Symptoms Of Endometriosis You Shouldn't Ignore
Endometriosis is a chronic gynecological condition. According to Johns Hopkins Medicine, endometriosis occurs when tissue similar to the lining of the uterus grows outside the uterus. This diseased tissue is most often found on the outside of the uterus, the ovaries, the fallopian tubes, the bowels, or the bladder (per MedlinePlus). However, endometriosis tissue can grow anywhere in the body. In rare cases, it's even been found in the lungs.
This errant tissue behaves just like the tissue that lines the uterus. Each month when a person's menstrual cycle occurs, the diseased tissue follows the same pattern as the lining of the uterus. First it builds up, getting thicker and thicker to prepare for the implantation of a fertilized egg. When a fertilized egg doesn't implant, the tissue starts to break down.
When this process happens to the endometrium that lines the uterus, the broken-down lining expels itself from the body in the form of menstrual blood. The endometrium-like tissue outside the uterus cannot expel itself from the body. So when it starts to break down, the tissue bleeds, which leads to swelling, inflammation, tissue damage, and eventually scarring. This can lead to intensely painful and difficult periods.
Despite what people with uteri are often told, periods should not be intensely painful or difficult. If they are, endometriosis can be the cause. Here are some symptoms of endometriosis that you should never write off as "just a bad period."
Painful menstrual cycles
Anyone who's had a menstrual cycle knows that they come with some pain. Abdominal and pelvic cramps are common symptoms associated with a normal menstrual cycle. However, cramps so painful that they interfere with your life are not normal, per the Endometriosis Foundation of America.
Normal menstrual cramps can be treated with over-the-counter medications like Ibuprofen or Tylenol, and they don't interfere with day-to-day functioning. Menstrual cramps caused by endometriosis are debilitating. These cramps are so painful that people need to stay home from work or school or leave social events. Some people cannot even leave their beds when they have endometriosis cramps. And they cannot be treated with over the counter pain medications or home remedies like warm baths or showers or heating pads.
People with endometriosis often get painful cramps multiple times throughout their cycle instead of just the week before menstruation. The most common times that people with endometriosis experience these painful cramps is during ovulation, the days leading up to menstruation, and through menstruation.
If your menstrual cramps are so painful that you're missing out on your life and they occur at multiple times of the month for days at a time, don't ignore them! Normal menstrual cycles should not interfere with your life or put you in agony.
Heavy menstrual bleeding
According to the Cleveland Clinic, menstrual bleeding is classified as heavy when it lasts for more than seven days or when you lose an excessive amount of blood during menstruation. People with heavy menstrual bleeding often have to change their tampon or pad several times a day, sometimes every single hour. Sometimes people who experience heavy menstrual bleeding will expel blood clots, which can be the size of a quarter or even larger. Some people with heavy menstrual bleeding will lose so much blood that they develop secondary symptoms like chronic fatigue, shortness of breath, and anemia.
Many people dismiss heavy menstrual bleeding as a "bad period" because they believe that heavy bleeding is just part of having a menstrual cycle. But it's not! If you have to wear a tampon and a pad at the same time and excuse yourself to change them, that's not normal menstruation. If you regularly pack a second pair of underwear and pants because you think you might bleed through your clothes, that's not normal menstruation. If you're skipping out on life because of your menstrual bleeding, that's definitely not normal.
Several conditions can cause heavy menstrual bleeding, and endometriosis is one of them, according to the Mayo Clinic. So if your heavy menstrual bleeding is interfering with your life for multiple days out of each month, it's time to talk to your doctor.
Bleeding between periods
Heavy menstrual bleeding isn't the only kind of vaginal bleeding that can indicate a chronic gynecological illness like endometriosis. According to the Mayo Clinic, vaginal bleeding or spotting between your regular periods is a common symptom of endometriosis. A small study published in the American Journal of Gynecology and Obstetrics found that 89% of study participants with endometriosis experienced vaginal bleeding or spotting between their periods.
