Different Types Of Birth Control Explained
People who want to avoid getting pregnant have several birth control options. According to the National Institute of Child and Human Development (NICHD), the most common birth control methods fall into 5 categories: hormonal contraceptives, long-acting reversible contraceptives, barrier methods, emergency contraceptives, and surgical sterilization.
Birth control pills are oral medications taken daily, which introduce synthetic hormones into the body to prevent pregnancy. The Depo-Provera shot, the vaginal ring, and the transdermal patch are also hormonal birth control methods.
Long-acting reversible contraceptives are devices inserted into the body to prevent pregnancy. Intrauterine devices (IUDs) are T-shaped devices inserted through the cervix and into the uterus. The Mirena, Liletta, Skyla, and Kyleena IUDs all release a progestin hormone into the uterus to prevent pregnancy. The copper IUD, ParaGard, is non-hormonal and prevents pregnancy just by being present in the uterus. The birth control implants, Implanon and Nexplanon, are inserted under the skin in the arm and release a hormone called etonogestrel into the body to prevent pregnancy.
Barrier methods, like condoms, diaphragms, birth control sponges, and spermicide, reduce the chances of pregnancy by blocking sperm from entering the cervix, preventing fertilization.
Emergency contraceptives can be used to prevent pregnancy after unprotected intercourse. A copper IUD can be implanted as an emergency contraceptive, or pills can be taken to prevent pregnancy by introducing hormones into the body.
Finally, sterilization involves a surgical procedure that prevents pregnancy from occurring. These include tubal ligation, vasectomies, and hysterectomies.
Combined oral contraceptives
Combined oral contraceptives include a combination of estrogen and a progestin hormone. The very first birth control pill available to the public, Enovid, was a combined oral contraceptive (via Planned Parenthood). It was approved by the FDA in 1960.
Combined birth control pills are oral medications, taken daily, ideally around the same time. These pills prevent pregnancy in 2 different ways. First, they prevent an egg from being released into the fallopian tube. Second, the pills thicken the cervical mucus, which makes it harder for sperm to penetrate the cervix and meet up with an egg for fertilization.
According to the Mayo Clinic, combined oral contraceptives contain different amounts of estrogen and progestin, as well as different kinds of progestin, depending on the brand. This means that if one combined pill doesn't work well for your body, you can try one with a different hormone mix to see if it works better.
Conventional packs of combination birth control pills have 21-24 active pills — pills that contain hormones — and 4-7 inactive pills, or placebo pills. When you finish the active pills, you take the inactive pills while you have your period. If you want to skip your period entirely, it's totally safe to skip the placebo pills and go right back to the active pills. This is called continuous use. Some continuous use packs include inactive pills so you have your period every 3 months instead of monthly. Others don't include inactive pills at all.
Progestin-only pills
Like combined oral contraceptives, progestin-only pills (POPs) are oral medications, taken daily at the same time each day, per The American College of Obstetricians and Gynecologists (ACOG). As the name implies, progestin-only pills do not contain estrogen. They only contain progesterone, a hormone that plays a role in regulating the menstrual cycle.
POPs essentially work the same way as combined oral contraceptives. They thicken the cervical mucus to prevent sperm from getting through the cervix, and they prevent the ovaries from releasing an egg into the fallopian tubes. However, progestin-only pills are not as consistent at preventing ovulation as combined oral contraceptives. Some people who take POPs will continue to ovulate on a monthly basis. In these people, the progestin-only pill reduces the chances of pregnancy by preventing fertilization.
Progestin-only pills are a great option for people who can't take estrogen. According to ACOG, people with a history of high blood pressure, cardiovascular issues, and deep vein thrombosis should not take birth control pills with estrogen. Progestin-only pills can also be used while breastfeeding, so they're a great option for post-birth contraception.
POPs are also particularly effective for women who have heavy and painful periods. Because progestin-only pills thin the lining of the uterus, there's less lining to shed each time you have your period. This means less bleeding, shorter periods, and less painful menstrual cramps. Because of this, POPs are commonly prescribed for women with heavy, painful periods.
