How Rheumatoid Arthritis Affects Different Parts Of The Body
It's interesting how some acronyms can take on new meanings depending on what's happening in our lives. Take RA, for example. For a college student living in the dorms, RA might mean resident assistant or resident advisor. But those same two letters stand for something entirely different for someone with a specific form of arthritis.
As the Centers for Disease Control and Prevention (CDC) explains, RA is the acronym commonly used for rheumatoid arthritis. When a person has this condition, their immune system goes after their cells the same way it would a virus or a dangerous form of bacteria. This leads to various areas of their body becoming inflamed, which can lead to a range of health issues. Although we are still learning about RA and haven't determined yet what specifically causes this health problem, risk factors that can increase one's chances of developing rheumatoid arthritis include smoking cigarettes, having certain genes, and being obese.
While RA usually happens to adults in their sixties, it's possible for someone to start developing RA at any point in their lives. And even though you shouldn't self-diagnose yourself or others, being aware of the possible ways that rheumatoid arthritis can affect the body might help you determine if you need to reach out to a healthcare professional. Here's what you need to know.
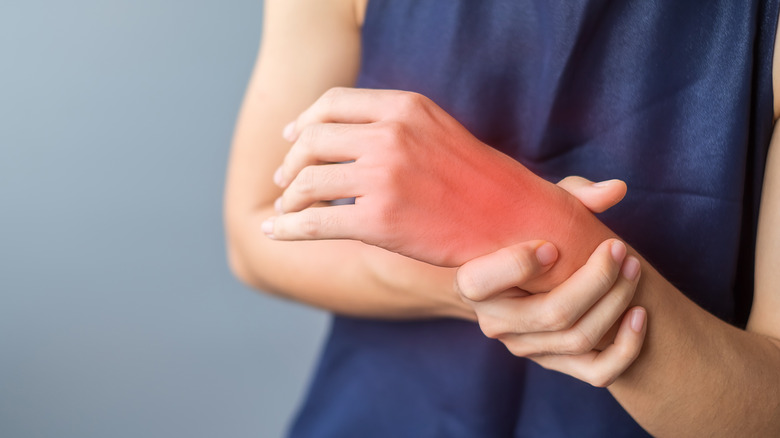
Joints
When most people think of rheumatoid arthritis (RA), the first thing that probably comes to mind is how it impacts the joints. As the Mayo Clinic explains, RA can impact the joint's lining, causing pain and inflammation.
But this doesn't mean that every joint in a RA patient's body is going to be impacted all at once. When a person is first developing RA, usually it's the small joints of the body (like the ones in the fingers and toes) that first become swollen, stiff, tender, and/or warm to the touch. But unfortunately, RA-related joint issues don't stop with the hands and feet. A rheumatoid arthritis patient can experience joint problems in other areas of their arm like their wrists and elbows, or even their shoulders. Other joints commonly impacted by RA include the hips, the knees, and the ankles. Generally the symptoms are symmetrical, meaning that an RA patient will likely experience the same symptoms on each side of the body.
Eyes
Although joint issues are common symptoms of rheumatoid arthritis, don't fall into the trap of thinking that RA can't significantly impact other areas of the body (via Arthritis Foundation). Case in point, collagen – a protein that is affected by RA– is found not only in the joints, but also in the eyes. In fact, Dr. Sunir J. Garg, retina physician and surgeon at Wills Eye Hospital in Philadelphia, told the Arthritis Foundation that the cornea and the white part of the eye (a.k.a. the sclera) are mainly made of collagen.
Now that we understand some of the biology involved, let's discuss what specific eye issues can go hand in hand with RA. According to the Arthritis Foundation, a patient with RA is very likely to experience Dry Eye Syndrome (or Keratitis Sicca), which causes your eyes to have an insufficient tear film, leading to symptoms like blurry vision and the sensation of dryness. Additionally, someone with RA can develop scleritis, where the white part of the eye becomes inflamed and thinner. And brace yourself: Dr. Garg told the Arthritis Foundation that for those with scleritis, "Minor trauma could cause that part of the eye to split open." Furthermore, NVISION Eye Centers caution that RA patients are more likely to develop glaucoma and cataracts.