Medical News Today defines vaginal bleeding or spotting between periods as any bloody discharge that occurs after the last day of your period and before the beginning of the next period. If you have irregular periods, it can be hard to determine the beginning and the end of your cycle if you experience bleeding between periods. But if you're bleeding and your period just happened or isn't due for a few days, then that's classified as bleeding or spotting between periods.
Most of the time, spotting or bleeding between periods isn't a big deal. There are a lot of reasons why this can happen including hormonal shifts, birth control, missed miscarriages, pregnancy, and sexually transmitted illnesses. However, if you regularly experience vaginal bleeding between your periods, it could be because of endometriosis. If you also have heavy periods and extremely painful cramps, this specific combination of symptoms is highly indicative of endometriosis.
Pain during sex
Another telltale sign of endometriosis is pain during sex. According to Everyday Health, the type of pain experienced during sex by people with endometriosis varies from person to person. While one person might experience a dull, aching pain during sex, another may experience sharp, stabbing pain. Some people only experience pain with deep vaginal penetration, while others experience pain with vaginal penetration of any kind. For some people, the pain even persists after sex is done, sometimes for days.
The misplaced, endometrium-like tissue characteristic of endometriosis often grows on the uterus, the ligaments surrounding the uterus, the cervix, and the vagina. This tissue often damages the surrounding healthy tissue (via Johns Hopkins Medicine). During sex, this damaged tissue is moved and stretched by penetration, which irritates it, leading to pain.
Any kind of persistent pain during vaginal penetration, even if it's mild, should be discussed with a gynecologist or primary care physician as soon as possible. It's not normal to experience pain during penetration. Pain during sex isn't always a sign of endometriosis. However, it's often one of the earliest signs of the disease.
Pelvic and abdominal pain between periods
Most people who experience menstruation are familiar with the abdominal and pelvic cramps that often occur in the days leading up to and during menstruation. Though these cramps can be painful enough to interfere with regular life, they're usually gone within a few days.
This is not the case for many people with endometriosis. According to a paper on endometriosis and pelvic pain published in the medical journal Nursing for Women's Health, endometriosis can cause near-constant pervasive pelvic and abdominal pain so severe that it significantly impacts people's quality of life. When this pain lasts for six months or longer, it's classified as chronic pelvic pain. Between 71% and 87% of people with chronic pelvic pain have endometriosis, though chronic pelvic pain has myriad causes. In some cases, chronic pelvic pain is caused by a combination of co-occurring conditions like endometriosis, interstitial cystitis, and irritable bowel syndrome.
Another paper on endometriosis and pelvic pain published in the medical journal Frontiers in Cellular Neuroscience stated that over 60% of people with endometriosis reported that they had chronic pelvic pain, and people with endometriosis were 13 times more likely to experience chronic pelvic pain that healthy people who experienced menstruation.
So if you have debilitating cramps, regardless of whether or not you're menstruating, it's definitely worth talking to your doctor about endometriosis.
Pain when you go to the bathroom
When you think about symptoms of gynecological illnesses, the first symptoms that come to mind probably don't have anything to do with your gastrointestinal or urinary tracts. However, painful bowel movements and painful urination can definitely be symptoms of endometriosis, according to Endometriosis.net.
Some people with endometriosis experience pain with urination, almost like an urinary tract infection, but without an infection. Some people also describe uncomfortable pressure when they urinate. Other people have trouble passing bowel movements. They experience uncomfortable pressure and pain in their anus and rectum even when they're not constipated and passing a relatively soft stool. Some people have painful bowel movements but not painful urination, while others experience both. The symptoms usually occur around the time of menstruation.
