14 Ways To Help Manage Pain After Surgery
Let's be real. Recovering from surgery can be downright uncomfortable. Depending on what you've had done, it could be just a nagging inconvenience that lasts a day or two, or something much more profound that incapacitates you for weeks or months. So there's simply no one-size-fits-all solution when it comes to pain management.
And some people really are more hypersensitive to pain, a study of MRI brain scans shows (via Science Daily). So it stands to reason that post-treatment plans need to be tailored to individual needs. "We have all met people who seem very sensitive to pain as well as those who appear to tolerate pain very well," says Robert C. Coghill, a professor of neurobiology and anatomy at Wake Forest University Baptist Medical Center. "Until [this study], there was no objective evidence that could confirm that these individual differences in pain sensitivity are, in fact, real."
While you should always consult with your own medical team first for the best treatment and pain management options for you, many options do exist. These range from opioid medication and nonsteroidal anti-inflammatory drugs (NSAIDs) to acupuncture and physical therapy. "Letting patients choose how they'd like to manage their pain is vitally important," says Dr. Shalini Shah, director of Pain Services at UCI Health in Irvine, California. "Patients should feel free to ask their doctor or a pain specialist questions about pain medications."
NSAIDs and acetaminophen
It's easy to think that something as common and as easily accessible as Motrin or Tylenol is not going to cut it when you're looking for real pain relief. But research tells a different story. In a 2021 study published in the Annals of Surgery, non-opioid drugs such as ibuprofen and acetaminophen were actually shown to be just as effective as opioid painkillers for relieving pain after surgery — if they are taken consistently and at the frequency recommended by the physician. Surprisingly, patients reported no difference in their comfort level or satisfaction of care in a postoperative survey.
"NSAIDs work by blocking key pain-signaling molecules," explains Jamie Alan, assistant professor of pharmacology and toxicology at Michigan State University, to Verywell Health. "The key with NSAIDs and acetaminophen is to use the medications 'around the clock.' This means you don't take the medicine when you feel the pain, but you keep on top of the pain by taking these medications on a scheduled basis."
Chiropractic
You may not think about chiropractic care as having a place in your recovery, but for certain conditions, chiropractic adjustments can be beneficial in improving joint movement after surgery. Numerous case studies, including those in the Journal of Chiropractic Medicine and the Journal of Manipulative and Physiological Therapeutics, have shown that people suffering from lingering postoperative pain were helped by chiropractors.
According to Total Chiropractic Care in New York, manual adjustments and soft tissue therapies performed by a chiropractor can be a part of an overall rehabilitation plan for many different types of surgeries — including those for the back, knees, and feet — after consultation with the patient's surgeon.
"Many patients who undergo back surgery have a higher satisfaction rate if it is combined with additional therapies after surgery," notes Wooster Community Hospital Health System in Ohio. "Generally, after a year following back surgery, you should be able to seek chiropractic care. Make sure to check with your surgeon first as some people have complications that need to be considered."
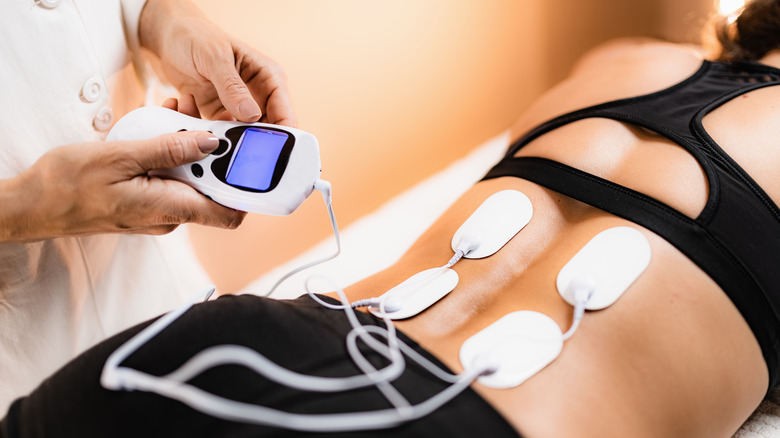
Electrical stimulation
Ready to shock your pain into submission? Electrical stimulation, or electrotherapy, can help dull your pain. The concept of this type of therapeutic treatment goes back to the Romans, who used electricity-producing black torpedo fish for pain relief, according to The New York Times. But don't worry, your healthcare provider won't zap you with electrified fish. Modern methods are much less hair-raising.
