Signs Your Itchy Skin Could Actually Be A Blood Clot
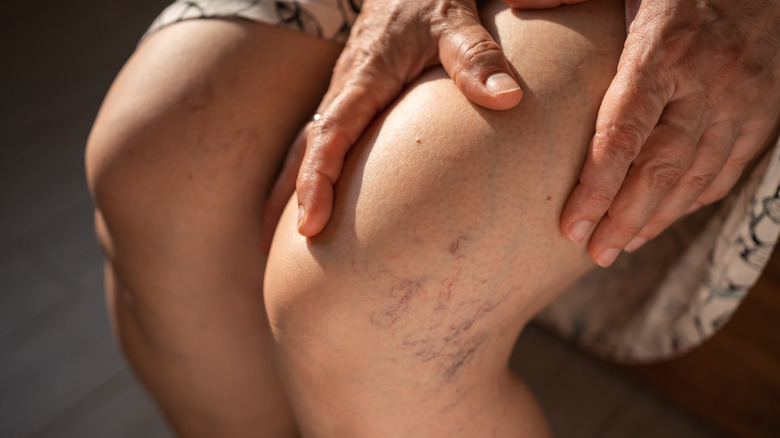
If you've had an itch that's been driving you nuts for a few days, you might need to look deeper rather than just blowing off that incessant itch as eczema or dermatitis. Itch can be an uncommon symptom of a serious type of blood clot called deep vein thrombosis (DVT).
You have a lot of deep veins that run through the muscles of your body. When a clot forms in this area, it can resolve on its own or cause symptoms and complications. According to InformedHealth.org (via National Library of Medicine), about one in 1,000 people develop this condition yearly. Once the clot forms, the blood can leak, and the vein becomes damaged. This damage leads to inflammation and dry skin in the affected area, which causes the rash and itch known as post-thrombotic syndrome. This syndrome can have devastating effects since the damage to the vein lingers after the clot has been resolved.
We will explore a few signs that your itch might indicate a blood clot lurking in your veins. You'll also learn how blood clots are diagnosed, what their treatment options are, and why you don't want to wait to treat this condition.
Blood clot symptoms that may accompany itchy skin
An itch alone isn't typically enough to state that you have a blood clot since many things can cause itchy skin, like a bug bite, psoriasis, and atopic dermatitis. But, when combined with a few other symptoms, it signals a blood clot could be lurking in your veins. WebMD states that swelling is usually one of the first symptoms. The area of the clot could swell up, or you might have swelling in your whole leg or arm, depending on where the clot is. The swelling can also be severe, causing pitting. This means when you push on the swollen area, the indent you create stays in the skin, leaving a pit.
Pain is also common with DVT, according to WebMD. When a blood clot starts, it might begin as tenderness in the arm or leg. It can even be a dull ache or cramp. You might experience pain when you walk on or use the affected limb, says UPMC Health Beat.
As the vein and surrounding tissue become inflamed and swollen because the clot is blocking the blood flow, the area can become red and hot. This typically happens as the condition has advanced, according to Informedhealth.org. It occurs because blood pools up due to damage in the vein caused by the clot.
Risk factors and diagnosis of blood clots
Before you head to the doctor to get your leg itch checked out to ensure it's not DVT, take note of any risk factors you have. Those sitting for a long time, like mandatory bed rest or on a long plane or car ride, might be more at risk due to the lack of movement. It's also essential to consider any blood clotting disorders you might have or if you've had a major surgery recently. These conditions are more likely to cause itching and swelling due to a blood clot.
However, they aren't the only risk factors, states InformedHealth.org. Those who are older than 60 or who've had a previous DVT should take their symptoms seriously. Additionally, your mom or dad having a DVT could make one more likely for you. It's also more frequent in those who are obese, smoke, take hormone therapy or contraception, or are pregnant, states the University of Michigan Frankel Cardiovascular Center.
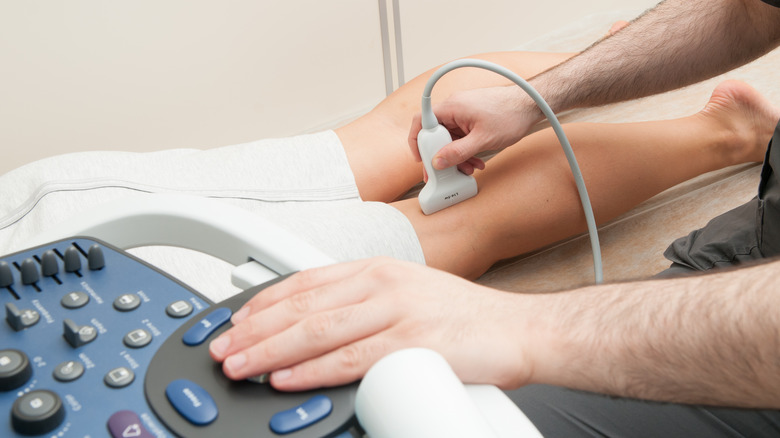
Treatment for DVT isn't done with symptom verification alone. Penn Medicine explains that a provider will perform a D-dimer blood test, which looks at the protein that breaks down clots. They also might do a CBC and ultrasound exam on the affected limb. Once the diagnosis is made, treatment can include surgery or medications to thin the blood.
How to prevent blood clots
Itchy skin that turns out to be a blood clot can have serious side effects. For example, the blot could break off and move into other areas of the body, specifically the heart and lungs. When blood stops reaching the heart or lungs, it can be fatal, according to the Centers for Disease Control and Prevention (CDC). Prevention is critical to making sure that a blood clot doesn't cause you trouble in the future.
For your blood to keep moving and pumping, you must also keep moving and pumping. Get up and walk around as soon as possible when you've had surgery or have been confined to bed. Invest in compression stockings when you're worried about DVT happening in your legs. Stop every few hours and walk around during long trips. You can even take walks down the aisles of the plane to keep moving. The CDC also recommends wearing loose clothing and avoiding a sedentary lifestyle to help prevent the formation of blood clots.