Doctors and researchers that specialize in endometriosis aren't entirely sure why the disease causes bladder and bowel pain. One potential reason is that diseased tissue can grow directly on the bladder and bowel, which creates lesions on these organs. Another possibility is that scar tissue from the lesions can build up in the pelvic cavity and prevent the organs from functioning as they should. Yet another theory is that the persistent inflammation caused by the lesions and scar tissue can impact the function of both the bowel and the bladder. Regardless of the reason, bladder and bowel pain that can't be explained by other pathologies may well be a sign of endometriosis.
Chronic digestive problems
While many people experience some digestive problems around the time of their period, most don't experience chronic, persistent digestive issues that just don't seem to go away. If you are dealing with frequent GI upset along with difficult periods, then endometriosis might be the cause. According to Healthline, people with endometriosis often experience chronic constipation, diarrhea, bloating, gas pain, and nausea.
A study of 174 women with and without endometriosis published in the medical journal BioMed Central Women's Health found that women with endometriosis reported more severe gastrointestinal issues than women without endometriosis. The study also found that gastrointestinal issues for the women with endometriosis were so severe that they regularly impacted their day-to-day lives. Interestingly, the study concluded that the severity of GI symptoms had little to do with where endometriosis lesions were found in the pelvic cavity, except in the cases where they were found directly on the bowel.
A meta-analysis of studies on women with both endometriosis and irritable bowel syndrome (IBS) found that women with endometriosis are twice as likely to have IBS than women without endometriosis. The review also found that there is significant evidence of a link between endometriosis and IBS. Because of this, people often get diagnosed with IBS while an endometriosis diagnosis is missed. The study suggested that people with IBS who have a menstrual cycle should be evaluated for endometriosis as well.
Chronic urinary tract problems
Chronic problems with urination that won't go away and can't be explained by other diseases can also be a sign of endometriosis. According to Verywell Health, there are two explanations: bladder endometriosis and interstitial cystitis (IC), also known as painful bladder syndrome.
Bladder endometriosis occurs when diseased tissue implants itself on the outside of the bladder or the ureters. This tissue tries to shed each cycle, causing lesions and scar tissue to build up on the bladder and/or ureters, inhibiting their proper function. Bladder endometriosis can cause uncomfortable symptoms like painful urination, bladder pain, pelvic pain, lower back pain, needing to urinate all the time, an urgent need to urinate, and even blood in the urine.
Another cause of urinary tract issues that often coincides with endometriosis is interstitial cystitis or painful bladder syndrome. Though endometriosis doesn't cause IC, the conditions often occur together. Experts believe that as many as 66% of people with endometriosis have interstitial cystitis. IC is a diagnosis for a collection of symptoms. The hallmark symptoms are constant pain and pressure in the urinary tract, accompanied by other urinary symptoms like painful, frequent, or urgent urination. Again, not all people with IC have endometriosis, but those who do should be evaluated for the disease.
Chronic urinary tract problems can be caused by a wide variety of conditions other than endometriosis. But if other conditions have been ruled out, it's worth being evaluated for endometriosis.
Infertility
Though not all people with endometriosis deal with infertility, experts believe that between 30% and 50% of people with endometriosis struggle with infertility, according to a paper published in the medical journal Obstetrics and Gynecology Clinics of North America. Another article published in the Journal of Assisted Reproduction and Genetics found that people with infertility are six to eight times more likely to have endometriosis than fertile people.
According to Medical News Today, endometriosis isn't necessarily the root cause of infertility even when both conditions are present. However, endometriosis contributes to infertility in several ways. Diseased tissue and scar tissue caused by endometriosis can build up in the pelvic cavity and directly on the organs involved in reproduction, which can make it very difficult to get pregnant. For example, tissue or scar tissue might block the fallopian tubes (so an egg can't travel to the uterus) or cover the ovaries and interfere with egg production. Endometriosis can also cause secondary issues that make it difficult to get pregnant. Endometriosis often creates severe hormonal imbalances, which throws off the menstrual cycle and ovarian function. Endometriosis also causes a ton of inflammation in the pelvic cavity, which can disrupt the function of the organs involved in reproduction.