Non-Hormonal IUDs
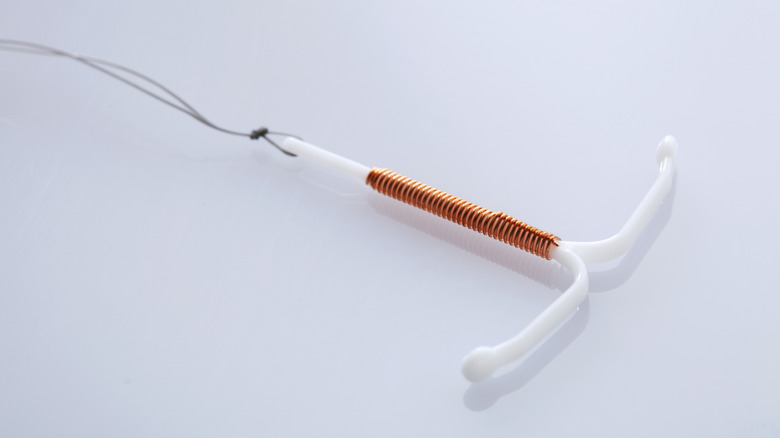
The copper IUD, which is sold under the brand name ParaGard in the United States, is a small T-shaped device made of plastic wrapped in copper, according to the Cleveland Clinic. This device is inserted through the cervix and into the uterus by a gynecologist. Once the ParaGard is present in the uterus, it reduces the chances of pregnancy by preventing sperm from meeting up with an egg to complete the fertilization process. Sperm don't like copper, so they avoid the uterus because of the presence of the copper IUD.
The ParaGard IUD does not rely on hormones to prevent pregnancy. People who choose the copper IUD continue to get their periods on a regular schedule and their cycle is still regulated by natural hormone production. Because of this, ParaGard is the ideal choice for people interested in a non-hormonal method of birth control.
One of the main benefits of any IUD is that it's a "set it and forget it" method of birth control. Once the IUD is inserted, it's effective for years without any extra effort. The ParaGard can be left in place for up to 10 years before it needs to be replaced. That's a decade of no-hassle birth control! However, the copper IUD isn't for everyone. People with heavy, painful periods might want to avoid the ParaGard IUD because it can cause heavier flow and more intense cramps.
Hormonal IUDs: Mirena, Liletta, Skyla, and Kyleena
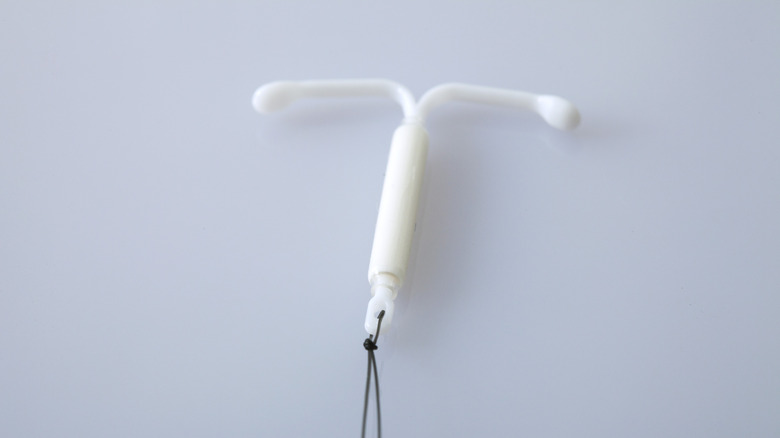
Hormonal IUDs are small devices inserted through the cervix into the uterus. They release small doses of the hormone levonorgestrel into your body daily (via Healthline). Right after these devices are inserted, they release a larger amount of levonorgestrel for a few months. The dosage tapers off the longer the device is in your uterus.
There are a few different brands of hormonal IUDs: Mirena, Liletta, Skyla, and Kyleena. Each of these brands uses the same type of hormone, but they all contain different amounts, and they also differ in size. Mirena and Skyla are the most widely used hormonal IUDs in the U.S. because the Liletta and Kyleena IUDs are newer.
The hormone dosage correlates to how long the device is effective, per Verywell Health. Skyla has the lowest dosage of levonorgestrel, so it can only be left in for 3 years. Mirena has the highest dosage, so it can be left in for up to 7 years. Like the Paragard, hormonal IUDs are "set it and forget it."
Hormonal IUDs prevent pregnancy by inhibiting fertilization and preventing the implantation of a fertilized egg. They thicken the cervical mucus to prevent sperm from entering the cervix to find an egg. Hormonal IUDs also thin the lining of the uterus, which makes it very hard for a fertilized egg to implant. Additionally, the hormones disrupt ovulation, making it less likely that an egg will meet up with sperm to complete fertilization.
