What It Really Means When You Have White Spots On Your Skin
If you've noticed white spots on your skin, it's understandable why this might raise red flags, but chances are those white spots should not be a cause for concern, according to Healthline. There are a number of possible diagnoses for white discoloration of the skin, and many of these conditions are benign.
For example, white splotches on the skin may simply be the result of hypopigmented scarring, or white scars (via Oliva Skin & Hair Clinic). Due to skin cell damage, melanin production may decrease in the affected area, making the injured skin lighter in color than the surrounding skin. As a complex chemical substance, melanin determines the skin's pigmentation. Examples of injuries that may lead to hypo-pigmented scars include burns or deep wounds. According to Kingsfold Medical Centre, white scars are also seen in many patients following a shingles infection, the same virus that's responsible for chickenpox. These scars usually appear as a white, patchy spot. Aside from scars, however, there are also a number of different skin conditions that could be the potential cause of this discoloration.
Idiopathic guttate hypomelanosis
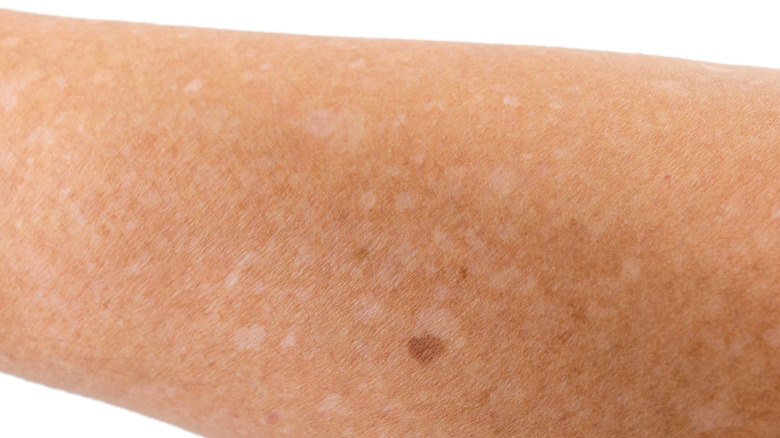
Idiopathic guttate hypomelanosis (IGH) is a condition that can also lead to the formation of white spots on one's skin (via Healthline). According to 2023 updated research published in StatPearls, IGH is a benign dermatosis that typically occurs in elderly people and fair-skinned individuals, although IGH can also emerge in darker skin. Research revealed that as many as 87% of people over the age of 40 have at least one IGH lesion. Genetic and environmental conditions are believed to be contributing factors. Although more evidence for a clear correlation is needed, researchers attribute exposure to sunlight as a contributing cause, though IGH has been found to manifest on skin not exposed to the sun. Nevertheless, wearing sunscreen and protective clothing may help to deter the onset of IGH.
Experts at the American Osteopathic College of Dermatology (AOCD) state that classic IGH spots — typically 1 to 3 millimeters in diameter — form due to lack of melanin. Your dermatologist will be able to determine through a visual examination if your white spots are IGH. Medical treatment for IGH is unnecessary, though people will sometimes seek cosmetic treatments.
Tinea versicolor
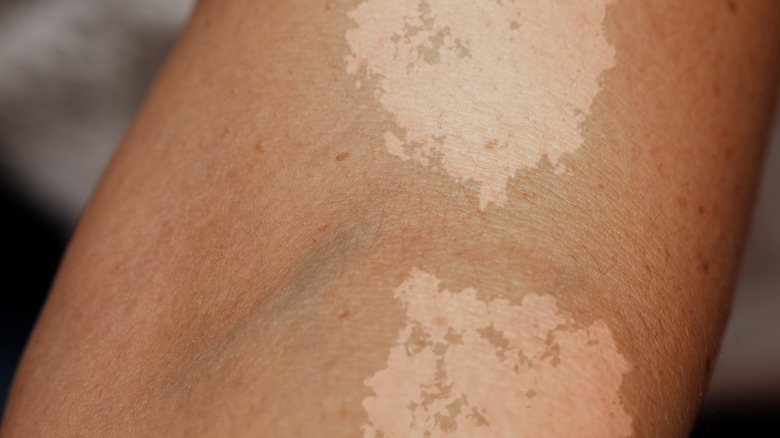
Tinea versicolor is a condition characterized by skin discoloration from an excess of yeast growth on the skin's surface (via Healthline). These spots may be darker or lighter in color, including white, and may expand in response to moisture or warmer temperatures. Often seen in adolescents, the condition has been linked with extreme sweating and oil production. Other risk factors include pregnancy, having compromised immunity, the topical use of oily skincare products, or having a family medical history of the condition, according to 2022 research published in StatPearls.