Luckily, treatments for endometriosis like surgery and hormone therapy can often help people with endometriosis get pregnant. Assisted reproductive technology like intrauterine insemination (IUI) and in vitro fertilization (IVF) can also help people with endometriosis get pregnant.
Chronic back and/or leg pain
According to The Femedic, back and leg pain is a common symptom for people with endometriosis. Since the endometrium-like tissue associated with endometriosis can grow nearly anywhere in your body, it's not uncommon for it to grow on the ligaments and nerves around the low back. This causes damage to these ligaments and nerves, leading to inflammation which causes chronic back pain.
Chronic back pain from endometriosis often feels like an ache or a sharp pain deep within your back. Some people with endometriosis experience this pain only around their period. Others experience back and leg pain all the time. According to Healthline, the disease tissue can also grow on and around the sciatic nerve, which can lead to pain that shoots or radiates down your leg. This pain is often described as sharp and stabbing or dull and throbbing, and it can switch back and forth between the two sensations.
Back and leg pain caused by endometriosis doesn't respond to typical treatments like stretching, changing position, or chiropractic adjustment. For some, over-the-counter pain medications like Ibuprofen and Aspirin provide relief. However, many people with endometriosis find that these remedies don't touch their pain. Other common home remedies include heating pads and hot baths. If you have chronic back and/or leg pain that hasn't been explained by another condition along with any of the other symptoms of endometriosis, definitely talk to your doctor.
Migraines
Several studies have shown a strong connection between endometriosis and migraines. One study published in the Journal of Endometriosis and Pelvic Pain Disorders found that women with endometriosis were significantly more likely to suffer migraines than women without endometriosis. Another study on endometriosis and migraines published in the medical journal PLOS One found that women with endometriosis were 37% more likely to get migraines than women without endometriosis. A third study on the subject published in the medical journal Current Pain and Headache Reports found that endometriosis is also more common in the population of people who get migraines than in the population of people who don't get migraines. Women with endometriosis also had more migraines per month than women without endometriosis, according to the same study.
Though the correlation between migraines and endometriosis is strong, doctors and researchers aren't quite sure why. They don't know if either condition causes the other or if the conditions have a common cause. One theory is that both migraines and endometriosis are influenced by the sex hormone estrogen and imbalances in this hormone cause both endometriosis and migraines. Another theory is that the synthetic hormones people often take to control the symptoms of endometriosis may cause migraines.
If you're a migraine sufferer who often gets migraines associated with different stages of your menstrual cycle, it's possible you may also have undiagnosed endometriosis. Check in with your doctor if you have migraines along with any other symptoms of endometriosis.
Severe and chronic fatigue
One study on fatigue and endometriosis published in the medical journal Human Reproduction found that a majority of people with endometriosis struggle with severe and chronic fatigue. The study also concluded that women with endometriosis are twice as likely to experience fatigue than women without endometriosis. Additionally, the study revealed that severe and chronic fatigue is one of the common symptoms of endometriosis that has the biggest impact on quality of life.
Another study that assessed the impact of fatigue in women with endometriosis found that fatigue had a significant impact on their quality of life. More than two-thirds of the participants said that their fatigue was "extremely bothersome" or "quite bothersome." They reported that fatigue regularly limited their ability to complete day-to-day tasks, succeed at work, and maintain strong relationships. They also stated that fatigue had a major impact on their emotions and overall mood.
The study included interviews with each of the subjects, during which they described their experience of fatigue. The women said that they often felt "exhausted, drained, tired, lethargic, worn out, and/or weak," and that they were often too tired to complete basic self-care activities like showering, washing their hair, and brushing their teeth. Additionally, the participants stated that they often canceled plans or avoided social situations because of fatigue, and that fatigue prevented them from exercising. So if you're tired and drained all the time and it's impacting your daily life, it could be a sign of endometriosis.
