Everything You Wanted To Know About Sciatica
According to a report by the National Center for Health Statistics, nearly 20.5% of the adults in the United States expressed that they were living with chronic pain, with about 7.4% of them experiencing work and life disruptions due to it. And the Health Policy Institute at Georgetown University also found that when it comes to chronic back pain, about 16 million adults are living with the condition. Sciatica is among the different types of low back pain that most people have chronically.
A 2020 report by Bloomberg predicted that, based on its trend over the years, the sciatica market may expand due to the rise in new cases of sciatica. It also points out that there will be a higher demand for sciatica interventions such as muscle relaxants, antidepressants, pain relievers, opioids, epidural steroids, and behavioral and physical therapy. This goes to show that sciatica is a growing concern for most people around the world. However, if we're well-versed with the condition in terms of how it comes about, and how we can prevent, treat and manage it in the long term, we can reduce the growing population that gets it.
In this article, we'll take a look at everything you want to know about sciatica — we're hoping the information will help you reduce days off from work and have fewer life disruptions because of it.
Sciatic nerve pain comes in varying forms
Sciatic nerve pain expresses itself in varying forms, and so it responds differently when it's addressed. Going by Spine Health, there are times when it becomes intense and weakening to the one who has it — through extended periods or sometimes brief but consistent moments of pain. Two months is usually the average lasting period for the pain. If it goes beyond that, the pain may be chronic sciatica. On the other hand, if it persists for a period under two months, it's classified as acute sciatica. Four types of sciatic nerve pain exist: Bilateral, neurogenic, alternating, and referred sciatica (per Early Bird by Amerisleep).
Bilateral sciatica is the pain that appears when there's a strain (pinching) on each of the sciatic nerve ends. The pain may affect one leg more than the other, and you feel it not only in your legs but also your backside. Neurogenic sciatica is the type of pain that originates in the spine. When the sciatic nerve stretches, your spine gets unnecessarily stressed — causing sudden excruciating pain in your feet, legs, and back. Alternating sciatica "may be a result of degenerative issues in the sacroiliac joint, the joint connecting the spine to the hips, or sacroiliac arthritis." The pain felt in this type arises from one compressed side of the sciatic nerve but impacts both legs. Lastly, referred sciatica brings pain caused by issues with your joint and muscles. The pain may be less intense but persistent and can be more severe in the back compared to your legs (via Early Bird by Amerisleep).
Factors that influence sciatica's occurrence
Dr. Bonaventure Ngu from the Premier Spine Institute says that there are several aspects that make sciatica more likely to be a problem for you in the near future. One of them is smoking. If you smoke a lot, you increase the nicotine content in your body, which ends up reducing blood flow and causing issues like slow recovery from nerve injuries and a longer-than-normal healing period. Also, people with obesity have higher chances of getting sciatica because the additional weight causes a contracting effect in the sciatic nerve — leading to the condition. If your job also involves carrying strength-requiring objects over and over again, the hustle will slowly create tension in your sciatica nerve and spine, and put you at risk.
Your posture matters a great deal, too. Some postures may keep your spine away from its natural and proper placement, which may cause unevenness and muscle strain — with time, exhaustion and nerve pain follows. Also, people with diabetes may be on the edge of developing sciatica. They experience slow healing and have poor blood flow due to the extreme amounts of blood glucose in their body. Plus, this state puts them at risk of diabetic neuropathy — a common form of nerve impairment for those with diabetes.
First Choice Chiropractic also mentions age, being unhealthy, consistent low back pain issues, sleep-related issues, injuries that affect your bottom and hips (or which hits at the sciatic nerve straightforwardly), and being mentally overwhelmed as other possible factors.
Mild and extreme symptoms
Sciatica symptoms often vary from mild common symptoms experienced by people with other general health issues to extreme symptoms unique to sciatica. The affected spinal nerve root (a bundle of fiber that stems from the spinal cord) is what often determines the severity of the symptoms you'll experience — although there's always a possibility that several spinal nerve roots can get pinched all at once (via Spine Health).