Instead, your physical therapist or doctor will use a transcutaneous electrical nerve stimulation (TENS) device, which delivers low-voltage electrical pulses through your body, explains OrthoInfo. Small electrodes on adhesive pads will be attached on your skin along nerve pathways. Those electrodes will produce a focused electrical pulse that will feel like tingling or muscle twitching, depending on the intensity selected. The electricity is thought to release natural hormones that block pain signals in the brain. Chiropractors, physical therapists, and many doctors use TENS devices routinely. According to WebMD, "[TENS is] most effective in treating mild to moderate pain after several types of operations, including heart surgery, chest surgery, hysterectomy and other gynecological surgeries, orthopedic surgery, and abdominal surgery."
Opioids
When you have surgery, the main form of pain relief your doctor provides — at least for a couple of days — is often in the form of narcotic drugs. "Historically, it wasn't uncommon to see American physicians send patients home with a 30-day supply of opioid medication after surgery," confirms Dr. Shalini Shah, director of Pain Services at UCI Health.
Opioid medications are still routinely written for postoperative pain for many patients in the United States, with 30% of them prescribed for orthopedic and spine conditions, says WebMD. One obvious problem with this practice is that opioids are highly addictive, and for some people the physical addictions can take hold within just a few weeks, warns Johns Hopkins Medicine. Another problem is specific to the elderly, who may have stronger reactions to opioids that make them feel "confused, disoriented, or delirious," warns Dr. Paul F. Lachiewicz, orthopedic surgeon at Duke University Medical Center in North Carolina (via Healio).
The Centers for Disease Control and Prevention (CDC) reports that more than 70,000 people in the U.S. died from overdoses in 2019, and about 70% of those were from opioid drugs. "Opioids have been a routine part of postsurgical pain care for decades, but the risk that they could lead to persistent use has been clearly documented," says Dr. Ryan Howard, lead author of a 2021 opioid study, to Michigan Medicine. "Perhaps it's time to make [opioids] the exception, not the rule."
If you or anyone you know is struggling with addiction issues, help is available. Visit the Substance Abuse and Mental Health Services Administration website or contact SAMHSA's National Helpline at 1-800-662-HELP (4357).
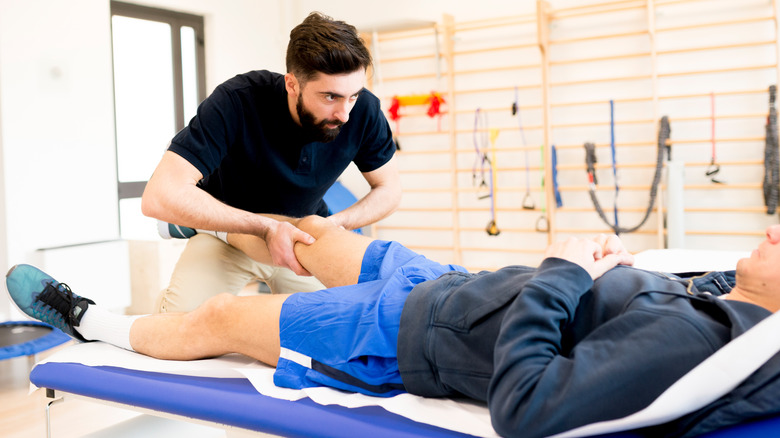
Massage therapy
When you're in constant pain, a massage is no longer an indulgence — it's a necessity. For a medical or therapeutic massage, the end goal isn't relaxation and stress relief, but instead it's to facilitate the healing of your medical condition, notes the Mayo Clinic College of Medicine and Science. Medical massage therapists have advanced training and typically work in clinical settings.