As temperatures fall, tinea versicolor usually resolves on its own. However, more severe cases may take longer to heal or require prescription medication. For more mild cases, an over-the-counter anti-fungal cream may be sufficient to treat the condition. With that said, cases of tinea versicolor often do come back. Considered a relatively common condition, especially among more tropical environments, tinea versicolor is not contagious.
Vitiligo
Another possible diagnosis for white spots on your skin could be vitiligo, which occurs when your skin cells stop producing melanin (via Healthline). Vitiligo is a benign condition that most frequently affects people in their 20s but can also happen at any age. Vitiligo most often appears on places like the knees, hands and hair.
While there may be a genetic component to the condition, external factors may also play a role, such as in the case of chemical-associated vitiligo. A 2020 case study published in Mayo Clinic Proceedings presented a case of a healthy, middle-aged man who had developed white spots on his skin. The researchers established a link between this hypopigmentation and continuous exposure to detergent chemicals through the man's job at a laundry facility. Vitiligo has also been associated with certain health conditions.
Treatments for vitiligo will have varying success and can include steroids and ultraviolet therapy. In more extreme circumstances, you may want to look at surgical treatment.
Lichen sclerosus
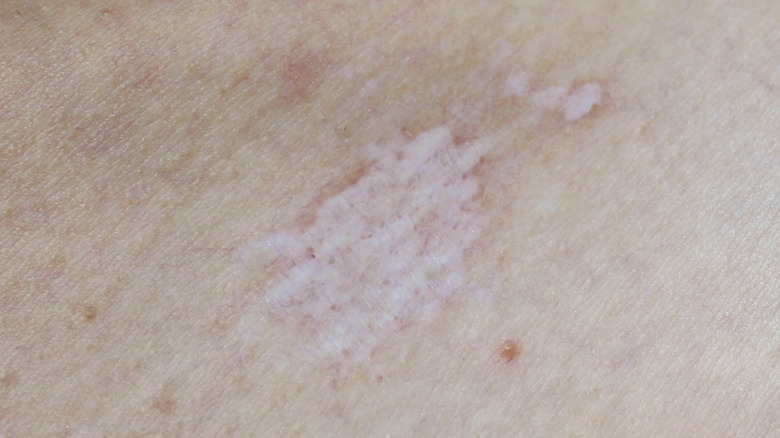
Most often developing around intimate areas, lichen sclerosus is characterized by the presence of thin, asymmetrical white blotches on the skin's surface (per Healthline). In some instances, these white spots may emerge elsewhere on the body. Cases are more often observed in prepubescent or postmenopausal females (via Water's Edge Dermatology). Those with the condition may additionally experience bruising, bleeding, pain, blistering, or itching. People with a genetic predisposition for lichen sclerosus, an overactive immune system, or an imbalance of hormones may be at increased risk.
Lichen sclerosus often resolves on its own in young children. Generally speaking, however, it's important for individuals to seek treatment from their physician, as there are rare cases in which these white patches may be malignant. Topical skincare products, such as corticosteroid creams, are usually the go-to treatment methods for lichen sclerosus in order to help alleviate discomfort, minimize scarring, and potentially enhance the look of affected skin.
Milia
While most types of white spots we've discussed thus far have been flat, there are instances in which the white spots on one's skin may be elevated. Such is the case with milia, particularly if you find these small bumps forming in groups on your face, according to experts at Water's Edge Dermatology. People who deal with acne may be more susceptible to milia. These tiny cysts form due to an accumulation of dead skin cells beneath the epidermis. However, prolonged use of topical corticosteroid products, as well as trauma to the skin (like sunburn) can also lead to the development of milia.
