The COVID Vaccine Rollout Has Been Slower Than Expected. Here's Why
Only about one-third of the 20 million coronavirus vaccinations the federal government promised have occurred, leaving public health officials frustrated and pinpointing a number of reasons for the slow rollout (via Associated Press).
As of Jan. 8, the federal vaccine program known as Operation Warp Speed has distributed more than 22 million doses of the two COVID-19 vaccines available, according to the U.S. Centers for Disease Control and Prevention. But just 6.7 million people — about 34 percent — have received their first dose of the two-dose vaccine, CDC records show. That's fewer than 1 million people per day, says Associated Press. For widespread national immunity by the summer, the American Hospital Association estimates 1.8 million people must be vaccinated daily from Jan. 1 to May 31.
Alabama, Georgia, and Mississippi have the slowest vaccination rates, according to CDC data (via Healthline). Colorado, Connecticut, North Dakota, and West Virginia are among the fastest. Overall, low funding, a lack of consistent communication, new storage and distribution guidelines, and technical issues have contributed to the "slower-than-expected start to the largest vaccination effort in U.S. history," according to Associated Press.
The U.S. Department of Health and Human Services said states will receive $3 billion for COVID-19 vaccination efforts by Jan. 19, with an additional $19 billion in aid for testing and contact tracing (via Associated Press).
With freezer failures and delivery mix-ups, health officials urge a more coordinated effort
Both vaccines developed by the teams of Pfizer/BioNTech and Moderna required new safety protocols, including frozen storage and thawing before injection. In addition to freezer failures, as reported by CNN, states have coped with staff shortages and delivery mix-ups, which in West Virginia led to 42 people mistakenly receiving an antibody treatment instead of the vaccine (via The New York Times).
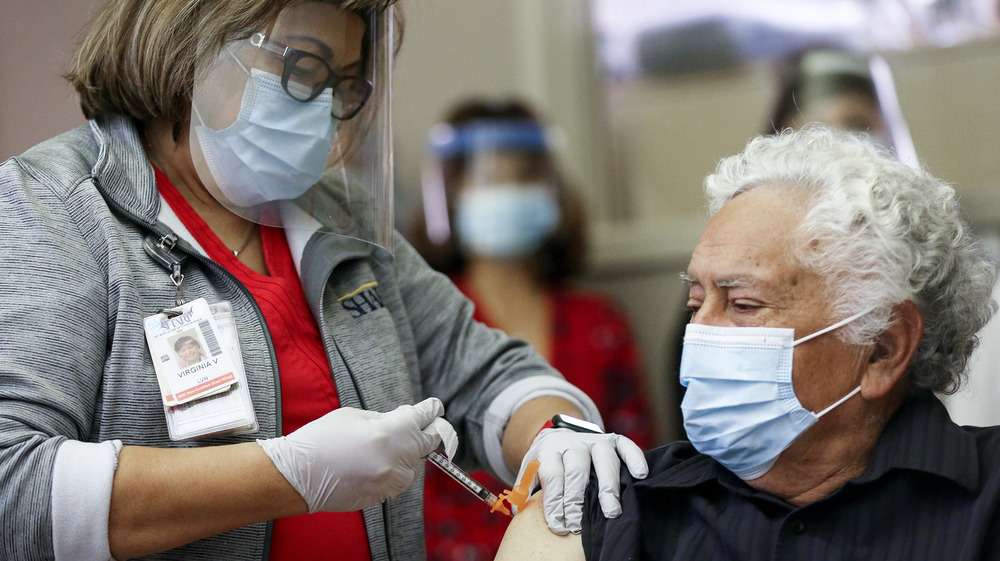
The CDC has prioritized vaccinations for high-risk groups such as healthcare workers and the staff and residents of long-term care facilities, but officials say that some locations have more doses for these groups than they need. Nancy Messonnier, who heads the CDC's immunization center, urged distribution sites to move to the next priority group as necessary. "Don't leave vaccine in the fridge. Don't leave vaccine in the vial," she said.
Several health officials said the federal government should coordinate a "national, wartime-type effort" to immunize as many people as possible. For instance, there are no information resources for municipalities to tailor to their communities that address concerns about the vaccine, said Dr. Michael Osterholm, an infectious disease expert at the University of Minnesota, who is a member of President-elect Joe Biden's COVID-19 advisory board. "You don't need 50 different states trying to do this kind of work. What you want to have is a smorgasbord of information sources that address different populations that any one state can use," Osterholm told the Associated Press. "That's what we don't have right now."