Myths You Should Stop Believing About Hysterectomies
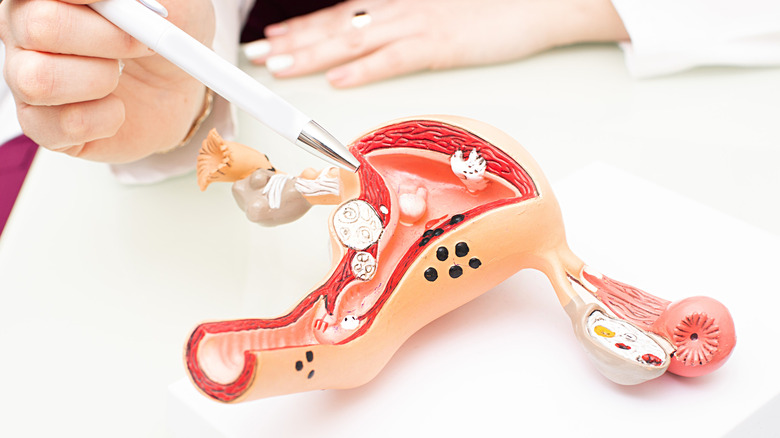
The uterus or womb is a lightbulb-looking, fist-sized organ that rests between the bladder and rectum of women (via the Cleveland Clinic). It's where the fetus grows. In the absence of a fetus, its lining sheds and women menstruate. This organ is the source of symptoms like pain, discomfort, or heavy bleeding for many women. These can be caused by certain conditions, including cancers of the uterus, cervix, or ovaries, fibroids, endometriosis, pelvic prolapse, pelvic pain, or excessive bleeding. Getting a hysterectomy, that is, removing the womb through surgery, treats these conditions (via the New York State Department of Health). This procedure saves the lives of some women. For others, it improves their quality of life.
The National Women's Health Network (NWHN) reports that among U.S. women of childbearing age, hysterectomies are the second most performed surgeries, after the cesarean section. Some procedures include the removal of the cervix, upper part of the vagina, ovaries, fallopian tubes, or surrounding tissues, depending on the illness. The surgery can be performed through the vagina or abdomen. It can be done laparoscopically through these routes. Robot-assisted methods are also available.
Getting a hysterectomy is a big decision. There's a lot of information about the procedure and its outcomes. Some are untrue — and scary. Here are some misconceptions you should dismiss.
Myth: A hysterectomy is a high risk surgery
A hysterectomy is a major surgery just like heart surgeries, cesarean sections, or joint replacements (via Far North Surgery). Major surgeries involve cutting the body to access, repair, or remove damaged tissues. All major surgeries have risks. However, hysterectomies are safe and have fewer risks than many major surgeries. The chances of encountering surgical complications depend on your health, the type of surgery being performed, and how good your doctor is (per U.S. Pharmacist).
Surgical risks are usually anticipated. So, they can be prevented or corrected during or after the surgery. The most common minor complication (seen in 6% to 25% of cases) is infection of the surgical wound or surrounding tissues. This is prevented and treated with antibiotics. A more serious complication is excessive bleeding (hemorrhage). It's seen in up to 3% of cases. It's usually caused by a cut in the vagina that can be stitched. Blood for transfusion is always prepared before the surgery, should the need arise. Thromboembolic disease (blood clots) is another possible complication. It can be prevented using blood thinners before or after the surgery. Women are also encouraged to move around or wear compression socks to prevent blood clots. Injury to the bladder, bowels, or ureter during surgery is possible, but rare. Injuries can be corrected during or after the surgery.
Myth: All hysterectomies leave a large scar
Scars form when wounds heal, and surgical wounds are not exempt. You might envision a large, awful scar from a hysterectomy, but that's not always the case. Vaginal hysterectomies don't leave any outward scars (via Healthline). Meanwhile, laparoscopic and robotic techniques leave scars, but they're small and can even be hidden in the belly button.
