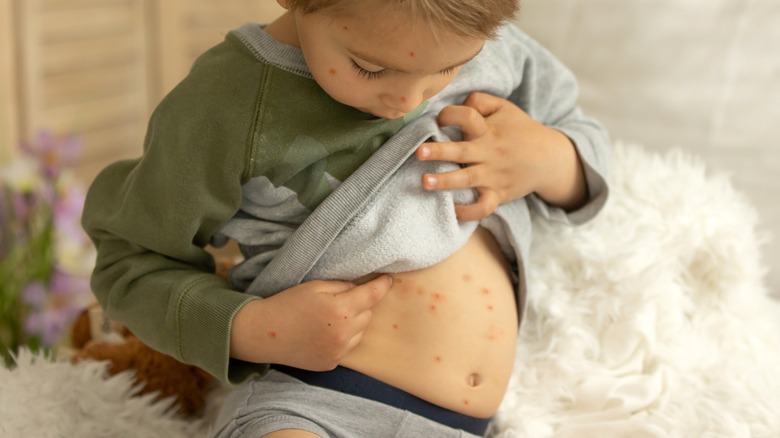
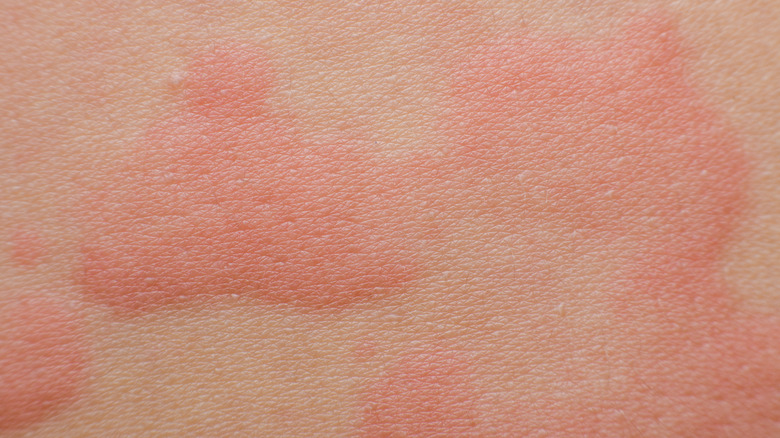
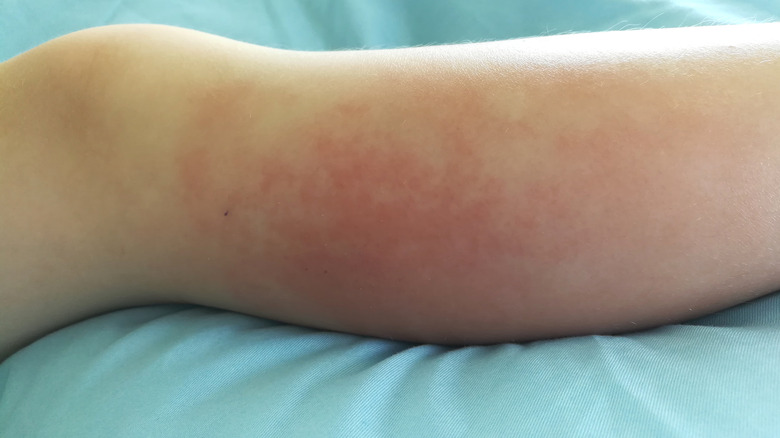
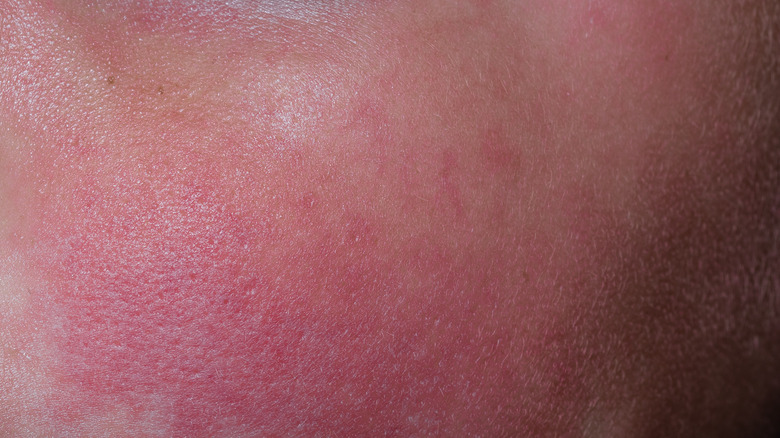
Types Of Skin Rashes Explained
Everyone strives for clear, beautiful skin. So it's no wonder that entire industries are devoted to helping solve skin issues, given the American Academy of Dermatology Association (AAD) reports that more than 25% of the population has some form of skin issue. While zits and wrinkles generally occur at specific stages of life, rashes know no bounds.
