Strep Throat Explained: Causes, Symptoms, And Treatments
When eating or drinking feels like razor blades in your throat, guess what? You might have strep throat. Most cases of pharyngitis, the medical term for sore throat or "inflammation of the pharynx," are caused by a cold virus, explains the Mayo Clinic. But strep throat is different. It's the result of a bacteria called group A streptococcus, and it's highly contagious.
You might think that strep throat is common because you hear about it a lot, but the condition actually accounts for only 5% to 15% of all sore throats in adults, and 20% to 30% in children, according to OnHealth. Left untreated, however, it can result in some serious complications.
"A strep infection can make it feel very painful to swallow, and often comes with fever of 101 degrees or higher," says Rosemary Schairer, a family nurse practitioner at Samaritan Internal Medicine in Oregon. "Strep throat is far more common in children than adults," she says via Corvallis Health Services.
While school-aged children are the usual target, strep throat still leaves a lot of adults vulnerable, so it's important for everyone of all ages to know the key symptoms and how to get rid of it.
Strep throat can be serious
Strep throat might not seem like a big deal at first. Sometimes the symptoms — although painful — don't feel any worse than an ordinary viral illness, according to WebMD. With strep, you'll usually escape the uncomfortable upper respiratory annoyances like a runny nose and congestion. And since it is bacterial, antibiotics will clear up a case of it quickly. But without treatment, you'll remain contagious much longer and be taking a chance of significant complications.
The big risk with strep is that the bacteria that causes it can creep into other areas of your body, leaving you vulnerable to issues like rheumatic fever or tonsil abscess, which you could have avoided — in most cases — with a simple course of antibiotics, notes Yale Medicine.
Rheumatic fever is a serious disease that mostly affects children. It attacks the heart, blood vessels, and joints. The Cleveland Clinic explains that, "[Rheumatic fever] happens when the body's immune system overreacts to a strep throat or scarlet fever infection that hasn't been fully treated." It may scar your heart valves, resulting in permanent damage that can eventually lead to congestive heart failure (via Texas Heart Institute).
This is how you get strep throat
When someone coughs or sneezes who has strep throat, those respiratory droplets may enter your system and infect you with the bacteria called streptococcus pyogenes, also known as group A streptococcus. You can also get strep throat by touching contaminated surfaces and then touching your mouth, nose, or eyes, according to Yale Medicine.
Flu and viral infections are the usual reason for sore throats, and not every tickle requires a doctor visit. However, you should be evaluated for strep, mono, or even COVID-19 by your physician, says GoHealth Urgent Care, if your fever is 101 degrees or more Fahrenheit and goes longer than one to two days.
When you understand the basic concept of how disease is spread, it becomes clear why it's so easy to pick up the strep bacteria. In the days of COVID-19 and the regular wearing of masks, hand washing, and using hand sanitizer, the level of prevention many people routinely take today has helped cut down on the transmission of many other diseases. "Something we've been telling people for years," Dr. Richard Malley, infectious disease physician at Boston Children's Hospital told Time, "may finally sink in."
The tonsil myth
So you had a tonsillectomy years ago and thought that would be the end to strep throat infections. Sorry to disappoint you, but it's not. The bacteria that causes strep can still affect the tissues in the back of your throat even without tonsils, according to Healthline. Not having tonsils usually helps reduce the severity of strep throat and makes future infections less likely, according to Medical News Today, but it doesn't completely eliminate the possibility of getting the painful condition again.
Tonsillectomies aren't nearly as routine as they were decades ago, but the outpatient procedure can still be a worthwhile option for cutting down on frequent tonsil infections while also offering other health benefits. "Restless sleep or apnea due to enlarged tonsils can cause children to be hyperactive and fidgety during the day," says Dr. Avani Patel Ingley, a Piedmont Healthcare ear, nose, and throat specialist based in Georgia. "Sleep apnea can also put a strain on the heart and lungs, as well as disrupt hormones in children, which can lead to obesity."
