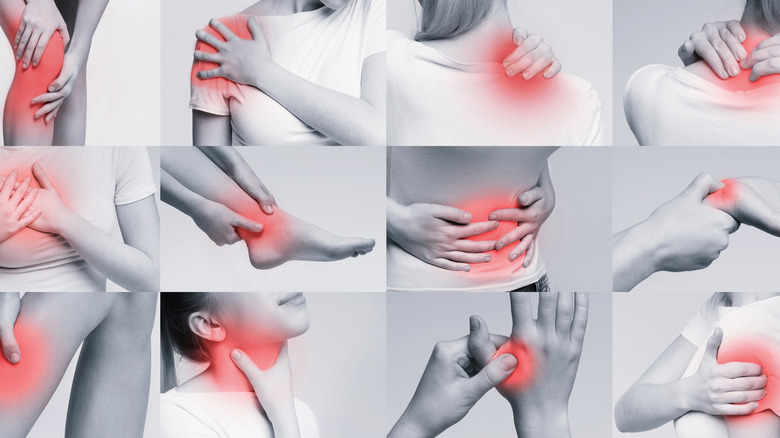
Symptoms Of Crohn's Disease You Shouldn't Ignore
Crohn's disease is one of the two main kinds of inflammatory bowel diseases (IBD). Over three million Americans have Crohn's disease, and over a quarter of those diagnosed have a close relative who shares the diagnosis (via the Crohn's & Colitis Foundation).
Those with Crohn's disease suffer from symptoms associated with swelling in parts or all of their small and large intestines. The type of Crohn's disease you're diagnosed with depends on where inflammation occurs, and it's possible to have more than one type (via WebMD). Ileocolitis, which affects the end of the small intestine (ileum) and the entire large intestine, is by far the most common type. Another common form of Crohn's, ileitis, affects only the ileum. The gastroduodenal kind occurs when Crohn's affects your stomach and the beginning of your small intestine (duodenum). Meanwhile, jejunoileitis is more commonly diagnosed in children (via IBDrelief) and affects the jejunum, the small intestine's upper half. Lastly, granulomatous colitis is rare, and affects only the large intestine.
While both Crohn's disease and ulcerative colitis (UC) fall under the umbrella of IBD, they are two different illnesses. Crohn's affects all layers of the bowel walls, while UC is contained to the colon. Additionally, with Crohn's, you still have some healthy sections of the intestine; with UC, your entire colon is inflamed (via UCLA Health). Here are some symptoms of Crohn's disease you shouldn't ignore.
Appetite/weight loss
Nearly 20% of those diagnosed with Crohn's disease report a loss in appetite, according to InflammatoryBowelDisease.net. Loss of appetite results from several factors, including cramping, nausea, diarrhea, frequent bowel movements, and tiredness (via MyCrohnsAndColitisTeam). Many people with Crohn's disease try to change their diets to contain these symptoms. Instead, it's essential to work with your doctor to determine what is causing your appetite suppression, as some of the medications prescribed for Crohn's patients also cause a loss in appetite.
Another cause of loss of appetite in those with Crohn's is that your brain and stomach monitor and respond to changes in each through signals from neurons, hormones, metabolism, the immune system, and microbes. Inflammation disrupts equilibrium, resulting in, amongst other things, appetite loss (via a study published in Inflammatory Bowel Diseases).
Loss of desire to eat is one factor that leads to undernutrition in close to three-quarters of those with Crohn's disease, according to a study published in Nutrition. Your body doesn't get what it needs, and you could end up with serious vitamin deficiencies and malnutrition. Without the proper nutrition, you could end up with further complications, including anemia and osteoporosis. Children with malnutrition can delay growth (per MyCrohnsAndColitisTeam). Your doctor can prescribe medication to help stimulate your appetite. Weight loss can also be avoided by eating healthier foods more often in smaller quantities.
Abdominal pain
In 2019, over three-quarters of those diagnosed with Crohn's disease report having abdominal pain, with over half experiencing it in the previous month (via Statista). Stomach pain associated with Crohn's disease is often debilitating and results from various factors, including signaling a relapse, side effects of medication, or surgical complications. Between one-quarter and one-half of Crohn's patients have abdominal pain while in remission (via the Cochrane Database of Systematic Reviews).