MedicineNet defines a rash as "a change in the color and texture of skin that usually causes an outbreak of red patches or bumps on the skin." Rashes usually start in one area of your body, and the inflammation can spread from there. Resulting from a variety of health issues or exposure to an irritant, rashes often feel itchy and look red and swollen. While difficult, it's best to try and not scratch or pick at the affected area.
Rashes are a part of life. It's likely that you've already had at least one and will have several more in your lifetime. Home remedies and over-the-counter medications can help diminish the side effects (via WebMD). However, if your rash doesn't clear up quickly, it's best to have these anomalies diagnosed and treated by a medical professional.
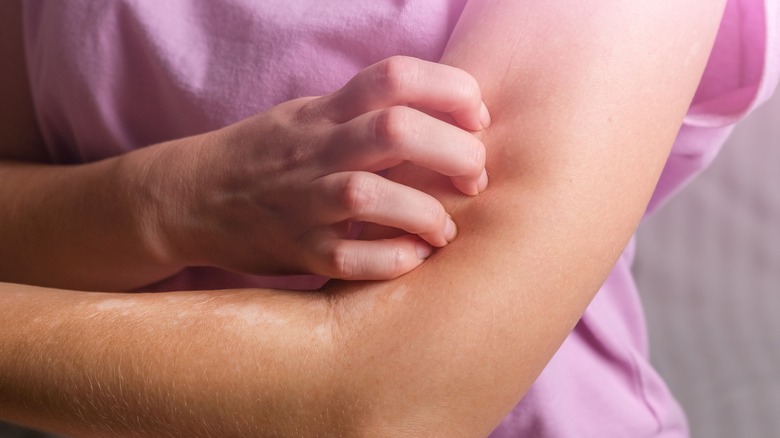
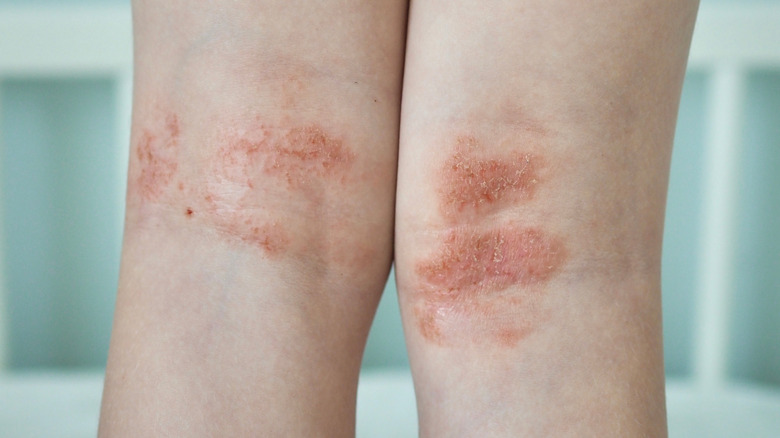
Eczema
One of the most common rashes results from an immune trigger. Also referred to as atopic dermatitis, eczema causes irritation mostly in areas where skin rubs against itself, including behind your knees and elbows (via National Eczema Association). People suffering from eczema report dry, itchy skin with bumps that leak when scratched. Scratching also causes swelling, thickening, and infections in some patients.
Eczema is not contagious, and symptoms appear periodically resulting from exposure to one or more of the many known triggers (via Mayo Clinic). Unfortunately, many patients are unaware of what makes their eczema flare. Some of the more common substances that instigate an eczema flare-up include additives in soaps, washes, and cleaners, as well as prolonged exposure to extreme temperatures, nickel, and wool (via National Eczema Association). Food allergies and stress can also cause eczema to flare. And as if itching and oozing weren't enough, because eczema is an immune response, it often comes with additional health issues. Diagnoses of hay fever and asthma often accompany eczema.