Milia do not pose any health risks, although some people may consider these white spots a cosmetic concern. Talk to your dermatologist about removal options. This may include cryotherapy, chemical peels, or laser or surgical removal, amongst other treatment methods. In some cases, milia may take care of itself.
Eczema
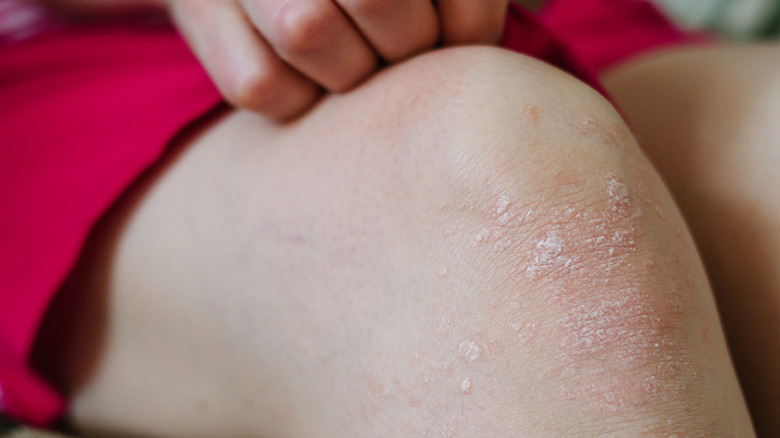
White spots that develop on the skin's surface could alternatively be indicative of atopic dermatitis, also known as eczema (via Healthline). Characterized by skin inflammation, atopic dermatitis can manifest as white patches and red, itchy rashes with raised bumps. Eczema, which typically occurs in children but can also affect adults, can come and go without any clear pattern. A person may also experience additional symptoms, such as scaling, flaking, leaking, and skin that feels warm to the touch. Your doctor will likely suggest applying moisturizer or a prescribed medicated cream to the area, as well as avoiding dry soaps. Keep your baths and showers short and tepid, and wear protective gloves when handling household cleaning products.
Considered to be a more mild form of eczema, pityriasis alba is a skin condition that can produce small, scaly patches of skin on the face. Once these spots naturally heal, they can leave behind a light-colored marking. Suggested treatment options to improve the skin's appearance include the use of moisturizers, non-steroidal creams, or topical steroids.
Vitamin deficiency
In some cases, white spots on one's skin may not have anything to do with a skin condition at all. Rather, it could indicate a potential vitamin deficiency, according to experts at The Derm. Essential for the health of our skin and red blood cells, a folate deficiency can lead to skin pigmentation loss, particularly in cases of folate-deficiency anemia. Other vitamin deficiencies that can cause skin to take on a pale appearance include a vitamin C deficiency, as vitamin C supports collagen production. A vitamin D deficiency can also affect the appearance of skin, as it plays a role in skin pigmentation. A vitamin B-12 deficiency is also known to cause white spots to develop on the skin's surface.
If you suspect a vitamin deficiency may be the cause of your skin discoloration, consult with your doctor to develop a treatment plan to ensure you're getting the vitamins and minerals you need. Certain cosmetic treatments, such as light therapy, may help reduce the appearance of these white spots, explains Asarch Dermatology.
When to see a doctor for white spots on your skin
Depending on the cause, white spots on your skin may not require medical treatment, though you may treat them for cosmetic purposes. Using sunscreen on a regular basis and wearing protective clothing can help prevent the formation of white spots related to UV ray exposure. Generally speaking, however, if white patches on the skin do not improve on their own within a few weeks, you'll want to reach out to a healthcare professional. The same is true if at-home remedies or other preventive measures are not reducing the appearance of white spots. In these instances, you may need to consult with your dermatologist about alternative treatments.
Finally, you'll want to speak to your doctor promptly if you experience additional symptoms along with the emergence of white spots, including severe itching or pain. Additional testing, such as a biopsy, may be needed to rule out any underlying health conditions.