Abdominal hysterectomies, on the other hand, leave long horizontal scars at the bikini line (above the pubic hairline) or vertical ones from the belly button to this line. However, the other techniques are preferred to abdominal hysterectomies. Abdominal hysterectomy scars don't always look bad. Good scars are flat and bend into the skin. But some scars are widespread or stretched, raised and thick (hypertrophic), or severely raised, thick, and widespread (keloid), via Scar Score. While this does depend more on your skin type, the doctor's expertise contributes.
There are some things you can do to make your scar look better. While it heals, avoid straining it by lifting heavy stuff, doing chores, swimming, or being constipated (so you need lots of fiber and water). You should also watch out for signs of infection like discharge, fever, heat, or redness. You need to get infection addressed, as it could worsen your scar. After your scar heals you can use special bandages or massage to improve its appearance. You can talk to your dermatologist about skin resurfacing for old scars. Tattooing around (but not on) an old scar can be a creative way to conceal it (per Wise Geek).
Myth: It'll be easy to bounce back after your procedure
You can't jump right off the operating table to your busy life. You just had a major surgery after all. The good news is you won't stay long in the hospital. Most patients are discharged two or three days after an abdominal hysterectomy (via WebMD). And discharge for laparoscopic, robotic, or vaginal hysterectomies can be the same day or the next. Afterwards, you'll need to recover at home. Recovery can take up to eight weeks after an abdominal hysterectomy, while other procedures have recovery times as short as two weeks.
Take things easy during your recovery. You shouldn't lift heavy stuff, or do anything strenuous (via Spire Healthcare). Light walking is encouraged, but sit out the heavy exercises or gradually reintroduce them. You shouldn't have sex, or put anything into your vagina till you're given the clear. You should eat a balanced diet with lots of fiber. Also, don't drive until you're comfortable operating a car. And you'll need your doctor's okay to return to work.
You might battle with symptoms during your recovery: exhaustion, bad appetite and palate, vaginal bleeding or discharge (which should become lighter), hot flushes, and other signs of menopause (if your ovaries are removed). It might take as long as five days to poop after your surgery. It's also normal to get depressed, feel a sense of loss, or have trouble concentrating or sleeping after your surgery (via Dana Farber Cancer Institute).
Myth: How you view your womb doesn't matter
The womb is part of the identity of many women. It's a symbol of sexuality, fertility, and motherhood. Many women worry about their femininity, attractiveness or sexual appeal post-hysterectomy. This concern is greater among younger women. Many women also experience grief over the loss of the womb even if they can't see or feel that something's gone. Additionally, women are prone to other psychological health issues (such as depression, anxiety, agitation, and sexual dysfunction) due to hysterectomies. These prompt many women to seek professional help after a hysterectomy (via a study published in the Journal of Nursing and Health Science).
How women feel about removing their wombs influences the decision to get a hysterectomy (per research published in The Qualitative Report). Facing a possible hysterectomy, some women got protective of their wombs, for cultural reasons, to carry children, or just because it's their wombs. These feelings were often ignored because they weren't considered "rational." However, the author observed that these feelings play a big role in the decision to have the surgery. Participants chose doctors and consumed health information that aligned with their values of protecting the womb. The author urged that the values of women should be considered when deciding to have a hysterectomy.
Myth: You won't enjoy sex after a hysterectomy
After your recovery, you should be able to have (and enjoy) sex. Some women even find that they enjoy sex more after surgery because the symptoms they experienced are gone (via Flo Health). Sex after a hysterectomy can even be freeing because you won't get pregnant. However, it's more than just being able to have sex. You might need time to adjust due to emotional changes or because sex doesn't feel the same.
