dignity and be surrounded by the love and understanding of those closest to them.
Confusion and visions
Near the end of life, the brain's ability to process information becomes impaired, leading to symptoms such as confusion and visions. With confusion, a person may have difficulty understanding their surroundings, recognizing familiar faces, or recalling recent events (via Crossroads Hospice). Per the site, factors such as pain, medication side effects, emotional distress, or a reduced oxygen supply to the brain can both explain and exacerbate this symptom. When it comes to its management, Crossroads Hospice recommends simply validating the experience by listening to your loved one and responding in ways that acknowledge and affirm what they're going through.
Regarding visions (commonly known as deathbed visions), they can take many forms, including seeing people, religious icons, or scenery (via Psychology Today). Despite not being a clinical near-death symptom, Crossroads Hospice states that they are undoubtedly common. Per the site, experiencing said visions can help soften the grieving process and provide a sense of peace and closure. Thus, when a loved one shares these experiences, the most important thing is to acknowledge and support them without questioning or attempting to rationalize their visions. Arguing, correcting, or dismissing their experiences can cause distress and undermine their sense of comfort and validation.
Changes in bladder and bowel habits
In the final days of life, it's common for people to experience changes in bladder and bowel function, such as urinary and fecal incontinence or constipation. This can be influenced by various factors, including underlying health conditions and the body's natural processes as it starts to shut down (per Continua). Additionally, certain medications, particularly those used to manage pain, constipation, or other symptoms, can contribute to bladder and bowel incontinence. Furthermore, underlying health problems, such as brain disorders, obesity, advanced cancer, or damage to the muscles or nerves that control the rectum and bladder, can also impact bladder and bowel function (via Marie Curie).
Regarding constipation, Continua explains that digestion is expected to become less efficient near the final days, resulting in fewer bowel movements and harder stools. Furthermore, lifestyle factors such as reduced mobility and changes in diet or fluid intake, certain medications, and pre-existing conditions like hemorrhoids or hypothyroidism can all contribute to constipation (per Marie Curie). Managing bladder and bowel issues in the last days of life should be centered around ensuring the comfort and dignity of the person. For incontinence, providing appropriate toileting assistance and using absorbent pads might be of great help. Meanwhile, adjusting medications, increasing fluid intake, and incorporating dietary changes can help alleviate constipation.
Terminal lucidity
When nearing death, some people with cognitive decline may experience a phenomenon known as terminal lucidity. According to a review published in Archives of Gerontology and Geriatrics, doctors and researchers have mentioned this event over the last 250 years, referring to a sudden return of mental clarity or awareness in dying patients, often shortly before death. More specifically, the phenomenon has been reported in people with conditions such as dementia, Alzheimer's disease, and even brain tumors or strokes.
For people with cognitive decline, moments of terminal lucidity can be surprising and deeply meaningful for both the individual and their loved ones, as they provide a sense of connection and closure. During these periods, the person may suddenly become more alert, communicative, and responsive. They may recognize family members, engage in conversations, or express thoughts and emotions that seem clear and coherent (via Healthline). Per the review, while the exact cause of terminal lucidity is not understood, some researchers believe it may be linked to changes in brain processes as the body approaches death. It's thought that as the brain begins to shut down, some abilities may function differently compared to a normal brain, resulting in moments of clarity. However, per Healthline, it's important to note that not all individuals with cognitive decline will experience terminal lucidity, and its occurrence can be unpredictable.