While most commonly diagnosed in childhood, this chronic condition affects people of all ages, especially if there is a history of eczema in the family. Symptoms often diminish with age. However, it is best to avoid known triggers.
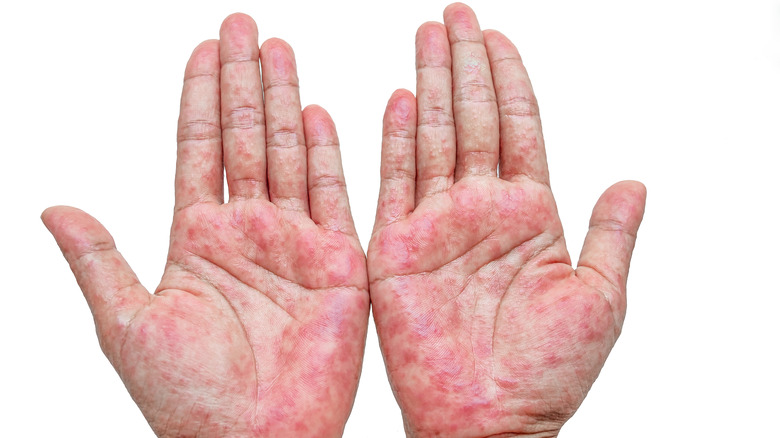
Contact dermatitis
Red, raw skin that burns or is itchy may result from contact dermatitis (via Cleveland Clinic). This common skin rash results from a reaction to an allergen and is not chronic or contagious. Because contact dermatitis usually appears in the areas directly exposed to the allergen, it's most commonly found on your hands. Your skin turns red at the point of contact, making it appear blotchy.
According to Mount Sinai, there are two types of contact dermatitis: allergic contact dermatitis and irritant contact dermatitis. Both result from exposure to chemical irritants including pesticides, preservatives, and rubber or latex, as well as nickel, certain plants, and dyes. Allergic contact dermatitis develops over time. Therefore, multiple exposures are required before a reaction occurs. In fact, you could use a product consistently for years before a rash develops. On the other hand, irritant contact dermatitis occurs soon after exposure to the problem substance. Therefore, regardless of the type of contact dermatitis you're diagnosed with, once a culprit is determined, it's best to avoid exposure.
Contact dermatitis may appear similar to the skin's reaction to more extreme allergic reactions that result in anaphylaxis. However, the most common complication of contact dermatitis is infection from scratching the affected areas — though more serious reactions are possible.
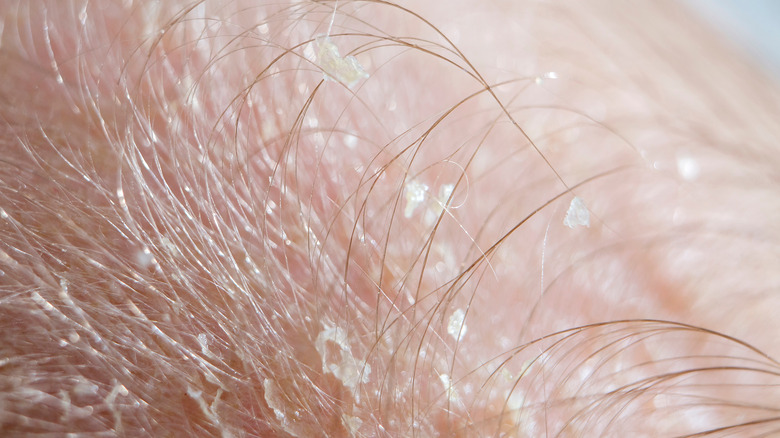
Seborrheic dermatitis
Another prevalent, noncontagious rash is seborrheic dermatitis (via Mayo Clinic). This skin issue affects over 10% of the population and is less itchy than its cousins, atopic and contact dermatitis. Seborrheic dermatitis most often appears on the scalp. In babies, this rash is referred to as cradle cap. Cradle cap will clear up on its own in a few months, and most children show no signs by their first birthday. Adults with this skin issue often present with greasy hair and bad dandruff.