Lungs
Let's face it, our lungs are especially crucial to our lives. Take away a someone's oxygen, and that person will die within minutes (via SpinalCord.com). Healthy, well-functioning lungs are extremely important, and unfortunately, rheumatoid arthritis can negatively impact these organs.
According to CreakyJoints, RA can cause inflammation in the lungs. And make no mistake, this can be very problematic. Inflamed lung tissue (especially inflammation that is chronic) can become scarred and less flexible, making it more difficult for someone to breathe and sometimes causing issues like dry cough and fatigue. Besides scarring, RA can cause bumps called nodules to develop in the lungs. And if one of these bumps breaks, a person could find themselves with a collapsed lung. An RA patient can also experience fluid building up in the chest, which can also result in a collapsed lung, although it might only cause shortness of breath, coughing, and discomfort.
In addition, someone with RA might be at higher risk of developing severe chronic obstructive pulmonary disease or COPD. Having rheumatoid arthritis also means you're at a higher risk for developing an infection like pneumonia. This is both because having RA negatively affects your immune response and because some RA medications suppress the immune system, meaning your body is less able to fend off viral or bacterial invaders.
Heart
Since rheumatoid arthritis often impacts the joints, it's perhaps not a surprise that it can do harm to the muscles that buttress the joints (via Verywell Health). But remember, an extremely important muscle in your body — your heart — isn't directly connected to a joint. That doesn't mean, however, that RA can't harm it.
As rheumatologist Dr. Konstantinos Loupasakis told CreakyJoints, high amounts of inflammation (like the kind caused by RA) can lead to more fat accumulating on the walls of the arteries. This, in turn, can make it harder for blood to flow throughout the body and be bad for the heart. Also, some over-the-counter medications taken for RA-related pain can up the chances of developing blood clots and experiencing heart failure. What's more, corticosteroids, a type of medication taken for arthritis, can also increase the chances of developing cardiovascular problems, since corticosteroids can interfere with how your body uses insulin, as well as increase "bad" cholesterol.
Speaking of cholesterol, if you have RA and your healthcare professional finds your "bad" cholesterol is low, that doesn't guarantee you have low cholesterol. Known as the "lipid paradox," this is an inaccurate test result that can happen for RA patients. The exact reasons for this false reading aren't known at this time, although cardiologist Dr. Martha Gulati told CreakyJoints that it might be that the particles measured in a standard cholesterol test are physically different in RA patients. And, of course, "bad" cholesterol can be detrimental to one's heart.
Mouth
If you have rheumatoid arthritis, then you're more likely to develop an autoimmune disorder known as Sjogren's syndrome, which can cause dry mouth (via Arthritis Foundation). Dry mouth, in turn, can lead to a host of other health problems. Now, let's be clear: Everyone's mouth feels dry from time to time. But chronic dry mouth, or xerostomia, is more than just feeling a momentary dry sensation. Xerostomia patients cannot produce the right amount of saliva, which can interfere with both swallowing and talking. Chronic dry mouth can also cause cracks in both the lips and the skin near the lips.
While dry mouth might seem like more of a nuisance than a real concern, ignoring it and trying to cope by using gum and lip balm rather than speaking with a healthcare professional is a bad idea. As the Arthritis Foundation explains, dry mouth can increase the chances of developing gum disease and tooth decay. And having less saliva makes it harder for your body to break down what you eat and drink. Additionally, Sjogren's syndrome can also negatively impact one's eyes, skin, kidneys, lungs, and joints.