So don't expect your massage sessions to be soothing, spa-like experiences. A licensed massage therapist (LMT) will use a variety of techniques, but will spend a lot of time on deep-tissue work, myofascial release, and trigger point massage. These targeted methods will not address the whole body, but instead will focus on specific problem areas. For example, they can stimulate your lymphatic system to lessen swelling and increase circulation with lymphatic drainage massage, or use trigger point or deep-tissue massage to soften and release stubborn muscle knots, explains the Cleveland Clinic.
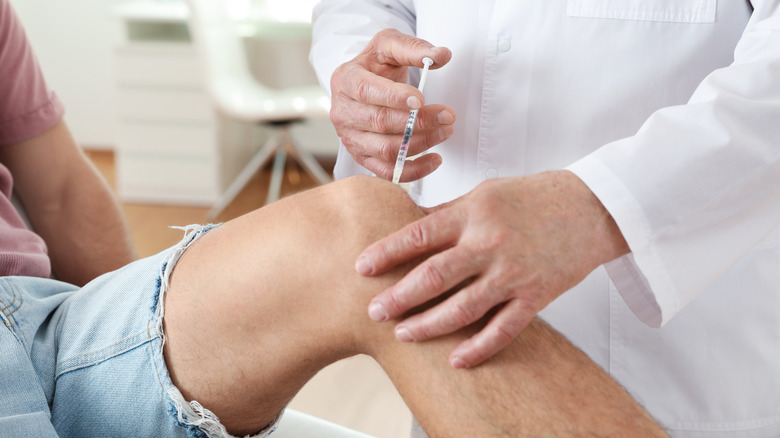
Local anesthetics
If you've ever had a cavity filled, a mole removed, or stitches for a deep cut, then you've probably been given a local anesthetic. For minor surgical procedures that don't need the heavy-hitting general anesthesia that knocks you out cold, local numbing works great (via Medical News Today). It's routinely used in medical and dental practices, and is sometimes combined with sedating medications. The most common local anesthetic used in the United States is lidocaine, but believe it or not, cocaine came first (though it's rarely used today).
What makes these numbing drugs so effective is that they prevent the nerves from sending signals to your brain, and they are low-risk, says U.K.'s National Health Service. The effects can last several hours and keep you pain free for a bit even after you get home from surgery. Besides injectables, local numbing can also come in the form of topical sprays, gels, ointments, and transdermal patches, which are convenient for at-home use (via MedicineNet) for dulling pain you may be having in small areas of the body.
Hot or cold therapy
Sometimes the simplest things are the best, and this is definitely the case with the tried-and-true ice pack or heating pad. When you sprain an ankle you grab an ice pack, right? It's the same principle with surgeries. Ice usually comes first to help with the body's initial response to acute injury, as cold narrows blood vessels and reduces the swelling to the injured area. As Three Rivers Orthopedic Services notes, "Using ice is critical for use after procedures such as total joint replacements, joint manipulations under anesthesia, fusions, tendon repair, etc." Indeed, a number of studies have shown that applying ice postoperatively offers effective pain relief for surgery patients, even after major abdominal procedures (via Reuters Health) and emergency surgery for sports injuries (via BMJ Open Sport & Exercise Medicine).
Heat does the opposite of ice — it widens blood vessels and stimulates blood flow — which makes it effective to manage pain over the long-term. Three Rivers Orthopedic Services says that "Heat is great to use for more chronic-type pain. A lot of patients find it helpful to loosen arthritic, stiff joints, and also to relax muscles and decrease spasm."