A sore throat without cough is a hallmark symptom of strep
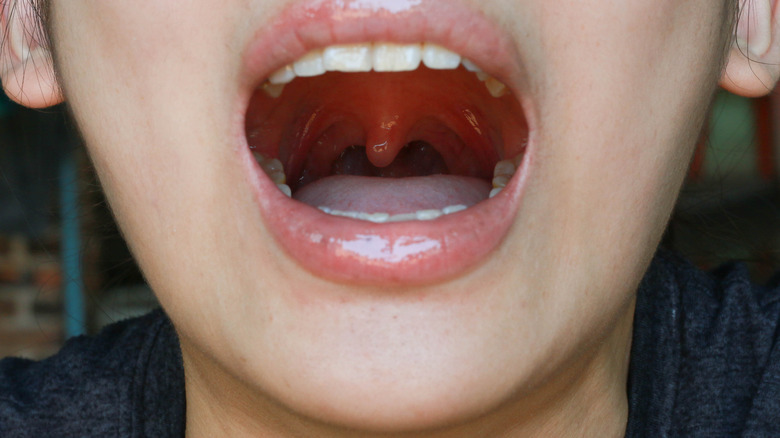
You're burning up and feeling crummy. The swollen glands on the sides of your neck are huge, and your throat is so raw that even eating or drinking feels like torture. Oh and are those white streaks on your tonsils? Anything that looks and feels this bad has got to be strep, right? Actually, maybe not.
"You do not have a cough with strep. If you're coughing, that typically means no strep," says Dr. Daniel Allan, who specializes in family medicine at the Cleveland Clinic. "Also, when you look in the throat of a person with a sore throat caused by a cold virus, you typically do not see pus or exudate in the back of the throat."
Most sore throats are viral and have upper respiratory symptoms such as a runny nose and coughing. But even though coughing is not typically a sign, your doctor may still swab your throat for a rapid test, notes After Hours Kids in Austin, Texas, if your other symptoms lean toward strep. It's the only definitive way to know if you have the condition.
Rash can sometimes accompany the disease
If your face, neck and chest are getting red and blotchy, accompanied by a fever and fiery throat, you may have the beginnings of scarlet fever. In short: strep throat with a rash. Other telltale signs of the illness include bright red areas on skin creases at the underarms, elbows, and groin, according to the Centers for Disease Control and Prevention (CDC).
Scarlet fever used to be a severe illness before antibiotics were discovered. "Certain strains" of the strep bacteria create a toxin that develops into the rash, explains Dr. Camille Sabella, director of the Center for Pediatric Infectious Diseases at the Cleveland Clinic (via Everyday Health).
The condition has a bumpy red (or scarlet) appearance, notes Yale Medicine. Although more difficult to see on darker skin, the rash will be noticeably rough like sandpaper. It pops up on the neck and chest first and then spreads over the whole body, and it can look alarming. Thankfully, antibiotic therapy will take care of the disease. Scarlet fever typically lasts about seven days, but outer layers of skin on your hands and feet may peel for weeks, according to the CDC.
The main thing is to get on a course of antibiotics right away, advises the Mayo Clinic, as dire complications such as rheumatic fever — an inflammatory disease — can lead to long-term organ damage.
Here's how strep differs from sore throat or mono
A common sore throat and strep throat may feel or even look similar, and both can be bacterial. However, most run-of-the-mill sore throats are caused by viruses from a cold or flu. Strep throat has some important differences that set it apart.
"Aside from getting body aches and fatigue, you don't tend to have a lot of other symptoms with strep throat. You don't tend to get runny noses; you don't get cough or other respiratory problems. It usually is isolated just to the throat," explains Dr. Craig P. Chase, a partner of Oviedo Medical Research in Florida.
Sometimes a really bad sore throat could actually be mononucleosis, known as "mono" or the "kissing disease," explains the Mayo Clinic. The illness features a raw, red throat, swollen tonsils, and swollen glands in the neck, just like other sore throats or strep. But while you'll typically feel tired and rundown with any illness, mono is known for really wiping you out.
Unlike strep, mono is caused by a virus — specifically the Epstein-Barr virus — characterized by extreme fatigue that may linger for months. Mono may also lead to jaundice or an enlarged spleen (via Johns Hopkins Medicine). So unlike strep throat, which is bacterial and is cured by antibiotics, mononucleosis is a long-term viral condition.
What you think is strep could actually be something else
A 2015 study at a University of Alabama health clinic reported that more students with strep-like symptoms were actually infected with the bacteria Fusobacterium necrophorum, and not group A streptococcus. It's a significant finding, because if left untreated it can lead to severe health consequences.
"Fusobacterium is an anaerobic bacterium, so routine throat culture will not pick it up ... nobody had previously determined what it looks like compared to strep," says Dr. Robert Centor, lead author and a professor at the University of Alabama School of Medicine. "[It] looks just like strep pharyngitis and explains a lot of the people that we might want to give antibiotics to but have a negative strep test," he told Reuters Health.