According to a paper published in Inflammatory Bowel Diseases, abdominal pain felt by Crohn's patients can also be attributed to one of three problems: a partial blockage, a gut distention, or extreme inflammation in the intestines. The cramping usually subsides when treating the cause. However, for those who continue to have abdominal pain, even through remission, it is believed that the chronic inflammation associated with Crohn's changes how the body processes pain. Constant pain not only affects the nervous system, but also changes cognitive functioning and how the brain processes pain, contributing to the increased number of Crohn's patients who are also treated for anxiety and depression.
Medical professionals recommend keeping a journal to help identify foods, food combinations, or situations that trigger abdominal pain (via Colon and Rectal Surgical Specialists of New York). It's best to speak to your doctor about new or persistent stomach pain, as it could also result from stomach ulcers, appendicitis, or acid reflux.
Flu-like symptoms
While not everyone with the flu will get a fever, it is a common symptom of the illness, as is having chills, according to the Centers For Disease Control and Prevention (CDC). These symptoms also affect those with Crohn's disease, even if they aren't experiencing stomach problems (via MyCrohnsAndColitisTeam).
When your body fights an invasion, your immune system activates, and inflammation often results. Crohn's disease inflames your intestinal tract and often brings with it fever and chills. Without treatment, this inflammation can cause abscesses to develop. Another common flu-like symptom associated with Crohn's is night sweats. Sweating brings down any body temperature rises associated with a fever. Over one-third of Crohn's patients report an inability to sleep well due to night sweats, per a paper published in Clinical Gastroenterology and Hepatology.
Doctors often prescribe immunosuppressants to those diagnosed with Crohn's disease; however, flu-like symptoms may indicate the medication isn't working as expected (via IBD News Today). Immunosuppressants stop an overactive immune system from attacking healthy cells that it mistakes for germs, but doing so also makes it difficult for your immune system to fight off infection. While acetaminophen (Tylenol) helps alleviate flu-like symptoms, speak with your doctor to treat any underlying infection (via MyCrohnsAndColitisTeam).
Joint pain
According to a paper published in BMC Musculoskeletal Disorders, over half of those diagnosed with IBD, including Crohn's, report joint pain. The inflammation associated with IBD and Crohn's isn't always the culprit of joint pain, though, as nearly half of those with Crohn's and joint pain have arthralgia or pain without inflammation. Arthritis, pain with swelling, occurs in about one-fifth of those with Crohn's and joint pain, per data published in Gastroenterology and Hepatology.
Crohn's patients with joint pain often report discomfort in their wrists, knees, ankles, and other small joints. Additionally, the pain manifests equally on both sides of the body and tends to resolve when bowel swelling subsides (via research published in Gastroenterology and Hepatology). It's important to point out that even if you are diagnosed with arthritis and Crohn's, arthritis won't damage your joints like a non-Crohn's patient with arthritis (via Crohn's & Colitis Foundation). Another cause of joint pain is steroid withdrawal. Corticosteroids are commonly prescribed to those with Crohn's disease to control inflammation, though some patients experience joint pain when they no longer require these drugs (via Gastroenterology and Hepatology).
If acetaminophen fails to relieve your pain, doctors recommend rest, using a heating pad, and seeing a physical therapist (via Crohn's & Colitis Foundation).
Nausea & vomiting
Over 70% of those diagnosed with Crohn's disease reported nausea, vomiting, or both at some point after diagnosis, per 2019 data from Statista.
While nausea and vomiting can occur without warning, medical professionals believe that, for the most part, these symptoms indicate a flare-up is about to happen in Crohn's patients (via MyCrohnsAndColitisTeam). Other causes of nausea and vomiting in Crohn's patients include bowel obstructions and reactions to medications. Regardless of the cause, see a dentist if these symptoms persist, as stomach acids can erode the enamel on your teeth (via Healthline). Additionally, your hair and nails break easily. Finally, persistent vomiting and nausea can lead to dehydration and malnourishment.
If Crohn's disease causes you to feel nauseous, it is recommended that you eat smaller portions more often instead of having three large meals (via Crohn's and Colitis Canada). Also, eat plain foods slowly and avoid triggering smells and tastes. These steps enable you to always have food in your stomach and not fill it up too fast. If you vomit, avoid solid foods and drink clear liquids slowly. Lastly, if problems persist or if you experience blurry vision, feel chest pain, or vomit blood, seek immediate medical attention.