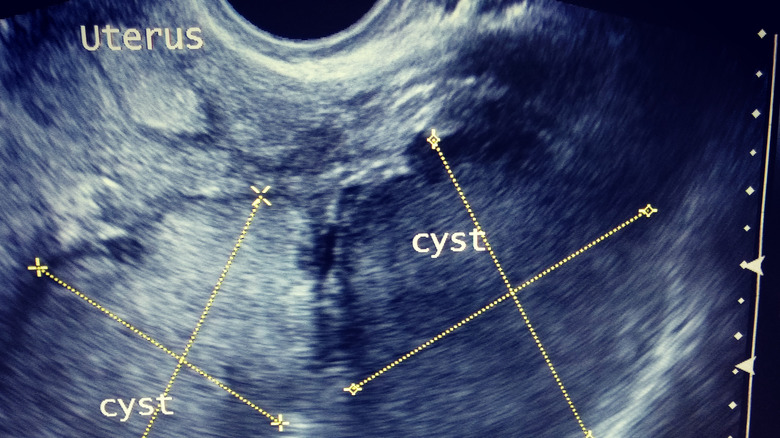
Ovarian endometrioma, or "chocolate cysts"
Ovarian endometriomas are a specific kind of ovarian cyst that develops only in people who have endometriosis, per the Cleveland Clinic. These cysts are filled with menstrual blood, which makes the cysts look like they're filled with chocolate syrup. That's why they're nicknamed "chocolate cysts." Between 17% and 44% of people with endometriosis will develop an ovarian endometrioma at some point.
Doctors and researchers that specialize in endometriosis don't have a definitive explanation for why ovarian endometriomas happen or why only some people with endometriosis get them. The predominant theory is that when endometrium-like tissue grows on the ovaries and bleeds with each menstrual cycle, the blood pools and forms ovarian endometriomas.
The most common symptoms of ovarian endometriomas are the same as the classic symptoms of endometriosis — pelvic and abdominal pain, nausea, back pain, pain during sex, pain when you go to the bathroom, and painful periods.
If your doctor suspects that you have an ovarian endometrioma, they'll likely do a transvaginal ultrasound, a cat scan, and/or an MRI to visualize the cyst. However, these tests can only confirm the presence of a cyst, not whether it's actually an ovarian endometrioma. If the cyst is small, your doctor may recommend monitoring it to see if it resolves on its own. If the cyst is large or causing significant symptoms, your doctor will likely schedule laparoscopic surgery to remove the cyst. Then, they can take biopsies to confirm if it is actually an ovarian endometrioma.
Diagnosing and treating endometriosis
Endometriosis cannot be definitively diagnosed without laparoscopic surgery, per the National Institute of Health. Though diagnostic tests like ultrasounds and MRIs can provide your doctor with information that suggests endometriosis, they cannot definitively diagnose endometriosis.
If you have several of the symptoms of endometriosis, your doctor may unofficially diagnose you with endometriosis and start treatment like hormonal birth control or hormone therapy, per the Office on Women's Health. If you get significant relief from these treatments, then you most likely have endometriosis, and your doctor will continue to treat your symptoms with a combination of hormone therapy, birth control, and/or pain medications. If your symptoms are severe and these methods do not provide relief, your doctor will likely recommend laparoscopic surgery. Your doctor will make several small incisions in your abdomen and insert a special instrument to visualize the inside of your abdomen. This will allow them to see where the endometrium-like tissue has grown and formed lesions and adhesions. During the same procedure, they can remove the diseased tissue, lesions, and adhesions. They will also do biopsies to confirm the endometriosis diagnosis. Once the endometrium-like tissue is removed, many people find great relief from their symptoms. However, the tissue can regrow, causing symptoms to recur. Some people need multiple surgeries for endometriosis.
If you have any of these signs or symptoms of endometriosis, do not ignore them! Schedule an appointment with your gynecologist ASAP to see what they think.