The more oily your skin, the more likely you are to suffer with seborrheic dermatitis (via Cleveland Clinic). Other factors that increase the possibility that you'll have seborrheic dermatitis include family history, an overgrowth of the skin yeast Malassezia, and an increase in androgen hormones. Environmental factors also play a role in seborrheic dermatitis flare-ups. The condition is often worse in the dryer winter months. Summertime may lead to fewer flare-ups as the sun's rays help to kill off the excess skin yeast.
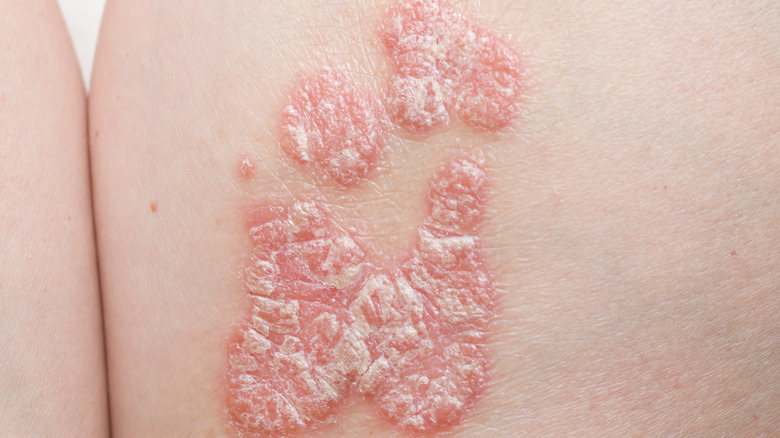
Psoriasis
Like eczema, psoriasis is an autoimmune condition that results from your immune system attacking healthy cells (via Healthline). In this case, your white blood cells (aka T cells) assault your skin cells. The result is that your skin growth cycle speeds up, and your body is producing new skin cells faster than the old ones shed, leading to buildup. Those with psoriasis have itchy, red, inflamed skin covered in silvery-white scales. According to the National Psoriasis Foundation, about 3% of American adults suffer from psoriasis.
There are five types of psoriasis; plaque, guttate, pustular, inverse, and erythrodermic (via AAD). Plaque psoriasis is the most common form of the disease and appears mainly around your joints and on your scalp. Those with severe plaque psoriasis are at greater risk of having it affect their joints as psoriatic arthritis. Often diagnosed in childhood, guttate psoriasis is found on your gut, arms, and legs. As its name implies, pustular psoriasis involves blisters, mainly on your hands and feet, that ooze liquid. If you have psoriasis in areas where skin rubs against skin, it's most likely inverse psoriasis. The least common and most serious form of psoriasis is erythrodermic. Erythrodermic psoriasis forms on a large portion of your body and makes you look sunburned. Regardless of the kind, genetics is the most significant factor in developing psoriasis (per Healthline).
Rosacea
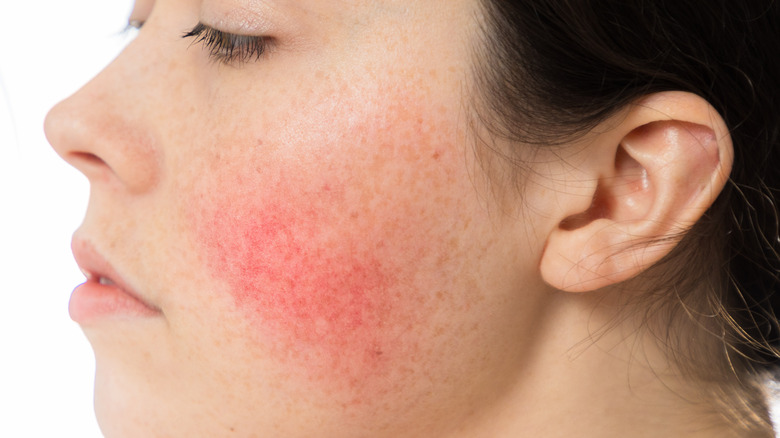
During your 30s, a number of skin issues can begin to appear due to stress and hormonal factors, according to Byrdie. These include breakouts (including of cystic acne), dark spots, and fine lines. And unfortunately, according to the Cleveland Clinic, it's also the time that your chances of being diagnosed with rosacea are at their highest, especially if you're fair-skinned.