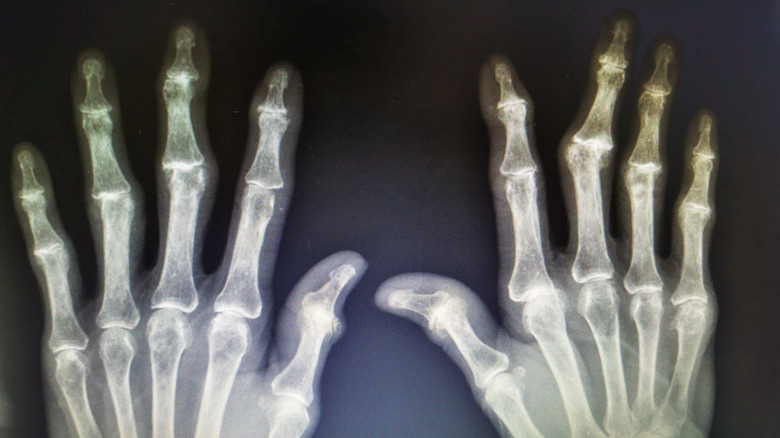
Bones
If rheumatoid arthritis affects the joints, it stands to reason that it can affect bones. As a matter of fact, there's a domino effect that happens because of RA that can have a terrible impact on our skeletons. As the National Institutes of Health (NIH) explains, RA causes inflammation in the membranes around joints. These membranes react by releasing enzymes that cause wear and tear on the bones.
Of course, we can't talk about bone loss without discussing osteoporosis. This is when bones lose density, making them more brittle and likely to experience fractures. And, yes, the enzymes we talked about above are a factor when it comes to RA patients developing osteoporosis. But they aren't the only reason why these two conditions can occur together. RA can cause pain in the joint that might make a patient want to move around less, which can lead to bone loss. Also, glucocorticoid medications used to treat RA can also make bones more brittle.
Just as there are risk factors for rheumatoid arthritis, there are also ones for osteoporosis. These include smoking, drinking excessive amounts of alcohol, taking in small amounts of calcium, and having a small frame. So, if you have RA and can check the boxes on risk factors for osteoporosis, you might want talk with your healthcare professional about ways to help safeguard your bones.
Bone marrow
Did you know that one of the functions of your bone marrow is to make red blood cells (via Healthline)? And make no mistake, red blood cells are incredibly important since they are responsible for transporting oxygen to all the areas of your body. But if you have rheumatoid arthritis, you could also develop another health issue that can lower your red blood cell count.
As Healthline explains, anemia is when your body makes lower than normal amounts of red blood cells. Fewer red blood cells means your circulatory system has a harder time transporting oxygen, which can lead to severe health problems. And, yes, the inflammation caused by RA can be the culprit behind anemia, as well as impact the way your body uses iron. So, it's not surprising that RA patients might experience different types of anemia like iron deficiency anemia and anemia of chronic inflammation. Plus, drugs used to treat RA, like nonsteroidal anti-inflammatory drugs (NSAIDs) and disease-modifying antirheumatic drugs (DMARDs), can also cause anemia.
Once a person is anemic, they might experience health concerns like fatigue, shortness of breath, weakness, and headaches. They also might notice their skin is paler and their hands and feet are cold. Plus, if their case of anemia has escalated to the point that their heart is receiving less oxygen, then they might have chest pain, an irregular heartbeat, or even a heart attack.
Skin
While rheumatoid arthritis can cause bumps called nodules to form inside the lungs (via CreakyJoints), that's not the only place these nodules might occur in a RA patient. According to WebMD, rheumatoid nodules are very common for individuals with RA and can form not just on organs, but also places like the fingers, the elbows, and the ankles under the skin. And although it isn't common, these bumps could be indicators of other problems developing below the surface.
As WebMD explains, sometimes nodules are telltale signs that a RA patient's blood vessels are becoming inflamed — a condition known as rheumatoid vasculitis. This can impact the skin in different ways, depending on the size of the affected blood vessel or vessels. For example, if someone with RA has inflammation in larger blood vessels like those found in the legs, this can cause ulcers and rashes. On the other hand, inflamed smaller blood vessels (such as the ones in the fingertips and near the fingernails) could lead to redness and/or sores forming around the fingernails, as well as pits developing on the fingertips.
