Hypothermia Explained: Causes, Symptoms, And Treatments
We tend to think of hypothermia as a life-threatening condition caused by extreme cold. However, as a clinical matter, hypothermia refers, simply, to a core body temperature below 95 degrees Fahrenheit. At temperatures between 90 and 95 degrees Fahrenheit, hypothermia is rarely deadly, according to MedScape. Indeed, hypothermia has an overall mortality rate of only 12%, including both mild and severe cases. Moreover, not all hypothermia occurs accidentally as a result of extreme weather conditions. In fact, sometimes hypothermia is induced intentionally in a clinical setting for therapeutic purposes.
That being said, hypothermia can cause death — and that's true even when it occurs indoors, at moderate temperatures, intentionally, and/or in a seemingly controlled environment. Even when hypothermia does not cause death, or when hypothermia is caused intentionally, it can lead to debilitating organ damage (via Up To Date). What is most important in all hypothermia cases is the initiation of treatment as soon as possible after recognizing that hypothermia is occurring. And that doesn't actually require a temperature reading so much as an understanding of hypothermia's causes, symptoms, and treatment modalities. In fact, to truly understand hypothermia, how to avoid it, and how to recover from it, it is helpful to recognize that regardless of the proximate cause of hypothermia in any particular case, it always results from the same mechanism: the loss of body heat faster than the body can create and maintain heat, per Mayo Clinic.
Medically-induced hypothermia can have therapeutic value
Although hypothermia is a clinical diagnosis, it also refers to a state induced, locally or systemically, by medical practitioners for therapeutic purposes, according to a 2006 paper published in the journal Continuing Education in Anesthesia Critical Care & Pain, which traces this treatment modality to Ancient Greece, where it was used to treat hemorrhage and other trauma. A 2009 paper published in the Scandinavian Journal of Trauma, Resuscitation, and Emergency Medicine suggests that inducing hypothermia to treat trauma is still seen as beneficial. The Miller-Keane Encyclopedia and Dictionary of Medicine, Nursing, and Allied Health specifically discusses its current use in improving limb amputation outcomes. Moreover, locally induced hypothermia has shown promise in improving survival in patients with severe pancreatitis, according to the Mayo Clinic, citing a 2019 study published in the academic journal, Gastroenterology.
As the 2019 paper explains, "induced hypothermia generates a state of metabolic depression," which is to say that controlled cooling slows cellular turnover and decreases oxygen needs in cells, which can be the difference between cell death and cell preservation. Given the catastrophic nature of brain cell death, induced hypothermia has shown perhaps the greatest utility in improving neurological outcomes after cardiac arrest, which immediately deprives brain cells of oxygen, according to the American Medical Resource Institute, which cites a promising protocol developed at the University of Pennsylvania for cardiac arrest patients at risk for "ischemic brain damage" (i.e., insufficient blood flow to the brain). Induced hypothermia can also be used to help babies deprived of oxygen at birth.
Accidental hypothermia may be primary or secondary
Accidental hypothermia is most commonly a response to extreme environmental cold, according to 2004 paper published in American Family Physician. Clinicians refer to this diagnosis as "primary hypothermia." However, anything that may be going on within the body that interferes with thermoregulation (i.e., the body's ability to regulate its temperature) may also cause or exacerbate accidental hypothermia, according to ScienceDirect. When a secondary cause is at work, "secondary hypothermia" may be diagnosed.
For example, consuming alcohol may lead to hypothermia under cold environmental conditions that would not necessarily cause hypothermia in someone who has not consumed alcohol, per Drug and Alcohol Research and Training Australia. One reason is that consuming alcohol is associated with heat loss due to expansion of blood vessels. Additionally, alcohol may reduce the body's impulse to shiver (while associated with "feeling" cold, shivering is a protective mechanism by which the body generates heat, per The Journal of Physiology). Further, alcohol may diminish one's ability to perceive loss of body heat, thus prolonging exposure to cold.