According to the National Institutes of Health, rosacea "is a long-term inflammatory skin condition that causes reddened skin and a rash, usually on the nose and cheeks. It may also cause eye problems." This rash comes and goes. Sun exposure and stress tend to exacerbate symptoms, as do heat, sweat, and alcohol intake. Some of the first signs of this rash are known as prerosacea (via Johns Hopkins Medicine). Your face may look like you are constantly blushing. Often, for women especially, this malady then turns into vascular rosacea, in which blood vessels in your face swell and your face feels warm.
Men diagnosed with rosacea most often have rhinophyma, which causes their noses to change shape and get larger, and their oil glands to grow. Another form of this affliction is inflammatory rosacea. You get what looks like zits and, like vascular rosacea, this rash includes enlarged blood vessels. Due to the rash's proximity to the eye, those with rosacea often also complain of eye irritation, with symptoms such as redness, burning, and eyelids that are inflamed.
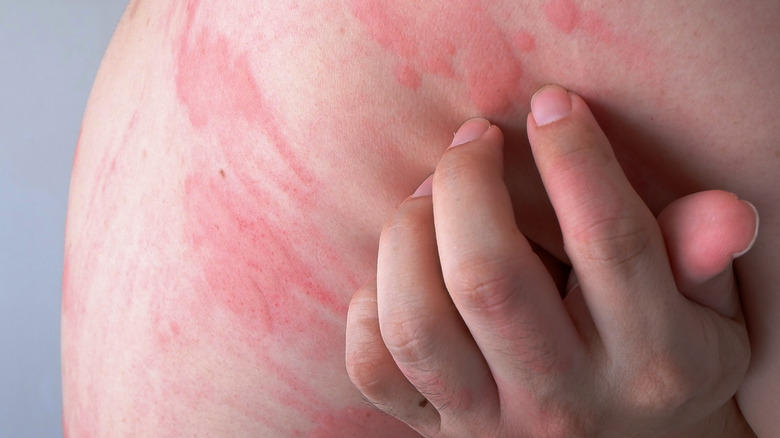
Hives
Doctors refer to hives as urticaria, while others call them welts (via the American College of Allergy, Asthma, and Immunology, ACAAI). Like contact dermatitis, hives are most commonly attributed to an allergic reaction to a foreign substance. In many cases, hives result from the body's production of histamine, a protein designed to fight against exposure to allergens (via Medical News Today). However, hives can also result from things like stress, pressure or scratching on the skin, exposure to extreme temperatures, or another health issue such as a virus or infection.
Hives are itchy, red bumps that turn white in the middle when touched. While medical professionals will tell you that itching can lead to infection, the real fear with hives is that they may not be your only symptom. Both angioedema and anaphylaxis are associated with hives, and both require medical treatment (via ACAAI). Angioedema occurs when the tissue under your skin swells. It can look like hives, or come with hives. Therefore, if you develop hives, it's important to watch for more symptoms. Swelling in and around your mouth, increased heart rate, clammy skin, and feeling faint are all signs of a severe allergic reaction known as anaphylaxis.
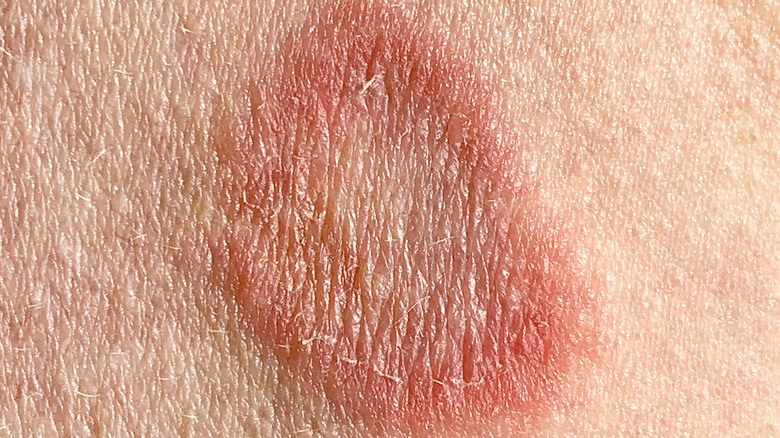
Ringworm
Contrary to what the name implies, worms have nothing to do with ringworm. Instead, this extremely infectious rash gets its name from the round shape it takes on your skin. Medically referred to as "tinea" or "dermatophytosis," ringworm can appear almost anywhere on your body, according to the Centers for Disease Control and Prevention (CDC). The most common forms of ringworm are athlete's foot and jock itch (via Cleveland Clinic). However, ringworm can also affect your scalp, beard, and nails.