Beginning with the mild ones, some noticeable symptoms include a feeling of feebleness in your feet and legs that make taking continuous steps an arduous task, and pain increase or reduction as you change your posture. As for the posture change symptom, if you notice that when you stand or make an attempt to stand, or when you stretch yourself on your bed or couch, you feel more pain or the pain lessens, you may have sciatica. Deep leg pain may also be an indicator of sciatica. The Dynamic Physiotherapy & Sports Injury Clinic notes that, unlike most conditions where the pain shows up mostly where a health problem is, sciatica presents pain that stretches to your leg from the area around your buttocks. If you also feel pain when you lift your leg, you may need to get a test called the Straight Leg Raise to determine if your case is really sciatica.
Some of the extreme sciatica symptoms are losing your reflexes in your ankles and knees, losing sensitivity in your legs (especially your inner calves and some toes), and having frail hips and thighs (per Spine Health).
Sciatica causes
According to Harvard Health Publishing, sciatica occurs when there are health issues with some of your nerve roots such as the S1 (located below the L5 nerve root in the lower back), L4 (located above the L5 nerve root) and L5 (located between the L4 and S1 nerve roots). When one of your joints, ligaments, bones, or disc causes friction against your sciatic nerve, some contraction and vexing may happen, which may lead to inflammation. The inflammation then heightens the sensitivity of your nerves and tissues which, in turn, increases sciatica pain. Some known contributors of sciatic nerve contraction and vexing include trauma and herniated disc.
Beginning with trauma, when you get into a car accident or get bruises from your favorite sport or even drop from a high place and land on your lower back, you may affect the sciatic nerve and get sciatica. Herniated discs come from the damage to the spinal disc's content that looks like gel. The content causes a noticeable protrusion on your lower back and may cause tension on a neighboring nerve which may lead to mixed signals in your brain that eventually bring about sciatica. Health Harvard Publishing further mentions pregnancy, spinal stenosis (the restriction of the canal that preserves your spinal cord), and spondylolisthesis (the unintentional sliding of one spinal bone on top of the one above it) as other possible causes. Spinal tumors and piriformis syndrome may also bring about sciatica (via Ortho Bethesda).
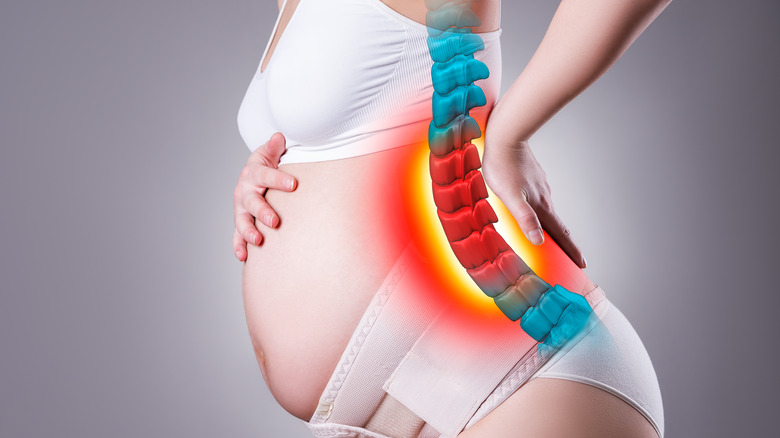
Sciatica and pregnancy
When you're pregnant, lower back pain is among the many complications you experience. And sciatic nerve pain is one of the contributors. The pain comes about from spinal contraction caused by the different pregnancy-related changes that happen in your body. Firstly, relaxin — a hormone that makes the ligaments less tense and also adjusts the pelvis for a smoother delivery — gets released in your body during pregnancy. Secondly, as the pregnancy advances the size of the baby increases, and both the size increase and less firm ligaments can change your gravity's center and put your sciatic nerve under pressure, causing sciatica (per WebMD).