Healthline notes that women who have their ovaries removed often experience vaginal dryness and lubricants can ease the discomfort. Another reason why sex might feel different (per Flo Health) is that if the cervix is removed, the vagina becomes shorter affecting the depth of penetration. A hysterectomy also could affect your ability to orgasm, but shouldn't stop it, notes Healthline. The womb and cervix contract during an orgasm, contributing to the sensation. Thus, the removal of these parts could reduce the intensity of an orgasm. Also, the cervix is pretty sensitive and adds to the pleasure of sex. But the clitoris, that nub at the top of your inner vulva, is spared. It's also sensitive and likely connected to the hard-to-find G-spot claimed to be responsible for an orgasm. Clitoral orgasms are possible, but it might require some getting used to if you're new to them. The site advises you to take your time, explore, and be open with your partner.
Myth: Removing your womb means you'll go through menopause
Removal of just the womb doesn't send women to menopause (via WebMD). They go through menopause later if they're premenopausal. However, it's possible for these women to experience an earlier menopause than other women with wombs. But if the ovaries are removed, a premenopausal woman will immediately enter surgical menopause. The procedure for this has its own name (oophorectomy) and it's done with some hysterectomies. The ovaries produce estrogen, and menopause happens when estrogen levels decline. This decline is sharper in surgical menopause than natural menopause. So, women experience sudden, sometimes severe, menopausal symptoms.
Oophorectomies are commonly done with hysterectomies to treat ovarian cancer, or prevent it in high-risk women (per a systematic review in the Cochrane Database of Systematic Reviews). There's debate about its necessity for premenopausal women who don't have cancer. Ovarian cancer, while deadly, is rare, with a 1.4% risk in all women. The chance that oophorectomies reduce this risk is low. But they're more beneficial to women who have high ovarian cancer risks. Apart from plunging women into menopause, studies show that there's an increased risk of cardiovascular diseases, osteoporosis, and dementia following oophorectomies. Per another systematic review in the Cochrane Database of Systematic Reviews, the most common (and deadliest) form of ovarian cancer originates from the fallopian tubes. So, removal of the fallopian tubes during a hysterectomy (opportunistic salpingectomy) could reduce the risk of ovarian cancer. Both reviews call for more studies on the actual benefits of these surgeries, though.
Myth: Hysterectomies cause weight loss
For different reasons, some women lose weight after a hysterectomy (via Healthline). But weight loss is not directly caused by the removal of the womb. Weight loss could be due to nausea or vomiting, which some people experience following the surgery. These could be caused by pain, or could be a side effect of the anesthesia used. Some women get chemotherapy and hysterectomies to treat reproductive cancers; nausea, vomiting and weight loss are side effects of chemotherapy.
Hysterectomies, however, are associated with a risk of weight gain overtime in women who keep their ovaries. Menopause is associated with an average weight gain of five pounds. So, women who have their ovaries removed run this risk. You might also gain some weight during your recovery period while you avoid strenuous activity. If you're concerned about this, Flo Health advises that you talk to your doctor about engaging in light exercises. You can also opt for low-calorie foods and small portion sizes, avoid alcohol, and eat whole grains, fresh fruits, lean proteins, and dark, leafy vegetables.
Myth: There would be a void where your womb used to be
You might wonder what happens to the space the womb occupies after it's removed. Is there just a big hole where the womb used to be? This is a concern of many women who undergo hysterectomies, says Dr. Streicher.
The womb itself is the size of a small pear. So, the space left behind might not be too large if you don't have large fibroids (some fibroids can be as large as a nine-month pregnancy). In any case, there's no void left behind. The Nava Center notes that nearby organs (like your intestines) will move to occupy the space. As this happens, you might experience incontinence or other symptoms. If your cervix will be removed, your doctor will stitch the top of your vagina to form a vaginal cuff, so it's not left open.
So, what happens to the other parts of the reproductive system once the middle part is removed? If your cervix isn't removed, it will have its bearings on the walls of your vagina (via Healthline). If the ovaries are spared, they will maintain their attachments to the fallopian tube and abdomen via ligaments. So, they will maintain their position, even if they aren't attached to the womb anymore. If the ovaries release eggs, they will disappear into your abdomen.