There are several ways people get infected with ringworm. The most common is through contact with people or animals who already have the rash (via New York State Department of Health). This contact could be direct, or you could get it from touching an area that an afflicted person recently handled.
Symptoms vary depending on what body part is affected. According to the New York State Department of Health, "Ringworm of the scalp usually begins as a small pimple which becomes larger in size and leaves scaly patches of temporary baldness. Infected hairs become brittle and break off easily. Occasionally, yellowish cuplike crusty areas are seen." You'll know if you get jock itch by the itchy, red spots around your groin area. Athlete's foot not only makes your feet and toes itchy, but it might also cause them to peel and smell. When ringworm affects your nails, they thicken, fade, and eventually disintegrate.
To reduce your chances of infection, the CDC recommends that you wear shoes in the locker room and wash your hands often, especially after playing with animals. If you have ringworm, don't share personal items.
Chickenpox and shingles
While caused by the same virus, chickenpox and shingles are two different rashes. Both illnesses result from exposure to varicella-zoster, a highly contagious herpes virus (via Missouri Department of Health & Senior Services). You cannot get shingles without first having chickenpox at some point in your life.
Chickenpox and shingles appear as itchy blisters that scab over within a few days. For the most part, chickenpox is a childhood disease. It begins with a fever, headache, and lethargy. Blisters appear a few days later and disappear within a week or so. You get chickenpox either by direct contact with the rash or by breathing in airborne virus particles that escape when the blisters pop. The time from exposure to infection takes about ten days. The virus remains in your body after recovery. Shingles is the reawakening of the virus that causes chickenpox, typically later in life (via the Association for Professionals in Infection Control and Epidemiology). Shingles mainly affect older individuals, and is more painful and lasts much longer than chickenpox.
Vaccines are available for both rashes. The chickenpox vaccine is offered during childhood, though those over the age of 13 who have never had the disease can still get vaccinated (via CDC). The shingles vaccine is recommended for those age 50 and over, or to adults who are immunocompromised (via CDC).
Rashes related to drug allergies
When your doctor prescribes a new medication, they often tell you what side effects have been prevalent in other patients. One possible reaction is a rash. NYU Langone Health explains that this symptom is caused by "drug hypersensitivity" — basically, that your body is overreacting to your medication, and this overreaction results in your skin showing signs of disapproval.
There are a few types of drug-induced skin rashes. The most common type of drug-induced rash is called exanthematous, in which red flat spots appear on your skin (via Healthline). Exanthematous reactions generally don't occur until around ten days after the first dose. If you notice swelling accompanies your rash, it could be eosinophilia. Though it looks similar to an exanthematous rash, this type of rash also elevates white blood cells and often causes a fever, as well. These symptoms take at least two weeks to appear. And as mentioned above, hives are another common reaction to drug hypersensitivity.
Itchy, red, scaly skin all over your body that is hot to the touch and accompanied by a fever a few days after starting a new drug could be erythroderma. This type of reaction is more prevalent in those with other skin conditions, including psoriasis and atopic dermatitis. Erythroderma is a serious condition that can be fatal, so if you experience these symptoms, you should seek treatment immediately. In addition, Stevens-Johnson syndrome is another serious drug-related rash. Those with this condition suffer with body-covering blisters. Without proper medical intervention, an infection can develop and spread. Another side effect of Stevens-Johnsons is conjunctivitis (pinkeye), in which tissue inside your eyelid becomes irritated and inflamed.
Cellulitis
All of us have bacteria that live on our skin, and typically they don't cause any problems. But if these bacteria get into the body, it can lead to an internal infection known as cellulitis. Medical News Today defines cellulitis as "a bacterial infection in the deeper layers of skin and the fat and soft tissue underneath."