Pain and redness in eyes
According to the Crohn's & Colitis Foundation, eye problems affect nearly 10% of Crohn's patients. While medical professionals aren't entirely sure what causes Crohn's to affect your eyes, they believe it stems from the extreme sensitivity of your eye tissues (via Medical News Today).
Episcleritis, which most often occurs during a flare-up, is caused by inflammation of the tissues between the inner eyelid lining and the whites of your eyes (via Crohn's and Colitis Canada). As a result, your eyes look red and ache. Doctors treat this condition with medicated drops. A similar but less common condition is uveitis. Per Healthline, uveitis occurs when the colored part of your eye and the tissue under the white of your eye becomes inflamed. Pain, redness, blurry vision, and light sensitivity are the result. If left untreated, uveitis can lead to glaucoma and vision loss. Keratopathy affects the cornea, or clear outer part of your eye, and often causes blister-like swelling that results in light sensitivity, excess tearing, and feeling like there's something in your eye (even when nothing is there).
Some Crohn's patients experience keratoconjunctivitis sicca, or a decrease in tear production and dry eyes (per the Crohn's & Colitis Foundation). This may cause irritation, infection, and night blindness. Lastly, glaucoma and cataracts can result if your doctor prescribes corticosteroids over a long period. Schedule regular eye examinations and see your doctor if you notice eye changes.
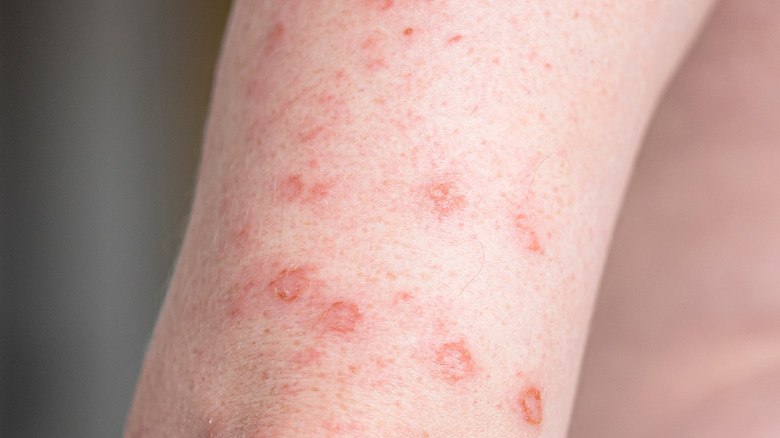
Red bumps on the skin
Less than half of Crohn's patients report skin issues (via DermNet New Zealand). Rashes and other skin issues result directly from the intestinal inflammation associated with the disease and as a side effect from some of the medications prescribed to alleviate discomfort, per a review published in Frontiers in Physiology.
According to the Crohn's & Colitis Foundation, two common skin conditions that affect Crohn's patient's legs are erythema nodosum (EN) and pyoderma gangrenosum (PG). EN appears as red bumps and often accompanies a flare-up. If left untreated, PG looks like small blisters that can turn into deep chronic ulcers. PG flare-ups usually follow the same pattern as Crohn's flares. Additionally, swelling and friction can cause some Crohn's patients to develop skin tags. Often found around the anus, these small flaps get irritated by feces and signal a flare-up by becoming tender and rubbery.
Lastly, nearly half of all Crohn's patients will develop fistulas (via the Crohn's & Colitis Foundation). Fistulas are painful lesions that connect two body parts that shouldn't be linked. Liquids often drain into the opening, resulting in an infection that needs antibiotics. If left untreated, surgery may be your only option, says Healthline.
Changes in bowel movements
Diarrhea affects 80% of those with Crohn's disease, and is the most common symptom associated with the disorder, per a paper published in Gastroenterology Clinics of North America. The severity (meaning how often you have to go) and the texture of your movements depends on where the inflammation occurs in your intestines and how bad the swelling is.
A symptom that often accompanies diarrhea is the urgent need to use the bathroom, and then not going or only releasing a little feces (via Crohn's and Colitis Canada). Fortunately, medications and diet changes can help reduce your symptoms. The main concern with diarrhea is that it can lead to dehydration, so be sure to drink plenty of water and liquids with electrolytes to avoid thirst, dry skin, and fatigue.