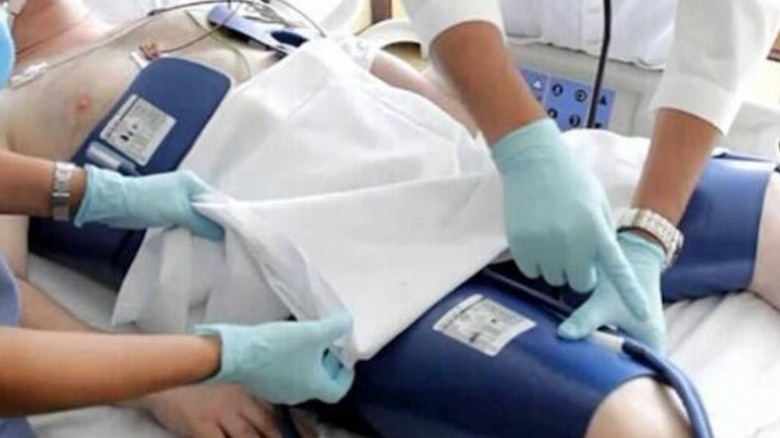
Secondary hypothermia may also occur post-surgery due to factors such as anesthesia drugs (which may impair the body's ability to regulate temperature), a cold operating room environment, or intentional cooling techniques used during surgery (via Acute and Critical Care). Other causes of secondary hypothermia include metabolic disorders such as hypothyroidism and diabetes, as well as malnutrition, Parkinson's disease and other brain disorders, central nervous system dysfunction, and spinal cord injury (via Mayo Clinic).
Anyone is at risk for accidental hypothermia under the right circumstances
Hypothermia is a broad term that refers to the body's core temperature being below a level that is considered functional (via Medical News Today. The fact that it is most commonly associated with extreme outdoor weather conditions is really just due to the fact that as the external temperature drops, hypothermia becomes a risk for even in the healthiest people with no secondary factors. For example, hypothermia could occur in literally anyone who sets foot outside during Antarctica's harsh "permanent night," per Cool Antarctica. It can also occur in anyone who finds themselves submerged in water with a temperature of below 40 degrees Fahrenheit, per the law firm of Hofmann & Schweitzer, which specializes in maritime accidents, including cases of immersion-related hypothermia.
Ultimately, anyone is at risk for experiencing accidental hypothermia when exposed to any level of cold for which their particular body is ill-equipped to generate sufficient heat to make up for the resulting heat loss, according to Cleveland Clinic. Accidental hypothermia can even happen indoors, and not just in the context of surgery. "There are no hard-and-fast rules as to the exact temperature at which you can get hypothermia or the amount of time it takes," as ER doctor Thomas Waters said to the Cleveland Clinic. He adds, "Even at room temperature, you can become hypothermic," depending on your own particular circumstances.
Health conditions that can contribute to hypothermia
As warm-blooded animals, humans rely on an internal system known as "thermoregulation" in order to maintain a body temperature of approximately 98.6 degrees Fahrenheit (via Medical News Today). Human thermoregulation involves the convergence of multiple systems. These include, among others, thermoreceptors throughout the body that recognize (without conscious thought) that the body's temperature is getting out of whack, and the central nervous system, which among other things produces hormones that respond to cold environmental stimuli via shivering and other heat-generating bodily mechanisms. Thermoregulation also involves the circulatory system, which dilates and expands blood vessels to warm extremities. Further, thermoregulation involves cognitive processes such as those that help us to dress appropriately for the external temperature.
Accordingly, any disease or condition affecting any bodily system supporting thermoregulation can place an individual at risk for hypothermia, with or without extreme environmental cold. For example, sepsis, a serious systemic infection, has been associated with hypothermia for reasons that are still under investigation (per ApolloMD). Hypothermia is also seen in diabetes patients experiencing severe hypoglycemia, possibly reflecting a "decrease in energy demand during glucose deprivation" (via Diabetes and Metabolism). A propensity toward hypothermia (and hyperthermia) has been seen in people with brain damage, per 1994 study published in Brain Injury.
Reasons the elderly are at increased risk for hypothermia
The elderly population is at an increased risk of experiencing hypothermia — whether outdoors or indoors, and even at temperatures that might not strike a younger person as particularly cold — because many of the realities of aging undermine the body's ability to regulate its own temperature. Among those realities are certain underlying medical conditions, according to the National Institutes of Health. For example older adults are more likely to have diabetes, per Endocrine Web, and diabetes presents an increased risk for hypothermia, per 2012 study published in Diabetes and Metabolism. Older adults are more likely to experience circulatory problems, including high blood pressure, which may increase the relative risk of hypothermia, per Cleveland Clinic.