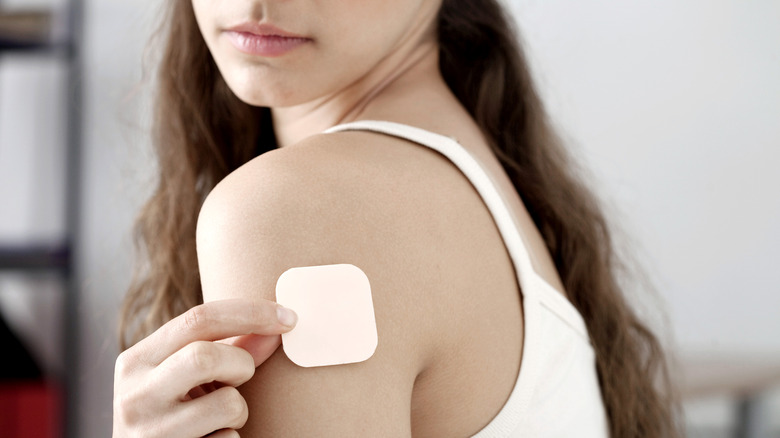
The patch
The birth control patch is a small, band-aid-like patch that you wear on your skin (via the Mayo Clinic). It contains estrogen and progestin, like combination birth control pills. The patch delivers these hormones into your body through your skin. They prevent pregnancy by disrupting ovulation and thickening the cervical mucus so it's harder for sperm to get into the uterus.
The patch must be changed weekly. It's a more convenient option than taking a birth control pill every day, and it's just as effective, as long as you remember to change the patch. Unlike birth control pills, the patch cannot be used continuously to skip your period entirely. You need to apply a new patch every week for 3 weeks, then go patch-less for a week while you get your period.
Though the patch is a convenient, easy birth control method, it's not for everyone. The patch is less effective for people over 198 pounds. It's also not safe for people with certain pre-existing conditions like liver disease, migraines with auras, and diabetes. People with a history or family history of cardiovascular problems, high blood pressure, blood clots, or certain cancers should avoid the patch as well.
Some people find that their skin won't tolerate the patch — they get an itchy rash where they've applied the patch. This may be more common in people with pre-existing skin conditions, like psoriasis or eczema. If your skin is bothered by the patch, check in with your doctor.
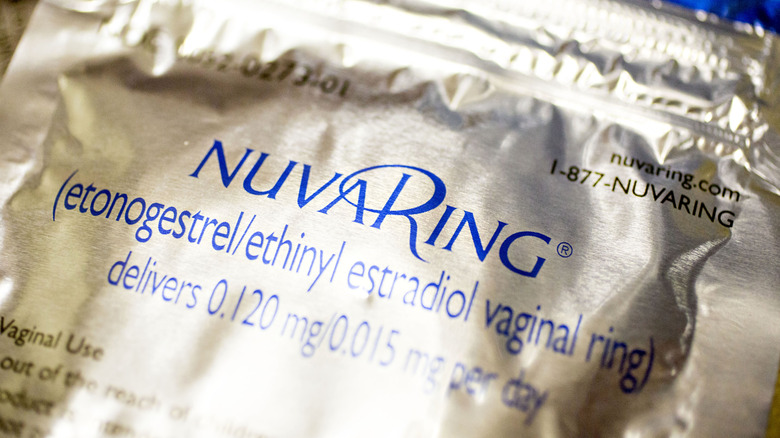
Vaginal rings: NuvaRing and Annovera
Vaginal rings are small circles of plastic containing both estrogen and progestin. To be used, they are inserted into the vagina, per the National Health Service. The vaginal ring prevents pregnancy by disrupting ovulation, thickening the cervical mucus, and thinning the lining of the uterus.
There are 2 brands of vaginal rings, NuvaRing and Annovera. According to Everyday Health, the NuvaRing only contains enough hormones for 1 month's use. You can either remove it after 3 weeks and have your period, or use it for 4 weeks to skip your period. At the end of the month, you need to get a brand new ring, which usually requires a trip to the pharmacy and perhaps a renewed prescription.
The Annovera ring contains enough hormones for an entire year. After 3 weeks of use, you take the Annovera out so you can have your period. After properly sanitizing the ring, you reinsert it after your period for another 3 weeks and continue this cycle for up to a year. You don't have to remember to call in your prescription or go out to pick it up.
Vaginal rings are an effective and convenient form of birth control, but they aren't for everyone. There isn't much data on how effective they are in people who are overweight. Those who are sensitive to estrogen shouldn't use a vaginal ring, and neither should those with conditions that compromise the liver. Vaginal rings can also cause yeast infections.
