Warning Signs From Your Tongue You Shouldn't Ignore
You may not know this, but your tongue is one of your strongest muscles (via WebMD). Your tongue enables those necessary acts of chewing, swallowing, talking, and tasting. It also makes it possible for you to blow bubblegum (via The Kid Bucket List). Okay, so maybe this isn't essential. But, like whistling, it involves a specific manipulation of the tongue (via Healthline).
So, your tongue is absolutely involved in sustaining life, and in many ways joyfully so. Think: whistling, blowing bubblegum, and slurping up a delicious bowl of noodles. But how often do you really think about your tongue, unless you've bitten it, or burned it on a hot cup of cocoa? You won't typically notice the feeling of your tongue unless it is highly stimulated (via BrainFacts.org). So if it's looking or feeling a bit odd, that muscle in your mouth can be telling you something about your health (via Glossitis).
A burning sensation
Have you ever felt a burning or prickling sensation on your tongue without apparent reason? Burning Mouth Syndrome (BMS) is a chronic condition that may cause various parts of your mouth (including your tongue) to feel the burn (via the Mayo Clinic). BMS may include dry mouth, a bitter or metallic taste, stinging, tingling or numbness in the mouth, and/or a burning sensation on the tongue. It can occur suddenly or come on gradually. It may also be a symptom of perimenopause or post-menopause.
When BMS occurs without any obvious underlying cause, it is known as Primary Burning Mouth Syndrome. Some research suggests it may be related to sensory and peripheral nerve dysfunction, according to a 2018 review in Pain. Secondary BMS, on the other hand, can be caused by underlying medical conditions. These include xerostomia (dry mouth), fungal conditions in the mouth such as oral thrush, a number of vitamin deficiencies, food allergies, acid reflux, thyroid disorders, anxiety and depression, and certain medications such as high blood pressure drugs (per the Mayo Clinic). Working closely with your healthcare practitioner and making lifestyle changes (such as avoiding problematic foods) may help reduce the severity of symptoms.
Swollen tongue
A swollen tongue, clinically known as glossitis, can be benign and temporary, albeit uncomfortable and painful (via a Glossitis). It may be a result of burning the tongue, food irritants, or direct trauma. But a swollen tongue may also be a sign of an underlying condition such as anemia, a protein or vitamin B deficiency, or a viral or bacterial infection. By properly treating such deficiencies or infections, the swelling will be relieved once the condition is resolved.
To evaluate potential causes for the inflammation, an overall medical nutritional screening will be necessitated. Additionally, the doctor may evaluate potential of cause from certain medications. During a physical evaluation of the tongue, the doctor will note its texture (rough or smooth), whether it looks shiny and/or dry, and determine whether there are any lesions. In some cases, blood tests and biopsies may be performed. Most cases of glossitis are harmless and will resolve without treatment. Proper oral hygiene is always important. The use of mouthwashes may help soothe the condition.
Glossy tongue (atrophic glossitis)
Glossy tongue (a.k.a atrophic glossitis) occurs when your tongue has lost some of its papillae — the little bumps where your taste buds live (via Healthline). This alters the tongue's texture, smoothening out its normally bumpy surface. Lacking sufficient papillae affects one's ability to properly taste. Additionally, this condition may also cause pain, burning, and numbness. These may be more annoying than serious, but a glossy tongue may also be telling of an underlying digestive ailment.
A glossy tongue has been associated with nutritional deficiencies due to poor diet or malabsorption issues, according to a 2016 review in The Open Dentistry Journal. Problems associated with atrophic glossitis include deficiencies in riboflavin, folic acid, niacin, iron, cobalamin, and zinc. Celiac disease is a prime contributor to compromised absorption of those nutrients. In fact, gastrointestinal disease is one of the most common causes of malabsorption associated with the development of atrophic glossitis. Other potential underlying conditions include infections such H. pylori and candidiasis, and lack of sufficient saliva production (via Healthline).