Guided imagery and meditation
Guided imagery is the act of focused relaxation (via GoodTherapy). The idea behind it is that the mind is a powerful healing tool, so by concentrating on peaceful images, sounds, or experiences, you can calm your mind and feel less physical pain. So instead of working yourself up with negative thoughts that produce more stress, you instead do the opposite and train your mind to think of positive, peaceful things.
GoodTherapy describes guided imagery techniques as similar to hypnosis, except that hypnosis focuses on suggestion whereas guided imagery targets the senses. It's possible to teach yourself guided imagery with the aid of online scripts and self-help books, but for the most benefit it's recommended to see a trained professional first.
"Guided imagery may significantly reduce stress and anxiety before and after surgical and medical procedures," says the Cleveland Clinic, adding that over 200 research studies have shown that mind-body techniques may reduce anxiety, shorten recovery times in hospitals, and limit the need for painkillers after surgery.
Acupuncture
Sticking needles in the body to reduce pain? It sounds counterintuitive, but that's exactly what acupuncture can accomplish. Practiced in traditional Chinese medicine for thousands of years, acupuncture restores balance of the life force Qi (pronounced "chee") in the body. Practitioners believe that any imbalance of this life force can cause disease and illness, explains Johns Hopkins Medicine. Qi flows through meridians, or pathways, and an acupuncturist inserts long, thin needles into specific acupuncture points to bring the energy flow back into balance.
It may sound like magic, but many studies have shown that acupuncture can work. In one example, randomized controlled trials found that hospital patients treated with acupuncture for pain relief after surgeries experienced less pain and used fewer opioid painkillers than those who didn't receive the treatment (PLOS One).
"Each acupuncture needle produces a tiny injury at the insertion site, and although it's slight enough to cause little to no discomfort, it's enough of a signal to let the body know it needs to respond," explains licensed acupuncturist Paul Kempisty to Healthline. "This response involves stimulation of the immune system, promoting circulation to the area, wound healing, and pain modulation."
Therapeutic touch and Reiki healing
Some people describe the holistic practice of Reiki as "acupuncture without needles," says Forbes Health. Japanese in origin ("rei," for universal, and "ki" for vital life-force energy), this specialized stress-reduction therapy has been used for centuries in cultures to reduce pain and restore balance to the body's natural systems by transferring energy through hands, according to the NIH's National Library of Medicine.
The International Association of Reiki Professionals explains that Reiki can reduce stress levels before and after surgery and may even reduce sensations of pain. In a 2017 randomized controlled trial, published in Holistic Nursing Practice, only Reiki showed significant reductions in pain, blood pressure, respiration rate, and state of anxiety.
One of the things that some may find particularly appealing about Reiki is that it "is completely noninvasive. During a reiki session, the practitioner places his or her hands gently on the client in specific positions in order to encourage the proper flow of the client's own ki or chi energy" (via International Association of Reiki Professionals). As Pamela Miles, a New York City–based Reiki master, told Everyday Health, "[Reiki] is a spiritual practice, like meditation is a spiritual practice."
Essential oils
Essential oils are plant extracts. Every part of the plant is used to produce the oils that we then inhale, massage into our skin (diluted in a carrier oil), or ingest. Because it takes so much of the plant to make an essential oil, it's a powerful botanical medicine," says Cleveland Clinic integrative medicine specialist Dr. Yufang Lin.
The therapeutic benefits of essential oils are numerous. This is where aromatherapy — a centuries-old holistic practice — comes into play, says Johns Hopkins Medicine. The oils are used in treating a wide range of conditions including nausea, insomnia, headaches, anxiety, and pain. Many of them, from lavender to rosemary to peppermint, have shown positive outcomes as pain relievers. In one example, a 2013 study demonstrated that children who underwent tonsillectomy procedures took less Tylenol during their recovery if they inhaled lavender essential oil.
Since the Food and Drug Administration doesn't regulate essential oils, Healthline warns that it's important to do research to find reputable brands because a product's purity and authenticity can vary widely between manufacturers.