Birth control shots: Depo-Provera, Noristerat, and Combined Injectable Contraceptives
Birth control shots inject hormones directly into your body to prevent pregnancy, per Verywell Health. There are currently 3 different kinds of birth control shots on the market, though only 1 is available in the United States.
Depo-Provera, a progestin-only birth control shot often referred to as simply Depo, is the only one available in the U.S. Noristerat is another progestin-only birth control shot available in Latin America, the United Kingdom, parts of Europe, and Africa. Research shows that it is just as safe and effective as the Depo shot. Several brands of combined injectable contraceptives are available in Latin America, Africa, and Asia. As the name implies, these shots contain both estrogen and progestin. These shots may be less effective than Depo and Noristerat. Depo and Noristerat both prevent pregnancy by disrupting ovulation and thickening the cervical mucus. Combined injectable contraceptives prevent pregnancy through the same mechanisms as combination birth control pills, vaginal rings, and the patch.
The Depo shot is effective for up to 14 weeks. However, you should plan to get your shot every 12 weeks. Noristerat is only effective for 8 weeks, so you'll need to get shots more frequently. Although these birth control methods are more convenient than taking a pill every day, changing a patch each week, or a ring once a month, there is the downside of having to schedule your shot on a regular basis and go in for the injection.
Birth control implant: Nexplanon
The birth control implant is a small plastic rod that gets inserted under the skin in the arm, per WebMD. The rod contains a form of progesterone called etonogestrel, which is released into the body over time to prevent pregnancy by disrupting ovulation and thickening the cervical mucus.
In the U.S. the implant goes by the brand name Nexplanon, which is a newer version of Implanon. Nexplanon is effective for up to 3 years, and it is a highly convenient and effective form of birth control. Once it's in, you don't have to think about birth control for a few years. Studies have shown that it can also lead to lighter, less painful periods, making it a great option if you struggle with difficult periods.
The main drawbacks of Nexplanon are the insertion and removal procedures, in addition to the cost. Since the rod is inserted under the skin, your arm may be painful and swollen after the insertion. However, the insertion itself doesn't hurt because your doctor will numb the area. When it's time to get the implant removed, your doctor will have to make a small incision to remove the device and then implant a new one. Again, you'll be sufficiently numbed up for this as well, so the procedure shouldn't hurt, but you may be sore after. The implant can cost up to $600 for the first one and up to $100 for every removal and reinsertion.
Condoms
Condoms are thin pouches of material that are worn on the penis or in the vagina to prevent pregnancy, according to the Cleveland Clinic. Condoms are a "barrier method" of birth control, meaning that they prevent pregnancy by creating a barrier between the sperm and the eggs so that fertilization cannot occur. When used properly, a condom contains ejaculated sperm within the pouch, preventing it from reaching the cervix. Male condoms cover the penis, while female condoms are inserted into the vagina.
Condoms are the only method of birth control that also provides protection from sexually transmitted infections (STIs). Most STIs are passed on via skin-to-skin contact or via bodily fluids. Since condoms create a barrier between the penis and the vagina, the skin and the fluids of the penis and the vagina never touch. Even if you are using another form of birth control to prevent pregnancy, it's always a good idea to use condoms until you and your partner are tested for sexually transmitted infections.
To ensure effectiveness, the condom must be put on or inserted before the penis has any contact with the vagina. Male condoms need to be rolled down the penis until they are fully unrolled, and the bottom is secure around the base of the penis. Female condoms need to be manually inserted into the vagina, ensuring that the ring at the bottom of the condom is secure around the vaginal opening.
Diaphragms
Diaphragms are another barrier method of birth control. According to the Mayo Clinic, these devices are small silicone or rubber cups that are inserted deep into the vagina to cover the cervix. Diaphragms create a physical barrier between the ejaculate and the cervix so sperm cannot reach an egg to complete fertilization. However, diaphragms are not effective at preventing pregnancy on their own — they need to be used with spermicide.
You'll need to visit your doctor or gynecologist to get fitted for a diaphragm. During that visit, your doctor will show you how to properly insert the device and how to place it correctly. Proper placement is essential to a diaphragm's effectiveness, so make sure you leave your doctor's office as an expert on insertion and placement.
Diaphragms can be inserted up to 24 hours before intercourse and must be inserted before the penis enters the vagina for the first time. Before you insert the diaphragm, fill the small cup with spermicide and rub the spermicide around the edge of the cup. Then, insert the diaphragm with the bowl upward by putting your fingers in your vagina. Make sure that the diaphragm is placed correctly, and recheck the placement before intercourse.