Some medicines that tend to be taken by the elderly may also increase the risk of hypothermia by interfering with the body's response to cold. These include antidepressants and blood pressure medications. Even some over-the-counter cold medications may even interfere with the body's optimal thermoregulation, per NIH. Moreover, the elderly are at an increased risk of falling and not being able to get up — which can be a set-up for hypothermia, for example, when someone is stranded on a cold floor in an unheated basement (via Cleveland Clinic). And cognitive decline may interfere with an older adult being able to detect significant temperature changes or to react to them appropriately (by adding layers or going inside).
Why babies are at higher risk for hypothermia
Babies, and especially newborn babies and premature babies, are at higher relative risk for accidental hypothermia, even at temperatures that might not seem particularly cold to an adult, per University of Rochester Medical Center. In fact, the threshold for hypothermia in a baby is not 95 Fahrenheit, but slightly higher at 97.5, per Kids' Health. One reason that babies are at higher risk for hypothermia is that they may not be able to adequately communicate to their caregivers that they are feeling cold, according to Better Health Channel –one of the baby-specific symptoms of hypothermia is a weak cry, per Kids Health. Further, and from a physiological standpoint, babies do not yet possess a fully developed thermoregulation system. For example, babies are born with neither the ability nor the impulse to shiver, according to Merck Manual Professional Version. Shivering, which is an important mechanism in thermoregulation, develops outside the womb over the first several months of life.
In addition, babies simply tend to lose heat at a faster rate than adults due to their "high surface area to volume ratio." This heat loss process is even faster in low-birth-weight newborns, per Merck Manuals Professional Version. But several specific factors at play in all newborn babies, regardless of weight, include the fact that all babies are born wet (with amniotic fluid) and completely bare, both of which can accelerate heat loss upon exposure to the air.
Why accidental hypothermia is not uncommon after surgery
If you have ever woken up after a surgery during which you were under general anesthesia, you may be familiar with the phenomenon known as post-operative shivering. Post-operative shivering is a common and often discomfiting complication after anesthesia, according to a 2018 study published in the Romanian Journal of Anesthesia and Intensive Care, and it is frequently caused by hypothermia. In fact, "mild hypothermia" (clinically defined as a core body temperature of between 90 and 95 Fahrenheit, per Better Health Channel), is common after general anesthesia, according to a 2010 study published in Anesthesia Progress. Declines in temperature that go beyond the clinical definition of mild hypothermia are also sometimes seen after surgery, and these may be associated with cardiovascular complications, the need for transfusion, and higher rates of post-operative infection and post-operative hemorrhage. In addition, post-operative hypothermia can affect the way drugs are metabolized by the body. Although there has been little clinical data on the long term effects of post-surgical hypothermia, it may be associated with a higher mortality rate within the one year following surgery (via Acute and Critical Care).
How to recognize the mild to moderate stages of accidental hypothermia
Accidental hypothermia is a progressive condition. Accordingly, its symptoms tend to evolve as the condition progresses. In what is clinically known as "mild hypothermia," the core body temperature is between about 90 and 95 Fahrenheit, and in addition to a sensation of coldness — regardless of the environmental temperature — one may feel such vague symptoms as fatigue, nausea, hunger, rapid heart rate, and pale-dry skin, according to a Hypothermia (via StatPearls). Shivering is also very common in mild hypothermia. However, it's absence should not rule out hypothermia, because shivering stops as the body depletes itself of energy and the core body temperature dips to between about 86 and 90 Fahrenheit.
As hypothermia progresses toward the moderate stage (82.4 to 86 F core body temperature), your central nervous system will begin slowing down, as will the blood flow to your brain and other vital organs, including your heart and lungs. Although you will likely remain conscious throughout the moderate stage of hypothermia, it will become increasingly challenging to stay awake and alert as fatigue and lethargy set in. Your reflexes may slow. Your pupils may become dilated and increasingly unresponsive. Your ability to communicate will become increasingly impaired, as will your mental clarity. And that includes your ability to recognize that your body temperature is dropping and that you are in the midst of a medical crisis (per Centers for Disease Control and Prevention).