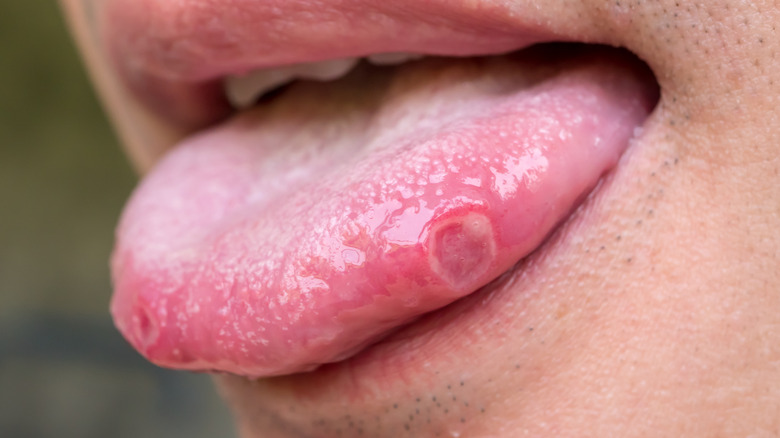
Canker sores on the tongue
Canker sores are a common type of mouth ulcer (via WebMD). Many people will get them at some point. Although associated with hormonal changes and allergies, flare-ups and exacerbations can also be exacerbated during times of stress (via Pioneer Dental). Besides appearing along the inner cheeks or at the base of your gums, they can also be found under the tongue.
The good news is that canker sores are not contagious, nor are they harmful. Soreness from the ulcer may be alleviated by over-the-counter oral medications for numbing. Milk of magnesia may help them heal faster. To help prevent irritation, you may want to avoid spicy foods while you have a canker sore. In most cases, they will heal within a week or two (via Mayo Clinic). If they persist for more several weeks, get larger, or you develop a fever and/or extreme pain, you should contact your health professional. Canker sores may also be a result of more extreme health conditions such as Celiac disease, inflammatory bowel disease, and immunosuppressive HIV.
Partial loss of taste
The taste buds carry signals to the brain to detect specific tastes such as bitter, salty, sour, sweet, and umami (via Nemours KidsHealth and Colgate). So, if you are missing or have damage to any taste buds, you may experience a partial loss of taste.
Your taste buds are located in the tiny bumps on your tongue known as papillae, and like many cells in your body, your taste bud cells are frequently renewed. On average, each person has 10,000 taste buds that get replaced every couple of weeks (via KidsHealth). However, as a person ages, the level of replacement is reduced. Thus, the intensity of certain tastes may be diminished as you get older. In fact, an older person may have only half as many working tastebuds. Additionally, factors such as smoking, sickness, or medication can cause damage to the taste buds, diminishing the ability to fully experience specific flavors (per Colgate).
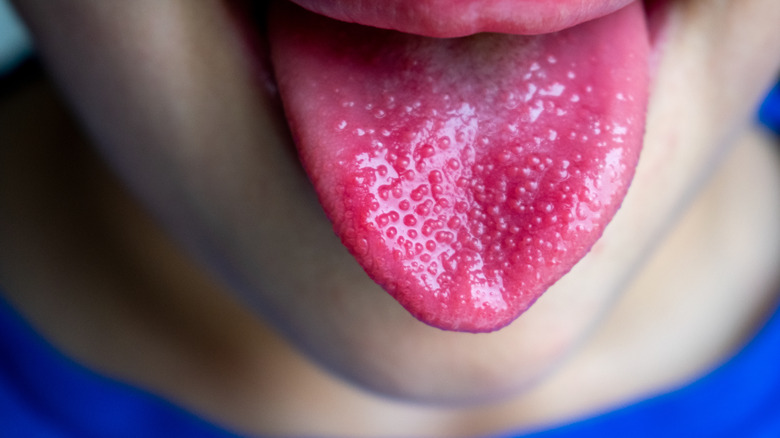
Strawberry tongue
Strawberry tongue typically appears red and swollen — resembling a strawberry's plump, seeded texture, as the condition's name would suggest (via WebMD). It can be a symptom of various conditions. Some causes of this lingual manifestation may include childhood inflammatory diseases such as Kawasaki syndrome. It may accompany high fever, sore throat, and headaches, which can result from bacterial infections associated with scarlet fever (typically affecting children between the ages of 5 and 15) or the rare but serious toxic shock syndrome, which is commonly linked to improper tampon usage. It may also be a result of food or drug allergies, which can affect anyone.