Myth: Many women regret getting hysterectomies
You might wonder if other women who have had hysterectomies would wish to take it back. After all, how women feel about their decision post-hysterectomy matters.
In a 2019 study published in the Journal of Patient Experience, 96% of women interviewed did not regret their surgery. Another 2019 study, published in the Journal of Obstetrics and Gynecology Canada, included only women under 35 years. They found that 90% would make the same decision again, and 91.5% agreed that it was the right choice.
With that said, not having regrets immediately after the surgery doesn't mean a woman's opinion can't change. A 2020 study published in the Journal of Patient-Centered Research and Reviews interviewed women to find the patterns of regret in the following year post-hysterectomy. They found that 7.4% of participants had high regret scores that worsened over time, while 13.3% had high regret scores that reduced over time. The women with lower regret scores (79.3%) had even lower scores over time. Another 2020 study, published in the American Journal of Obstetrics and Gynecology, found that over 90% of women were satisfied with their hysterectomy. The authors also assessed the regret of the loss of fertility after 3 years. They found that 21% of women who removed their wombs alone and 43% of women who removed the ovaries as well regretted the loss of fertility 3 years later.
Myth: You don't have a say when it comes to getting a hysterectomy
U.S. history from the 20th century has it that some women were forced into getting hysterectomies, while some who wished to have the surgery were denied (via Women Advance). Some women had to jump through hurdles (e.g., insurance, religious institutions, medical guidelines) before getting sterilized. It was common for women of color to be threatened and sterilized during labor, says sociologist Heather Dillaway.
The American College of Obstetricians and Gynecologists notes that funded programs targeted and forced women of color, women of low income, and women in prison into hysterectomies and tubal ligations. Now, they call for better patient counseling about the risks, benefits, and alternatives before sterilization procedures. They discourage the "doctor knows best" manner of approach and urge for a more collaborative one. Overall, it's what matters to the women that should come first.
Per one study published in the Journal of Patient-Centered Research and Reviews, many women felt they were well informed about their options and surgical plan. However, they also reported that they depended on what their doctor recommended. And because of this, they felt they weren't in charge of their decision. They recommend that women research for themselves before deciding. A study published in Geburtshilfe und Frauenheilkunde found that proper counseling, informed consent discussions, sufficient time to make a decision, and a patient's confidence in the decision to have a hysterectomy influenced quality of life, sexual function, and patient satisfaction post-surgery.
Myth: Getting a hysterectomy is your only option
Per the National Women's Health Network, getting a hysterectomy is the only available option and can be life-saving in instances of invasive cancer of any reproductive organs, unmanageable infection or bleeding, and certain labor complications. However, women have other options for many other diagnoses.
Talk to your doctor about alternative treatments before resorting to a hysterectomy. This procedure can be life-altering and comes with risks, so it shouldn't be done unnecessarily. Research from 2015 (via the American Journal of Obstetrics and Gynecology) indicated that alternative treatments to hysterectomies were underused for women with abnormal uterine bleeding, endometriosis, uterine fibroids, and pelvic pain. These are benign conditions, and a hysterectomy is not required to save a life. Alternative treatments were not explored for 38% of the women, and many of the remaining women explored one option. They also found that 18% of the hysterectomies performed were unnecessary.
Hysterectomy alternatives depend on your condition. For fibroids, there's the option of "watching and waiting" for them to shrink after menopause. More proactive measures include techniques to shrink the fibroids and some surgeries like myomectomy and myolysis to remove fibroids without removing the womb or terminating fertility (via the Office on Women's Health). For uterine prolapse, Kegel exercises or using vaginal pessaries may be effective. Drugs like pain relievers and hormonal birth control can be used for endometriosis. Lastly, endometrial ablation and dilation & curettage (D&C) are available to some women with excessive vaginal bleeding.