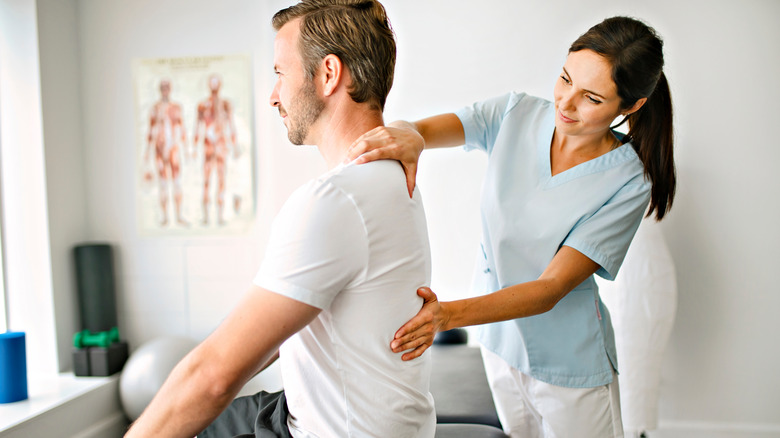
Physical therapy
Physical therapists work with patients to help them regain range of motion and manage their pain. They do this by evaluating soft tissue, joint mobility, and strength, then developing a treatment plan of hands-on techniques that may include exercises, electrical stimulation, ultrasound, and more, notes Verywell Health.
After you have surgery, you may be referred by your doctor to a rehabilitation center, where you'll be assigned a team of specialists who will help you heal and regain full functionality, according to WebMD. A physical therapist will be part of that team. These healthcare professionals are licensed by the state and hold a master's or a clinical doctorate degree.
"Many people worry that physical therapy may cause them more pain. However, physical therapy actually increases muscle strength and joint function which helps alleviate pain over time," says Southwoods Health in Ohio. "This can make your recovery time shorter and decrease the need for pain medication."
Hypnosis
Hypnosis has been used for a long time and for lots of things, including pain management, says the American Psychological Association. But despite the proof that it really can work for some people, it still gets a bad rap. After all, none of us wants to be the poor sap who stands up in front of an audience and quacks like a duck, right?
"Hypnosis is the oldest Western form of psychotherapy, but it's been tarred with the brush of dangling watches and purple capes," says Dr. David Spiegel, Stanford professor and associate chair of psychiatry and behavioral sciences, to Stanford Medicine. "In fact, it's a very powerful means of changing the way we use our minds to control perception and our bodies." In a study that he led, researchers looked at scans from 57 subjects and discovered that neural changes in the brain occurred in hypnotized subjects.
For pain management, hypnotherapy has been proven successful. This is no surprise to psychiatrists, The Washington Post reports, because they know that pain perception originates in the brain. In a therapeutic setting, and with verbal cues and repetition, a trained therapist can guide their patients to a "focused state of concentration" that makes them more receptive to suggestion. So if the goal of the patient is to minimize pain and anxiety, a therapist can guide them to those goals while they're in that heightened state of attention.
Staying ahead of the pain
Staying ahead of your pain — meaning you don't wait until it's severe to take your next dose of medicine — is vitally important after any surgery so it doesn't get out of control. If you try to tough it out and delay taking your medication, you may end up needing stronger painkillers or more frequent doses of prescribed drugs just to maintain adequate relief. "Postoperative pain is not just annoying or unpleasant," warns the American Society of Anesthesiologists. "If it's not treated correctly, it can sometimes become chronic pain — pain that lasts longer than three months — and become more challenging to manage."
Take your medications on time at the intervals you've been advised, get plenty of restorative sleep, and keep your body reasonably active to help reduce inflammation and accelerate healing, advises AARP. By doing all these things, WebMD says, you'll actually speed up your recovery and even feel less stressed.