Furthermore, medications used to treat RA can also affect the skin in a variety of ways, including making a RA patient more sensitive to sunlight and/or causing them to bruise more easily. It's also possible for someone to be allergic to different RA medicines, which can cause reactions like rashes and/or itching.
Digestive system
Inflammation of the blood vessels from rheumatoid arthritis – a condition known as rheumatoid vasculitis (via WebMD) – can cause gastrointestinal tract (or GI tract) problems like diarrhea, nausea, abdominal pain, and vomiting, as gastroenterologist Dr. Dana Lukin explained to CreakyJoints. Before we go any further, keep in mind that the GI tract is split into two areas: the upper tract and the lower tract. And RA can cause issues in both areas. Mayo Clinic researchers found that problems in the upper GI tract, like an inflamed and swollen esophagus, as well as stomach ulcers, occurred at notable rates in RA patients. This same research found that lower GI tract conditions, like inflammation of the bowels and infections, happened for a large number of individuals with RA. Additionally, RA can also lead to difficulty swallowing and bloating. And if you're wondering if different medications prescribed for RA can also cause GI tract problems, the answer is a definite yes.
Even if you suspect RA is behind your GI problems, you should still speak with your healthcare professional. As CreakyJoints points out, conditions like inflammatory bowel disease (IBD), fibromyalgia, and celiac disease can occur with RA — and all of these can cause digestive system issues.
Hair
As the old saying goes, there's good news and bad news. On the plus side, according to CreakyJoints, rheumatoid arthritis usually doesn't directly lead to hair loss. But this brings us to the not-so-good news: People with RA can experience hair loss for a variety of reasons.
Like other health concerns on this list, certain medications prescribe to treat RA can lead to hair loss, although this isn't a common occurrence. Nevertheless, if you have RA and are taking disease-modifying antirheumatic drugs (DMARDs) like methotrexate or leflunomide and are experiencing hair loss, you might want to speak with your healthcare professional. As a matter of fact, Dr. Max Hamburger, Founder and Executive Chairman of United Rheumatology, told CreakyJoints that "I've had some patients bring bags of hair that had fallen out into the office" as a result of taking leflunomide. However, Dr. Hamburger pointed out that "... leflunomide isn't used much these days."
Besides medications, the stress caused by RA can be enough to affect one's hair. Obviously the symptoms of RA can be stressful, but so too can efforts to manage it. For instance, if your healthcare professional changes your medication, that can cause stress even if it's better for your overall health in the long run. So, if you're noticing unusual things happening to your hair — like it's coming out in patches — let your doctor know.
Nails
When one hears the term "longitude," the first thought is probably map coordinates. We use vertical longitudinal lines and horizontal latitudinal lines to locate places in the world. However, if you have rheumatoid arthritis (RA), then longitudinal lines could occur on your body — specifically on your nails.
According to Healthline, the condition onychorrhexis is when vertical, parallel grooves or ridges appear on the nails. And, yes, their vertical nature is why they're referred to as longitudinal ridging. Not only is it possible for someone with RA to have this nail condition, a study from The British Journal of Dermatology involving 50 RA patients found that it was one of the "only nail abnormalities significantly associated with RA." The other type that came up often in their research was clubbing, where the nails curve downward, causing the fingers to swell and mimic the shape of a club.
Besides clubbing and longitudinal ridges, someone with RA might also experience yellow nail syndrome (via Healthline). As its name suggests, nails with this condition become yellow, and the lighter half circle at the base of the nail may no longer exist. Other symptoms of yellow nail syndrome can include thicker nails that curve on the sides. Also, RA patients should also be on the lookout for red lines under their nails. This could mean the tiny capillaries beneath their nails are leaking.