Some Crohn's patients suffer from constipation due to colon inflammation (via Crohn's & Colitis UK). This causes them to be unable to poop at all or fail to completely empty their bowels when they do go. Stools are usually hard or lumpy, and require you to exert extra pressure to get them out. Drinking more water, consuming more fiber, and changing your posture on the toilet help alleviate constipation.
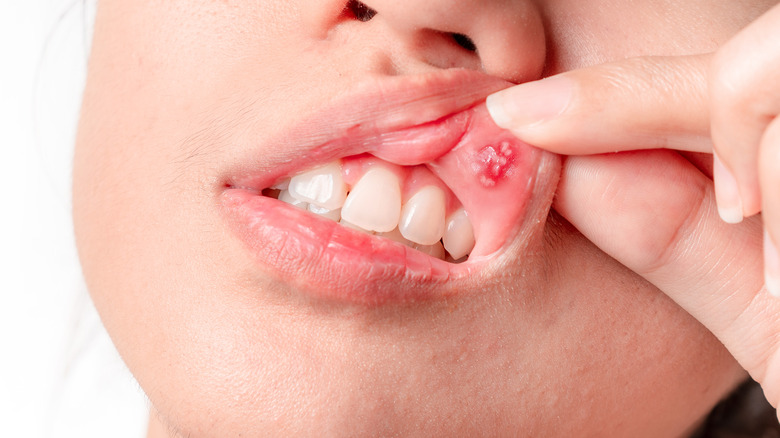
Mouth sores
Mouth sores have been said to affect up to 50% of all Crohn's patients, and often occur well before any other symptoms (via World Journal of Gastroenterology). Children with Crohn's tend to have more mouth sores than adults, and there is little to no correlation between Crohn's flare-ups and when mouth sores appear. Per the Mayo Clinic, tingling and burning usually precede the eruption of mouth sores. Once they appear, eating or drinking anything hot, spicy, or acidic can be painful (via MyCrohnsAndColitisTeam). Mouth sores can be a direct result of Crohn's. They can also result from malnutrition brought on by the disease, a vitamin B12 deficiency, and a reaction to some prescriptions used to treat the disorder.
Another mouth issue affecting Crohn's patients is oral thrush, which results from an overgrowth of bacteria and fungus (via Mount Sinai). Oral thrush is white and appears on the tongue and makes swallowing difficult. In addition, the sores associated with oral thrush bleed more when pressure (like that from a toothbrush) is applied.
Doctors often prescribe antimicrobial mouthwashes, as well as mouthwashes, gels, sprays, and lozenges that dull the pain (via MyCrohnsAndColitisTeam).
Pain in or around the anus
Nearly one-third of those with Crohn's have a version known as perianal Crohn's that results in anal inflammation (via IBDrelief). It can occur alone or in addition to other types of the disease, and causes anal pain and bleeding. If left untreated, perianal Crohn's can result in abscesses that contain infection-causing pus, skin sores, and tags, leading to pain on your bottom, tears in the lining of your anal canal, and scar tissue blocking your anal opening (via Healthline).
When the lining of your anal canal is torn, it's called an anal fissure. According to Crohn's and Colitis Canada, anal fissures often result from constipation, and are not only painful, but also annoying and itchy. Prescription ointments and increasing fiber intake usually help fissures clear.
The chronic diarrhea and constipation associated with Crohn's make hemorrhoids more common in those with the disease, per the experts at Los Angeles Colon and Rectal Surgical Associates. Hemorrhoids result from the extra pressure you put on the veins in your anal lining when you have trouble pooping. The exertion and strain cause twisting, swelling, pain, itching, and bleeding. Additionally, doctors are concerned with the development of anemia in those with both Crohn's and hemorrhoids.
Anal leakage
Nearly three-quarters of those with Crohn's suffer anal leakage or bowel incontinence (via Crohn's & Colitis UK). Medical professionals classify this symptom as either urge (which means you don't make it to the toilet in time) or passive (where you don't even realize you've gone). Diarrhea and constipation, which are symptoms of Crohn's disease, cause muscle and nerve damage that results in anal leakage (via the Mayo Clinic). Your rectum stretches and loses its ability to hold your stool.