The bacteria is the leading cause of Lemierre's syndrome, a rare but dangerous condition that affects otherwise healthy teens and young adults who had a bacterial throat infection, explains the NIH. It's also "a more common side effect than [strep's] acute rheumatic fever," warns Dr. Centor (via The University of Alabama at Birmingham).
The concern is that antibiotic treatment might be delayed if a patient infected with Fusobacterium necrophorum was assumed to have strep, and only received a strep test with a negative result. Without antibiotics, the condition could progress to the serious Lemierre's syndrome, American Family Physician reports. Early intervention with antibiotics can cure both types of these bacterial illnesses.
This is how a doctor will diagnose you
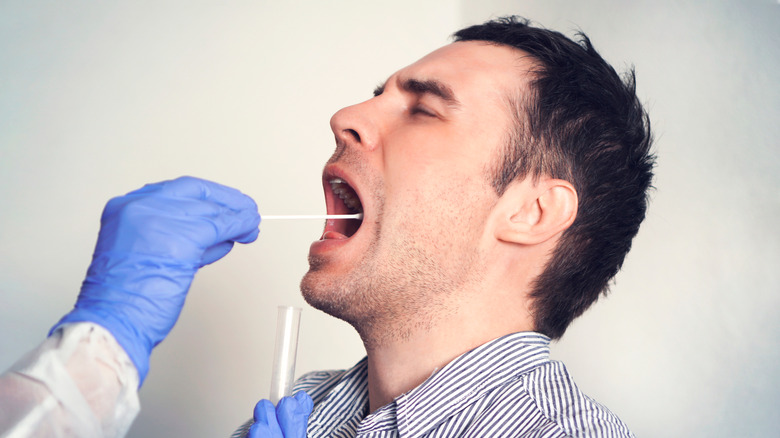
Common signs of strep throat that doctors look for are fever, chills, sore throat that hurts when swallowing, white patches on the throat, and swollen neck glands, says the Icahn School of Medicine at Mount Sinai. However, the only way to really know if you have strep is by getting a positive result on a rapid strep test or a throat culture.
Your doctor will use a long cotton swab for collecting some fluid from the back of your throat, and you'll get results from the rapid test within minutes. "Many times, a doctor may give antibiotics thinking that it's pus — when it's not," says Dr. Jason Abramowitz, physician at ENT and Allergy Associates in New York, according to The Healthy.
White spots or pus on your tonsils can be an indication of strep — especially if you have some of the other classic symptoms — but it's definitely not a conclusive sign. It could just be calcium deposits from tonsil stones, or a common case of tonsillitis, (via Healthline).
You might be concerned you have COVID-19
Every sniffle, sore throat, or twinge of headache pain in life's new-normal leads many to question even the smallest signs of illness. In a nervous whisper, we ask ourselves: "Could it be COVID?"
"We as a society used to be kind of dismissive of cold symptoms, but we can't be dismissive of them now," warns Dr. Brian Curtis, vice president of Clinical Specialty Services for OSF HealthCare in Illinois. "If you have just a sore throat with no other symptoms, it's less likely to be COVID-19. But with other symptoms, it is possible you have COVID. Sore throat, cough, fever — I would be worried about COVID."
Of course, not all of our aches and pains are coronavirus, but some symptoms for the Omicron variant and strep throat do overlap. Dr. Allison Arwady, commissioner for the Chicago Department of Public Health, told NBC 5 that instead of coughing and shortness of breath, breakthrough COVID-19 infections for the fully vaccinated are oftentimes just mild illness. "They may only feel like they have a cold," she says, instead of "seriously ill and having fevers for days and difficult breathing." Luckily, both strep and COVID-19 can be diagnosed with simple rapid tests. Strep throat is usually a mild bacterial ailment when treated early with antibiotics.
The best meds for strep treatment
Before antibiotics, strep throat could kill you. It still can, as there's no vaccine for it, but antibiotics make it a very treatable and even mild disease these days. Like so many other bacterial illnesses, the turning point for strep throat was antibiotics. British scientist Alexander Fleming discovered the naturally growing bacteria-killing substance, penicillium mold, in the 1920s. Penicillin became the wonder drug. After extensive testing and use during World War II "curing battlefield wound infections and pneumonia," penicillin was finally available to the general public by the late 1940s (via the American Academy of Pediatrics).