Severe hypothermia involves an altered state of consciousness
Hypothermia that is allowed to progress to the point where the core body temperature dips below 82.4 F is known as "severe hypothermia," according to Medscape. The skin may begin to look blue, and reflexes will gradually be lost. Severe hypothermia is characterized by an altered state of consciousness due to the fact that as your body temperature decreases, your heart rate, cardiac output, and blood pressure also decrease, thereby diminishing blood flow to the brain (via Hypothermia). Accordingly, in severe hypothermia, it's difficult, if not impossible, for an individual to seek help for themselves, per Safety + Health Magazine. At the same time, respiratory distress, heart failure, and cardiac arrest become significant risks. In severe hypothermia, the risk of death approaches 40%, even if hospital treatment is initiated, per Medscape. However, in many who die from hospital-treated severe hypothermia, an infection has also taken hold.
Strangely enough, severe hypothermia is also characterized by what is clinically referred to as "paradoxical undressing" (via Hypothermia). In paradoxical undressing, one feels so overheated that they are compelled to remove layers of their clothing. According to TrustCare, this may be a function of the blood vessels dilating in a "last ditch attempt to warm freezing tissue in your limbs." It would also seem to go along with impaired cognitive function.
How hypothermia is treated
At all stages of hypothermia, the first thing to do is stop the heat loss and provide insulation from further heat loss, according to John A. Downing, Director of Minnesota Sea Grant. In mild hypothermia, "getting the person to warm conditions and wrapping them in dry insulating materials should help enable them to shiver and rewarm themselves," Downing explains. In addition, applying heat to the torso via a hot water bottle, electric heating pad, or a chemical heating pack can benefit people with all stages of hypothermia, although care must be taken because hypothermic skin is susceptible to burning at temperatures not otherwise considered to be risky.
In mild hypothermia, consuming food and beverages that are high in calories can help someone replenish their energy stores. In moderate and severe hypothermia, by contrast, food or beverages are contraindicated, and the patient should be kept lying down (and in some cases, there is no other option). Further, in moderate and severe hypothermia, Downing recommends speedy evacuation to a hospital setting for further evaluation, not to mention intravenous fluids to prevent dehydration and exhaustion. In severe hypothermia, both breath and pulse may be too weak to be detected, particularly in the field. However, before it is assumed that the person is dead or that the person requires cardiopulmonary resuscitation (CPR), the pulse should be checked at the carotid artery for at least a minute. If the heart has indeed stopped, then CPR may be indicated.
Someone with severe hypothermia may be revivable
Paradoxical undressing is not the only paradox at play in severe hypothermia. Another is the fact that while hypothermia may cause cardiac arrest, it may also function as a form of life support, preventing or delaying death by keeping the patient in a sort of suspended animation. In other words, in hypothermia, if someone is found cold and unconscious with no discernable pulse or heartbeat, they should be presumed to be alive (in the absence of a catastrophic injury), according to John A. Downing, the Director of Minnesota Sea Grant. Or at least they should be presumed alive until they've been warmed and resuscitation has been attempted, according to a 2014 retrospective study published in the journal Resuscitation, the title of which begins with the phrase "Nobody is dead until warm and dead."
In fact, thanks to the accumulated scientific data regarding people who have survived hypothermia-induced cardiac arrest, the medical community has been able to make the leap to investigating the use of medically induced hypothermia in victims of gunshot and stab wounds to give surgeons an expanded window of time in which to operate, per Smithsonian Magazine.
The connection between hypothermia and COVID-19
Back in December 2019, when COVID-19 was first identified in Wuhan, China, one of the very first patients studied by clinicians and researchers alike was a 62-year old man whose first symptoms were simply fatigue and hypothermia, per 2020 paper published in the journal eNeurologicSci. Since hypothermia was not a known symptom of COVID-19, it led to some confusion before the man was finally diagnosed with the virus. The upshot was that the research team made a recommendation that "special attention" be given to hypothermia and its relationship to the COVID-19 pandemic.
So it was written, so it was done: In April 2021, a different set of researchers published in the journal Cureus the results of a study they conducted to determine where hypothermia fits into the pandemic. What they came up with was that hypothermia is, in fact, one of the many symptoms of COVID-19 — of 57 ICU patients with severe COVID-19 whom the researchers studied, 21 presented with hypothermia during their stay in ICU. Further, the ones with hypothermia were 2.18 times more likely to die from COVID-19 than the patients who didn't have hypothermia. Accordingly, not only can COVID-19 cause hypothermia, but hypothermia would appear to worsen one's prognosis.