Sciatica-related pain occurs anywhere along the pregnancy period, although most women feel it around the 28th week. Some of the symptoms people experience include problems when you sit, walk or stand, short-lived (and sometimes persistent) pain in one leg especially from the foot to the hip, feeling like you generally lack strength, losing sensations, and having pain pricks. When you notice these symptoms, you should seek immediate medical attention from the doctor who's helping you through your pregnancy. Some of the solutions your doctor may advise you to use include prenatal massage, physical therapy, or chiropractic therapy. Gentle stretches including the seated piriformis stretch, the pigeon pose, foam rolling (for hamstrings and glutes) and the hip flexor stretch can really help (via Healthline). RMC Health System also mentions the child's pose as part of prenatal yoga for this kind of pain.
The diagnosis
When you finally decide to go for a medical checkup, the first step you'll have to take is consultation. Here, you're going to discuss your concerns with a spine expert and they'll ask you several questions to understand your situation and also get to know your medical history (per Spine Universe). Dr. Jean-Jacques Abitbol says some of the questions to expect include where your pain pops up the most, your activities in the last few days or weeks, when you began feeling the pain, how severe you feel the pain is, things you do that increase or lessen the pain, and the interventions you've used to handle it in the past.
Complete Orthopedics also adds that your doctor will want to know if you've lost your bladder or bowel control and if you can sense tissue paper when it touches your backside.
After the consultation, you'll do a series of tests that help determine for sure if you have sciatica. Some of the tests include imaging tests like a discogram (that reveals any issues with your intervertebral disc) and an MRI (Magnetic Resonance Imaging) that provides the doctor a clear view of your sciatic nerve and nerve roots, along with any herniated discs, tumors, and inflammations around that area. Other tests you may do are the slump test and the straight leg raise test. Both of these tests include raising your legs while in different positions to check for pain and sensation alteration as you move, which may show the possibility of sciatica (via Spine Health).
Sciatica treatment methods
Once the diagnosis is complete and sciatica is there, the next step is to begin treatment. Your doctor may recommend different treatment options based on your case. There are several non-surgical options you can explore if surgery is not on the table. One of them is using medication — you might be prescribed drugs that reduce inflammation and release tension in the muscles. For short-term pain alleviation, medications such as Non-Steroidal Anti-Inflammatory Drugs (NSAIDs — for example naproxen and aspirin) or Acetaminophen are good selections. Although not all the time, medications that deal with seizures or depression may be viable options as well (per WebMD).
Southern Pain and Neurological also recommends cold-heat therapy (using ice packs on the source of pain and following that up with hot objects if the pain persists), and nerve blocks together with radio-frequency (using nerve blocks to understand how your pain works, and then using radio frequency to neutralize the pain in the long term) and epidural steroid injections (administering local anesthesia and steroid drugs straight into the area around the spinal cord and nerve roots).
Illinois Bone & Joint Institute also says the more passive treatment Transcutaneous Electrical Nerve Stimulation — which uses low electric voltage to target sciatica pain — can be useful in handling sciatica. This intervention enhances the production of endorphins, which are natural pain relievers in your body to handle the pain.
Surgery for sciatica
WebMD explains that surgery is a less common approach for most people with sciatica. A handful of people who may have to consider this option include those who have been on the previously mentioned non-surgical treatments and didn't get any effective results after about 90 days — or those who, during diagnosis, mentioned issues with their bladder and bowel regulation. Disc Sports & Spine Center also states that if the sciatica is causing major interruptions in your work, social and personal life, your doctor may tell you to consider surgery. Also, if the feebleness and sensation loss symptoms are recurring and getting worse by the day, the most preferred treatment may be surgery.
To treat sciatica, you can have one of two surgical procedures: laminectomy and diskectomy. In a laminectomy, you receive general anesthesia, followed by a two-hour procedure where the surgeon takes away the lamina (a section of the bone ring surrounding your spinal cord) and neighboring tissues which are responsible for the tension and pain in your sciatic nerve. This procedure may require you to take some time before you can continue walking as usual. Diskectomy, unlike laminectomy (which is more focused), targets anything including a bone spur that's bringing tension to your sciatic nerve. You'll get general anesthesia and (possibly) return home the same day as your diskectomy surgery (via WebMD).