Unlike common sore throats whose origins are overwhelmingly viral, strep throat is caused by bacteria, so "antibiotics will quickly wipe out the bacteria causing the infection," explains the Mayo Clinic.
"The treatment for a strep infection is antibiotics and, sometimes, steroids to decrease the inflammation," explains Dr. Karla O'Dell, otolaryngologist at Keck Medicine of USC. As a bacterial infection, the first-line course of antibiotics for strep are penicillin and amoxicillin, or non-penicillin options like Zithromax to speed you back to health (via WebMD).
Without antibiotics you're contagious for much longer
Antibiotics are not always the most comfortable medicine to take, as they can take a toll on your gut and make you feel nauseous or have an upset stomach (via Healthline). So do you really need to take antibiotics to beat strep throat? The short answer is no, according to MyHealth Alberta, but you're taking a chance if you don't. "Strep throat will usually resolve without antibiotics within seven to 10 days, but there is increased risk of other conditions [like rheumatic fever] and a person stays contagious for two to three weeks," Dr. Toni Brayer, internal medicine physician in San Francisco, told Singlecare.
Making sure all that nasty group A strep bacteria is completely gone is very important. Without finishing a full course of antibiotic therapy, it's possible that you may still have lingering strep bacteria that could spread to other parts of your body. If that happens, it puts you at risk of complications from the disease, according to Blueberry Pediatrics. Rheumatic fever and organ damage are real problems that severely affect your health, so why put yourself at needless risk?
The isolation factor
It's a real drag to take yourself away from things you want to do and people you want to see, but we're probably all used to it now anyway because of the COVID-19 pandemic. Strep throat is a disease that spreads easily. So if you have symptoms and haven't been treated with antibiotics yet, you need to isolate to protect others.
"Strep throat is very contagious," says Dr. Soma Mandal, board-certified internist at Summit Medical Group in New Jersey. "Typically, the bacteria spreads through sneezing and coughing," she told Singlecare. It can also spread to others by sharing drinks or personal items, or by touching surfaces like doorknobs or a table then touching your mouth or eyes.
The good news is once you get diagnosed and start on a course of antibiotics, you should begin feeling a lot better within 24 to 48 hours — and no longer be contagious (via the CDC). However, if you go without antibiotics, you're looking at up to a week to 10 days of symptoms and two to three weeks of isolation, plus possible serious complications, warns UrgentCare Omaha. Knowing these facts makes it an easy decision to seek early treatment.
Here are some ways that offer relief from symptoms
While you wait for your antibiotics to do their job, treating the symptoms and nourishing your body are incredibly important. Top of the list are getting plenty of rest, gargling with warm salt water to reduce throat irritation, and — if needed — taking over-the-counter pain relievers ibuprofen or acetaminophen for fever and body aches. Not everyone has a humidifier, but if you do, use it! (via Singlecare)
When your throat feels like broken glass shards, warm and cold foods both provide relief if they're easy to swallow and, importantly, non-acidic, advises Livestrong. So put down the crusty piece of bread, deep-fried chicken leg, and stay away from spicy sauces — but say yes to mashed potatoes, apple sauce and scrambled eggs.
Have you heard how chicken soup is good for the soul? It's also good for easing throat pain. Age-old favorites like soup and tea became classics for a reason, they're restorative and easy to digest (per MedicineNet). "A warm drink like tea can help soothe throat irritation, and compounds in tea might help calm inflammation and relieve pain," says Samantha Cassetty, a registered dietician (via Insider). Reach for teas with anti-inflammatory properties like green tea or ginger root, or that create a gel-like coating, such as slippery elm.
Strep can return
You don't build immunity after having strep throat. So that means you can get it again and again. In fact, there was even one weird and unusual case when all five members of a Wisconsin family kept getting recurrent bouts of strep from their pet cat, according to The Washington Post.
"But recurrent strep throat is a big concern in the developing world because kids who do not get antibiotics have a real risk of developing acute rheumatic fever or rheumatic heart disease, which is a major cause of acquired heart disease among young adults in the world," warns Dr. Jennifer M. Dan, infectious disease specialist at UC San Diego Health (via La Jolla Institute for Immunology). A 2019 study concluded that immunological factors combined with genetic susceptibility were prime factors for recurrent strep infections in children.
Besides finishing your antibiotic therapy, Yale Medicine advises throwing out your toothbrush and washing your bedding to avoid spreading the bacteria to others or getting yet another round of it yourself.