There may be more benign causes, however. A vitamin B12 deficiency may cause a strawberry tongue (via Medical News Today). Fortunately, if that is the case, treating the deficiency through dietary changes or a vitamin injection (if necessary) can resolve the problem. Regardless, a medical professional should evaluate to determine if there is a more serious underlying issue. In either case, a swollen, bumpy tongue can make eating and swallowing more difficult. It also makes it easier to bite the tongue.
Hairy tongue
While it may sound monstrous, a black hairy tongue is actually a benign condition (via Mayo Clinic). The build-up of dead skin cells on larger-than-normal papillae results in trapped bacteria, which can appear dark and furry on the tongue. The condition may be unsightly, but the good news is that it is does not cause pain. However, it may be accompanied by a metallic taste, bad breath, or even cause a gagging sensation.
And if you suffer from chronic acid reflux, you may be more likely to develop this fur on your tongue. According to a 2020 study in Medicine, GERD sufferers had more hairy patches on their tongue than those without the GI disorder. In fact, the thickness of fur (as well as salivary increases) was greater in those with GERD. Thus, the authors suggest that incidence and degree of a hairy tongue might predict risk and / or severity of GERD. Though, further studies are necessary.
Common home remedies for hairy tongue include exercising proper oral hygiene — brushing after eating, and flossing at least once a day — and brushing the tongue (via the Mayo Clinic). Regular dental visits are important. And a healthy, balanced diet is always recommended.
Enlarged papillae
Inflammation on the tongue may result in enlarged papillae, those tiny bumps that house your taste buds (via WebMD). When a group of papillae becomes enlarged, it results as one irritated and uncomfortable bump on the tongue. This can be caused by something as simple as biting your tongue (via Sherwood Park Dental). Other causes include viruses, bacterial or fungal infections, herpes, and autoimmune disorders. Geographic tongue, where the tongue's cells exfoliate inconsistently (leaving a non-uniform appearance), may also be a culprit. Regardless, you may notice it visibly, and it may feel a bit odd.
Unless the bumps persist for over 10 days, seeking medical treatment is generally not necessary. Rinsing with salt water, drinking plenty of water, and brushing twice daily (including your tongue), can help reduce the inflammation. Preventative care includes routine oral hygiene, eating and chewing with care, and wearing a mouthguard during activities where you may be at risk of biting your tongue. Refraining from smoking and decreasing stress are also key to preventing tongue injury.
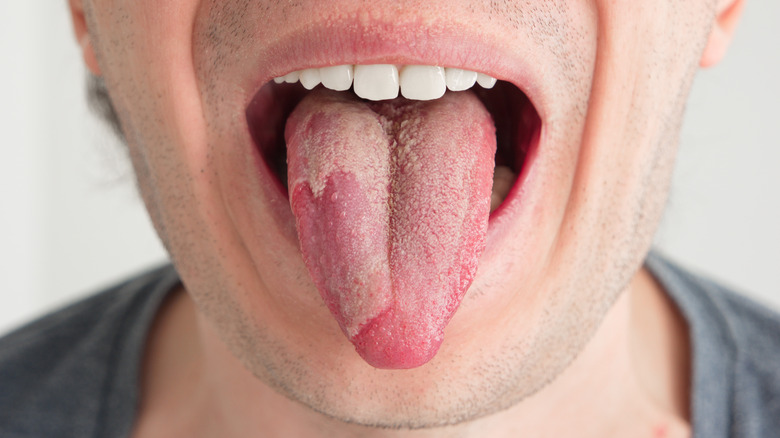
White patches (oral thrush)
Oral thrush, which may be identified by white patches on the tongue, is a fungal infection (via NHS Inform). But you'll want to be careful wiping that creamy white film off because that may lead to slight bleeding. Since this infection is caused by the Candida yeast, it is thus also known as Candidiasis. This infection may leave an unpleasant taste in the mouth, and make it more difficult to eat and drink due to redness, soreness, and burning in the oral cavity (via the Mayo Clinic).