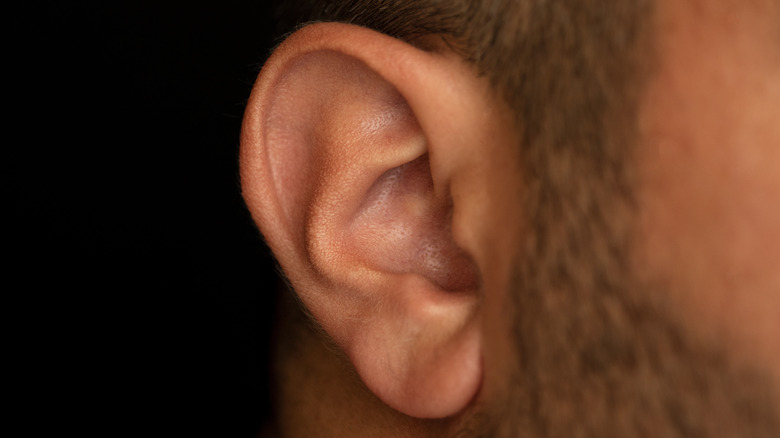
Ears
Chances are you know someone who has hearing loss. But did you know that there's more than one type? What's more, the odds of developing a certain type of hearing loss can go up if a person has rheumatoid arthritis (via Medical News Today).
So, let's first talk about the types of hearing loss. As the Hearing Loss Association of America explains on their website, the ear has three main sections: the outer ear, the middle ear, and the inner ear. If the outer or middle are damaged, then it's difficult for soundwaves to travel properly through the ear. This is what's known as conductive hearing loss. On the other hand, if the inner ear is damaged, that can lead to the brain not being able to correctly interpret the signals coming from the ear. If this occurs, then a person can have sensorineural hearing loss. Additionally, it's possible to have a combination of the two types.
Although data points to a connection between RA and hearing loss, the scientific community is still exploring what that exact connection is, according to Medical News Today. For instance, a review published in The Open Rheumatology Journal noted that rheumatoid nodules or bumps could do damage to the outer and/or middle ear. RA-related inflammation might be the culprit behind inner ear nerve damage. Environmental risk factors for RA like smoking and alcohol are also potentially involved. And additional research is exploring the possible connections between some RA medications and hearing loss.
Nerves
As WebMD points out, rheumatoid arthritis, as well as its treatments, has the potential to impact the nerves inside one's ears. But remember, our nervous systems are complex and cover far more than just our ears. So, possible RA-related nerve problems can also occur in various areas of our bodies.
Before we explore specific types of nervous system conditions, keep in mind that RA can both damage and compress nerves. The latter is why RA might worsen conditions such as carpal tunnel syndrome, since, as Orthroinfo explains, this condition occurs when the median nerve in the hand is compressed. And since this nerve is so important for the hand to function, it's not surprising that carpel tunnel can cause hand issues like numbness, pain, and tingling. But be warned, whether or not you have RA, ignoring carpel tunnel syndrome can lead to permanent nerve damage.
What's more, RA can also cause a type of nerve damage called peripheral neuropathy, per Mayo Clinic. When this happens, a patient tends to experience problems like a numb sensation and/or weakness in their feet and hands. They also might have pain in these areas that can range from tingling to burning or stabbing. However, peripheral neuropathy can also impact one's circulatory, excretory, and digestive systems. Regardless of which parts of the body are affected, if you suspect you or someone you know has a form of nerve damage, seek medical help right away.
Brain
Imagine this: You have a friend with rheumatoid arthritis. They call you upset because they forgot both their doctor's and their dentist's appointments. They confide in you that lately they've felt like their brain's been in a fog. While this might sound like a case of someone with a great deal on their mind, it could be more than that when RA is a factor.
According to the Arthritis Foundation, memory problems like the one described in the above scenario are common complaints and concerns for RA patients. But it can go beyond just forgetting appointments. A person with RA can sometimes have difficulty in conversations because they might have trouble coming up with the right words to say. Other tasks like making plans and maintaining focus can become more challenging once someone develops RA.
With that said, research is lacking when it comes to RA and cognitive issues. While the inflammation caused by RA could be a factor, the research on this has had mixed findings. The medical community is also exploring how things like the pain caused by RA and different medications prescribed to treat RA might both impact whether a patient develops brain fog. Cardiovascular disease, depression, and not enough physical activity are also potential contributing factors to RA brain fog.