Cellulitis occurs when staph and strep bacteria enter the bloodstream, typically via some kind of wound that has left a vulnerable opening in the skin (per Cedars Sinai). When this happens, the area around the wound turns red and the infection quickly spreads. The severity of the infection depends on the strength of your immune system and how quickly treatment is administered. Mild cases clear up within a week or so with oral antibiotics. More severe cases could require hospitalization and medication administered through an IV.
Other medical conditions, including diabetes, other dermatological issues, and circulatory problems, increase your risk of developing cellulitis any time you create an opening in your skin (via Medical News Today).
Fifth disease
Before vaccines were prevalent, children were likely to develop five "viral rash diseases": measles, rubella, chicken pox, roseola, and erythema infectiosum (via Arthritis Foundation). This final one, also referred to as fifth disease, results from exposure to parvovirus B19.
Symptoms of fifth disease include a low-grade fever, flu-like symptoms, and a rash that begins on the face. This rash of pink and red lacy patches is very itchy and spreads to the affected person's midsection, arms, and legs. Symptoms typically develop within a week of exposure and last up to 10 days. Fifth disease is highly contagious and is spread through the liquid released when someone with the infection coughs or sneezes (via Nemours KidsHealth). However, many with fifth disease are unaware they have the illness because the signature rash doesn't develop until after they are no longer infectious.
Unlike the other viral rash diseases common to children, there is no vaccine against fifth disease. And preventing the spread of fifth disease is difficult because the primary symptom — rash — doesn't appear until after the contagious period has passed. However, generally it's a mild disease that passes without special treatment.
Impetigo
Impetigo is a bacterial infection caused by one of two types of bacteria: group A Streptococcus and Staphylococcus aureus (via CDC). It starts as itchy red facial sores that can spread to other body parts. Within a few days, these sores break open and leave behind a brownish yellow scab.
The rash associated with impetigo appears around ten days after coming into close contact with the infection (via Mayo Clinic). This contact might include touching the sores of an infected person, or touching things like linens or clothing that may have been used by the infected person. Therefore, the best ways to prevent the spread of the disease are to wash your hands frequently, cleanse sores or any open wounds with soap and water, cover open sores with a bandage, and take care to wash any personal items thoroughly (via CDC).
If you develop impetigo, keep scratching to a minimum and see a medical professional as soon as possible. The most common way for doctors to treat impetigo is using topical antibiotics that get rubbed directly into the affected skin areas (via Mayo Clinic).
Things to try at home for your rash
Beyond how it looks, the itch is the often worst part of having a rash. You probably know that scratching is a bad idea because it could cause the rash to spread and cause open sores to become infected (via Healthline). However, several remedies you can try at home help ease your comfort level and diminish a rash's effects.
One of the first things you can try is cold. Cold reduces swelling and inflammation. Try a cold compress, an ice pack, or even a cold shower. Whatever you decide, let it sit on your skin long enough for the itch — and in some cases, the heat — to subside. An oatmeal bath also soothes and helps treat itchy, sore skin. But don't bathe in your breakfast — instead, purchase colloidal oatmeal and add it to your bathwater. The oils from the oats have antioxidants that help repair skin. In addition, aloe, baking soda, and some plant oils, including coconut and tea tree, also help soothe angry skin.
If natural remedies aren't doing enough for you, head to the drug store and pick up hydrocortisone cream and a strong antihistamine like Benadryl. Use the cream twice a day to reduce itching.
Signs you should see a doctor for your rash
If you try over-the-counter and home remedies for your rash and nothing seems to help, that's a sign you need to see a medical professional (via Healthline). There are also some other symptoms that, if they accompany your rash, should have you seeing a doctor sooner rather than later. The most obvious is difficulty breathing or anaphylaxis, a severe allergic reaction. However, some other symptoms are also concerning. If a fever accompanies your rash, it could indicate an infection, because your body uses heat to kill off intruders (via AAD). In this case, an antibiotic might be necessary.
A rash that spreads quickly, appears suddenly, or is painful is also cause to seek medical attention. The same is true if the rash covers all or almost all of your body. And regardless of how good or bad a rash looks or feels, if you are uncomfortable, it's best to seek help before things get serious.