The major drawbacks of the diaphragm are that it's hard to use correctly, and it doesn't prevent sexually transmitted infections. However, when used properly, it's an effective form of birth control that doesn't require your partner to wear a condom.
Birth control sponges
Birth control sponges work similarly to diaphragms. Instead of a little plastic cup, a birth control sponge is a soft, round piece of plastic with a loop on one end, according to Healthline. Before intercourse, you manually insert the sponge all the way into your vagina until it covers your cervix. As with the diaphragm, proper placement is very important. Birth control sponges contain spermicide, which kills the sperm before it can get through the cervix. They also work by creating a barrier over the cervix, which prevents sperm from getting through. Additionally, the sponge can absorb sperm so they're less likely to make it to the cervix.
Birth control sponges are a great option for people who want a convenient birth control method, but don't want to consult with their doctor or get a prescription. Unlike diaphragms, birth control sponges don't have to be fitted by your doctor or gynecologist. They are available at most drugstores and do not require a prescription. They're just as easy to obtain as condoms and are a great substitute for those who don't want to use condoms.
However, they are not as effective at preventing pregnancy as condoms, mainly because they can be tricky to use. Make sure you understand how to correctly insert the sponge before you use it to ensure effectiveness.
Spermicide
According to the University of Michigan Health, spermicide is often used in conjunction with a barrier method of birth control like condoms, diaphragms, or birth control sponges. However, spermicide can also be used as a standalone birth control method.
Spermicide comes in four forms — a jelly, a foam, a cream, or a suppository. Regardless of the form, spermicide is used by inserting it into the vagina before intercourse. Most spermicides come in an applicator, which is inserted into the vagina to disperse the spermicide. Suppositories come in capsule form. The capsule is manually inserted into the vagina, where it dissolves, releasing the spermicide. If you're using the jelly, foam, or cream, you can have sex right after the spermicide is inserted. If you're using the suppository, you need to wait at least 15 minutes to ensure the capsule fully dissolves.
Spermicide is a convenient and cost-effective method of birth control that's easily obtained and cheaper than some other birth control methods. However, it's not as effective. Spermicide is more effective when used with a barrier method, and isn't typically recommended as the sole method of birth control.
Emergency Contraceptives: ParaGard, Plan B, and Ella
If you've had unprotected intercourse and still want to prevent pregnancy, you have a couple of options. According to the World Health Organization, the copper IUD ParaGard is the most effective emergency contraceptive available. The IUD must be inserted within 5 days after unprotected sex in order to prevent pregnancy. Once inside the uterus, the copper IUD disrupts the fertilization process and repels any sperm that made it past the cervix.
The other option is emergency contraceptive pills (ECPs). Plan B can be purchased in most drugstores without a prescription, according to Planned Parenthood. You can also get Plan B at local Planned Parenthood clinics. The Ella morning after pill requires a prescription from a provider. If you don't want to go to your doctor or gynecologist, you can always make an appointment at a Planned Parenthood clinic. Emergency contraceptive pills work much like regular birth control pills. They introduce hormones into your body that disrupt ovulation, preventing an egg from meeting up with sperm for fertilization. ECPs must be taken within 5 days of unprotected sex to prevent pregnancy.
Emergency contraceptives are also very effective as a backup form of birth control. If the condom broke, you're not sure the diaphragm was in properly, or you missed a few days of the pill, emergency contraceptives can provide extra protection against pregnancy.
Surgical birth control options
If you're looking for a permanent form of birth control, there are a few surgical options, per MedicineNet. People with uteri have 2 options: tubal ligation and hysterectomy. According to Verywell Health, tubal ligation — or "getting your tubes tied" — involves blocking the fallopian tubes so an egg cannot travel to the uterus. The procedure is done laparoscopically under general anesthesia. A surgeon will make a few small incisions on your abdomen so they can insert instruments. Then, they either cauterize your fallopian tubes shut, clip them, or tie them to create a permanent blockage.
A hysterectomy involves removing the uterus. This procedure is rarely performed as a form of birth control, according to MedicineNet. It's only done if other health issues necessitate removing the uterus.
People with penises can get a vasectomy. According to the Urology Care Foundation, a vasectomy is a small surgical procedure that prevents sperm from getting to the ejaculate. During the procedure, the vas deferens — the tubes through which the sperm travel before they mix with the semen — are blocked so that sperm cannot make it into the semen. A surgeon does this by making two small cuts and then either cutting the vas deferens or blocking them with the surrounding tissue. Vasectomies can be performed with general anesthesia or local anesthesia.