Complementary remedies
Some of the reliable complementary remedies that can help ease the pain that comes with sciatica include chiropractic treatment combined with massage and physical therapy, explains Southern Pain and Neurological. When it comes to chiropractic treatment, the intervention can improve how your spine moves by slightly tweaking it. If you still have tight muscles after that, a follow-up massage can help relax the tense muscles. Physical therapy, on the other hand, can be useful alongside physical exercises in addressing the root cause of sciatica, keeping sudden pain intensification at bay, and dealing with the symptoms. It makes the tissues in your backside, abdomen, lower back, and pelvis stronger and more flexible. Illinois Bone & Joint Institute suggests strength training, aerobics, and stretching as some of the recommended physical exercises that accompany physical therapy.
Another effective complementary option is yoga. This ancient practice seeks to bring your body, spirit, and mind together to work in oneness. Several types of yoga approach this goal through different techniques. Some of them include Hatha yoga (which works with controlled force), Kripalu yoga (which uses compassion, meditation, physical healing, and acceptance), Power yoga (which uses fitness techniques that resemble aerobic exercises), and Vinyasa yoga (which combines poses with breath). Some of the commonly used yoga poses and stretches that help with sciatica are the basic seated stretch, scissor hamstring stretch, sitting spinal stretch, standing hamstring stretch, knee-to-opposite shoulder, and the forward, reclining, and sitting pigeon poses (per Healthline).
The advancement of sciatic pain and later complications
When you receive quick and proper treatment, sciatica may completely disappear in about a month or a month and a half. Those people who don't seek treatment risk suffering long-lasting pain as sciatica may be originating from a serious nerve root impairment. Aside from the pain, other complications that may develop along the way include muscle atrophy (muscle mass thinning or loss) in the leg experiencing pain, and having walking problems. Hyperalgesia — the condition where you experience heightened pain sensitivity which makes normal pain feel twice as severe as it should — is another likelihood (via Painscale).
In extreme cases, you may get irreversible nerve impairment. This normally occurs when the cause of the tension in your sciatic nerve becomes more intense over time or if the nerve contraction stays for long periods. The after-effects of this damage may include responding poorly to sciatica interventions and the pain becoming even more intense. Moreover, you may lose control of your bladder and bowels permanently. This problem begins as a regular symptom but becomes permanent if you don't get treated immediately. Additionally, your motor control can be impacted too. When your sciatica advances, the nerves develop more problems and end up entirely affecting how your muscles and signals of pain operate on the affected area (per Westside Pain Specialists).
Painscale also explains that advanced sciatica may cause cauda equina syndrome which is "compression of a collection of nerve roots" and bring about other issues like paralysis in the lower side of your body, sexual dysfunction, and even losing sensations in your private parts, thighs or backside.
Prevention and management
Preventing and managing sciatica takes the same shape and form. A series of affordable and easy-to-work-with tips can help keep sciatica nerve pain away and also keep it under control (if you already have it). The Center for Spine & Orthopedics advises you to mind your posture every time, make sure that when picking up massive objects from the ground you keep your knees bent, and engaging in physical exercises often.
Some of the exercises you should consider adding to your daily routine include the back flexion stretch, sciatica stretch, sitting spinal stretch, reclining pigeon stretch, and hamstring stretch. And as you go to sleep, you can also engage in some of these stretches and then have a warm bath afterward. Also, a firm and comfy mattress can help vastly cut down the pain you normally feel as you sleep (via Spine & Pain Clinics of North America).
Harvard Health Publishing states that keeping tabs on your weight can also go a long way in managing sciatica. Excess weight in your body can make your spine become overwhelmed and increase the possibility of herniated discs. And if you have sciatica and obesity, your recovery journey for sciatica may be longer than it should. Also, if your daily routine involves extended sitting periods, you should consider workarounds — for example, working at standing desks and having regular breaks in order to stretch and walk. These simple changes can help you reduce the stress on ligaments and discs in your lower back that come from sitting for an extended period.