It may not be surprising that poor dental hygiene may contribute to an oral infection such as this. But oral thrush is more likely to occur in those with reduced immunity, such as babies and the elderly. Some health conditions and medications may also make someone more prone to oral thrush. It may also be a symptom of dry mouth, long-term high-dose antibiotic usage, or a side effect of chemo or radiation therapy (via NHS Inform). Medical conditions that may lead to this infection include iron or vitamin B deficiencies, hypothyroidism, and HIV. Treatment includes antifungal medications including gels, creams, and oral tablets.
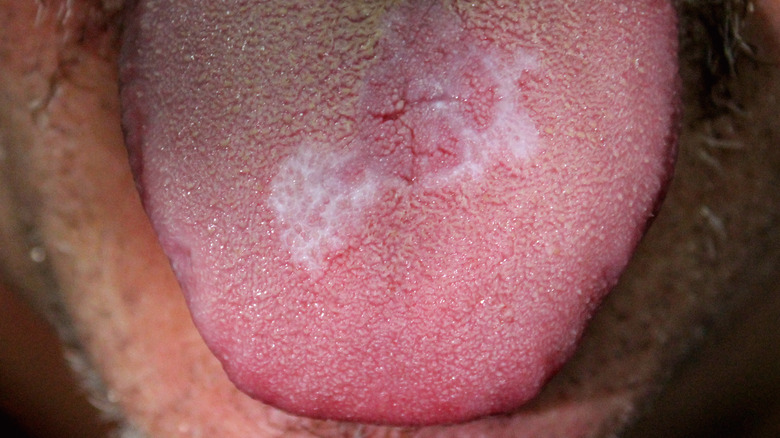
Lace-like appearance on tongue
If your tongue is sore and swollen with a lace-like appearance, you may have what is known as oral lichen planus. This non-contagious inflammatory disease may present with white patches, redness, and open sores on the tongue, cheeks, and gums (via the Mayo Clinic). And this condition will likely make one sensitive to hot, spicy, and acidic foods. Additionally, it can make talking, chewing, and swallowing a challenge. In rare cases, it may cause an esophageal stricture. Though oral lichen is a more common condition in people over 40, anyone can get this disease (via WebMD).
There is little known regarding the specific cause(s) of oral lichen planus. However, doctors suspect the following may contribute to it: family history, autoimmune disorders, and hepatitis C. Triggers include high blood pressure drugs or diabetes medications, an adverse reaction to dental fillings, food allergies, and oral injury such as biting tongue or cheeks. While there is no cure, topical numbing agents may be applied to affected areas, and corticosteroids may help reduce swelling (via Mayo Clinic). Immune-suppressing medications may be required for in more severe cases.
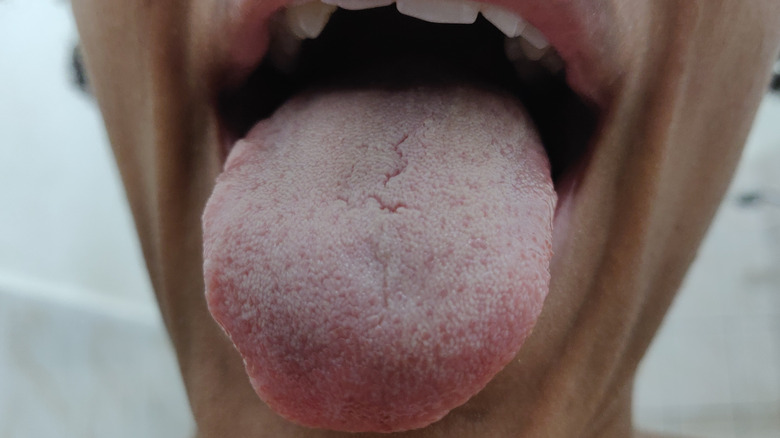
Geographic tongue
Geographic tongue (aka migratory glossitis) is a benign inflammatory condition where lesions change in size and shape and migrate across the top of tongue, according to a 2021 review Canadian Medical Association Journal (CMAJ). It generally has few (if any) symptoms, but may present with soreness or burning, according to the National Organization for Rare Disorders (NORD). Pattern changes and distribution of the lesions may occur daily.