Additionally, hemorrhoids resulting from Crohn's and rectum vein swelling make it difficult for your anus to completely close, leading to anal leakage. It may also result from the inflammation associated with Crohn's, which gives your rectum less room to store your stool. Another cause of anal leakage is surgery related to Crohn's for fistula and other colorectal repairs (via InflammatoryBowelDisease.net).
Treating your underlying Crohn's symptoms is the best way to treat anal leakage. Increasing your fiber intake and taking anti-diarrhea medications also help treat anal incontinence.
Bleeding rectum
Rectal bleeding occurs when blood exits out of your anus (via MedlinePlus). Two types of rectal bleeding can affect Crohn's patients: melaena and hematochezia. According to IBDrelief, melaena bleeding occurs due to inflammation in the upper portion of your gastrointestinal (GI) tract, including your esophagus, stomach, or the first part of your small intestine. This type of bleeding is black or plum-colored because it's older (as it takes time to travel through your body) and because your body has had a chance to digest it (per MedlinePlus). On the other hand, hematochezia affects nearly half of Crohn's patients, per a paper published in Pediatric Gastroenterology, Hepatology & Nutrition. It appears bright red because it is fresh from your lower GI tract, either your colon or rectum.
In addition to the disease itself causing bleeding, Crohn's patients can also develop rectal bleeding due to hemorrhoids, fissures, fistulas, and infection (via IBDrelief). Moreover, bleeding associated with Crohn's disease often signifies active disease and inflammation.
Rectal bleeding doesn't just occur in bowel movements. In fact, you may not see it at all, and your doctor may need to test for it. Losing too much blood can cause anemia, shock, low blood pressure, fatigue, and, if left untreated, hospitalization. Let your doctor know if you suspect rectal bleeding.
Anemia
As the Mayo Clinic explains, anemia occurs when your body doesn't have enough red blood cells to keep an adequate amount of oxygen flowing. One-third of those diagnosed with IBD, including Crohn's, also have anemia (per the Crohn's & Colitis Foundation). Crohn's patients develop anemia due to intestinal inflammation interfering with iron absorption and resulting from blood loss caused by the disease. Certain medications block the body from absorbing nutrients like the iron required to help make the red blood cells it needs.
The most common symptoms associated with anemia include fatigue and an inability to concentrate, according to an article in Gastroenterology Review. These result from your heart working harder to pump oxygen (via the American Academy of Family Physicians). Other anemia symptoms include paleness, shortness of breath, cold hands and feet, intense headaches, and dizziness. However, Crohn's disease and managing the related symptoms can also cause these issues, particularly fatigue (per Mount Sinai).
The concern with Crohn's patients developing anemia is twofold. First, due to the slow nature of its occurrence, many patients "are usually unaware that they are losing blood," said Dr. James Marion, a professor of medicine and gastroenterology at Mount Sinai's Icahn School of Medicine. Additionally, many patients adapt to anemic symptoms making it difficult for them and their doctors to recognize them, per a review in Gut. Left untreated, anemia can result in being so tired you can't get out of bed, pregnancy complications, and irregular heartbeat (via the Mayo Clinic).
Kidney stones
When you urinate, liquid waste leaves your body. When there's insufficient liquid, the waste crystalizes and grows, forming a kidney stone (via the National Kidney Foundation). While some stones are small enough to pass, others cause pain through irritation and blockage. Kidney stone symptoms include intense pain on one side of your lower back and a stomach ache that doesn't seem to go away. Bloody urine, or urine that looks cloudy and smells terrible, and flu-like symptoms including nausea, vomiting, fever, and chills are other indications of kidney stones.
According to research published in the Archives of Gastroenterology, one-third of Crohn's patients develop kidney stones (usually due to the disease changing how your body digests food, per IBD News Today). As the Crohn's & Colitis Foundation explains, the disease makes it difficult for your body to absorb fat and water. The chronic diarrhea often associated with Crohn's can cause dehydration that leads to the creation of kidney stones, as do bowel resections and other Crohn's-related surgeries (via a paper in the Proceedings of UCLA Healthcare).
Diet changes, including limiting sodium consumption and drinking more water, help limit your body's creation of kidney stones (via the Cleveland Clinic). Kidney stones put you at greater risk of developing kidney disease, so seek immediate medical attention if the pain is unbearable. If a kidney stone develops and becomes too large, cannot be passed, blocks the flow of urine, or causes an infection, surgery may be required for removal (via the National Kidney Foundation).