Geographic tongue is estimated to affect 1-5% percent of individuals, and is more common to individuals under 30 years of age (via CMAJ). Though topical steroids or anesthetics may help with any burning that may occur, this condition may resolve spontaneously without or without treatment. That being said, geographic tongue may be associated with psoriasis, allergies, and anxiety, according to a 2018 review in Revista Clínica Española. It may also accompany juvenile diabetes, Reiter's syndrome, and hormonal dysfunction (via NORD).
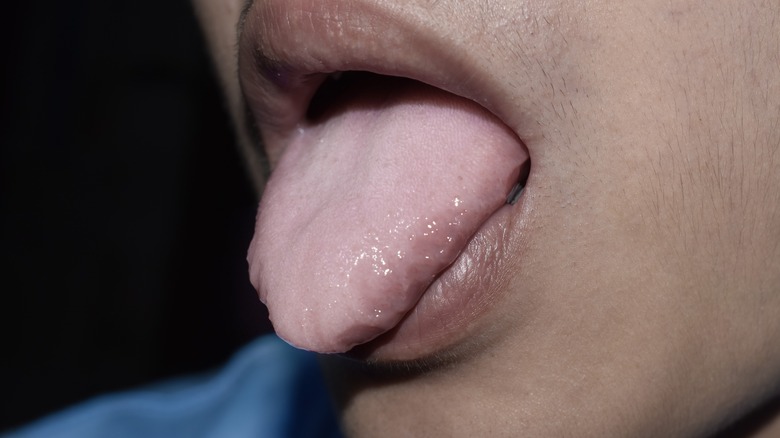
White tongue
If your tongue is white, it may be a sign of dehydration (via Mayo Clinic). Your tongue might simply be telling you to cut back on alcohol or to drink more water. It may also be telling you something about your stress levels. When individuals are anxious, they are more apt to breathe through their mouths — exhibiting abnormally rapid and shallow breathing (via Healthline). This mouth-breathing can also cause a tongue to turn white (via Mayo Clinic).
Scientifically speaking, white tongue is the result of an overgrowth and inflammation of papillae on the tongue. This can appear as a white film or white hairy appearance. The buildup may happen over time, or be a result of an infection or indicate a specific condition (via Cleveland Clinic). Conditions associated with the appearance of white coating on the tongue include oral thrush, geographic tongue, and oral lichen planus with its lace-like appearance (via Mayo Clinic).
Diagnosis for tongue issues
When your tongue feels odd, is in pain, and/or looks a bit abnormal, you may want to start with your dentist for an evaluation. A dentist can determine if their scope of practice is suitable for your oral needs or refer you to a specialist if necessary (via MedicineNet). In those who can't move their tongue normally, an ENT (ear, nose, and throat) specialist or otolaryngologist may be required (via ENT Health).
Certain types of growths on the tongue may need to be biopsied to fully diagnose and direct the best treatment (via MedicineNet). A dentist may evaluate any tongue abnormalities to rule out any cancer (via Brookside Dental). That said, the incidence of tongue cancer is rare, representing just under 1% of newly diagnosed cancers (via National Cancer Institute). Even unsightly bumps may be benign (via MedicineNet). They may result from direct trauma to the tongue, such as irritation from chronic biting.
Home remedies for a sore tongue
Your tongue can be highly sensitive (via Medical News Today). Whether your tongue experienced direct trauma such as a hard bite, or you feel a canker sore coming on, you can rely on some simple home remedies to ease your pain.
Always exercise good oral hygiene, as keeping your mouth clean with aid in healing. Rinsing with salt water can help to clean a wound and reduce the risk of infection; and sucking on ice can help soothe the pain. Additional ways to soothe a sore tongue include the use of chamomile tea and sage. A person can simply steep a chamomile tea bag and press it on the inflamed area (it must be cooled, of course). Cooled, boiled sage leaves is an herbal remedy to reduce inflammation and help heal those pesky canker sores. Avoiding hot and spicy foods can prevent further irritation (via Healthline). And over-the-counter pain medications may help. But keep in mind, if your tongue issue is severe and doesn't resolve within several days, it is important seek medical attention for proper evaluation and treatment.